Did you know your anti-Müllerian hormone (AMH) can drop 65 % between age 30 and 38—yet 1 in 4 women with “low” numbers still conceive naturally?
If you are concerned about your fertility, you are not alone. Many people in the United States are seeking clear answers about their reproductive health, especially as they consider family planning. Ovarian reserve naturally declines with age, and this decline can impact your chances of conception. Understanding your ovarian reserve is a practical step in making informed decisions about your future.
Two key hormones, anti-Müllerian hormone (AMH) and follicle-stimulating hormone (FSH), are commonly measured to assess ovarian reserve. AMH reflects the number of growing follicles in your ovaries, while FSH helps regulate egg development. These tests, along with your age, provide valuable information about your reproductive timeline and can guide your next steps, whether you are trying to conceive now or planning for the future. While these markers offer important insights, remember that they do not predict your ability to get pregnant with certainty—age remains the strongest factor influencing fertility outcomes.
Taking charge of your reproductive health is empowering. By learning about AMH, FSH, and your biological clock, you can approach your fertility journey with knowledge and confidence. If you have questions or concerns, seeking guidance from a fertility specialist can help you interpret your results and explore your options.
- What exactly is ovarian reserve, and how fast does it decline?
- How do AMH and FSH tests “read” your egg bank?
- Which AMH and FSH levels are normal for your age—and what if they disagree?
- Can lifestyle choices or supplements really slow the biological clock?
- When should you test, seek help, or consider egg freezing or IVF?
- Your top questions about ovarian reserve, answered
- Final thoughts: turning numbers into hopeful next steps
- References
What exactly is ovarian reserve, and how fast does it decline?
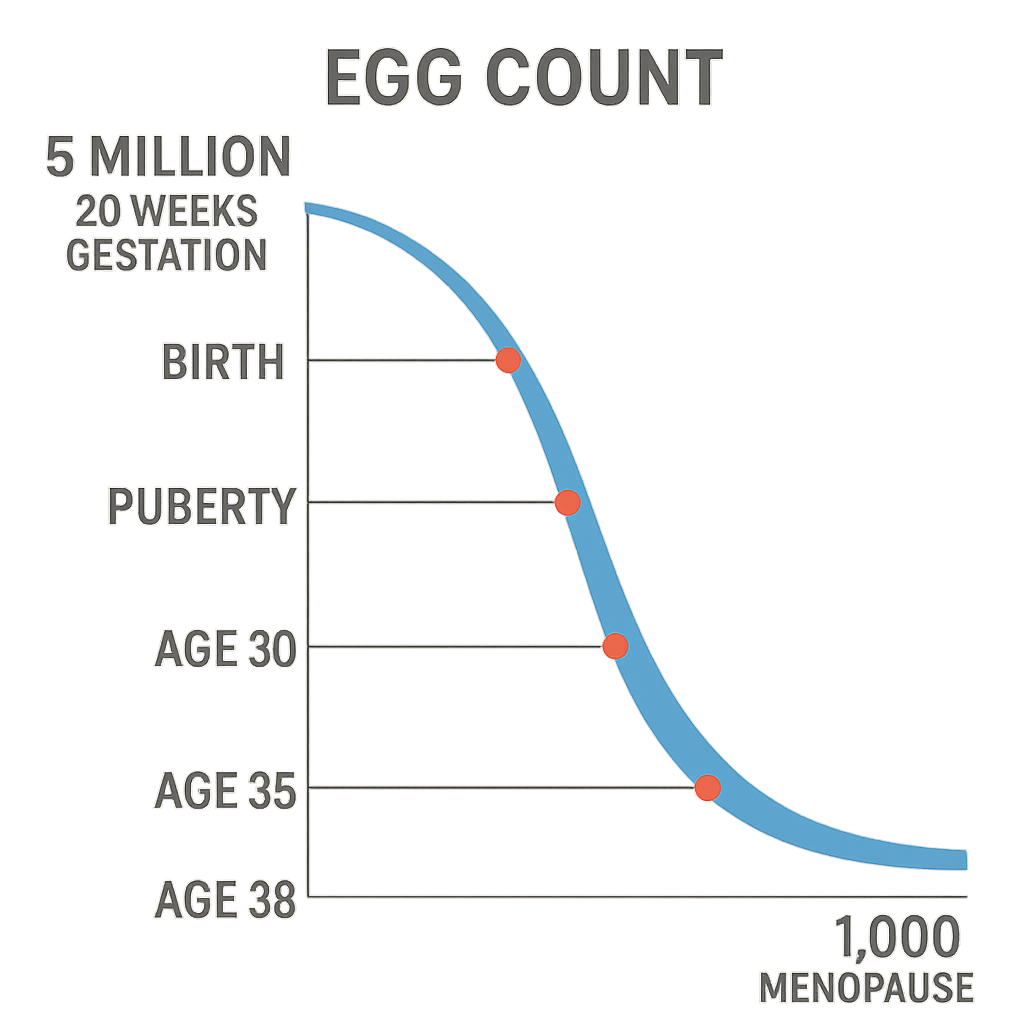
Ovarian reserve is the total number of eggs (oocytes) remaining in your ovaries, and it is established before birth. This reserve declines throughout your life in a non-linear pattern: the loss is gradual in your twenties, but accelerates in your thirties, with a marked drop after age 35. By age 30, only about 12% of your original egg supply remains, and by age 40, this drops to around 3%. For most people, a significant decline in ovarian reserve begins around age 31–34, though the exact timing can vary based on genetics, health, and lifestyle.
The decline is measured using markers like anti-Müllerian hormone (AMH) and antral follicle count (AFC), both of which decrease as you age. Studies show that AFC declines at a rate of about 3.8% per year in fertile women, and AMH levels follow a similar pattern. While age is the main driver, factors such as chronic illness, endometriosis, or cancer treatments can accelerate this decline. In some conditions, like polycystic ovary syndrome (PCOS), the rate of decline in AMH may be faster, but the overall pattern of loss remains. Understanding your ovarian reserve helps you make informed decisions about fertility and family planning, as the number and quality of eggs both decrease with age, affecting your chances of conception.
For a broader tour of the reproductive basics, see our step-by-step primer Fertility 101.
How do AMH and FSH tests “read” your egg bank?
AMH (anti-Müllerian hormone) is produced by the granulosa cells of small, growing follicles in your ovaries. The level of AMH in your blood directly reflects the number of these developing follicles, making it a reliable marker for estimating your ovarian reserve, the size of your remaining “egg bank.” AMH levels are relatively stable throughout your menstrual cycle and are not significantly affected by hormonal fluctuations, so they can be measured at any time. Higher AMH levels generally indicate a larger pool of eggs, while lower levels suggest a diminished reserve and a potentially shorter reproductive window. However, AMH does not provide information about the quality of your eggs or guarantee your chances of pregnancy, and factors like age, body mass index, and certain medical conditions can influence AMH readings. AMH is especially useful for predicting how your ovaries might respond to fertility treatments, such as ovarian stimulation, but it should always be interpreted alongside other clinical information and not as a stand-alone predictor of fertility.
FSH (follicle-stimulating hormone) is produced by your brain and stimulates your ovaries to mature eggs each cycle. When your ovarian reserve is low, your body compensates by increasing FSH production, so higher FSH levels; especially when measured early in your menstrual cycle can signal a reduced egg supply. FSH levels can fluctuate from month to month and are influenced by factors such as stress, illness, and hormonal medications, making them less stable than AMH. Typically, FSH is measured on day 2 or 3 of your cycle for the most accurate assessment. High FSH levels, especially when combined with low AMH, are strong indicators of diminished ovarian reserve. However, like AMH, FSH does not predict egg quality or guarantee pregnancy outcomes, and it is best used as part of a broader fertility evaluation. Combining AMH and FSH results with your age and other clinical factors provides a more complete picture of your reproductive health.
AMH and FSH act like dashboard lights for your ovaries, but they measure different things:
| Feature | AMH | FSH (day 2–3) |
|---|---|---|
| Where it’s made | Growing follicles | Pituitary gland |
| Cycle timing | Any day | Early follicular phase |
| What rising / falling means | Higher = more antral follicles; very high can signal PCOS | Higher = ovaries need more “push” → diminished reserve |
| Stability | Steady month to month | Fluctuates cycle to cycle |
| Best use | Predicts ovarian response to IVF, egg freezing | Adds context, confirms diminished reserve |
For more myth-busting on “one number tells all,” drop by Fertility Myths Debunked.
Which AMH and FSH levels are normal for your age—and what if they disagree?
AMH (anti-Müllerian hormone) levels are a direct reflection of the number of small, growing follicles in the ovaries and thus serve as a sensitive marker of ovarian reserve. AMH levels are highest in the early twenties, with median values around 6.2 ng/mL, and decline steadily with age, dropping to about 1.1 ng/mL by the early forties. The normal range for AMH is broad and age-dependent: for example, the 5th to 95th percentile ranges from 2.1–12.7 ng/mL at age 20–24, and from 0.08–5.7 ng/mL at age 40–55. AMH is considered more stable than other hormones, as it does not fluctuate significantly during the menstrual cycle, and is negatively correlated with FSH and age. Low AMH levels, especially below 0.5 ng/mL, are associated with a higher risk of diminished ovarian reserve and conditions like premature ovarian insufficiency.
FSH (follicle-stimulating hormone) is produced by the pituitary gland and stimulates the growth of ovarian follicles. FSH levels are typically measured early in the menstrual cycle (days 2–4), and normal values are generally below 10 IU/L in younger women. As ovarian reserve declines with age, FSH levels rise, often exceeding 10 IU/L in women with reduced egg supply. However, FSH can fluctuate from cycle to cycle and may not increase until ovarian reserve is already quite low, making it a less sensitive early marker compared to AMH. High FSH levels, especially when combined with low AMH, are strong indicators of diminished ovarian reserve.
If AMH and FSH results do not match such as a low AMH but normal FSH, or vice versa, it can be confusing. This discordance can occur because AMH is an earlier and more stable marker of declining ovarian reserve, while FSH may remain normal until the reserve is very low or fluctuate from cycle to cycle and may not rise until ovarian reserve is already quite low 34. In such cases, AMH is generally considered the more sensitive and reliable indicator, especially for early changes in ovarian reserve. However, both results should be interpreted in the context of age, menstrual history, and other clinical factors. If your results are discordant, consulting a fertility specialist can help clarify your reproductive outlook and guide next steps. Using anti-Müllerian hormone to predict premature ovarian insufficiency: a retrospective cross-sectional study..
Below is a snapshot many clinics use. Always compare with your lab’s reference range.
| Age band | Typical AMH (ng/mL) | Typical FSH (IU/mL) |
|---|---|---|
| 20–24 | 4–9 | <8 |
| 25–29 | 3–6 | <8 |
| 30–34 | 2–4 | <9 |
| 35–39 | 1–3 | <10 |
| 40–44 | 0.5–1.5 | 10–15 |
| 45+ | <0.5 | >15 |
Remember, ovulation patterns play a starring role as well—learn daily signs in our guide Ovulation Signals.
Can lifestyle choices or supplements really slow the biological clock?
You can influence your reproductive health through lifestyle choices, but you cannot stop the natural decline of your ovarian reserve. Here’s what the latest research and expert guidance say:
Lifestyle Choices That Support Ovarian Health:
- Maintain a healthy body mass index (BMI). High BMI is linked to lower ovarian reserve and poorer egg quality.
- Eat a balanced, nutrient-rich diet. Diets high in fruits, vegetables, whole grains, and healthy fats; sometimes called “profertility diets”—are associated with higher anti-Müllerian hormone (AMH) and antral follicle count (AFC), especially in people with overweight or obesity.
- Avoid smoking and limit alcohol. Both can accelerate ovarian aging and reduce fertility.
- Manage stress and prioritize sleep. Chronic stress and poor sleep can disrupt reproductive hormones and menstrual cycles.
- Exercise moderately. Excessive or very intense exercise may harm ovarian reserve, but regular moderate activity is beneficial.
Supplements:
- Dehydroepiandrosterone (DHEA) may improve ovarian reserve and pregnancy rates in people with diminished ovarian reserve, but should only be used under medical supervision.
- Excessive iron supplementation (over 45 mg/day) may lower ovarian reserve, so only take iron if your provider recommends it.
- The benefits of other supplements, like folic acid, are still under study; no supplement is proven to “pause” the biological clock.
In a 2023 review of nearly 6,000 women, over half the studies found a clear link between nutritional status and ovarian reserve. Dr. Laura Prieto-Huecas, PhD, lead author of a 2023 systematic review, states: “A high body mass index has a negative impact on the ovary, decreasing antral follicle count and anti-Müllerian hormone. Oocyte quality is compromised, increasing the rate of reproductive problems and the demand for assisted reproductive techniques”.
You can support your fertility by maintaining a healthy weight, eating well, and avoiding harmful habits. No lifestyle change or supplement can fully stop ovarian aging, but healthy choices may help you preserve your reproductive potential for longer. For personalized advice, consult a reproductive endocrinologist or your healthcare provider.
Pair these habits with the lifespan insights in Egg vs. Sperm Lifespan and keep your uterine “home” healthy via Uterine Environment 101.
When should you test, seek help, or consider egg freezing or IVF?
You should consider fertility testing if you are planning to delay pregnancy, have irregular periods, or have been trying to conceive for 12 months (or 6 months if you are 35 or older). Early testing can help you understand your ovarian reserve and fertility potential, allowing you to make informed decisions about your reproductive future. Seek help from a reproductive endocrinologist if you have risk factors such as a history of cancer, endometriosis, or family history of early menopause, or if you have not conceived after the recommended time frame.
Egg freezing (oocyte cryopreservation) is most effective when done before age 35, as egg quality and quantity decline with age. Freezing your eggs in your early 30s can “freeze in time” your fertility potential, giving you more options later. In the words of Dr. Richard Anderson, MD, FRCOG: “Freezing a woman’s eggs at age 30 literally ‘freezes in time’ her fertility potential and gives her the chance of a healthy pregnancy at a time of her choosing”. The success rates for using frozen eggs are now similar to those for fresh eggs, thanks to advances in vitrification technology.
In vitro fertilization (IVF) may be considered if you have not conceived after trying for a year (or six months if over 35), have known fertility issues, or after unsuccessful less-invasive treatments. IVF can use fresh or frozen eggs/embryos, and both approaches have similar live birth rates, though the “freeze-all” strategy may reduce the risk of ovarian hyperstimulation syndrome.
Key points:
- Test early if you have risk factors or are considering delaying pregnancy.
- Seek help after 6–12 months of trying, depending on your age.
- Consider egg freezing before age 35 for best results.
- IVF is an option if other treatments fail or if you have specific fertility challenges.
- Consult a fertility specialist for personalized guidance.
A 2020 review in BJOG highlights that while more people are freezing eggs, the number of cycles using stored eggs remains low, so early, informed decisions are crucial for maximizing your options.
The luteal phase after ovulation still decides implantation success—see why in The Luteal Phase.
Your top questions about ovarian reserve, answered
Does low AMH mean early menopause?
Low anti-Müllerian hormone (AMH) levels are strongly associated with a higher risk of early menopause, especially if measured in your early to mid-30s. Each 0.10 ng/mL decrease in AMH increases your risk of menopause before age 45 by about 14%. For example, women with AMH of 0.5 ng/mL have a much higher risk of early menopause than those with 2.0 ng/mL. However, low AMH does not guarantee early menopause; it is a risk marker, not a diagnosis. Other factors like genetics and lifestyle also play a role.
Can I get pregnant naturally with AMH <0.5 ng/mL?
Yes, natural pregnancy is still possible with AMH below 0.5 ng/mL. While low AMH reflects a reduced ovarian reserve, it does not predict your ability to conceive naturally in a given cycle. Many people with very low AMH have conceived without fertility treatment.
Will birth-control pills lower my AMH?
Birth-control pills do not permanently lower your AMH. While some studies suggest a temporary decrease in AMH levels during use, these changes are reversible and do not affect your long-term ovarian reserve. AMH levels typically return to baseline within a few months after stopping the pill.
Do supplements like CoQ10 actually help?
Coenzyme Q10 (CoQ10) may support ovarian function, especially in people with obesity-related infertility. Animal studies show CoQ10 can improve the number of healthy follicles and ovulation rates, but it does not reverse age-related decline or metabolic issues. For most people, CoQ10 is best used as part of a broader plan that includes a balanced diet and healthy lifestyle. Evidence in humans is still limited, so discuss any supplement use with your healthcare provider.
Does low AMH affect implantation?
Low anti-Müllerian hormone (AMH) levels are linked to a reduced number of eggs and embryos during in vitro fertilization (IVF), but do not consistently lower the chance of implantation if a good-quality embryo is available. However, overall pregnancy and live birth rates may be lower in people with low AMH simply because fewer embryos are available for transfer. Check implantation steps in our Implantation Timeline.
Final thoughts: turning numbers into hopeful next steps
A low anti-Müllerian hormone (AMH) result can feel discouraging, but it does not define your fertility or your future. AMH reflects the number of eggs remaining, not their quality or your ability to conceive naturally or with treatment. Your age remains the most important factor for success, especially with in vitro fertilization (IVF).
If you receive a low AMH diagnosis, consider these hopeful next steps:
- Consult a reproductive endocrinologist to interpret your results in context and discuss your options.
- Remember that low AMH should not exclude you from trying fertility treatments, including IVF, as many people with low AMH still achieve pregnancy—especially if you are younger.
- Use your AMH level to guide decisions about timing, treatment strategies, and whether to consider egg freezing or IVF sooner rather than later.
- Focus on your overall health: maintain a healthy weight, avoid smoking, and manage stress, as these can support your fertility journey.
- Stay informed and proactive, but do not let a single number dictate your hope or plans.
As Dr. Marcelle Cedars, MD, Professor of Obstetrics, Gynecology, and Reproductive Sciences, notes: “AMH is a good marker of oocyte quantity but does not reflect oocyte health or chances for pregnancy. Age is still the strongest driver in determining success rates with fertility treatments”. With the right support and information, you can turn your numbers into a plan that fits your goals and values.
Ready to decode more of your body’s signals? Explore cervical mucus patterns in our Cervical Mucus Decoder. Understanding your numbers today can transform uncertainty into empowered, hopeful planning tomorrow.
References
-
‘Age specific variations in ovarian reserves in healthy fertile and infertile women: A cross sectional study. PLOS ONE, 19. https://doi.org/10.1371/journal.pone.0308865
-
Assessment of Nutritional Status and Its Influence on Ovarian Reserve: A Systematic Review. Nutrients, 15. https://doi.org/10.3390/nu15102280
-
Iron intake in relation to ovarian reserve among women seeking infertility treatment… Human reproduction. https://doi.org/10.1093/humrep/dead118
-
Risk factors for diminished ovarian reserve in women: Current state of the problem. Acta Biomedica Scientifica. https://doi.org/10.29413/abs.2024-9.3.6
-
Dietary patterns are associated with improved ovarian reserve in overweight and obese women: a cross-sectional study of the Lifestyle and Ovarian Reserve (LORe) cohort. Reproductive Biology and Endocrinology : RB&E, 20. https://doi.org/10.1186/s12958-022-00907-4
-
Effect of folic acid supplementation on diminished ovarian reserve: study protocol of a single-centre, open-label, randomised, placebo-controlled clinical trial. BMJ Open, 12. https://doi.org/10.1136/bmjopen-2021-057689
-
Ovarian aging in humans: potential strategies for extending reproductive lifespan. GeroScience, 1-13. https://doi.org/10.1007/s11357-023-00768-8
-
Evaluation of Female Fertility - AMH and Ovarian Reserve Testing… The Journal of clinical endocrinology and metabolism. https://doi.org/10.1210/clinem/dgac039
-
Evaluation of Serum AMH, INHB Combined with Basic FSH on Ovarian Reserve Function after Laparoscopic Ovarian Endometriosis Cystectomy. Frontiers in Surgery, 9. https://doi.org/10.3389/fsurg.2022.906020
-
Using anti-Müllerian hormone to predict premature ovarian insufficiency: a retrospective cross-sectional study. Frontiers in Endocrinology, 15. https://doi.org/10.3389/fendo.2024.1454802
-
Age-dependent changes in anti-Müllerian hormone levels in Lebanese females: correlation with basal FSH and LH levels and LH/FSH ratio: a cross-sectional study. BMC Women’s Health, 20. https://doi.org/10.1186/s12905-020-00998-4
-
Elective Egg Freezing for Non‐Medical Reasons. BJOG: An International Journal of Obstetrics & Gynaecology, 127, e113 - e121. https://doi.org/10.1111/1471-0528.16025