You may wonder if your exercise habits are helping or hindering your fertility. This concern is valid; fertility is sensitive to many lifestyle factors, and physical activity is no exception. Just 30 minutes of extra vigorous exercise a week can slash conception odds by 16%. The relationship between exercise and fertility is complex, and finding the right balance can feel overwhelming.
Research shows that moderate exercise can support reproductive health for all genders, improving hormone balance, metabolic health, and, in some cases, pregnancy rates. However, too much or too intense exercise may disrupt ovulation in women or lower sperm quality in men, especially when combined with low energy intake or chronic stress. The key is to avoid extremes and tailor your activity to your unique needs and health status, knowing that both inactivity and overtraining can pose risks to your fertility goals
Below you’ll find the science behind that balance and practical steps to find your personal sweet spot.
- How does exercise intensity biologically change fertility outcomes?
- What is the evidence-based “sweet spot” of weekly exercise for fertility?
- Where do current guidelines fall short—and how can you personalize your plan?
- Which warning signs tell you your workouts are hurting fertility?
- How should men balance exercise for optimal sperm health?
- Can syncing workouts with your menstrual phases boost conception chances?
- Which exercises boost fertility without overtaxing the body?
- What adjustments keep you safe during IVF or other fertility treatments?
- Your Top Questions, Answered
- So where is your personal sweet spot?
- References
How does exercise intensity biologically change fertility outcomes?
Exercise intensity directly affects your fertility by influencing hormones, inflammation, and reproductive organ function. Moderate physical activity supports fertility for all genders. It helps balance hormones, reduces inflammation, and improves blood flow to reproductive organs. For men, moderate exercise can boost sperm quality and testosterone, while for women, it can regulate ovulation and improve outcomes, especially if you have obesity.
However, high-intensity or excessive exercise can disrupt your reproductive system. In women, it may cause irregular periods or stop ovulation. In men, it can lower testosterone, increase oxidative stress, and reduce sperm quality. One recent systematic review found that high-intensity physical activity was linked to an approximately 16% reduction in fertility odds compared to low activity, while moderate activity showed no negative effect.
Key biological changes from intense exercise include:
- Disruption of the hypothalamic-pituitary-gonadal axis, which controls reproductive hormones
- Increased oxidative stress and inflammation, harming sperm and egg quality
- Lowered testosterone in men and altered menstrual cycles in women
As Dr. Behzad Hajizadeh Maleki, PhD, notes: “Chronic moderate-intensity exercise is superior to high-intensity training in improving markers of male reproductive function, suggesting that intensity, duration, and type of exercise all matter for fertility outcomes”.
Aim for regular, moderate exercise to support your fertility, and avoid extremes unless advised by your healthcare provider.
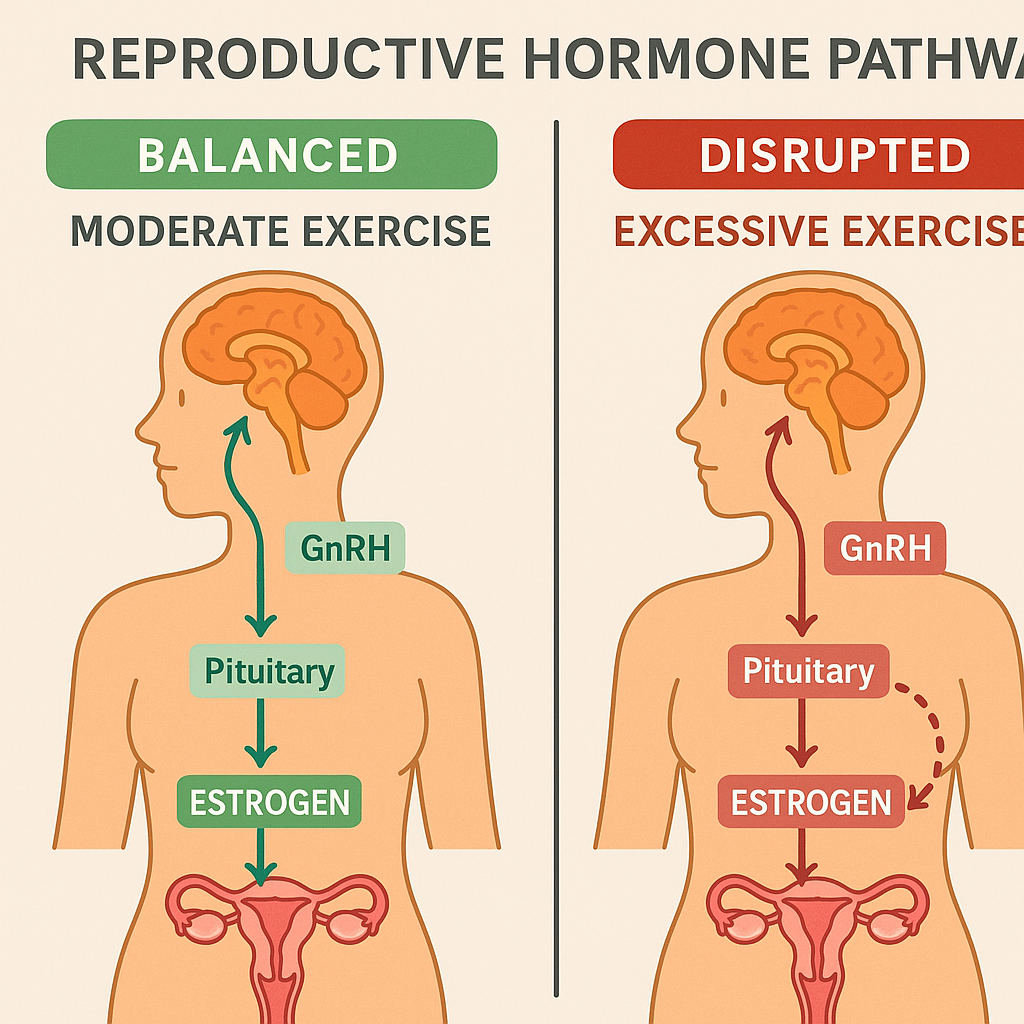
What is the evidence-based “sweet spot” of weekly exercise for fertility?
The best evidence suggests that moderate exercise—about 30 to 60 minutes per day, most days of the week—strikes the right balance for supporting fertility in both women and men. For women, especially those trying to conceive, vigorous activity in this range is linked to a lower risk of ovulatory infertility, while very high levels of exercise (over 60 minutes daily) may increase the risk of missed ovulation or menstrual irregularities. For men, moderate physical activity improves semen quality and hormone balance, but excessive or intense training can have the opposite effect, reducing sperm quality and testosterone levels.
Key recommendations:
- Aim for 150 to 300 minutes of moderate-intensity exercise per week (such as brisk walking, cycling, or swimming).
- Avoid extreme endurance training or very high daily exercise volumes unless advised by your healthcare provider.
- Combine aerobic activity with some strength and flexibility work for overall health.
- Choose moderate-intensity activities like brisk walking, cycling, or swimming for 150–300 minutes per week. This range supports hormone balance and reproductive health for all genders.
- Include both aerobic and strength-training exercises. Strength training 2–3 times per week can improve metabolic health, which is linked to better fertility outcomes.
- Prioritize consistency over intensity. Regular, moderate exercise is more beneficial than sporadic, high-intensity workouts.
- Listen to your body. If you notice missed periods, fatigue, or decreased libido, consider reducing exercise intensity or duration and consult your healthcare provider.
- For women with polycystic ovary syndrome (PCOS) or obesity, combining exercise with dietary changes can help restore ovulation and improve fertility.
- Avoid excessive endurance training (over 60 minutes of vigorous activity daily), as it may increase the risk of ovulatory issues in women and lower sperm quality in men.
- Incorporate stress-reducing activities, such as yoga or meditation, which may further support reproductive health
Dr. O. Hakimi, PhD, notes: “Vigorous exercise of 30–60 minutes per day is associated with reduced risk of anovulatory infertility, but extremely heavy exercise (>60 minutes/day) increases risk”. Following these guidelines can help you find the “sweet spot” that supports your fertility while promoting your overall well-being.
Need a starter plan? Download the Low-Impact Workout Calendar: 30-Day TTC Plan for day-by-day guidance.
Where do current guidelines fall short—and how can you personalize your plan?
Current exercise guidelines for fertility often fall short because they lack specific, individualized recommendations. Most guidelines suggest general activity levels but do not address the ideal type, frequency, or intensity of exercise for improving fertility outcomes. This is especially true for people with obesity or specific conditions like polycystic ovary syndrome (PCOS), where research shows exercise can help but does not clarify which routines work best. For men, the evidence is also mixed—while moderate activity is usually beneficial, the effects of different exercise types and intensities are not well defined, and few randomized trials exist.
To personalize your plan:
- Track your menstrual cycles or semen quality to see how your body responds to different exercise routines.
- Adjust intensity and duration based on your energy levels, stress, and any changes in reproductive health.
- If you have a specific diagnosis (like PCOS or obesity), work with your healthcare provider to tailor your exercise plan.
- Combine exercise with other healthy lifestyle changes, such as balanced nutrition and adequate sleep, for the best results.
- Remember, what works for one person may not work for another—listen to your body and seek professional guidance when needed.
As Dr. R. Maher, PhD, notes: “There is a lack of information on the ideal type, frequency, intensity, and setting of exercise to improve fertility outcomes. Closer attention to the principles of exercise prescription will help improve fertility outcomes, mainly live birth rates, for those with female infertility and obesity”
Wearable Fitness Guide will help you monitor heart-rate variability and recovery—early clues you’re veering off balance.
Which warning signs tell you your workouts are hurting fertility?
Warning signs that your workouts may be harming your fertility include changes in your menstrual cycle, such as missed periods, irregular cycles, or complete loss of menstruation (amenorrhea) for women. For men, watch for decreased libido, erectile dysfunction, or noticeable changes in semen quality, such as reduced volume or motility. Both genders should be alert to persistent fatigue, trouble recovering from workouts, or frequent injuries, which can signal overtraining and hormonal disruption.
Specific warning signs include:
- Missed or irregular periods (women)
- Loss of ovulation (women)
- Decreased sex drive (all genders)
- Erectile dysfunction (men)
- Noticeable drop in semen quality (men)
- Chronic fatigue or poor workout recovery (all genders)
- Unexplained weight loss or low body fat (all genders)
- Increased stress, anxiety, or mood changes (all genders)
“An energy drain, low leptin, and fluctuating opioids caused by excess exercise have been implicated in hypothalamic-pituitary-adrenal dysfunction, leading to ovulatory disturbances” 1. If you notice these signs, consider reducing exercise intensity or duration and consult your healthcare provider to protect your fertility.
If any appear, review the checklist above on Overtraining Warning Signs.
How should men balance exercise for optimal sperm health?
To optimize your sperm health, balance is key. Aim for regular, moderate-intensity exercise—such as brisk walking, cycling, or resistance training—about 150 to 300 minutes per week. This level of activity improves sperm count, motility, and morphology, and reduces oxidative stress and inflammation, which are linked to better fertility outcomes.
Both aerobic and resistance exercises are beneficial, but avoid excessive endurance training or very high-intensity workouts, as these can disrupt hormone balance, increase testicular temperature, and harm sperm quality.
- Choose a mix of aerobic (e.g., cycling, swimming) and resistance training.
- Avoid prolonged, intense endurance sports (like long-distance triathlons) unless advised by a specialist.
- If you have obesity or metabolic issues, combining exercise with dietary changes can further improve sperm health.
- Listen to your body: persistent fatigue, reduced libido, or other warning signs may mean you need to scale back.
Low-to-moderate intensity exercises are more beneficial for male reproductive health than high-intensity exercises, which have a negative effect on spermatozoa. By maintaining a consistent, moderate exercise routine, you support your fertility and overall well-being.
Can syncing workouts with your menstrual phases boost conception chances?
Current research does not provide strong evidence that syncing workouts with specific menstrual phases significantly boosts conception chances. While hormone levels fluctuate throughout the menstrual cycle and may cause small, individual differences in exercise performance, a large systematic review and meta-analysis found only trivial reductions in exercise performance during the early follicular phase (when menstruation begins). However, no clear guidance for optimizing fertility by timing workouts to cycle phases. Instead, the evidence suggests that a personalized approach like listening to your own body and adjusting exercise based on how you feel during each phase may be most effective.
Importantly, excessive or strenuous exercise, especially if combined with weight loss, can disrupt menstrual cycles and temporarily reduce fertility, so moderation is key. For women with conditions like PCOS, regular exercise and a healthy lifestyle can help regulate cycles and improve conception chances, but there is no data showing that syncing workouts to menstrual phases offers additional benefits. Overall, while tracking your cycle may help you optimize comfort and performance, there is no strong evidence that it directly increases your chances of conception.
Cycle-Smart Workouts and Two-Week Wait Workouts will help you work through this journey.
Which exercises boost fertility without overtaxing the body?
Exercises that boost fertility without overtaxing the body are those performed at moderate intensity and tailored to individual comfort and health status. For both men and women, activities like brisk walking, cycling, swimming, and gentle circuit training have been shown to improve reproductive health by enhancing hormone balance, reducing inflammation, and supporting cardiovascular function. For women, especially those with obesity or polycystic ovary syndrome (PCOS), regular moderate aerobic exercise such as walking or cycling can help restore ovulation and improve conception rates, while excessive or high-intensity workouts may disrupt cycles and reduce fertility.
For men, moderate aerobic and resistance exercises are linked to better semen quality and hormonal health, but strenuous endurance training or very high volumes can have the opposite effect. Incorporating core strengthening, stretching, and relaxation techniques such as yoga or targeted “reproductive gymnastics” may further support fertility by improving blood flow and reducing stress. The key is to avoid overtraining: aim for 30–60 minutes of moderate activity most days, listen to your body, and adjust as needed to maintain energy and regular reproductive function.
Browse five proven poses in Yoga for Fertility. Add light resistance twice weekly—body-weight squats, mini-band rows—to maintain muscle; find safe routines in Strength Training.
What adjustments keep you safe during IVF or other fertility treatments?
To stay safe during IVF or other fertility treatments, focus on gentle, moderate-intensity activities like walking, light aerobic exercise, and relaxation techniques, while avoiding high-impact or strenuous workouts.
Research shows that maintaining an active lifestyle with these types of exercise can reduce risks such as gestational diabetes and preeclampsia in women undergoing IVF, without increasing adverse maternal or fetal outcomes.
However, many women experience anxiety about physical activity during IVF, often choosing gentler routines and listening closely to their bodies to avoid overexertion or discomfort.
Progressive muscle relaxation and stress-reducing activities, such as yoga or laughter therapy, can help manage anxiety and depression during treatment, though they do not directly affect IVF success rates.
If you are overweight, a supervised program of diet and exercise before starting IVF may improve your chances of a live birth, but once treatment begins, prioritize safety and emotional well-being over aggressive fitness goals.
Always consult your fertility specialist before starting or changing your exercise routine, and stop any activity that causes pain, bleeding, or unusual symptoms.
Detailed guidance lives in Exercise During IVF. Continue matching calories to activity; a slight surplus may even enhance follicle growth.
Your Top Questions, Answered
Will keeping HIIT classes hurt my chances if my cycles are regular?
If your menstrual cycles are regular and you feel well, continuing HIIT classes is unlikely to harm your fertility. In fact, high-intensity interval training (HIIT) can reduce inflammation and oxidative stress, which may benefit reproductive health, but moderate-intensity exercise tends to have the most favorable impact on fertility markers. The key is to avoid overtraining or excessive exercise, which can disrupt cycles and reduce fertility, especially if you notice changes in your period or energy levels.
Does my partner’s heavy weight-lifting routine affect sperm quality?
Heavy weight-lifting, if not excessive, generally does not harm sperm quality and may even support hormonal health and semen parameters. However, very intense or prolonged training; especially if combined with anabolic steroid use or inadequate recovery can negatively affect sperm count and motility. Moderation and proper recovery are important for optimal sperm health.
Is yoga alone enough exercise while TTC?
Yoga can be a beneficial form of exercise while trying to conceive (TTC), as it reduces stress and supports overall well-being. However, for optimal fertility, combining yoga with moderate aerobic activities like walking or cycling may provide additional benefits, especially for those with obesity or metabolic concerns. Yoga alone is safe, but a varied routine may be more effective for reproductive health.
How fast will fertility improve after adjusting exercise?
Improvements in fertility markers, such as semen quality or menstrual regularity, can often be seen within a few weeks to a few months after adjusting exercise habits. For men, semen parameters may start to improve after about 1–3 months of consistent, moderate exercise, with some studies noting changes as early as 30 days. For women, cycle regularity and ovulation may also improve within a similar timeframe, especially if exercise helps achieve a healthier weight or reduces stress.
So where is your personal sweet spot?
The “sweet spot” for exercise and fertility is regular, moderate-intensity activity; enough to support overall health and reproductive function, but not so much that it stresses the body or disrupts hormonal balance.
For most people, this means aiming for about 30–60 minutes of moderate aerobic exercise (like brisk walking, cycling, or swimming) most days of the week, possibly combined with some resistance or core-strengthening work. This level of activity is linked to improved sperm quality and ovulation, better hormone regulation, and reduced inflammation, all of which support fertility in both men and women. In contrast, very intense or prolonged exercise such as daily sessions over 60 minutes or high-volume endurance training can impair reproductive hormones and fertility, especially if it leads to fatigue, weight loss, or menstrual changes.
For women with obesity or PCOS, moderate exercise (with or without dietary changes) is especially effective for restoring ovulation and improving conception rates. For men, moderate activity boosts semen quality, but excessive training or overheating (from tight clothing or long cycling) can be harmful. Ultimately, the best approach is a balanced, sustainable routine that feels energizing; not exhausting while supporting a healthy weight and regular cycles or semen parameters.
Download the Low-Impact Workout Calendar, and start tuning your routine today.
References
-
The effects of three different exercise modalities on markers of male reproduction in healthy subjects: a randomized controlled trial… Reproduction, 153 2, 157-174 . https://doi.org/10.1530/REP-16-0318.
-
Effects of physical activity and sleep duration on fertility: A systematic review and meta-analysis based on prospective cohort studies. Frontiers in Public Health, 10. https://doi.org/10.3389/fpubh.2022.1029469.
-
The Effects of Menstrual Cycle Phase on Exercise Performance in Eumenorrheic Women: A Systematic Review and Meta-Analysis. Sports Medicine (Auckland, N.z.), 50, 1813 - 1827. https://doi.org/10.1007/s40279-020-01319-3.
-
Effect of Exercise on Ovulation: A Systematic Review. Sports Medicine, 47, 1555-1567. https://doi.org/10.1007/s40279-016-0669-8.
-
The Current Landscape of Exercise and Female Fertility Research: A Narrative Review… Reproduction. https://doi.org/10.1530/rep-22-0317.