You may wonder if pushing your body too hard in the gym could be working against your fertility goals. This concern is valid. Women who log more than 5 hours of high-intensity exercise a week are 32 % less likely to conceive than those who keep activity moderate. Research shows that while regular exercise supports overall health and reproductive function, excessive training, especially at high intensity or duration can disrupt the delicate hormonal balance needed for conception. Overtraining may lower testosterone, reduce semen quality, and even damage sperm DNA, all of which can decrease your chances of starting a family.
For people of all genders, the relationship between physical activity and fertility is complex. Moderate exercise often benefits fertility, but too much can have the opposite effect, particularly in men. Studies suggest that the impact depends on how much, how hard, and how often you train, as well as your individual health status. Recognizing warning signs of overtraining such as persistent fatigue, mood changes, or changes in menstrual or sexual health, can help you protect your reproductive well-being.
If you’re working out intensely and struggling with fertility, you are not alone. Listening to your body and seeking guidance from healthcare professionals can help you find the right balance between fitness and fertility.
- What counts as overtraining when you’re trying to conceive?
- How is “overtraining” defined for future parents?
- How do you separate vigorous from moderate activity?
- Does “too much” differ for certain groups?
- How does overtraining disrupt reproductive hormones in women and men?
- What chain reaction knocks hormones off course?
- What happens in women?
- What happens in men?
- Which fertility considerations are missing from most overtraining advice?
- Are men being left out of the conversation?
- What about non-binary or transgender athletes?
- Is resistance training risky?
- Where’s the self-assessment tool?
- What early warning signs tell you it’s time to scale back?
- Can overtraining cause missed periods?
- Physical cues to watch
- Psychological cues
- How can you redesign your routine to stay in the fertility “sweet spot”?
- What weekly rhythm supports conception?
- How much should you eat on hard days?
- How do you monitor real-time stress?
- Ready to return after OTS?
- Your top questions, answered
- Final thoughts
- References
What counts as overtraining when you’re trying to conceive?
How is “overtraining” defined for future parents?
Overtraining is defined as exercising at a level where your body cannot recover adequately, leading to negative effects on your health and fertility. For those trying to conceive, this means training with excessive intensity, duration, or frequency, without enough rest. Overtraining disrupts the balance between training and recovery, causing hormonal imbalances, chronic fatigue, mood changes, and reduced reproductive function. In men, it can lower testosterone and semen quality; in women, it may disrupt ovulation and menstrual cycles. Key warning signs include persistent tiredness, declining performance, and changes in sexual or menstrual health.
For most people TTC, moderate movement like brisk walking, swimming, light strength work lands squarely in the “fertility-friendly” zone. See how to dial that in at Exercise vs. Fertility: Finding the Sweet Spot.
How do you separate vigorous from moderate activity?
Vigorous activity is exercise that significantly raises your heart rate and breathing, such as running, intense cycling, or competitive sports. You can usually only say a few words before needing to breathe. Moderate activity, like brisk walking or gentle cycling, raises your heart rate but still allows you to talk comfortably. The distinction is important because moderate exercise supports fertility, while excessive vigorous activity can harm it, especially if recovery is insufficient.
Use the talk test and wearable data:
- Moderate: You can speak full sentences; heart rate ~50–70 % of max (3–6 METs).
- Vigorous: Only 1–2 words at a time; heart rate > 70 % of max (≥6 METs).
Tracking tools covered in our Wearable Fitness Guide help you spot creeping intensity before it crosses the line.
Does “too much” differ for certain groups?
Yes, what counts as “too much” varies by individual. Factors like your baseline fitness, health status, age, and previous exercise habits all play a role. People with underlying health conditions, those new to exercise, or those with a history of reproductive issues may be more sensitive to overtraining’s negative effects. Men and women may also experience different impacts, with men more likely to see reduced testosterone and semen quality, and women more likely to have disrupted menstrual cycles. Tailoring your exercise routine to your unique needs and watching for warning signs is essential for protecting fertility.
How does overtraining disrupt reproductive hormones in women and men?
What chain reaction knocks hormones off course?
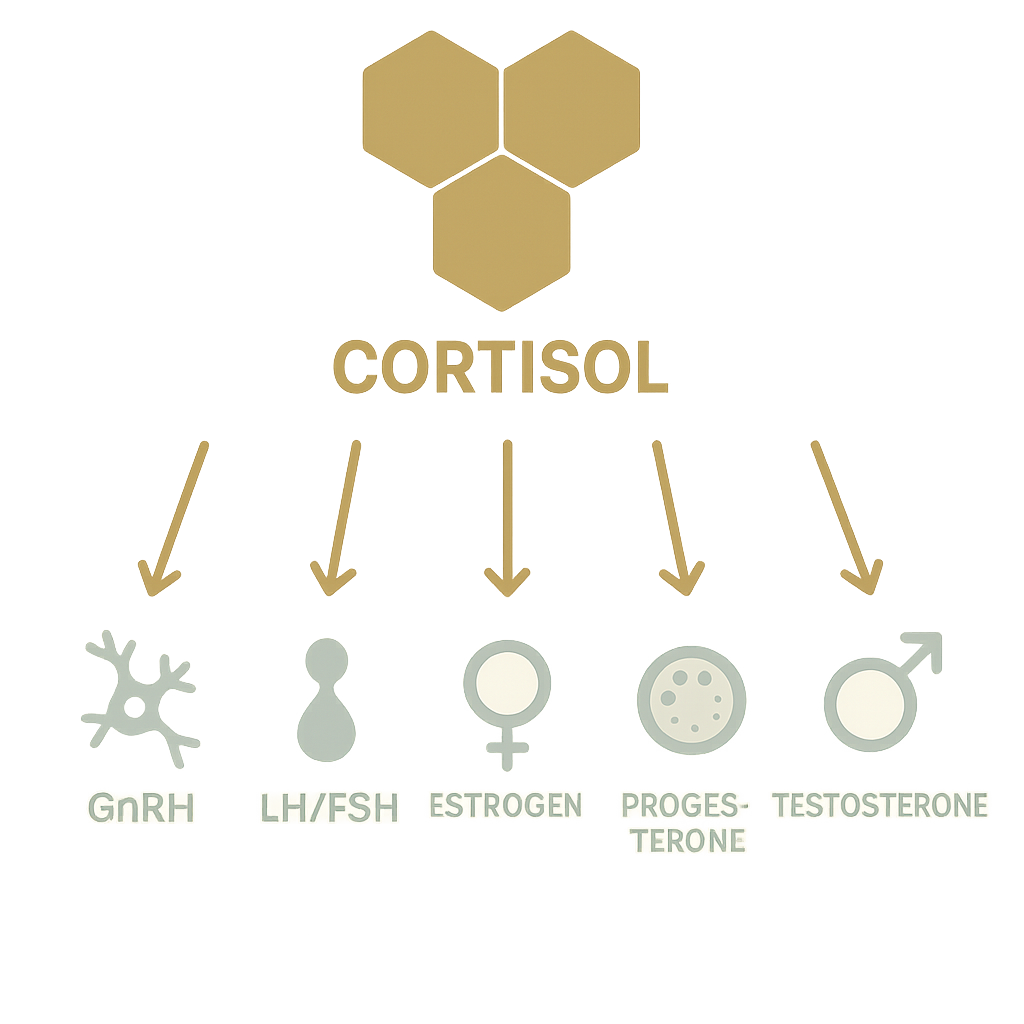
Overtraining triggers a stress response in your body, activating the hypothalamic-pituitary-adrenal (HPA) axis. This leads to increased production of stress hormones like cortisol, which can suppress the hypothalamic-pituitary-gonadal (HPG) axis—the system that regulates reproductive hormones. As a result, the normal signaling that controls the release of sex hormones (such as estrogen, progesterone, and testosterone) is disrupted, leading to hormonal imbalances that can impair fertility in both women and men.
The fallout:
- Cortisol ↑ → GnRH ↓
- LH/FSH ↓ → Estrogen & Progesterone ↓ in women
- LH ↓ → Testosterone ↓ in men
The medical term is functional hypothalamic dysfunction, often bundled into RED-S (Relative Energy Deficiency in Sport).
What happens in women?
In women, overtraining can disrupt the balance of hormones that regulate the menstrual cycle. High levels of physical stress and low energy availability may suppress the release of gonadotropin-releasing hormone (GnRH), which in turn reduces levels of luteinizing hormone (LH) and follicle-stimulating hormone (FSH). This can lead to irregular or absent periods (amenorrhea), anovulation (lack of ovulation), and lower estrogen levels, all of which can make it harder to conceive. Women with underlying conditions like polycystic ovary syndrome (PCOS) may be especially sensitive to these disruptions.
Amenorrhea or irregular cycles: Competitive runners experience menstrual disturbances at much higher rates than sedentary women. A recent comparative study found that amenorrhea and irregular cycles are common among highly trained female runners, while these issues are rare in sedentary controls. Reviews confirm that secondary amenorrhea and other menstrual dysfunctions, such as luteal phase defects and delayed menarche, are significantly more prevalent in athletes than in the general population. This highlights the strong association between high training loads and menstrual irregularities in female athletes.
Luteal-phase defects: Luteal phase deficiency (LPD) is also frequently observed in active women, even those who continue to menstruate regularly. In a study of recreational runners, a substantial proportion of menstrual cycles in exercising women were classified as luteal phase deficient, compared to sedentary controls. These women exhibited hormonal changes consistent with a hypometabolic state, likely due to intermittent negative energy balance from training and inadequate calorie intake. LPD can occur without obvious symptoms, making it an important but often overlooked concern for active women.
Implantation trouble: Low progesterone, often a result of luteal phase defects or amenorrhea, can compromise the uterine lining and make implantation more difficult. Studies have found that amenorrheic runners and those with LPD have significantly lower plasma progesterone levels than regularly menstruating athletes or sedentary controls, which may impair the endometrial environment needed for successful implantation. This hormonal disruption underscores the importance of adequate nutrition and balanced training for reproductive health in active women.
Learn how to sync workouts with your menstrual phases in Cycle-Smart Workouts.
What happens in men?
In men, overtraining can lower testosterone production and disrupt the balance of other reproductive hormones. This hormonal imbalance can reduce sperm production, decrease semen quality, and even damage sperm DNA. Chronic excessive exercise may also increase oxidative stress and inflammation, further impairing fertility. While moderate exercise supports healthy hormone levels and sperm quality, consistently pushing beyond your body’s recovery limits can have the opposite effect.
Sperm decline: A major 2022 meta-analysis including U.S. data found that sperm concentration among men in North America including the USA, declined by over 50% between 1973 and 2018, with the rate of decline accelerating after 2000. However, studies specifically examining the immediate effects of overtraining on sperm count in U.S. men are limited. Research does show that overtraining is linked to poorer semen quality, such as reduced sperm motility and increased abnormal sperm, as well as lower testosterone, but not always a significant drop in sperm concentration. Overall, while a dramatic, acute drop in sperm count after overtraining.
Low libido & mood dips: Testosterone is central to male reproductive health, influencing libido, mood, and overall well-being. Systematic reviews from 2025 highlight that low testosterone is associated with reduced sexual desire, erectile dysfunction, and mood disturbances such as depression. Overtraining can suppress testosterone levels, which in turn may lead to hallmark symptoms like low libido and mood dips, underscoring the importance of hormonal balance for both mental and sexual health in men.
Proper recovery tips are covered in Post-Workout Recovery: Tips for TTC Parents.
Which fertility considerations are missing from most overtraining advice?
Key fertility considerations often missing from most overtraining advice include:
- Effects on male fertility, such as reduced sperm quality and testosterone levels.
- Impact on non-binary and transgender athletes, whose unique hormonal and medical needs are rarely addressed.
- The role of diet and nutrition in supporting or impairing fertility during intense training.
- Risks of overtraining for people with overweight or obesity, and how weight loss interventions may affect reproductive outcomes.
- Lack of clear, evidence-based recommendations on exercise frequency and intensity for optimal fertility.
- Absence of practical self-assessment tools to help you monitor warning signs like missed periods, low libido, or mood changes.
- Limited discussion of how overtraining may interact with other lifestyle factors, such as work stress or sleep, to influence fertility.
- Insufficient focus on both partners’ health in couples trying to conceive, rather than just one individual.
Addressing these gaps can help you make more informed, inclusive, and practical decisions about your training and reproductive health.
Are men being left out of the conversation?
Yes, men are often left out of the conversation on overtraining advice and fertility. Most research and public guidance have historically focused on women, even though male infertility accounts for about half of all infertility cases. Recent systematic reviews highlight that excessive or intense training can significantly reduce sperm quality, testosterone, and overall reproductive health in men, but these risks are rarely addressed in mainstream overtraining advice. For example, a 2025 review found that 16 weeks of intensive cycling led to lower sperm concentration, motility, and morphology, with only partial recovery after rest. Experts emphasize that moderate exercise benefits male fertility, but overtraining can cause hormonal disruption and oxidative stress, directly harming sperm and reproductive function. Despite these findings, men often do not receive targeted, practical guidance on how to balance training and protect fertility. You deserve advice that recognizes and addresses these specific risks.
What about non-binary or transgender athletes?
Non-binary and transgender athletes face unique fertility considerations that are often missing from mainstream overtraining and fertility advice. Gender-affirming hormone therapy and surgeries can significantly impact your future fertility, sometimes making it difficult or impossible to have genetic children without prior fertility preservation. Many athletes are not fully informed about these risks or the available options, such as egg or sperm freezing, before starting treatment. Barriers include high costs, lack of inclusive counseling, and limited research on long-term outcomes for non-binary and transgender individuals. Only a small percentage of transgender and non-binary people are offered or can access fertility preservation, even though most believe it should be available to all. Inclusive, individualized counseling and early discussions about fertility are essential so you can make informed decisions that align with your goals and identity. As one review notes, “inclusive health systems that provide comprehensive reproductive health care to transgender individuals can help them make informed decisions about fertility preservation and improve their quality of life”.
Is resistance training risky?
Resistance training is generally not risky for fertility and, in fact, can offer significant benefits when performed at appropriate intensity and with adequate recovery. In men, regular resistance exercise has been shown to reduce inflammation and oxidative stress, improve semen quality, enhance sperm DNA integrity, and increase pregnancy rates, especially in those with infertility issues. For women, resistance training during pregnancy is considered safe and can improve maternal health, support glucose control, and even benefit fetal development, provided certain precautions are taken (such as avoiding exercises that risk abdominal trauma or overheating). However, the best outcomes for male fertility are often seen with a combination of aerobic and resistance training rather than resistance training alone. For women, the menstrual cycle and contraceptive use may influence how the body responds to resistance training, but current evidence does not suggest major risks to fertility. Overall, resistance training is safe and beneficial for reproductive health when balanced with proper nutrition, rest, and individualized adjustments.
Research is thin, but balanced lifting programs like those in Strength Training: Build Muscle Without Harming Fertility—show neutral or positive hormone effects when paired with adequate calories.
Where’s the self-assessment tool?
Few resources offer self-assessment tools for tracking fertility risks from overtraining. You should have access to checklists or digital tools to monitor changes in your cycle, libido, or mood. Early detection helps you seek help before problems worsen. The Centers for Disease Control and Prevention (CDC) recommends regular health check-ins if you are concerned about your reproductive health.
Try the Fertility-Fuel Score:
Daily calories eaten – Estimated workout calories burned
Aim for a score ≥ 0 on most days. If you dip negative repeatedly, use the Low-Impact Workout Calendar to reset volume.
What early warning signs tell you it’s time to scale back?
Can overtraining cause missed periods?
Yes, overtraining can cause missed periods, a condition known as exercise-induced or functional hypothalamic amenorrhea. The primary mechanism is low energy availability: when the body expends more energy through exercise than it receives from food, it triggers a stress response that disrupts the normal release of gonadotropin-releasing hormone (GnRH) from the hypothalamus. This disruption leads to reduced secretion of luteinizing hormone (LH) and follicle-stimulating hormone (FSH), which are essential for ovulation and regular menstrual cycles. As a result, estrogen and progesterone levels drop, menstrual cycles become irregular, and periods may stop altogether.
The transition to amenorrhea can be abrupt, often preceded by subtle changes such as longer cycles or lighter periods before menstruation ceases completely. Psychological and physical stress, as well as inadequate nutrition, can further exacerbate this effect by increasing stress hormones like corticotropin-releasing hormone (CRH), which also suppress reproductive hormone signaling. Importantly, restoring energy balance; either by reducing exercise intensity or increasing caloric intake can often reverse amenorrhea and restore normal menstrual function within weeks to months. Chronic amenorrhea is not only a sign of reproductive dysfunction but also increases the risk of bone loss, cardiovascular issues, and other long-term health problems if left unaddressed.
Physical cues to watch
Look for ongoing:
- Persistent fatigue that does not improve with rest
- Decreased athletic performance or endurance
- Prolonged muscle soreness and slower recovery from workouts
- Increased frequency of illnesses or infections, due to weakened immunity
- Disrupted or poor-quality sleep
- Loss of appetite or reduced food intake
- Unexplained changes in body composition, such as loss of muscle or increased body fat
- Slowed growth (in younger athletes) or stunted physical progress
- Elevated markers of inflammation in the body (such as increased cytokines)
Psychological cues
Be alert for:
- Mood disturbances, including increased irritability, anger, or emotional instability
- Loss of motivation or enthusiasm for training
- Feelings of depression, sadness, or hopelessness
- Heightened anxiety or restlessness
- Cognitive difficulties, such as poor concentration, indecisiveness, or slower reaction times
- Increased impulsivity or poor decision-making
- A sense of “burnout” or indifference toward training and competition
- Social withdrawal or reduced interest in activities outside of sport
During high-anxiety stretches like the two-week wait, switch to calming routines in Two-Week Wait Workouts: Gentle Moves to Calm the Mind.
How can you redesign your routine to stay in the fertility “sweet spot”?
To support fertility, aim for a balanced exercise routine that emphasizes moderate intensity and avoids extremes. Both men and women benefit from regular, moderate aerobic and resistance training, which improves hormonal balance, reduces inflammation, and supports reproductive health, while excessive or intense training can disrupt hormones and impair fertility. Include rest days and vary your workouts to prevent chronic stress and overtraining, and consider incorporating relaxation techniques like yoga or meditation to further reduce stress and support hormonal health. Individualize your routine based on your health status, fitness level, and fertility goals, and consult with a healthcare provider if you have specific concerns.
What weekly rhythm supports conception?
A weekly exercise rhythm that supports conception emphasizes moderate, consistent activity while avoiding extremes.
The most widely recommended pattern is at least 150 minutes of moderate-intensity aerobic exercise per week, spread over at least three days, such as brisk walking, cycling, or swimming. Moderate exercise 3–4 times weekly appears safe and effective for reproductive health, while increasing frequency beyond five sessions per week does not show additional benefits and may even have drawbacks. Each session should last less than an hour, and both aerobic and resistance (strength) training are beneficial, either alone or in combination. Intensity should be moderate—enough to raise your heart rate and make you breathe faster, but not so hard that you can’t hold a conversation.
Using both the Borg Rating of Perceived Exertion (RPE) scale and heart rate monitoring can help ensure you stay in the right intensity zone. It’s also important to include at least one or two rest or active recovery days each week to allow for recovery and hormonal balance. Overly frequent or intense exercise (such as daily vigorous workouts) may disrupt menstrual cycles and reduce fertility, so moderation and variety are key. Finally, individual factors like age, body composition, and previous activity levels can influence the ideal routine, so adjustments may be needed for your personal situation.
Sprinkle in the calming poses from Yoga for Fertility.
How much should you eat on hard days?
On hard training days, it’s crucial to eat enough to match your increased energy needs and support both recovery and fertility. This means increasing your total calorie intake, with a focus on high-quality carbohydrates to replenish glycogen stores, healthy fats (especially omega-3s), and adequate protein to repair muscle and maintain hormonal balance. Undereating or having a significant calorie deficit; even for a few days can disrupt the delicate hormonal signals that regulate ovulation and menstrual cycles, increasing the risk of fertility problems.
Aim to include whole grains, fruits, vegetables, lean proteins, nuts, seeds, and healthy oils in your meals, and avoid trans fats, excessive added sugars, and highly processed foods, which are linked to poorer fertility outcomes. Hydration is also important, as dehydration can add to physical stress. On especially demanding days, consider eating a balanced meal or snack both before and after exercise to ensure your body has the fuel it needs for performance and recovery. If you’re unsure about your specific needs, a sports dietitian can help tailor your nutrition plan to your training and fertility goals.
How do you monitor real-time stress?
Real-time stress can be monitored using a combination of subjective self-assessment and objective physiological measures.
- Self-report tools, such as daily diaries or validated questionnaires like the State-Trait Anxiety Inventory, allow individuals to track perceived stress levels, mood changes, and coping strategies on a regular basis.
- For more objective monitoring, salivary biomarkers, especially alpha-amylase and cortisol can be measured; elevated alpha-amylase, in particular, has been linked to reduced probability of conception during the fertile window, making it a useful indicator of stress that may impact fertility.
- Wearable devices that track heart rate variability (HRV), sleep quality, and resting heart rate can also provide real-time feedback on physiological stress responses, as disruptions in these patterns often reflect increased stress load.
- Monitoring menstrual cycle regularity and symptoms can serve as an additional, indirect marker of chronic stress affecting reproductive health.
Combining these approaches; subjective ratings, biomarker testing, and wearable data offers a comprehensive picture of real-time stress and its potential impact on fertility, enabling timely adjustments to lifestyle or training routines.
Ready to return after OTS?
Returning to training after Overtraining Syndrome (OTS) requires a cautious, gradual approach to avoid relapse and support full recovery. Recovery from OTS often takes 6–12 weeks or longer, depending on the severity and individual factors, and symptoms may persist or recur if training is resumed too soon. The first step is complete rest or very light activity, focusing on sleep, nutrition, hydration, and psychological support to restore physical and mental health. Once symptoms like fatigue, mood disturbances, and underperformance have resolved, reintroduce mild aerobic activities, gentle stretching, and relaxation techniques such as massage or hot/cold baths.
Training volume and intensity should be increased very slowly, with careful monitoring for any return of symptoms. Objective measures such as performance tests, heart rate, and mood tracking can help guide safe progression. Coaches and athletes should prioritize recovery strategies, including adequate sleep, balanced nutrition, and stress management, throughout the return process. If symptoms reappear, reduce training load immediately and allow more time for recovery. Collaboration with healthcare professionals or sports medicine specialists is recommended to individualize the return-to-play plan and ensure long-term health.
Runners can phase in mileage using the steps in Running While TTC: Safe Guidelines for Runners.
Your top questions, answered
Can overtraining alone make me infertile?
Overtraining especially prolonged, high-intensity endurance exercise can temporarily worsen fertility by disrupting hormone levels and reducing semen quality in men, and by affecting menstrual cycles in women. However, infertility from overtraining is usually reversible; most studies show that semen parameters and reproductive function improve after reducing training load or taking a rest period of several weeks to months 14. Complete, permanent infertility from overtraining alone is rare.
Does overtraining affect male fertility?
Yes, intense and sustained training can negatively impact male fertility by lowering sperm count, motility, and morphology, and increasing DNA fragmentation and inflammation. However, moderate exercise or combined aerobic and resistance training can actually improve semen quality and pregnancy rates, so the effect depends on the intensity and duration of training.
How fast can fertility rebound after I scale back?
Improvements in semen parameters and fertility can be seen within 1–4 weeks after reducing or stopping intense training, with further gains over several months. Some changes, like sperm concentration and motility, may take longer to fully recover, especially if overtraining was prolonged.
Is complete rest better than moderate exercise?
No, complete rest is not better for fertility than moderate exercise. Regular, moderate-intensity exercise is associated with improved reproductive health and higher pregnancy rates, while both inactivity and excessive training can be detrimental. The best approach is a balanced, moderate exercise routine.
What’s a simple self-check each month?
For men, a simple monthly self-check includes monitoring energy levels, libido, and, if possible, semen quality (through home test kits or clinical analysis). For women, tracking menstrual cycle regularity and ovulation is key. Both should watch for signs of overtraining, such as persistent fatigue, mood changes, or performance decline, and adjust training accordingly.
Final thoughts
Overtraining can negatively impact fertility, but its effects are typically reversible with appropriate changes in exercise habits. Excessive training, especially at high intensity or volume, can disrupt hormonal regulation, damage sperm DNA, and reduce sperm activity in men, leading to decreased reproductive potential. In women, overtraining is known to cause menstrual irregularities and ovulatory dysfunction, which can also impair fertility. However, moderate, regular physical activity is generally beneficial for reproductive health, improving hormone balance and semen quality, and supporting overall well-being.
The key is moderation: while too little activity can be harmful, so can too much. If overtraining is suspected, reducing training load and prioritizing recovery often leads to improvements in fertility within weeks to months. Monitoring for signs of overtraining and maintaining a balanced approach to exercise are essential for protecting reproductive health. Ultimately, a lifestyle that includes moderate exercise, good nutrition, and stress management offers the best support for fertility in both men and women.
References
-
Energy expenditure and slow-wave sleep in runners: Focusing on reproductive function, chronic training, and sex. iScience, 28. https://doi.org/10.1016/j.isci.2024.111717
-
Temporal trends in sperm count: a systematic review and meta-regression analysis of samples collected globally in the 20th and 21st centuries… Human reproduction update. https://doi.org/10.1093/humupd/dmac035
-
Impact of Testosterone on Male Health: A Systematic Review. Cureus, 17. https://doi.org/10.7759/cureus.82917
-
The Influence of an Intense Training Regime in Professional and Non-Professional Athletes on Semen Parameters: A Systematic Review. Journal of Clinical Medicine, 14. https://doi.org/10.3390/jcm14010201
-
The Impact of Physical Exercise on Male Fertility Through Its Association with Various Processes and Aspects of Human Biology. Journal of Clinical Medicine, 14. https://doi.org/10.3390/jcm14103442
-
Clinical management of transgender and non-binary patients in the fertility preservation service: Current evidence… International journal of transgender health, 25 4, 663-680. https://doi.org/10.1080/26895269.2023.2284775
-
Benefits of Resistance Training During Pregnancy for Maternal and Fetal Health: A Brief Overview. International Journal of Women’s Health, 16, 1137 - 1147. https://doi.org/10.2147/IJWH.S462591
-
Unlocking Female Fertility with a Specific Reproductive Exercise Program: Protocol of a Randomized Controlled Clinical Trail. Life, 15. https://doi.org/10.3390/life15010018
-
The Current Landscape of Exercise and Female Fertility Research: A Narrative Review… Reproduction. https://doi.org/10.1530/rep-22-0317
-
Stress, kisspeptin, and functional hypothalamic amenorrhea… Current opinion in pharmacology, 67, 102288. https://doi.org/10.1016/j.coph.2022.102288