If you are concerned about sperm health and male fertility, you are not alone. Up to half of infertility cases involve male factors, and research shows that sperm quality and quantity have declined in recent decades in the United States and worldwide. Low sperm count is not just a fertility issue; it can also signal broader health concerns, including higher risks for metabolic syndrome, diabetes, and low bone density.
Many factors influence sperm health, including age, genetics, lifestyle, and environmental exposures. Obesity, poor diet, and chronic stress can all negatively affect sperm quality, while healthy habits such as regular exercise and a balanced diet, can improve fertility outcomes. Understanding and addressing these factors empowers you to take proactive steps for your reproductive and overall health.
Advances in sperm testing and research now offer more precise ways to assess fertility and guide treatment. By learning about proven strategies and making informed choices, you can boost your chances of conception and support your long-term well-being.
- Why does sperm health matter for conception and a healthy baby?
- What lifestyle changes deliver the fastest, science-backed boosts to sperm quality?
- Can diet really change sperm in 90 days?
- How much exercise is ideal?
- Does weight loss make a difference?
- What about sleep and stress?
- Which nutrients and supplements are truly proven to enhance sperm parameters?
- What antioxidant “stack” has the best evidence?
- Do minerals matter?
- Are any herbs worth considering?
- What about CoQ10 or L-carnitine?
- How do heat, toxins, and everyday habits silently sabotage sperm—and how can you protect yourself?
- When and how should you test sperm health—and what numbers signal a problem?
- What if lifestyle tweaks aren’t enough to fix sperm issues?
- Quick-fire answers to your top questions on sperm health
- Final thoughts: Your 90-day roadmap to stronger sperm
- References
Why does sperm health matter for conception and a healthy baby?
Sperm health plays a vital role in your ability to conceive and in the lifelong health of your child. Healthy sperm are necessary for fertilization, but their quality also affects embryo development, pregnancy outcomes, and your child’s risk for conditions like obesity, diabetes, and metabolic disorders.
Research shows that paternal factors such as age, diet, body weight, and exposure to toxins, can alter sperm DNA and its epigenetic markers, which are then passed to the embryo at conception. For example, a recent study in Nature found that paternal overweight at conception doubles the risk of obesity in children and compromises their metabolic health, highlighting the direct impact of your health on your future family.
Key reasons sperm health matters for conception and a healthy baby:
- Sperm with damaged DNA or abnormal epigenetic patterns can lead to lower fertility, higher miscarriage rates, and delayed fetal development.
- Your lifestyle choices such as smoking, poor diet, and stress can cause changes in sperm that increase your child’s risk for chronic diseases.
- The seminal fluid, not just the sperm, influences the maternal environment, supporting healthy implantation and fetal growth.
- Improving your health before conception; through a balanced diet, regular exercise, and avoiding harmful exposures can boost both fertility and your child’s long-term well-being.
As Dr. Sarah A. Robertson, Professor of Reproductive Immunology at the University of Adelaide, explains: “A father’s wellbeing at the time of conception influences the development and long-term health of his offspring. Evidence is now emerging that poor paternal lifestyle factors such as diet can modify essential uterine responses, altering fetal development and ultimately long-term offspring health”.
Taking steps to improve your sperm health is a powerful way to support your fertility and give your future child the healthiest possible start.
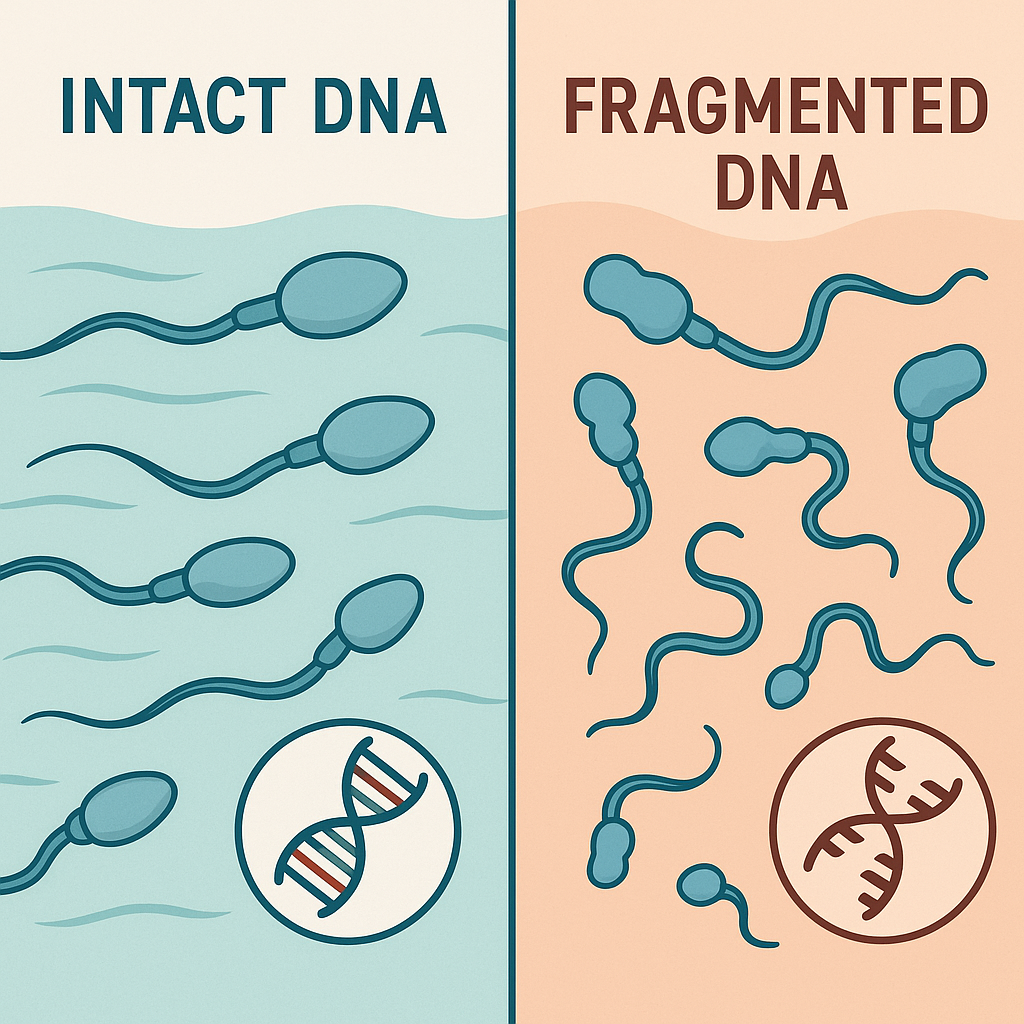
What lifestyle changes deliver the fastest, science-backed boosts to sperm quality?
You can improve sperm quality quickly by adopting a Mediterranean-style diet, engaging in regular moderate exercise, maintaining a healthy weight, and avoiding smoking and excessive alcohol. A four-month intervention with a Mediterranean diet and moderate physical activity led to significant increases in sperm concentration, motility, and normal morphology in healthy young men. Key nutrients such as zinc, selenium, omega-3 fatty acids, and antioxidants are especially beneficial.
Can diet really change sperm in 90 days?
Yes, diet can meaningfully improve sperm quality within about 90 days. Sperm take roughly 74 days to develop, so changes you make now can impact new sperm in three months. Studies show that adopting a balanced, nutrient-rich diet; especially one high in vegetables, fruits, whole grains, fish, nuts, and healthy fats can boost sperm count, motility, and reduce DNA damage in this timeframe.
Key nutrients like zinc, selenium, omega-3 fatty acids, and antioxidants are especially important. Remarkably, even short-term dietary changes can have rapid effects: one study found that sperm motility improved and molecular changes occurred after just two weeks of a healthier diet. The Centers for Disease Control and Prevention (CDC) also recommends a varied, balanced diet for those seeking to improve fertility.
How much exercise is ideal?
Moderate, regular exercise is best for sperm health. Aim for at least 150 minutes per week of moderate-intensity activity, such as brisk walking, cycling, or swimming. A recent systematic review and meta-analysis found that aerobic exercise (both indoor and outdoor), resistance training, and multi-component activities all significantly improved sperm count, motility, and morphology compared to inactivity.
However, excessive or very intense exercise may have negative effects, so balance is key. Regular, moderate exercise not only supports sperm quality but also helps manage weight and reduce inflammation, further supporting fertility.
Does weight loss make a difference?
Yes, weight loss can significantly improve sperm quality, especially if you have overweight or obesity. Obesity is strongly linked to lower sperm concentration, reduced motility, abnormal morphology, and increased DNA damage. Clinical studies show that losing as little as 10–15% of your body weight can increase total sperm count, improve semen volume, and boost testosterone levels.
Reducing abdominal fat also lowers sperm DNA fragmentation and oxidative stress, both of which are important for fertility and healthy pregnancies. In one study, all men who lost abdominal fat saw improvements in sperm quality, and their partners achieved successful pregnancies.
What about sleep and stress?
Both sleep and stress have a measurable impact on sperm health. Poor sleep quality and short sleep duration are associated with lower sperm concentration and motility 91. Chronic stress can further reduce sperm count, motility, and increase the number of abnormal sperm, especially when combined with obesity.
Managing stress through mindfulness, counseling, or relaxation techniques, and aiming for 7–9 hours of quality sleep each night, can help protect and improve your sperm quality. As highlighted in a 2024 review, “Lifestyle modifications including weight management, stress reduction, and improved sleep, can significantly enhance male reproductive health”. Pair these habits with the couple-focused checklist in Fertility 101.
Which nutrients and supplements are truly proven to enhance sperm parameters?
Several nutrients and supplements are strongly supported by clinical evidence for enhancing sperm parameters. The most effective, science-backed options include: zinc, selenium, omega-3 fatty acids, coenzyme Q10 (CoQ10), and carnitines (L-carnitine and acetyl-L-carnitine). Supplementation with these nutrients has been shown to significantly increase sperm concentration, total count, motility (both total and progressive), and morphology. For example, omega-3 fatty acids and CoQ10 produced some of the largest improvements in sperm count and motility, while carnitines were especially effective for motility and morphology.
What antioxidant “stack” has the best evidence?
The antioxidant “stack” with the best evidence for improving sperm quality includes coenzyme Q10 (CoQ10), carnitine, vitamin C, vitamin E, selenium, zinc, and sometimes folic acid. A 2021 network meta-analysis of randomized controlled trials found that CoQ10 was most effective for increasing sperm concentration, while carnitine had the strongest effect on sperm motility; vitamin C ranked highest for improving sperm morphology, though its effect was not always statistically significant. Clinical studies using combinations of these antioxidants such as vitamin C, vitamin E, selenium, zinc, L-carnitine, and CoQ10, have shown significant improvements in sperm concentration, motility, and DNA integrity after 3–6 months of supplementation in men with infertility.
Reviews also highlight that these nutrients work synergistically to reduce oxidative stress, protect sperm DNA, and enhance overall sperm function. However, not all studies find benefits in every population, and results may depend on baseline fertility status and the specific combination and dosage used 1. Overall, the most evidence-based antioxidant stack for sperm health is a combination of CoQ10, carnitine, vitamin C, vitamin E, selenium, and zinc, taken at clinically validated doses for at least three months.
Do minerals matter?
Yes, minerals play a crucial role in sperm quality and male fertility. Strong evidence shows that zinc and selenium are especially important: supplementation with these minerals significantly increases sperm concentration, motility, and normal morphology, and men with infertility often have lower seminal zinc levels than fertile men.
Manganese and iron have also been linked to higher sperm counts and vitality, while copper appears to have a negative effect, reducing sperm vitality and increasing the proportion of slow-moving sperm. Adequate intake of these micro- and macro-minerals improves not only sperm quality but also the antioxidant capacity of seminal fluid, helping to protect sperm from oxidative stress.
Animal studies further confirm that zinc and copper supplementation can enhance sperm production, motility, and integrity by boosting antioxidant enzyme activity and reducing oxidative damage. However, excessive or direct application of minerals can be harmful, so balance and proper dietary intake are key. Overall, maintaining optimal levels of zinc, selenium, manganese, and iron, while avoiding excess copper, supports healthy sperm and male fertility.
Are any herbs worth considering?
Several herbs have been studied for their potential to improve sperm quality, with varying levels of evidence. Meta-analyses and systematic reviews indicate that certain herbs and polyherbal formulations can significantly enhance semen parameters; including sperm concentration, motility, morphology, and semen volume in men with infertility or low sperm counts. Notably, herbs such as Mucuna pruriens, Withania somnifera (ashwagandha), Eurycoma longifolia (tongkat ali), Panax ginseng, Nigella sativa (black seed), and Lepidium peruvianum (maca) have shown positive effects on sperm count, motility, and antioxidant status in both human and animal studies.
Green tea polyphenols, particularly catechins, have demonstrated antioxidant properties that protect sperm from oxidative stress and improve concentration, motility, and DNA integrity. Ginger has also been found to enhance sperm count, motility, viability, and morphology, likely due to its strong antioxidant and androgenic effects, though more clinical trials are needed to confirm safety and optimal dosing in humans.
Polyherbal formulations, as used in traditional medicine systems like Ayurveda and Traditional Chinese Medicine, have produced substantial improvements in sperm parameters and hormone regulation in small clinical trials. However, the evidence for ginseng is mixed, with some studies showing benefits and others finding no clear effect, and overall research quality is limited. Additionally, some dietary herbs and foods recommended in traditional medicine, such as almonds, onions, garlic, and nuts may support sperm health due to their rich content of vitamins, minerals, and phytochemicals, though more rigorous studies are needed.
What about CoQ10 or L-carnitine?
Both CoQ10 (coenzyme Q10) and L-carnitine have strong evidence supporting their benefits for sperm quality and male fertility. Large network meta-analyses and randomized controlled trials show that CoQ10 significantly increases sperm concentration and motility, ranking among the most effective antioxidants for these outcomes. L-carnitine is particularly effective for improving sperm motility and morphology, and also boosts sperm concentration and testosterone levels.
Studies comparing these supplements suggest that L-carnitine may be superior to CoQ10 (even when combined with vitamin E) for overall improvements in sperm parameters, though both are beneficial. When used together, L-carnitine and CoQ10 further enhance sperm motility, reduce DNA fragmentation, and increase clinical pregnancy rates in men with idiopathic infertility.
Supplementation with blends containing CoQ10, L-carnitine, and other antioxidants (like zinc and lycopene) has also led to significant improvements in semen volume, sperm concentration, motility, and morphology. Additionally, these antioxidants help reduce oxidative stress and protect sperm from damage during processes like cryopreservation.
Want to skip hype? Bust supplement myths in Fertility Myths Debunked.
How do heat, toxins, and everyday habits silently sabotage sperm—and how can you protect yourself?
Heat, toxins, and everyday habits can silently sabotage sperm by disrupting the delicate environment needed for healthy sperm production and function. Elevated temperatures such as from heat waves, hot tubs, or tight clothing; impair sperm quality by reducing sperm count, motility, and normal morphology, mainly through oxidative stress, DNA damage, and increased cell death in the testes.
Heat stress also disrupts the balance of beneficial microbes and essential nutrients in the testicular environment, further harming sperm development. Toxins like pesticides, heavy metals, and air pollutants generate reactive oxygen species (ROS) that damage sperm DNA and membranes, while lifestyle habits such as smoking, excessive alcohol, poor diet, and lack of exercise increase oxidative stress and inflammation, compounding the damage to sperm quality and fertility. These factors can have both immediate and long-term effects, with some damage persisting for weeks after exposure.
To protect sperm health, it is important to minimize exposure to heat and toxins and adopt healthy daily habits. Practical steps include wearing loose-fitting underwear, avoiding prolonged exposure to high temperatures (like hot tubs or saunas), and seeking shade or air conditioning during heat waves. Improving ventilation and cooling in living and working environments, especially in hot climates, can also help. Reducing exposure to environmental toxins by choosing organic foods, avoiding unnecessary chemicals, and not smoking; lowers the risk of sperm damage.
A diet rich in antioxidants (from fruits, vegetables, and supplements like vitamins C and E, melatonin, or L-arginine) can help counteract oxidative stress and support sperm quality. Regular exercise, maintaining a healthy weight, and managing stress further protect reproductive health. In some cases, targeted supplements or medical interventions may be recommended to restore sperm quality after heat or toxin exposure.

When and how should you test sperm health—and what numbers signal a problem?
Sperm health should be tested when a couple has been trying to conceive for a year without success, or after six months if the female partner is over 35, or sooner if there are known risk factors such as a history of testicular problems, chemotherapy, or genital surgery. Early testing is also recommended if there are symptoms like erectile dysfunction, low libido, or a history of undescended testicles, as these can indicate underlying fertility issues. Testing may also be considered before starting fertility treatments or if there is a family history of genetic disorders affecting reproduction.
Sperm health is typically assessed through a semen analysis, which measures key parameters such as sperm concentration (count), motility (movement), and morphology (shape), following World Health Organization (WHO) guidelines. Advanced methods, including computer-assisted sperm analysis (CASA) and flow cytometry, can provide more detailed information on sperm motility, viability, membrane integrity, and DNA fragmentation. Functional tests, such as the sperm penetration assay, acrosome reaction, and binding assays, may be used in specialized cases to predict fertilization potential, especially when initial results are abnormal or assisted reproduction is being considered. These tests are performed in a laboratory setting, usually after a period of 2–7 days of sexual abstinence.
Normal semen analysis values, according to WHO, are a sperm concentration above 15 million per milliliter, total motility above 40%, and at least 4% of sperm with normal morphology. Results below these thresholds such as low sperm count (oligozoospermia), poor motility (asthenozoospermia), or abnormal morphology (teratozoospermia) signal a potential problem and may warrant further investigation or treatment. However, sperm morphology assessment can be variable and sometimes less reliable, so results should be interpreted alongside other parameters and clinical context. High levels of sperm DNA fragmentation or poor results on functional tests may indicate a higher risk of infertility or poor outcomes with natural conception and some assisted reproductive techniques.
Consider sperm banking if delaying fatherhood. Coordinate testing with cycle insights in Egg vs. Sperm Lifespan.
What if lifestyle tweaks aren’t enough to fix sperm issues?
If lifestyle changes alone aren’t enough to resolve sperm issues, several medical and technological options are available. Medical treatments can include hormone therapies such as selective estrogen receptor modulators, gonadotropins, and aromatase inhibitors, which have been shown to improve sperm production, motility, and even pregnancy rates in some cases. Antioxidant supplements (like vitamins E and C, coenzyme Q10, and omega-3s) can further reduce oxidative stress and improve sperm DNA integrity, especially when combined with lifestyle interventions.
For men with severe testicular failure or nonobstructive azoospermia, advanced options like microsurgical testicular sperm extraction (micro-TESE) and assisted reproductive technologies (ART) such as in vitro fertilization (IVF) with intracytoplasmic sperm injection (ICSI) can enable biological paternity, even in cases previously considered untreatable. Newer sperm separation technologies, which minimize DNA damage during preparation for ART, are also showing promise in improving outcomes.
Ultimately, if sperm abnormalities persist despite healthy lifestyle changes, a combination of medical therapies, targeted supplements, and advanced reproductive technologies can significantly improve the chances of conception. It is important to work closely with a fertility specialist to identify the underlying cause and select the most appropriate treatment, as some cases may require genetic testing or specialized interventions. While these approaches can be effective, ongoing research is needed to refine treatments and ensure the health of both parents and future children. For implantation details after lab help, see Implantation Timeline.
Quick-fire answers to your top questions on sperm health
Can I really improve sperm in a week?
Significant improvements in sperm quality usually take longer than a week, as sperm development (spermatogenesis) takes about 2–3 months. While some antioxidant supplements or dietary changes may help reduce oxidative stress quickly, noticeable changes in sperm count or motility generally require several weeks of consistent healthy habits.
What’s the best drink for sperm?
Green tea and other antioxidant-rich beverages may benefit sperm health. Studies show that regular green tea consumption is associated with higher sperm concentration and vitality, and long-term, frequent tea drinking can improve sperm quality. Water is always a good choice, while excessive alcohol should be avoided, as heavy drinking can reduce semen volume and lower reproductive hormone levels.
Is thin semen bad?
Thin semen is not always a sign of a problem, as semen consistency can vary with hydration, frequency of ejaculation, and other factors. However, persistently watery or very low-volume semen may indicate low sperm count or other reproductive issues and should be evaluated if conception is difficult.
Does underwear type matter?
Yes, underwear type can affect sperm health. Tight underwear can increase scrotal temperature, which may reduce sperm count and motility over time. Looser-fitting underwear, like boxers, is generally recommended for optimal sperm production.
How often should we have sex when TTC?
When trying to conceive (TTC), having sex every 1–2 days during the fertile window (the days leading up to and including ovulation) maximizes the chances of pregnancy. Frequent ejaculation does not harm sperm quality in healthy men and can actually help ensure fresh, motile sperm are available. For luteal-phase insights afterward, visit The Luteal Phase.
Final thoughts: Your 90-day roadmap to stronger sperm
A 90-day roadmap to stronger sperm centers on consistent lifestyle improvements and targeted supplementation, as this timeframe matches the full cycle of sperm development. Clinical studies show that combining healthy habits such as a balanced diet, regular exercise, and stress reduction with specific supplements like antioxidants, vitamins (E, C, folic acid), minerals (zinc, selenium), and omega-3 fatty acids can significantly improve sperm count, motility, and membrane integrity within three months. Herbal remedies, such as carrot seed extract, when combined with medical therapies and lifestyle education, have also demonstrated notable improvements in sperm parameters without adverse effects over 90 days.
Micronutrient supplementation, especially when paired with medications like phosphodiesterase inhibitors, can further enhance sperm motility and function. While some nutrients, like low-dose folic acid, may not alter sperm DNA methylation in the short term, overall sperm quality and function benefit from a comprehensive, sustained approach.
The key is daily commitment: maintain a nutrient-rich diet, avoid smoking and excessive alcohol, manage weight, and consider evidence-based supplements. Regular follow-up with a healthcare provider ensures progress and allows for adjustments if needed. With patience and consistency, most men can expect measurable improvements in sperm health by the end of 90 days.
Download our printable “90-Day Sperm Health Checklist” and continue your fertility journey with Fertility 101. You’ve got this—every smart choice today builds the family you dream of tomorrow.
References
-
Epigenetic inheritance of diet-induced and sperm-borne mitochondrial RNAs. Nature, 630, 720 - 727. https://doi.org/10.1038/s41586-024-07472-3
-
The influence of seminal plasma on offspring development and health… Seminars in cell & developmental biology. https://doi.org/10.1016/j.semcdb.2019.06.008
-
Influence of Age, Obesity, Smoking, Sleep duration and Sleep Quality on Concentration, Morphology, and Sperm Motility: A Cross-Sectional Study. International Journal of Fertility & Sterility, 18, 240 - 247. https://doi.org/10.22074/IJFS.2023.1983273.1413
-
Can lifestyle changes significantly improve male fertility: A narrative review?. Arab Journal of Urology. https://doi.org/10.1080/20905998.2024.2421626
-
Effectiveness of exercise interventions on sperm quality: a systematic review and network meta-analysis. Frontiers in Endocrinology, 16. https://doi.org/10.3389/fendo.2025.1537271
-
Effectiveness and tolerability of a novel blend of coq10, l-carnitine, zinc, lycopene, and astaxanthin in males with infertility: Findings from a UNESCO study. International Journal of Clinical Obstetrics and Gynaecology. https://doi.org/10.33545/gynae.2023.v7.i6a.1393
-
Sperm morphology: assessment, pathophysiology, clinical relevance, and state of the art in 2017. Andrology, 5. https://doi.org/10.1111/andr.12389
-
The effect of healthy dietary patterns on male semen quality: a systematic review and meta-analysis. Asian Journal of Andrology, 24, 549 - 557. https://doi.org/10.4103/aja202252
-
Micronutrient–Antioxidant Therapy and Male Fertility Improvement During ART Cycles. Nutrients, 17. https://doi.org/10.3390/nu17020324
-
Beneficial effects of oral antioxidant supplementation on semen quality parameters, reproductive hormones, and sperm DNA integrity in men with idiopathic oligoasthenoteratozoospermia. Clinical and Experimental Reproductive Medicine, 51, 135 - 141. https://doi.org/10.5653/cerm.2023.06555
-
The effect of antioxidant supplementation on sperm quality in infertile men: a randomized placebo-controlled clinical trial. Human Reproduction. https://doi.org/10.1093/humrep/deae108.467
-
The role of oral antioxidants in the improvement of sperm parameters in infertile men. World Journal of Urology, 42, 1-6. https://doi.org/10.1007/s00345-023-04766-5
-
Correlation of Dietary Macro- and Micro-Mineral Intake with Seminal Plasma Quality/Quantity and Oxidant/Antioxidant Status in Infertile Compared to the Normal Men: a Case-Control Study… Biological trace element research. https://doi.org/10.1007/s12011-023-03834-6
-
Protective effect of herbal medicine on murine spermatogenesis under heat stress and other injury models: Evidence from meta-analyses. Journal of Animal Behaviour and Biometeorology. https://doi.org/10.31893/jabb.2025007
-
Effectiveness of Herbal medicines on male reproductive system: Evidence from meta-analysis. Pharmacological Research - Modern Chinese Medicine. https://doi.org/10.1016/j.prmcm.2024.100462