You may wonder why the luteal phase matters so much for conception. The luteal phase, which follows ovulation, is when your body prepares for a possible pregnancy. During this time, progesterone rises to support the uterine lining, creating the best environment for an embryo to implant and grow. If this phase is too short or progesterone levels are too low, your chances of conception can drop, and the risk of early miscarriage may increase.
Research shows that even a single cycle with a short luteal phase can lower your odds of getting pregnant in the next cycle, though most people will still conceive within a year. In assisted reproduction, careful support of the luteal phase, often with progesterone, can significantly improve pregnancy and live birth rates, especially for those with low natural progesterone. Monitoring and, if needed, adjusting your luteal phase support is a practical, evidence-based way to boost your chances of success and help you feel more in control of your fertility journey.
- What exactly happens in the luteal phase and why is it the “make-or-break” window for pregnancy?
- How can you tell if your luteal phase is healthy or too short?
- What hidden factors shorten the luteal phase—and which puzzles remain unsolved?
- Which evidence-based steps can you take today to optimize your luteal phase naturally?
- When does medical luteal phase support make sense, and what really works?
- What new science could reshape luteal phase care by 2030?
- Your Top Questions, Answered
- Final Thoughts
- References
What exactly happens in the luteal phase and why is it the “make-or-break” window for pregnancy?
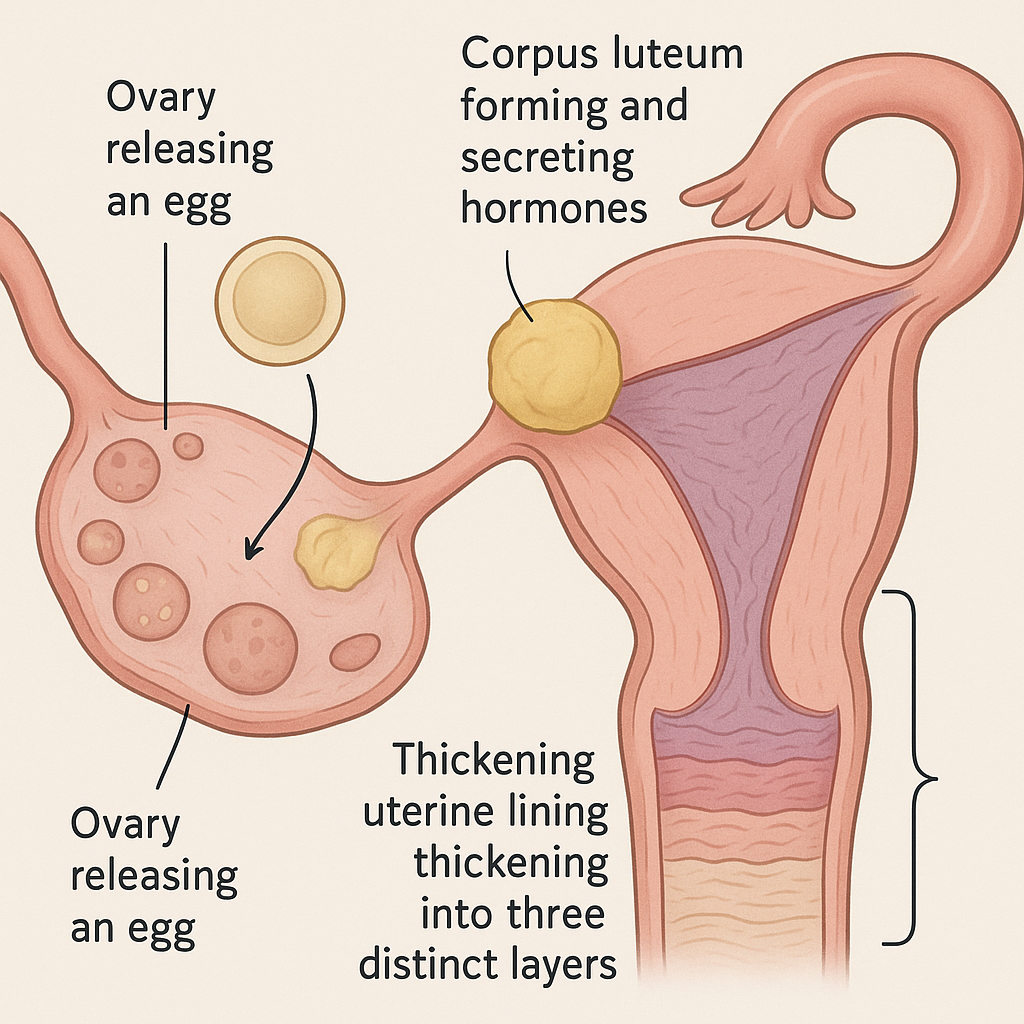
The luteal phase is the critical window between ovulation and your next period, typically lasting about 12–14 days. After ovulation, the follicle transforms into the corpus luteum, which produces progesterone and some estrogen. Progesterone’s main job is to prepare and stabilize your uterine lining, making it receptive for a fertilized embryo to implant. This hormone also calms uterine contractions and helps your immune system accept the embryo, both essential for early pregnancy to succeed. If fertilization occurs, the embryo signals your body to keep the corpus luteum active, maintaining high progesterone levels and supporting the pregnancy.
If the luteal phase is too short or progesterone levels are too low, the uterine lining may not be ready or may break down too soon, making implantation difficult or increasing the risk of early miscarriage. This is why the luteal phase is often called the “make-or-break” window for pregnancy: it is when the embryo must implant and signal its presence. In both natural and assisted conception, supporting the luteal phase, often with progesterone or similar medications, can significantly improve pregnancy and live birth rates, especially for those with known luteal phase issues. Monitoring and optimizing this phase gives you a real, evidence-based way to improve your chances of a successful pregnancy. For a day-by-day look, see the Implantation Timeline.
How can you tell if your luteal phase is healthy or too short?
To determine if your luteal phase is healthy or too short, you need to look at both the length of the phase and your hormone levels, especially progesterone. A healthy luteal phase typically lasts 11–13 days; if it is 10 days or fewer, this may indicate a luteal phase defect (LPD). The most reliable and widely recommended test is a blood progesterone measurement about 6–8 days after ovulation (the midluteal phase). A single progesterone level below 10 ng/mL, or a sum of three random midluteal progesterone levels below 30 ng/mL, suggests possible LPD. However, progesterone levels can fluctuate significantly, even within the same day, so timing and, sometimes, repeat testing are important.
Other methods, such as tracking basal body temperature or luteal phase length, are now considered unreliable for diagnosis due to low sensitivity and specificity. Endometrial biopsy, once the gold standard, is invasive and its results can vary from cycle to cycle, so it is now reserved for special cases or research. Advanced techniques like Doppler ultrasound to assess blood flow to the corpus luteum are being studied but are not standard practice. It’s also important to note that a short luteal phase or low progesterone in a single cycle does not always mean you have a persistent problem, as these can vary from month to month. If you are concerned about your luteal phase, consult a fertility specialist who can guide you through appropriate testing and interpretation.
For step-by-step ovulation timing, visit Ovulation Signals.
What hidden factors shorten the luteal phase—and which puzzles remain unsolved?
Several environmental and chemical exposures can subtly shorten the luteal phase, often without obvious symptoms.
Notably, exposure to air pollution, specifically particulate matter (PM10) and sulfur dioxide (SO₂) from fossil fuel combustion, has been linked to a shorter luteal phase, potentially affecting fertility by disrupting the hormonal environment needed for implantation. Additionally, certain chemicals found in plastics, such as bisphenol A (BPA) and some phthalates (notably monocarboxyoctyl phthalate, MCOP), are associated with a reduction in luteal phase length by up to about one day, even at common environmental exposure levels.
These factors do not appear to affect the follicular phase or overall cycle length, highlighting a specific vulnerability of the luteal phase to environmental toxins. Age and parity also play a role, with older women and those with certain reproductive histories experiencing more variability and sometimes shorter luteal phases. Medical conditions that affect progesterone production or endometrial response, such as luteal phase deficiency, can also contribute.
Despite these findings, many questions about luteal phase regulation remain unanswered. The precise molecular and cellular mechanisms that control the lifespan of the corpus luteum, the structure responsible for progesterone production, are still not fully understood, especially how environmental and internal signals interact to trigger its breakdown or maintenance. There is also ongoing debate about how to best diagnose and define luteal phase deficiency, as well as whether a short luteal phase is always clinically significant for fertility or pregnancy loss.
Furthermore, within-woman variability in luteal phase length is common and not fully explained by known factors, suggesting that additional, unidentified influences, possibly genetic, metabolic, or subtle hormonal shifts, may be at play. This complexity means that while some risk factors are recognized, the full picture of what shortens the luteal phase and how it impacts reproductive outcomes is still emerging.
For a full fertility overview, see Fertility 101.
Which evidence-based steps can you take today to optimize your luteal phase naturally?
To naturally optimize your luteal phase, focus on lifestyle and dietary habits that support healthy hormone production and reduce stress. These actions help your body produce and maintain healthy progesterone levels, which are crucial for fertility and early pregnancy.
- Eat a balanced diet: Focus on whole grains, lean proteins, healthy fats, and plenty of fruits and vegetables. These nutrients support hormone production and overall reproductive health.
- Maintain a healthy weight: Both underweight and overweight status can disrupt your menstrual cycle and shorten the luteal phase. Aim for a body mass index (BMI) in the recommended range.
- Manage stress: Chronic stress can interfere with ovulation and hormone balance. Practice mindfulness, yoga, or regular physical activity to reduce stress.
- Prioritize sleep: Aim for 7–9 hours of quality sleep each night. Poor sleep can negatively affect hormone regulation.
- Limit exposure to endocrine disruptors: Avoid chemicals like bisphenol A (BPA) and certain phthalates found in plastics, as these may shorten the luteal phase.
- Avoiding exposure to endocrine-disrupting chemicals (like BPA and some phthalates) and minimizing air pollution exposure may also help, as these have been linked to shorter luteal phases.
- Use cervical mucus patterns alongside OPKs. Our Cervical Mucus Decoder helps confirm you’re fixing the right phase.
A recent Cochrane review found that while progesterone supplementation may increase clinical pregnancy rates in some cases, the evidence for natural cycle support is still evolving, and lifestyle changes remain foundational. According to Dr. Hugh Taylor, MD, Chair of Obstetrics, Gynecology & Reproductive Sciences at Yale School of Medicine: “Optimizing your overall health—nutrition, stress, and sleep—can have a meaningful impact on your reproductive hormones and cycle regularity.”
While most evidence for luteal phase support comes from medical interventions like progesterone supplementation, these natural strategies can help create a hormonal environment more favorable for a healthy luteal phase and successful implantation. If you suspect a persistent luteal phase problem, consult a healthcare provider for personalized advice and possible medical support.

When does medical luteal phase support make sense, and what really works?
You may need medical luteal phase support if you have a diagnosed luteal phase defect (LPD), especially if you are undergoing assisted reproductive technology (ART) such as in vitro fertilization (IVF), or if you have a history of recurrent pregnancy loss with evidence of low progesterone.
Luteal phase support is standard in most ART cycles because ovarian stimulation can disrupt your body’s natural hormone production, making it harder to maintain a healthy uterine lining for implantation. If you have a consistently short luteal phase (10 days or fewer) or low mid-luteal progesterone levels, your provider may recommend support. The American College of Obstetricians and Gynecologists (ACOG) and other expert groups note that routine luteal support is not recommended for everyone, but may be considered after a thorough evaluation, especially if other causes of infertility or pregnancy loss have been ruled out.
Progesterone supplementation is the most evidence-based and widely used treatment for luteal phase support. It can be given as vaginal, intramuscular, or subcutaneous formulations, with studies showing similar pregnancy rates across these methods. Intramuscular progesterone is often favored for its effectiveness, but vaginal and subcutaneous routes are also effective and may be more comfortable for some people. Dydrogesterone, a synthetic progestogen, is another option with a good safety profile and similar effectiveness to natural progesterone. Human chorionic gonadotropin (hCG) can also be used, but it increases the risk of ovarian hyperstimulation syndrome and is less commonly recommended.
Some evidence suggests that adding estrogen to progesterone may further improve implantation rates in certain IVF protocols. Acupuncture, when combined with drug therapy, may improve pregnancy rates and hormone levels, but more high-quality research is needed before it can be widely recommended. According to a 2024 review in Obstetrical & Gynecological Survey, “no treatment modality has demonstrated efficacy in improving fertility outcomes for LPD patients, including progesterone supplementation, whose inconsistent data do not sufficiently support its routine use, despite its minimal risk”. Always discuss options with your reproductive endocrinologist to tailor treatment to your specific needs.
If male-factor issues also exist, pair luteal care with strategies in Sperm Health 101.
What new science could reshape luteal phase care by 2030?
By 2030, several scientific advances could reshape how you receive luteal phase care, making it more effective, comfortable, and personalized. Researchers are moving toward individualized luteal phase support, where your treatment is tailored to your unique hormone levels, ovarian response, and personal needs, rather than using a one-size-fits-all protocol. This approach may improve pregnancy rates and reduce side effects, especially for those undergoing in vitro fertilization (IVF) or other assisted reproductive technologies.
New medications and delivery methods are also on the horizon. Oral dydrogesterone, a synthetic progestogen, is gaining ground as a convenient and well-tolerated alternative to vaginal or intramuscular progesterone, with studies showing similar effectiveness for supporting the luteal phase in IVF cycles. Subcutaneous progesterone injections are another promising option, offering effectiveness comparable to vaginal products and potentially greater comfort and convenience for you.
Better diagnostic tools are being developed to identify the optimal “window of implantation” and to monitor endometrial receptivity in real time, which could help time embryo transfers more precisely and improve outcomes. Advances in understanding the molecular and genetic factors that influence luteal phase function may also lead to targeted therapies for those with persistent luteal phase defects.
A 2023 review in Nature Reviews Endocrinology highlights that “the next decade will likely see a shift from empirical protocols to evidence-based, individualized regimens that optimize both safety and success”. As Dr. Scott M. Nelson, Professor of Reproductive Medicine at the University of Glasgow, notes: “The future of luteal phase support lies in personalizing care—matching the right treatment to the right patient at the right time, based on robust scientific evidence and patient preferences.”
If you are planning fertility treatment, ask your provider about emerging options and how new science may benefit your care.
Your Top Questions, Answered
Can you get pregnant during the luteal phase?
Yes, you can get pregnant during the luteal phase, but only if you had unprotected sex just before or during ovulation. The luteal phase starts after ovulation, when the egg has already been released. Sperm can survive in your reproductive tract for up to five days, so if you ovulate shortly after intercourse, fertilization is possible. However, once ovulation has passed, the chance of pregnancy drops sharply because the egg survives only 12–24 hours.
Does a short luteal phase mean infertility?
A short luteal phase (10 days or fewer) can make it harder for an embryo to implant, but it does not always mean infertility. Many people with short luteal phases conceive naturally. The link between short luteal phase and infertility or recurrent pregnancy loss is debated, and current evidence does not prove that a short luteal phase alone causes infertility. If you have concerns, a thorough evaluation for other causes is important.
How long should progesterone supplementation last?
For those undergoing in vitro fertilization (IVF) or assisted reproduction, progesterone supplementation usually continues until 8–10 weeks of pregnancy, when the placenta takes over hormone production. Recent studies show that stopping progesterone after a positive pregnancy test is as effective as longer courses, with no difference in live birth or miscarriage rates. For natural cycles, the optimal duration is less clear and should be individualized.
What if my luteal phase is 9 days but cycles are regular?
A luteal phase of 9 days is considered short, but if your cycles are otherwise regular and you have no trouble conceiving, it may not require treatment. Short luteal phases can occur in healthy, fertile people. If you are struggling to conceive or have recurrent pregnancy loss, discuss further evaluation with your provider to rule out other causes.
What’s the best at-home test for luteal health?
At home, you can track your luteal phase by monitoring ovulation (using ovulation predictor kits or basal body temperature) and counting the days from ovulation to your next period. No over-the-counter test can directly diagnose luteal phase deficiency. If you suspect a problem, consult your healthcare provider for hormone testing and further assessment.
Final Thoughts
The luteal phase plays a crucial role in supporting early pregnancy by preparing the uterine lining for embryo implantation and maintaining it through progesterone production. Adequate luteal function is essential for successful conception and ongoing pregnancy, especially in assisted reproductive technology (ART) cycles.
Evidence shows that luteal phase support with progesterone can significantly increase clinical pregnancy and live birth rates in women undergoing ovarian stimulation and intrauterine insemination (IUI) or frozen embryo transfer (FET). For example, one randomized controlled trial found that women receiving vaginal progesterone had a live birth rate per cycle of 17.4%, compared to 9.3% without support. However, in natural cycles, a short luteal phase may only temporarily reduce fertility, with no significant difference in cumulative pregnancy rates after 12 months of trying.
Maintaining optimal serum progesterone levels during the luteal phase is associated with higher pregnancy and lower miscarriage rates in ART cycles. While luteal phase deficiency is a debated cause of infertility, targeted support can be beneficial in specific clinical scenarios. In summary, a healthy luteal phase is vital for pregnancy success, and medical support may improve outcomes for those with identified deficiencies or undergoing fertility treatments.
Ready for the next piece of the puzzle? Explore timing intimacy with Egg vs. Sperm Lifespan and feel confident you’re optimizing every fertile moment.
References
-
Correlation Between Luteal Phase Serum Progesterone Levels and Pregnancy Outcome in Frozen Embryo Transfer Cycles: A Prospective Cohort Study. Fertility Science and Research. https://doi.org/10.25259/fsr_27_2024
-
Luteal phase support in assisted reproductive technology… Nature reviews. Endocrinology. https://doi.org/10.1038/s41574-023-00921-5
-
Diagnosis and treatment of luteal phase deficiency: a committee opinion… Fertility and sterility. https://doi.org/10.1016/j.fertnstert.2021.02.010
-
Current Knowledge on the Multifactorial Regulation of Corpora Lutea Lifespan: The Rabbit Model. Animals : an Open Access Journal from MDPI, 11. https://doi.org/10.3390/ani11020296
-
Menstrual bleeding, cycle length, and follicular and luteal phase lengths in women without known subfertility: A pooled analysis of three cohorts… Paediatric and perinatal epidemiology. https://doi.org/10.1111/ppe.12644
-
Luteal phase support for women trying to conceive by intrauterine insemination or sexual intercourse… The Cochrane database of systematic reviews, 8, CD012396. https://doi.org/10.1002/14651858.CD012396.pub2
-
The Role of Dydrogesterone in the Management of Luteal Phase Defect: A Comprehensive Review. Cureus, 15. https://doi.org/10.7759/cureus.48194
-
Luteal Phase Defects and Progesterone Supplementation. Obstetrical & Gynecological Survey, 79, 122 - 128. https://doi.org/10.1097/OGX.0000000000001242
-
Acupuncture in the Treatment of Infertility due to Luteal Phase Defect: A Meta-Analysis. Clinical and Experimental Obstetrics & Gynecology. https://doi.org/10.31083/ceog19928