You are not alone if you feel uncertain about when and how an embryo implants. Even with advances in fertility care, human reproduction remains surprisingly inefficient—only about 15% of cycles result in pregnancy, in part because implantation is such a delicate, complex process. Understanding the timeline can help you feel more informed and empowered as you navigate your fertility journey.
84 % of successful pregnancies implant within a narrow “window” about 7 to 10 days after ovulation, when your uterus becomes receptive to the embryo. During this time, the embryo and your endometrium communicate through a series of signals, allowing the embryo to attach, invade, and begin forming the placenta. This process unfolds in distinct stages—apposition, adhesion, and invasion—each requiring precise coordination between your body and the developing embryo.
Knowing the day-by-day steps of implantation can validate your concerns and help you understand why timing and synchrony matter so much for successful pregnancy. If you are undergoing fertility treatment or tracking your cycle, this knowledge can guide your expectations and support your emotional well-being.
- How does an embryo travel from fertilization to the uterus in the first 5 days?
- What happens in the fallopian tube right after fertilization?
- When does the blastocyst “hatch” and why is it important?
- How exactly does attachment unfold between Days 6 and 10?
- What are apposition, adhesion, and invasion?
- Is the timeline different for IVF?
- Why do some embryos implant and others don’t—and can you tip the odds?
- Which factors matter most?
- What lifestyle choices actually help?
- How can you know implantation happened, and when should you test?
- Are symptoms reliable?
- When is the earliest accurate pregnancy test?
- Implantation bleeding vs. period—how can you tell?
- What daily actions support implantation during the “window”?
- Day-by-day checklist
- Evidence hierarchy (quick guide)
- Your Implantation FAQs, Answered Fast
- Final Thoughts
- References
How does an embryo travel from fertilization to the uterus in the first 5 days?
After fertilization in the ampulla of your fallopian tube, the embryo begins a carefully timed journey toward your uterus. This movement relies on two main forces: the rhythmic beating of cilia (tiny hair-like structures) lining the tube and the coordinated contractions of the smooth muscle wall, called the myosalpinx. Estrogen plays a key role by regulating ciliary function and muscle contractions, ensuring the embryo moves at the right pace. The embryo spends several days in the tube, dividing and developing as it travels. Secretions and extracellular vesicles from the tube’s lining provide nutrients and signals that support the embryo’s growth and protect it from harm. The journey is precisely controlled—if the embryo moves too slowly or too quickly, it can lead to problems like ectopic pregnancy or failed implantation.
What happens in the fallopian tube right after fertilization?
Right after fertilization, your embryo is still a single cell, called a zygote. It remains in the ampulla for a short time, where it begins to divide. The fallopian tube provides a nurturing environment, with secretions that protect the embryo and help it develop. Cilia and muscle contractions gently move the embryo toward the uterus, while the tube’s environment prevents it from implanting too early. Specialized pacemaker cells in the tube coordinate these contractions, and hormonal signals; especially from estrogen—fine-tune the process. The embryo continues to divide, becoming a multicellular structure as it approaches the uterus.
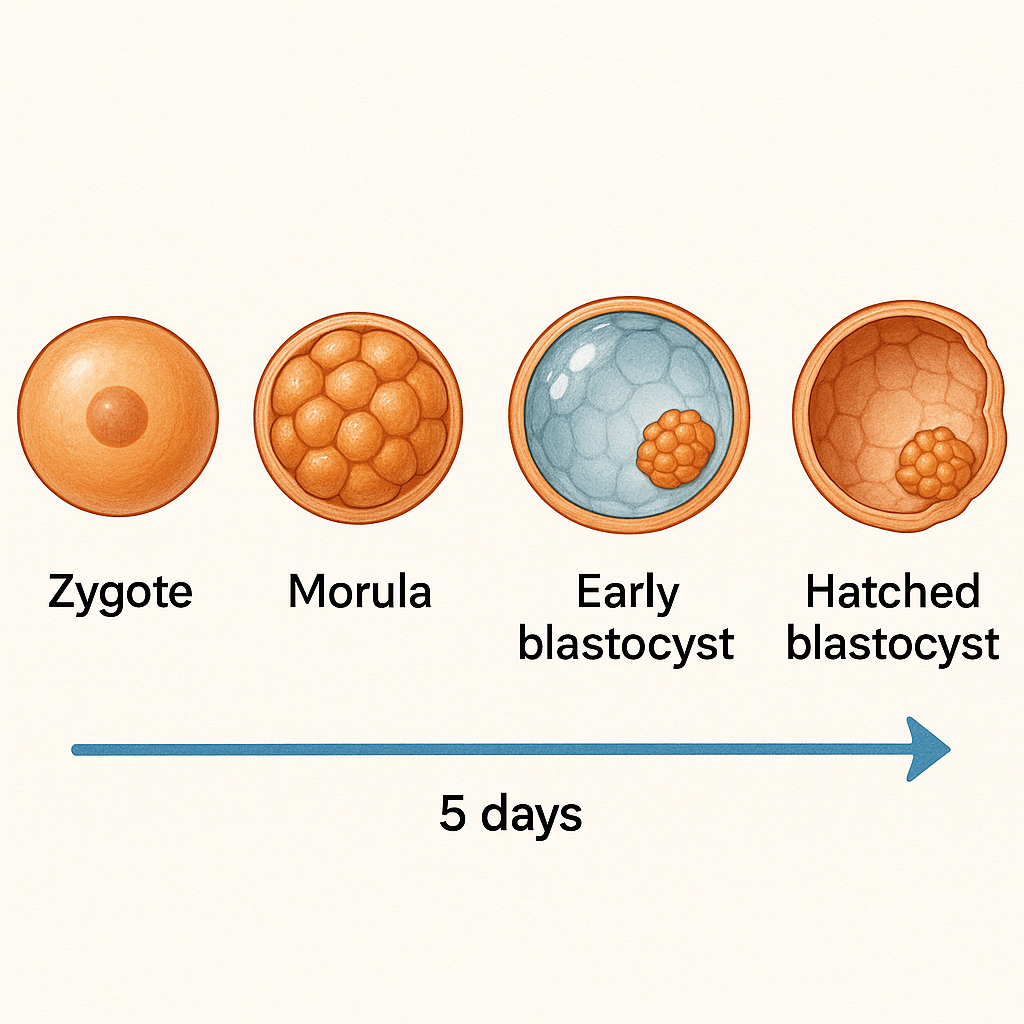
When does the blastocyst “hatch” and why is it important?
By day 5, your embryo has developed into a blastocyst, a hollow ball of cells. Before it can implant, the blastocyst must “hatch” from its protective shell, the zona pellucida. Hatching usually occurs just before or as the blastocyst enters the uterus. This step is crucial because only a hatched blastocyst can attach to the uterine lining and begin the process of implantation. If hatching does not occur, the embryo cannot implant, and pregnancy will not progress. Proper timing of hatching ensures the embryo is ready to interact with the uterine environment at the optimal moment for successful implantation.
| Embryo Age | Key Event | Natural Cycle | IVF Cycle (Day-5 Transfer) |
|---|---|---|---|
| Day 0 | Fertilization & zygote | Ovulation day | Retrieval/ICSI day |
| Day 3 | Morula (16–32 cells) | Still in tube | In lab dish |
| Day 5 | Hatched blastocyst | Enters uterus | Transferred to uterus |
Curious why timing intercourse matters long before implantation? See Egg vs. Sperm Lifespan: Timing Sex for Best Results.
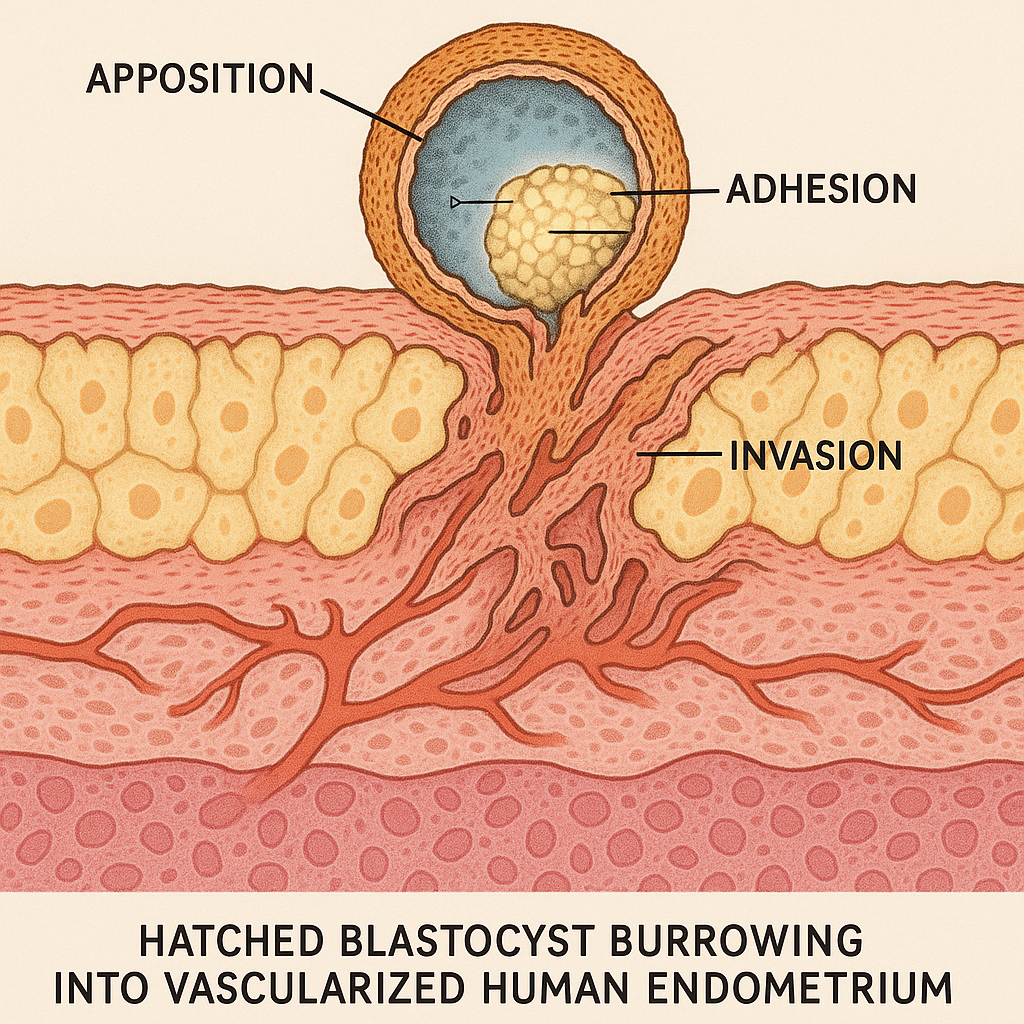
How exactly does attachment unfold between Days 6 and 10?
Between days 6 and 10 after fertilization, the process of embryo attachment to your uterus occurs in three main stages: apposition, adhesion, and invasion. First, during apposition, the blastocyst loosely aligns with the endometrial lining, finding the optimal spot for implantation. Next, in adhesion, the blastocyst forms stronger, more stable bonds with the endometrial cells, anchoring itself securely. Finally, during invasion, the outer cells of the blastocyst (trophoblasts) penetrate the endometrial surface, allowing the embryo to embed within the uterine lining and begin forming the placenta. This entire sequence is tightly regulated by your hormones, especially estrogen and progesterone, which prepare the endometrium to be receptive during this short “window” of implantation.
What are apposition, adhesion, and invasion?
Apposition is the initial, loose contact between the blastocyst and the endometrial surface, where the embryo “positions” itself at the most favorable site. Adhesion follows, with the blastocyst establishing firmer connections to the endometrial cells through molecular interactions, ensuring it stays in place. Invasion is the final step, where the trophoblast cells of the blastocyst actively penetrate the endometrial tissue, embedding the embryo and initiating the development of the placenta. Each stage is essential for successful implantation and pregnancy.
Is the timeline different for IVF?
The timeline for attachment can differ with IVF, as the timing of embryo transfer is carefully matched to your endometrial receptivity, often using hormone treatments to mimic a natural cycle. In natural cycles, apposition typically starts around day 6 after ovulation and is usually complete by day. With IVF, research shows that transferring blastocysts on day 5 after fertilization generally leads to higher implantation rates than day 6 transfers, likely because synchrony between embryo development and endometrial readiness is critical. Some clinics use personalized tests to pinpoint your unique window of receptivity, further optimizing the timing for embryo transfer and improving outcomes.
| Stage | Natural Cycle (DPO) | IVF Cycle (DPET) |
|---|---|---|
| Apposition | 6–7 | 1–2 |
| Adhesion | 7–8 | 2–3 |
| Invasion / Complete | 8–10 | 3–5 |
Learn how the uterine lining gets baby-ready in Uterine Environment 101.
Why do some embryos implant and others don’t—and can you tip the odds?
Implantation success depends on both the quality of the embryo and the receptivity of your endometrium. The most critical factor is whether the embryo is chromosomally normal (euploid); embryos with genetic abnormalities are much less likely to implant, regardless of other conditions. The timing and quality of blastocyst hatching, as well as the embryo’s ability to communicate with your immune system, also play major roles. On the uterine side, a receptive endometrium; properly prepared by hormones and free from inflammation or infection is essential for the embryo to attach and invade. The interaction between the embryo and endometrium involves a complex exchange of signals, including hormones, cytokines, and growth factors, which must be precisely synchronized. Age is another key factor; as you get older, both egg quality and endometrial receptivity tend to decline, making implantation less likely. While some extraembryonic factors (like the uterine microbiome or immune environment) can influence outcomes, their impact is generally smaller than that of embryo quality. Techniques like preimplantation genetic testing (PGT-A) and careful timing of embryo transfer can help tip the odds in your favor.
Which factors matter most?
The most important factors for implantation are:
- Embryo chromosomal normality (euploidy), endometrial receptivity, and precise timing of embryo transfer.
- Embryo quality, especially at the genetic and molecular level, is the strongest predictor of success.
- The endometrium must be hormonally primed and free from inflammation or infection, and the window of implantation must be accurately identified.
- Age, both of the egg provider and gestational carrier, also significantly affects outcomes.
- Technical aspects of embryo transfer such as avoiding trauma, contamination, or excessive uterine contractions can further influence success rates
What lifestyle choices actually help?
While lifestyle cannot change embryo genetics, certain choices can support your fertility and endometrial health.
- Maintaining a healthy weight, eating a balanced diet rich in antioxidants, and avoiding smoking and excessive alcohol can improve both egg quality and uterine environment.
- Managing stress, getting regular exercise, and ensuring adequate sleep may also support hormonal balance and immune function, which are important for implantation.
- Avoiding exposure to environmental toxins and following your healthcare provider’s recommendations for supplements (like folic acid) can further optimize your chances.
- If you are undergoing IVF, following medical advice on timing and preparation is crucial for maximizing implantation success
Deep dive basics in Fertility 101: A Step-by-Step Guide.
How can you know implantation happened, and when should you test?
Implantation itself is a silent process and cannot be directly detected at home. In clinical research, scientists are exploring molecular biomarkers such as specific proteins, microRNAs, and cytokines in blood or uterine fluid, that may signal successful implantation, but these are not yet available for routine use. For most people, the first reliable sign of implantation is a rise in the pregnancy hormone hCG (human chorionic gonadotropin), which is produced after the embryo embeds in the uterine lining 13. This hormone is what pregnancy tests detect.
Are symptoms reliable?
Symptoms like light spotting, mild cramping, breast tenderness, or fatigue are often reported around the time of implantation, but they are not reliable indicators. These symptoms can be caused by normal hormonal changes in your cycle or by the onset of your period, and studies show that there is no consistent, specific symptom pattern that confirms implantation. Most people who become pregnant do not notice any distinct symptoms at the time of implantation.
When is the earliest accurate pregnancy test?
The earliest accurate pregnancy test is a sensitive blood test for hCG, which can detect pregnancy about 8–10 days after ovulation or fertilization; sometimes as early as 6–8 days post-ovulation, but accuracy improves with time. Home urine pregnancy tests are most reliable from the first day of your missed period, which is typically about 12–14 days after ovulation. Testing too early can lead to false negatives because hCG levels may not yet be high enough to detect.
Implantation bleeding vs. period—how can you tell?
Implantation bleeding, if it occurs, is usually lighter and shorter than a normal period. It may appear as light spotting or pinkish/brown discharge and typically happens 6–12 days after ovulation, around the time your period would be due. In contrast, a menstrual period is heavier, lasts longer, and follows your usual cycle pattern. However, not everyone experiences implantation bleeding, and it can be easily confused with a light period or other spotting, so it is not a reliable way to confirm implantation or pregnancy. The only definitive way to know is with a positive pregnancy test after a missed period.
| Feature | Implantation | Period |
|---|---|---|
| Color | Pink / brown | Bright to dark red |
| Flow | Spotting only | Light to heavy |
| Duration | Few hours–2 days | 3–7 days |
| Clots | None | Common |
Your luteal hormones keep everything on track—learn more in The Luteal Phase: Why It Drives Conception Success.
What daily actions support implantation during the “window”?
Day-by-day checklist
The most effective daily actions to support embryo implantation during the “window” (days 6–10 after ovulation or embryo transfer) are those that optimize hormonal support and endometrial receptivity.
- If you are undergoing IVF or frozen embryo transfer, strictly follow your prescribed hormone regimen—especially progesterone, which is essential for preparing the uterine lining.
- Evidence shows that oral dydrogesterone (30 mg/day) or a combination of dydrogesterone and vaginal progesterone gel can significantly increase clinical pregnancy and live birth rates compared to vaginal progesterone gel alone.
- Higher doses of vaginal progesterone (800 mg/day) are more effective than lower doses (600 mg/day) for luteal phase support.
- Both daily intramuscular progesterone and vaginal progesterone gel (sometimes combined with weekly intramuscular injections) are effective, with no significant difference in live birth or implantation rates between these regimens.
- For fresh embryo transfers, intramuscular progesterone may be more effective than vaginal gel alone.
- Beyond medication, maintain a healthy, balanced diet, stay hydrated, avoid smoking, alcohol, and excessive caffeine, and engage in gentle physical activity while avoiding strenuous exercise or overheating.
- Prioritize adequate sleep and manage stress, as these support hormonal and immune function.
- Take any prescribed supplements, such as folic acid, daily, and avoid unapproved medications or herbal remedies.
- Attend all scheduled monitoring appointments and promptly report any unusual symptoms to your care team.
Evidence hierarchy (quick guide)
High-certainty help:
- Ultrasound-guided, soft-catheter embryo transfer: Strong evidence shows that using ultrasound guidance and a soft catheter during embryo transfer improves implantation and pregnancy rates by minimizing trauma and ensuring precise placement.
- Hyaluronic-acid–enriched transfer media: Adding hyaluronic acid to the embryo transfer medium has been shown in randomized trials and meta-analyses to modestly increase implantation and live birth rates, likely by enhancing embryo–endometrial interaction.
- Personalized embryo selection (including preimplantation genetic testing and algorithm-based selection): Selecting embryos based on genetic screening (PGT-A) or advanced ranking algorithms improves implantation rates and ongoing pregnancy outcomes, especially in single embryo transfers.
- Optimized endometrial preparation and timing: Careful synchronization of embryo development and endometrial receptivity, including the use of milder ovarian stimulation and natural or hormone-prepared cycles, is supported by strong evidence to improve outcomes.
Moderate-certainty or promising (needs more research):
- Intrauterine PBMC infusion, subcutaneous G-CSF, and intrauterine PRP: These immune-modulating therapies show promise for patients with repeated implantation failure, but evidence is moderate and further large trials are needed before routine use.
- Emerging “omics” biomarkers and personalized endometrial profiling: Molecular profiling of embryos and endometrium is advancing, but clinical implementation is still limited and evidence is evolving.
Low-certainty or myth:
- Pineapple core/bromelain, mandatory bed rest, lucky socks: There is no scientific evidence that eating pineapple core, strict bed rest after transfer, or wearing “lucky” items improves implantation rates. These are popular myths without clinical support.
- Unproven supplements and alternative therapies: Most supplements and alternative treatments lack robust evidence and should be approached with caution.
In summary, focus on evidence-based medical techniques and avoid unproven or anecdotal remedies to maximize your chances of successful implantation.
For more myth-busting fun, see Fertility Myths Debunked.

Your Implantation FAQs, Answered Fast
Is implantation timing different with frozen embryos?
Yes, implantation timing can differ with frozen embryo transfers (FET) compared to natural conception. In FET cycles, the timing is carefully controlled by synchronizing the embryo’s developmental stage with the endometrial “window of receptivity” using hormones or by tracking your natural cycle. This means implantation typically occurs a set number of days after the embryo is transferred, depending on whether it’s a day-3 or day-5 embryo, and is less variable than in natural cycles.
Can two embryos implant?
Yes, it is possible for two embryos to implant if more than one is transferred. This can result in twins or, less commonly, higher-order multiples. The likelihood depends on embryo quality, uterine receptivity, and other individual factors.
What if my cycles are irregular?
If your cycles are irregular, predicting natural implantation timing is more challenging. For those trying to conceive naturally, tracking ovulation with tests or monitoring can help. In fertility treatments, doctors use hormone medications or close monitoring to ensure the endometrium is receptive at the right time, so irregular cycles are less of a barrier. Master your cues in Ovulation Signals.
Does absence of symptoms mean failure?
No, the absence of symptoms does not mean implantation or pregnancy has failed. Many people experience no noticeable symptoms during implantation, and symptoms like spotting or cramping are not reliable indicators of success or failure.
When should I worry?
You should contact your healthcare provider if you experience heavy bleeding, severe pain, or signs of infection after embryo transfer or during the two-week wait. Otherwise, mild symptoms or no symptoms at all are common and not usually a cause for concern. If you have repeated implantation failures, your doctor may recommend further evaluation to look for underlying causes.
Final Thoughts
The implantation timeline in humans is a tightly regulated process that typically begins about 6 to 12 days after ovulation, with most successful pregnancies showing implantation between days 8 and 10. During this period, the blastocyst attaches to and then invades the uterine lining, establishing the early connection needed for nutrient and oxygen exchange. The timing of implantation is critical: research shows that later implantation (after day 10) is associated with a significantly higher risk of early pregnancy loss, while implantation within the 8–10 day window is linked to better outcomes. After attachment, the basic structure of the placenta starts forming by the end of the second week, and fetal-placental circulation is established by the third week.
Although the exact moment of implantation can be difficult to pinpoint, especially in natural cycles, assisted reproduction allows for more precise synchronization of embryo and endometrial readiness. Understanding this timeline helps explain why early pregnancy symptoms and positive tests may not appear until several days after conception. In summary, successful implantation depends on both precise timing and a receptive uterine environment, with most healthy pregnancies beginning implantation within a narrow window after ovulation.
Download our printable 10-Day Implantation Tracker and revisit Uterine Environment 101 whenever you need a reminder that your body is ready to welcome new life.
References
-
Gene expression changes in blastocyst hatching affect embryo implantation success in mice. Frontiers in Cell and Developmental Biology, 13. https://doi.org/10.3389/fcell.2025.1496298
-
Causes of embryo implantation failure: A systematic review and metaanalysis of procedures to increase embryo implantation potential. Frontiers in Endocrinology, 15. https://doi.org/10.3389/fendo.2024.1429193
-
Determinants of Embryo Implantation: Roles of the Endometrium and Embryo in Implantation Success. Reproductive Sciences, 30, 2339 - 2348. https://doi.org/10.1007/s43032-023-01224-w
-
Molecular Signaling Regulating Endometrium–Blastocyst Crosstalk. International Journal of Molecular Sciences, 21. https://doi.org/10.3390/ijms21010023
-
When the Embryo Meets the Endometrium: Identifying the Features Required for Successful Embryo Implantation. International Journal of Molecular Sciences, 25. https://doi.org/10.3390/ijms25052834
-
Molecular Determinants of Uterine Receptivity: Comparison of Successful Implantation, Recurrent Miscarriage, and Recurrent Implantation Failure. International Journal of Molecular Sciences, 24. https://doi.org/10.3390/ijms242417616
-
When the Embryo Meets the Endometrium: Identifying the Features Required for Successful Embryo Implantation. International Journal of Molecular Sciences, 25. https://doi.org/10.3390/ijms25052834
-
Endometrial fluid biomarkers and their potential as predictors of successful embryo implantation. BioMedicine, 13, 1 - 8. https://doi.org/10.37796/2211-8039.1413
-
The oviduct, sperm, and eggs : a multiomics AI integrated in vivo characterization during pregnancy. **. https://doi.org/10.32469/10355/105885
-
Outcomes of day 5 versus day 6 blastocysts: correlation of euploidy, implantation and embryo quality. Human Reproduction. https://doi.org/10.1093/humrep/dead093.661
-
Tailoring The Timing For Embryo Transfer: The Win-Test. Journal of Reproductive Immunology. https://doi.org/10.1016/j.jri.2022.103573
-
Preparation of the Endometrium for Frozen Embryo Transfer: A Systematic Review. Frontiers in Endocrinology, 12. https://doi.org/10.3389/fendo.2021.688237