Up to 70 % of “day-14” guesses miss the real fertile window.
If you are trying to conceive, understanding your ovulation signals is crucial. Many people worry about missing their fertile window, and this concern is valid, timing can make a significant difference. Research shows that ovulation is a complex process, influenced by hormones, your body’s internal clock, and even daily rhythms. Accurately identifying when you ovulate can increase your chances of pregnancy.
You are not alone if you find ovulation signs confusing. Hormone levels, such as progesterone and estradiol, shift in the days leading up to ovulation, and these changes can be tracked to pinpoint your most fertile days. Studies have found that monitoring these signals like changes in hormone levels or follicle size can help you better predict ovulation and time intercourse or fertility treatments for the best chance of success. Your attention to these details is a powerful step toward your goal.
- What is ovulation and why does its exact timing matter for TTC success?
- How does a 28-day model cycle unfold day by day, and where can yours differ?
- Which physical signs hint that ovulation is approaching—often days in advance?
- How can basal body temperature confirm yesterday’s ovulation and refine next month’s plan?
- Which hormone-based tools can pinpoint the fertile window within 24–36 hours?
- What if your cycles are irregular, PCOS-affected, or postpartum—can you still trust the signs?
- When—and how often—should partners have sex for peak conception odds?
- Which lifestyle tweaks sharpen ovulation signals and overall fertility?
- What red flags suggest you’re not ovulating—and when should you call a specialist?
- Your top ovulation questions—answered fast
- Final Thoughts
- Refeerences
What is ovulation and why does its exact timing matter for TTC success?
Ovulation is the process where one of your ovaries releases a mature egg, making it available for fertilization. This event is a key part of your menstrual cycle and is tightly regulated by hormonal signals and even your body’s internal clock. The exact timing of ovulation varies from person to person and even from cycle to cycle, but it typically occurs about midway through your cycle. For those trying to conceive (TTC), knowing precisely when you ovulate is critical because your chances of pregnancy are highest during a short fertile window—about six days ending on the day of ovulation itself.
The importance of timing comes down to biology: sperm can survive in your reproductive tract for up to five days, but your egg remains viable for only about 12–24 hours after ovulation. Research shows that nearly all pregnancies result from intercourse during this fertile window, with the highest probability of conception occurring when intercourse happens on the day of ovulation or the two days before. Missing this window can mean waiting another month for a chance at pregnancy. Accurately identifying ovulation—using signs like hormone levels, follicle size, or ovulation predictor kits—can help you time intercourse or fertility treatments for the best chance of success. Understanding and tracking your ovulation empowers you to take control of your fertility journey. Egg vs. Sperm Lifespan.
How does a 28-day model cycle unfold day by day, and where can yours differ?
The menstrual cycle unfolds in various phases:
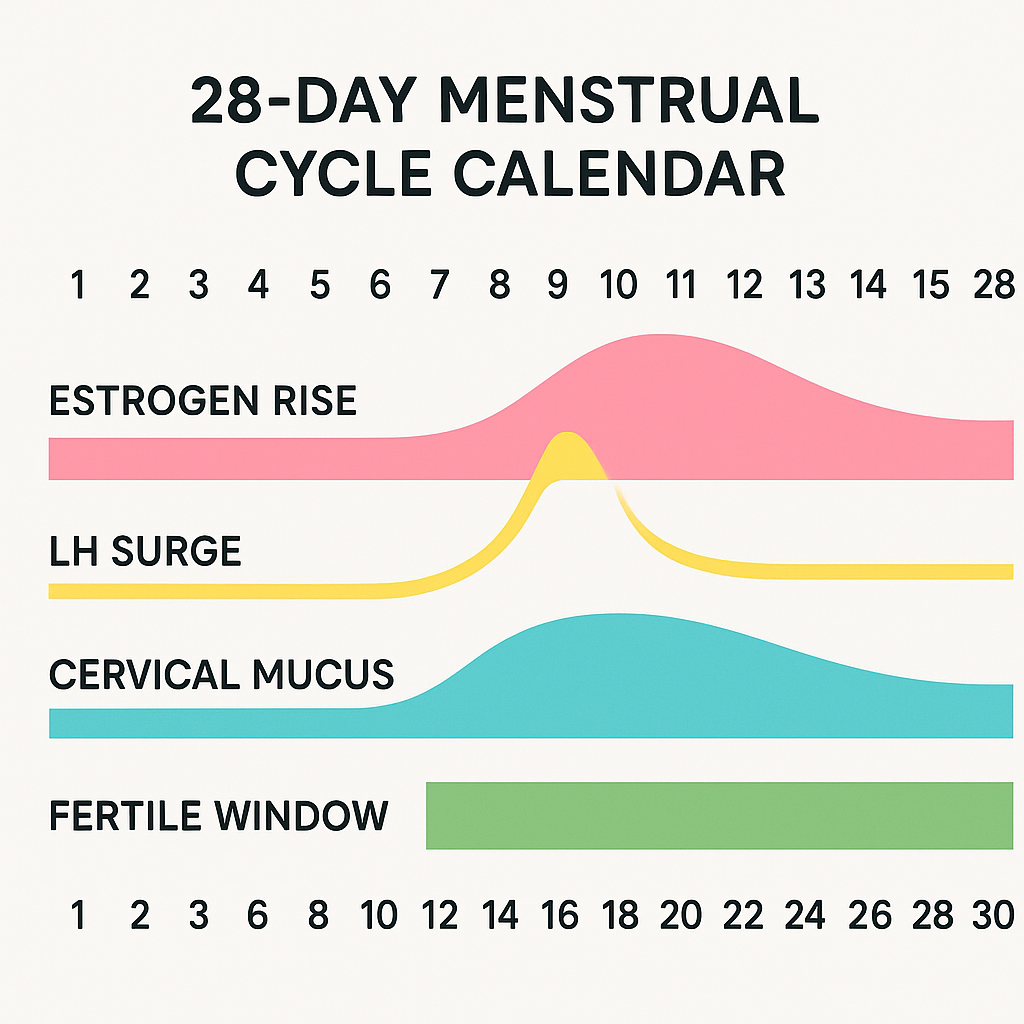
- Day 1–5: This is your period, when the uterine lining sheds and bleeding occurs. Estrogen levels are at their lowest, which can lead to fatigue or mood changes. The average period lasts about 4–6 days, but it can range from 2 to 8 days for some people.
- Day 6–9: As your period ends, your ovaries begin to grow several follicles, each containing an immature egg. Estrogen starts to rise, prompting the uterine lining to rebuild. Cervical mucus becomes more noticeable and creamy, signaling increasing fertility.
- Day 10–13: Estrogen peaks, causing the dominant follicle to mature fully. Cervical mucus becomes watery and then stretchy, resembling raw egg whites—this is the most fertile type of mucus. The uterine lining thickens further, preparing for a possible pregnancy.
- Day 14: A surge in luteinizing hormone (LH) triggers ovulation, releasing a mature egg from the ovary. This is your most fertile day, and the egg survives for about 12–24 hours. Some people may feel mild pain or notice a slight dip and then rise in basal body temperature (BBT).
- Day 15–28: After ovulation, progesterone becomes the dominant hormone. It raises your BBT by 0.5–1°F (0.3–0.6°C) and causes cervical mucus to thicken, making it less sperm-friendly. If the egg is not fertilized, hormone levels drop, and the cycle restarts with your next period.
Your cycle may differ from this model in several ways. The length of each phase, especially the follicular phase (before ovulation), can vary widely between individuals and even from month to month. Ovulation may not always occur on day 14; it can happen earlier or later, shifting your fertile window. Factors like age, stress, health, and body weight can influence your hormone levels and the timing of each phase. Some people experience shorter or longer periods, variable mucus patterns, or fluctuations in BBT. Tracking your own signs rather than relying on averages, helps you understand your unique cycle and optimize your chances of conception.
Which physical signs hint that ovulation is approaching—often days in advance?
As ovulation approaches, several physical signs can be observed days in advance, reflecting the body’s hormonal changes. One of the most reliable early indicators is a change in cervical mucus: it becomes more abundant, first creamy, then watery, and finally clear and stretchy (similar to raw egg whites) signaling peak fertility. Many women also notice increased libido and subtle pelvic discomfort or twinges (sometimes called mittelschmerz) as the dominant follicle matures and the ovary prepares to release an egg. Breast tenderness and mild bloating may also occur due to rising estrogen levels.
Another key sign is a surge in luteinizing hormone (LH), which can be detected in urine with home ovulation predictor kits; this surge typically happens 24–36 hours before ovulation and is a strong signal that ovulation is imminent. While basal body temperature (BBT) rises after ovulation, tracking BBT over several cycles can help you recognize the pattern and confirm ovulation retrospectively. Less commonly, some women may notice a heightened sense of smell, mood changes, or subtle shifts in energy. Other methods, such as observing salivary ferning or changes in skin temperature, have been studied but are less reliable or require special equipment. Combining cervical mucus observation with LH testing provides the most accurate and practical way to identify the fertile window and anticipate ovulation.
Learn the finer textures in the Cervical Mucus Decoder.
How can basal body temperature confirm yesterday’s ovulation and refine next month’s plan?
Basal body temperature (BBT) is a valuable tool for confirming that ovulation occurred the previous day. After ovulation, the hormone progesterone causes a woman’s resting temperature to rise by about 0.5–1°F (0.3–0.6°C), creating a clear biphasic pattern on a BBT chart. This temperature shift typically happens within 24 hours after ovulation and remains elevated until the next period, confirming that ovulation has taken place. By charting BBT daily, you can retrospectively pinpoint the day of ovulation as the last low temperature before the sustained rise. While BBT cannot predict ovulation in advance, it reliably confirms that ovulation has already occurred, which is especially useful for understanding your cycle’s timing and length.
Watch for:
• A tiny pre-ovulation dip (≈0.2°F / 0.1 °C) in 1 out of 5 cycles.
• Illness, alcohol, or restless nights, which can skew readings.
• Wearable sensors that log temps automatically, handy for shift workers.
For future planning, several months of BBT charts help you identify your personal ovulation pattern and fertile window, allowing you to better time intercourse for conception or avoidance in subsequent cycles. Recognizing the typical day your temperature rises each month refines your prediction of when ovulation is likely to occur in the next cycle, even though some variability is normal. Digital and wearable BBT devices can make this process easier and more accurate by automatically recording and analyzing temperature trends. However, BBT is best used alongside other ovulation signs or tests, as factors like illness, sleep disturbances, or inconsistent measurement times can affect accuracy. Overall, BBT charting is a practical, low-cost method to confirm ovulation and improve planning for future cycles.
Which hormone-based tools can pinpoint the fertile window within 24–36 hours?
Hormone-based tools that can pinpoint the fertile window within 24–36 hours primarily include urinary ovulation predictor kits (OPKs) and advanced fertility monitors. These devices detect the surge in luteinizing hormone (LH), which typically occurs 24–36 hours before ovulation, making them highly effective for identifying the most fertile days. Some modern monitors, such as the Clearblue Fertility Monitor and Mira Monitor, also measure urinary estrogen metabolites (like estrone-3-glucuronide, E3G) alongside LH, providing a broader fertile window by detecting the estrogen rise that precedes the LH surge. Smartphone-integrated devices and apps, such as Inito and Pearl Fertility, use lateral flow assays to quantify LH and E3G, offering precise, real-time predictions of impending ovulation and confirmation of the fertile window.
Recent innovations include wearable sensors and machine learning algorithms that analyze multiple physiological and hormonal parameters to predict the fertile window with up to 90% accuracy. While serum hormone measurements (estradiol, LH, and progesterone) are the gold standard in clinical settings, at-home urine-based tools remain the most practical and accessible for daily use. Combining LH surge detection with estrogen monitoring or digital integration enhances accuracy, especially for women with irregular cycles or variable ovulation timing. These hormone-based tools are considered the most reliable for pinpointing the fertile window within the critical 24–36 hour timeframe before ovulation.
Quick comparison of a few:
| Tool | Hormones Detected | Predicts or Confirms? | Approx. Cost | Best For |
|---|---|---|---|---|
| Urine OPK strips | LH | Predict | $15–$40 per cycle | Regular cycles |
| Digital LH + E₂ monitor | LH & estrogen | Predict | $120 device + $35 wands | Early warning, irregular cycles |
| Wearable temp sensor | Continuous skin temp | Confirm | $150–$300 | Night-shift users |
| Saliva ferning scope | Electrolyte pattern | Predict (variable) | $25–$40 | Budget backup |
Don’t fall for the myth that “apps alone are enough”—see Fertility Myths Debunked for the evidence.
What if your cycles are irregular, PCOS-affected, or postpartum—can you still trust the signs?
Yes, but layer methods.
Irregular Cycles: When menstrual cycles are irregular, the classic fertility signs such as changes in cervical mucus, basal body temperature (BBT), and ovulation predictor kits can be less predictable and harder to interpret. Ovulation may not occur every cycle, and the timing can vary widely, making it challenging to pinpoint the fertile window using standard methods. However, careful daily tracking of cervical mucus and BBT over several months can still reveal patterns, even if they are less regular, and combining these with hormone-based ovulation tests can improve accuracy. For those with persistent irregularity, consulting a healthcare provider is important to rule out underlying conditions and to discuss tailored fertility monitoring strategies.
PCOS-Affected Cycles: Polycystic ovary syndrome (PCOS) often causes chronic irregular cycles, anovulation (cycles without ovulation), and hormonal imbalances, which can make traditional fertility signs unreliable. Women with PCOS may have persistently high LH levels, making ovulation predictor kits less accurate, and their cervical mucus and BBT patterns may not follow typical cycles. Despite these challenges, some women with PCOS can still detect ovulation by combining multiple signs and using advanced hormone monitors that track both estrogen and LH. Medical management, lifestyle changes, and sometimes medications like metformin or ovulation inducers may be needed to restore more predictable ovulation and improve the reliability of fertility signs.
Postpartum Cycles: After childbirth, cycles can remain irregular for months, especially if breastfeeding, due to hormonal suppression of ovulation. Fertility signs such as cervical mucus and BBT may be inconsistent or absent, and ovulation can return unpredictably. While some women notice a gradual return of fertile-type cervical mucus before their first postpartum ovulation, others may not have clear signs until after cycles normalize. Patience and consistent tracking are key, and using a combination of signs; along with professional guidance if needed can help identify the return of fertility.
In all these scenarios, individualized approaches and, when necessary, medical support are crucial for interpreting fertility signs and optimizing conception chances. Red flags such as cycles shorter than 21 days or longer than 35 days merit a check of your Ovarian Reserve Explained.
When—and how often—should partners have sex for peak conception odds?
To maximize the chances of conception, couples should focus on both the timing and frequency of intercourse. The fertile window spans the six days ending on the day of ovulation, and conception is most likely if intercourse occurs during this period. Because ovulation timing can vary from cycle to cycle, having sex every one to two days throughout the cycle, especially during the fertile window, ensures that sperm are present when the egg is released, optimizing pregnancy chances. Studies show that higher intercourse frequency is strongly associated with increased fecundability: couples who have sex several times per week (at least two to three times) conceive faster than those with less frequent intercourse. In fact, the probability of conception rises with frequency, with the highest rates seen in couples having intercourse seven to eight times per week, though more than two to three times weekly is generally sufficient for most.
Timed intercourse, specifically during the fertile window, further boosts the odds, but even without precise timing, regular sex every two to three days is recommended to avoid missing the fertile days, especially if cycles are irregular or ovulation is unpredictable. Biological factors, such as increased libido around ovulation, may naturally encourage more frequent intercourse during the fertile window. Other factors like age, duration of marriage, and lifestyle can influence sexual frequency, but the most important modifiable factor is how often couples have sex. In summary, for peak conception odds, couples should aim for intercourse every one to two days during the fertile window, or at least two to three times per week throughout the cycle, to ensure sperm are always available when ovulation occurs.
Protect sperm quality: use sperm-friendly lubricants, skip hot tubs, and give briefs a break 72 hours before ovulation. For a deeper dive into semen health, visit Sperm Health 101.
Which lifestyle tweaks sharpen ovulation signals and overall fertility?
Several lifestyle adjustments can sharpen ovulation signals and boost overall fertility.
- Maintaining a healthy weight is crucial, as both obesity and being underweight can disrupt hormonal balance and ovulation; even modest weight loss in overweight women significantly improves ovulation rates and fertility.
- Regular physical activity, especially when combined with dietary changes, enhances insulin sensitivity, reduces central fat, and normalizes reproductive hormones, all of which help restore regular ovulation. This is particularly effective for women with PCOS or those who are overweight.
- Adopting a “fertility diet” rich in monounsaturated fats, plant-based proteins, low-glycemic carbohydrates, high-fat dairy, multivitamins, and plant-based iron is associated with a lower risk of ovulatory infertility.
- Avoiding smoking, excessive alcohol, and recreational drugs is important, as these substances negatively impact both ovulation and overall fertility in men and women.
- Managing stress and ensuring adequate sleep may also support reproductive health, though evidence is less robust compared to diet and exercise.
- Environmental exposures such as to endocrine-disrupting chemicals or excessive heat should be minimized when possible, as they can impair fertility.
- For men, similar lifestyle changes like healthy diet, regular exercise, weight management, and avoiding toxins improve sperm quality and reproductive outcomes.
In summary, a combination of balanced nutrition, regular moderate exercise, weight control, avoidance of harmful substances, and attention to environmental and psychological health can sharpen ovulation signals and significantly improve fertility for most individuals. Build a baby-ready body at Uterine Environment 101.
What red flags suggest you’re not ovulating—and when should you call a specialist?
Red flags that suggest you may not be ovulating include:
Menstrual cycles consistently shorter than 21 days or longer than 35 days, or cycles that are highly unpredictable. In adolescents, cycles outside 21–45 days are also concerning if persistent for over a year.
Missing periods (amenorrhea) or very infrequent periods (oligomenorrhea) and Unusually light, heavy, or erratic bleeding patterns.
Lack of typical ovulation symptoms, such as mid-cycle cervical mucus changes or premenstrual breast tenderness.
Difficulty confirming ovulation with home ovulation predictor kits or basal body temperature tracking.
Signs of excess androgens, such as increased facial/body hair (hirsutism), severe acne, or scalp hair thinning, which may indicate polycystic ovary syndrome (PCOS).
Unexplained weight gain, especially with other symptoms above.
You should see a reproductive specialist if:
- You have any of these symptoms for more than three months.
- You have been trying to conceive for 12 months (or 6 months if you are over 35).
- You have a history of PCOS, thyroid disorders, or other hormonal conditions.
- You experience abnormal uterine bleeding or amenorrhea that does not resolve.
According to the American College of Obstetricians and Gynecologists (ACOG), “Persistent menstrual cycles outside the 21–35 day range, or cycles that are unpredictable, are a strong indicator of ovulatory dysfunction and warrant further evaluation” (ACOG Practice Bulletin, 2023). About 30% of infertility cases are due to ovulation disorders, but many respond well to treatment. Early evaluation and intervention can improve your chances of conception and help address underlying health issues.
As Dr. R. Rosenfield, MD, a leading pediatric endocrinologist, notes: “Continued menstrual abnormality in a hyperandrogenic adolescent for 1 year prognosticates at least 50% risk of persistence”. If you notice these red flags, seeking timely care is the best step for your reproductive health.
Expect tests like AMH, FSH, or luteal-phase progesterone, plus ultrasound follicle tracking—topics explained in The Luteal Phase.
Your top ovulation questions—answered fast
How can I tell ovulation is over?
Ovulation is typically over when your most fertile cervical mucus (clear, stretchy, egg-white-like) dries up or becomes sticky, and your basal body temperature rises and stays elevated for several days. Some people notice a drop in ovulation symptoms, such as mild pelvic pain or breast tenderness, after ovulation ends.
Can I conceive without noticing any symptoms?
Yes. Many people do not experience noticeable ovulation symptoms, yet can still conceive. Ovulation can occur without obvious signs, and conception is possible as long as intercourse happens during the fertile window.
Does age shift my ovulation day?
Yes. As you age, your cycle length and ovulation timing can change. Ovulation may occur earlier or later in the cycle, and cycles may become shorter, longer, or more irregular, especially after age 35.
Are period-tracker apps alone reliable?
Most period-tracker apps are not highly reliable for predicting ovulation or period start dates, especially if your cycles are irregular. Many apps assume ovulation always happens on day 14, but research shows this is true for only about 24% of cycles. Apps that use your own cycle data over several months are more accurate, but should not be your only method if timing is critical.
Spotting: implantation or ovulation?
Spotting around the middle of your cycle may be ovulation spotting, which is usually light and brief. Spotting about 6–12 days after ovulation could be implantation bleeding, which is also light and short-lived. The timing and context help distinguish the two, but not all spotting is related to ovulation or implantation.
Final Thoughts
Daily ovulation timing is a finely tuned process, guided by both hormonal signals and your body’s internal clock. The surge in luteinizing hormone (LH) that triggers ovulation is closely linked to daily rhythms; typically occurring in the late afternoon or evening, influenced by the brain’s master circadian clock. For most people, ovulation happens about 24–36 hours after the LH surge, and the fertile window spans the five days before and the day of ovulation. Tracking daily changes in LH (using urine tests), estradiol, and cervical mucus can help pinpoint this window, but combining multiple markers is more accurate than relying on LH alone. Follicle size and estradiol levels also rise daily as ovulation approaches, with optimal egg maturity seen when follicles reach 18–22 mm and estradiol is high.
Disruptions to your daily routine like shift work or poor sleep, can interfere with these hormonal rhythms and reduce fertility. While apps and calendar methods are convenient, they often fail to predict the exact ovulation day due to natural cycle variability. For the best results, monitor your body’s daily signals and, if possible, use a combination of hormone tracking and physical signs to identify your most fertile days.
Download our printable symptom calendar and explore Fertility 101 to map your full conception journey. When you understand your daily ovulation signals, you and your partner step into TTC with confidence, hope, and a clearer path to the family you’re dreaming of.
Refeerences
-
Menstrual bleeding, cycle length, and follicular and luteal phase lengths in women without known subfertility: A pooled analysis of three cohorts… Paediatric and perinatal epidemiology. https://doi.org/10.1111/ppe.12644
-
Detection of ovulation, a review of currently available methods. Bioengineering & Translational Medicine, 2, 238 - 246. https://doi.org/10.1002/btm2.10058
-
Confirmation of human ovulation in assisted reproduction using an adhesive axillary thermometer (femSense®). Frontiers in Digital Health, 4. https://doi.org/10.3389/fdgth.2022.930010
-
The use of wearable devices for predicting biphasic basal body temperature to estimate the date of ovulation in women… Journal of thermal biology, 108, 103290. https://doi.org/10.1016/j.jtherbio.2022.103290
-
Consumer wearables and personal devices for tracking the fertile window… American journal of obstetrics and gynecology. https://doi.org/10.1016/j.ajog.2024.05.028
-
Current Advances in Cellular Approaches for Pathophysiology and Treatment of Polycystic Ovary Syndrome. Cells, 12. https://doi.org/10.3390/cells12172189
-
PCOS stratification for precision diagnostics and treatment. Frontiers in Cell and Developmental Biology, 12. https://doi.org/10.3389/fcell.2024.1358755
-
P-441 Frequency of sexual intercourse and fecundability among women trying to conceive in Japan. Human Reproduction. https://doi.org/10.1093/humrep/dead093.789
-
Factors influencing natural fecundity in fertile couples: a survey of puerperae and their partners… Reproductive biomedicine online, 48 6, 103751. https://doi.org/10.1016/j.rbmo.2023.103751
-
Comparative efficacy of exercise, diet and/or pharmacological interventions on BMI, ovulation, and hormonal profile in reproductive-aged women with overweight or obesity: a systematic review and network meta-analysis. Human Reproduction Update, 30, 472 - 487. https://doi.org/10.1093/humupd/dmae008
-
The Diagnosis of Polycystic Ovary Syndrome in Adolescents. Pediatrics, 136, 1154 - 1165. https://doi.org/10.1542/peds.2015-1430