Did you know a uterine lining thinner than 7 mm can slice implantation odds in half? You are not alone if you’re concerned about how your uterine environment affects your fertility. In the United States, up to 15% of couples face infertility, and research shows that the health of your uterus plays a crucial role in conception and pregnancy success. Factors like hormone balance, immune health, and even the community of bacteria in your uterus can influence whether an embryo implants and grows as it should.
Modern science has revealed that the uterus is not a sterile space. Instead, a healthy balance of bacteria, especially those from the Lactobacillus family, can support a receptive, baby-ready endometrium. Disruptions in this environment, whether from stress, obesity, environmental toxins, or infections, may make it harder to conceive or carry a pregnancy to term. Understanding and nurturing your uterine environment is a powerful step you can take on your fertility journey.
- What does a baby-ready uterus actually look like?
- How does each phase of your cycle help—or hurt—the uterine lining?
- Which foods and nutrients truly nourish the endometrium?
- How can movement and circulation upgrade your uterine “home”?
- Which hidden toxins quietly sabotage uterine health?
- Does stress, sleep, and mindset really change implantation odds?
- When is it time to go beyond lifestyle tweaks?
- How do you track progress and confirm your uterus is move-in ready?
- Do partner habits influence the uterine environment?
- What exciting research is emerging right now?
- Your Top Questions, Answered
- Final Thoughts
- References
What does a baby-ready uterus actually look like?
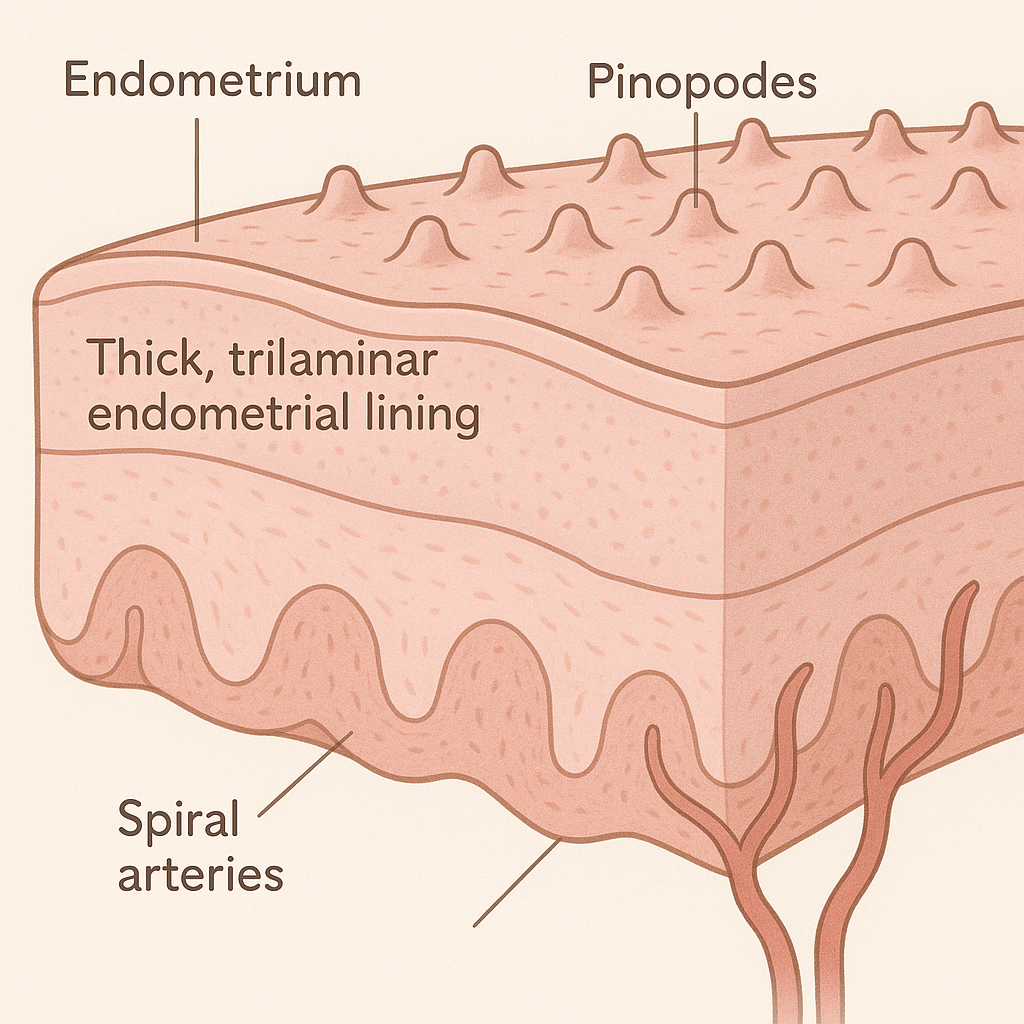
A baby-ready uterus is one that offers a welcoming, balanced environment for an embryo to implant, grow, and thrive. This means your endometrium—the lining of your uterus—should be receptive, with the right thickness, blood flow, and hormone signals to support early pregnancy. Healthy vascular remodeling, where blood vessels adapt to nourish the embryo, is essential for preventing pregnancy loss and ensuring the embryo receives enough oxygen and nutrients.
Your immune system also plays a key role. A baby-ready uterus maintains immune tolerance, allowing your body to accept the embryo while still protecting against infection. Specialized immune cells, including tolerogenic B cells and regulatory T cells, help create this balance. Additionally, a healthy uterine microbiome, dominated by beneficial bacteria like Lactobacillus, supports implantation and reduces the risk of inflammation or infection that could disrupt pregnancy. In short, a baby-ready uterus is hormonally synchronized, immune-tolerant, well-nourished, and microbially balanced, giving you the best chance for a healthy pregnancy.
How does each phase of your cycle help—or hurt—the uterine lining?
During menstruation, your uterine lining sheds and exits your body. This process is triggered by a drop in progesterone and marks the start of a new cycle. While this phase clears out the old lining, it also creates a temporary “wounded” surface that must quickly repair itself to prepare for the next opportunity for pregnancy.
In the proliferative (follicular) phase, rising estrogen levels stimulate your endometrium to regrow and thicken. This rebuilding is crucial: a healthy, well-structured lining is needed for an embryo to implant. The proliferative phase is marked by active cell growth and unique gene expression patterns that set the stage for later receptivity. Track ovulation signs with the tips in Ovulation Signals to catch the surge that drives lining proliferation.
Ovulation marks the release of an egg and a shift in hormones. The uterine lining continues to mature, becoming more receptive to a potential embryo. Blood flow to the uterus increases, supporting further growth and preparing the endometrium for possible implantation.
In the luteal (secretory) phase, progesterone from the ovary transforms the thickened lining into a nutrient-rich, embryo-friendly environment. The endometrium becomes more stable and receptive, with subtle changes in gene activity and immune function. If pregnancy does not occur, hormone levels fall, and the cycle begins again with menstruation. An under-powered luteal phase can cut implantation chances in half; learn more in the Luteal Phase guide.
Which foods and nutrients truly nourish the endometrium?
To truly nourish your endometrium, focus on foods and nutrients that support hormone balance, reduce inflammation, and provide antioxidants. Diets rich in fruits, vegetables, whole grains, legumes, and healthy fats, like those found in the Mediterranean or anti-inflammatory diet, are linked to better endometrial health and lower risk of endometriosis. Omega-3 fatty acids from fish, nuts, and seeds help reduce inflammation, while vitamins C, D, and E, along with polyphenols and minerals like calcium and magnesium, offer antioxidant protection and support tissue repair.
Dairy products, especially when consumed in moderation, may lower endometriosis risk, while high intake of red meat, trans fats, and saturated fats is associated with increased risk and inflammation. Plant-based proteins and dietary fiber can help regulate estrogen levels, which is crucial for a healthy uterine lining. Seaweed and certain micronutrients may also help modulate estrogen and reduce symptoms. In summary, a balanced, nutrient-dense diet, rich in plant foods, healthy fats, and key vitamins and minerals, can help create an optimal environment for your endometrium and support your fertility goals.

How can movement and circulation upgrade your uterine “home”?
Regular movement and healthy circulation are powerful ways to upgrade your uterine “home.” Physical activity, especially when tailored to your needs, helps maintain or even improve blood flow to the uterus without causing harm. Moderate and vigorous exercise, as recommended by health guidelines, does not reduce uterine artery blood flow and may even lower resistance in these vessels, supporting better delivery of oxygen and nutrients to your endometrial lining.
Good circulation is essential for the growth and remodeling of uterine blood vessels, a process that prepares your uterus for pregnancy by increasing its capacity to nourish an embryo. Hormones like estrogen and progesterone, released during your cycle and boosted by movement, help relax and expand these vessels, further enhancing blood flow. Improved blood flow also supports the removal of waste products and reduces inflammation, creating a healthier environment for implantation and early development.
Which hidden toxins quietly sabotage uterine health?
Several hidden toxins can quietly sabotage uterine health by disrupting hormones, increasing inflammation, and damaging reproductive tissues. Common culprits include endocrine-disrupting chemicals like phthalate esters and bisphenol A (BPA), which are found in plastics, personal care products, and food packaging. These chemicals can mimic estrogen in your body, promoting the growth of uterine fibroids and interfering with normal uterine function. Heavy metals such as cadmium, lead, and mercury are also linked to uterine toxicity; they can trigger oxidative stress, inflammation, and even alter muscle activity in the uterus, sometimes without obvious symptoms.
Persistent organic pollutants, pesticides, and microplastics are increasingly recognized for their negative effects on fertility and uterine health, often acting through hormone disruption or by accumulating in body tissues over time. Mycotoxins like zearalenone and HT-2, which can contaminate grains and food crops, have been shown to alter the gut microbiome, increase uterine inflammation, and disrupt early reproductive processes, even affecting the fertility of future generations. Tobacco smoke and occupational exposures to solvents or industrial chemicals further add to the risk, with some toxins causing subtle epigenetic changes that may not show up until later in life.
These toxins often work together, making their effects difficult to detect but potentially significant for your reproductive health. Reducing exposure, by choosing fresh foods, avoiding plastics when possible, and being mindful of environmental and occupational hazards, can help protect your uterine environment and support your fertility.
For more myth-busting on environmental exposures, see Fertility Myths Debunked.
Does stress, sleep, and mindset really change implantation odds?
Stress can negatively impact implantation odds by disrupting hormonal balance and increasing inflammation in the body. Women undergoing fertility treatments often experience high levels of perceived stress, which has been shown to impair sleep quality and may interfere with the delicate hormonal environment needed for successful embryo implantation. Chronic or acute stress activates the hypothalamic-pituitary-adrenal (HPA) axis, leading to elevated cortisol levels that can further disrupt reproductive processes and reduce the likelihood of implantation.
Sleep quality is closely linked to both stress and reproductive health. Poor sleep, whether due to stress or other factors, heightens the reactivity of the HPA axis, making the body more sensitive to stress and potentially exacerbating hormonal imbalances that can hinder implantation. Persistent sleep disturbances can also have long-term effects on the body’s ability to maintain a healthy reproductive environment.
Mindset plays a powerful role in shaping how stress affects the body. Interventions that promote a growth mindset and teach individuals to view stress as potentially enhancing, rather than purely harmful, have been shown to improve psychological well-being, reduce anxiety, and even modulate physiological stress responses. These mindset shifts can help individuals cope better with the emotional challenges of fertility treatments, potentially supporting a more favorable environment for implantation.
When is it time to go beyond lifestyle tweaks?
It’s time to go beyond lifestyle tweaks and seek medical evaluation for infertility if you have been trying to conceive for 12 months or more with regular, unprotected intercourse and are under age 35, or after 6 months if you are 35 or older. Immediate evaluation is also warranted at any age if you have known risk factors such as irregular periods, a history of pelvic infections, endometriosis, or if your partner has known fertility issues. Women over 40 should seek prompt assessment and treatment, as fertility declines rapidly with age. Both partners should be evaluated, since male factors contribute to infertility in up to half of cases.
Medical intervention may include diagnostic tests to assess ovulation, ovarian reserve, tubal patency, and semen quality, followed by treatments such as ovulation induction, intrauterine insemination (IUI), or in vitro fertilization (IVF), depending on the underlying cause and age. For unexplained infertility, initial cycles of ovarian stimulation or IUI may be tried, but IVF is often considered if these are unsuccessful, especially for women over 38.
If you have a condition known to cause infertility, such as polycystic ovary syndrome or severe male factor infertility, early or immediate specialist referral is recommended. In summary, if lifestyle changes have not led to pregnancy within the recommended timeframes or if you have risk factors, it’s important to seek medical advice to identify and address any underlying issues.
How do you track progress and confirm your uterus is move-in ready?
Tracking progress and confirming your uterus is “move-in ready” for implantation involves a combination of imaging, molecular, and minimally invasive tests. Traditionally, transvaginal ultrasound is used to assess endometrial thickness, texture, and blood flow, with a “triple-layered” appearance and good subendometrial blood flow linked to higher implantation rates. Doppler ultrasound can further evaluate uterine and subendometrial artery resistance, as lower resistance and better vascularization are associated with improved receptivity.
Beyond imaging, molecular markers in uterine fluid or menstrual blood—such as specific proteins, cytokines, and small non-coding RNAs—are emerging as powerful tools to assess endometrial receptivity with high sensitivity and specificity, often without the need for invasive biopsies. For example, profiling proteins or RNAs in uterine fluid can help pinpoint the optimal “window of implantation” and identify subtle issues that might hinder embryo attachment. Additionally, measuring endometrial tissue blood flow directly has been shown to be a strong predictor of successful implantation, sometimes outperforming traditional ultrasound markers.
These advances allow for more personalized and precise monitoring, helping you and your care team confirm when your uterine environment is most receptive and ready for embryo implantation.
Low-tech clues still help: stretchy, egg-white cervical mucus (decode it with the Cervical Mucus Decoder) and a stable basal body temperature shift.
Do partner habits influence the uterine environment?
Yes, partner habits can influence the uterine environment and affect fertility outcomes. Seminal fluid from the male partner plays an active role in preparing the uterus for implantation by triggering immune and vascular changes in the endometrial tissue, which can enhance or impair uterine receptivity depending on its composition and the timing of exposure.
Lifestyle factors such as smoking, alcohol consumption, and diet in the male partner can impact sperm quality and seminal fluid composition, which in turn may affect embryo implantation and pregnancy rates. For example, smoking is associated with reduced uterine receptiveness and lower pregnancy rates, while excessive alcohol intake and poor dietary habits in the male partner are linked to lower sperm quality and decreased fertilization and implantation success.
Additionally, certain sexual and social behaviors may influence the risk of uterine conditions through shared hormonal and immune pathways, although direct causal links are still being explored. Overall, both partners’ habits; especially those related to smoking, alcohol, and nutrition, can quietly shape the uterine environment and the chances of a successful pregnancy. For a deep dive, visit Sperm Health 101.
What exciting research is emerging right now?
Exciting research in uterine health and implantation is rapidly advancing thanks to new technologies and deeper molecular insights.
Scientists are now using endometrial organoids (miniature, lab-grown versions of the uterine lining) to closely mimic natural tissue and study how hormones, genes, and embryos interact during implantation. These organoids, combined with powerful “omics” tools (like single-cell RNA sequencing), are revealing the complex signaling pathways and cellular changes that make the uterus receptive to an embryo. Innovative “implantation-on-a-chip” platforms are also allowing researchers to model the early stages of embryo attachment and invasion in the lab, providing new ways to study immune cell roles and test treatments.
There’s growing interest in how the uterine and vaginal microbiome, especially the presence of beneficial Lactobacillus bacteria, affects endometrial receptivity and the risk of repeated implantation failure or pregnancy loss. On the clinical front, uterus transplantation is emerging as a groundbreaking option for women with absolute uterine factor infertility, offering the possibility of biological motherhood where it was previously impossible.
Meanwhile, researchers are mapping the genetic and immune factors that underlie common uterine disorders, aiming to develop more targeted therapies to improve implantation and early pregnancy outcomes. Together, these advances are paving the way for more personalized, effective fertility treatments and a better understanding of what makes the uterus truly “move-in ready” for pregnancy.
Your Top Questions, Answered
How fast can I improve my lining?
Endometrial lining can sometimes be improved within a few days to a week, especially with targeted medical interventions. For example, intrauterine administration of granulocyte colony-stimulating factor (G-CSF) in women with thin, unresponsive endometrium has been shown to increase thickness significantly within 48–72 hours, leading to better pregnancy rates. Standard treatments like estrogen supplementation, sildenafil, and other medications may also help, but the speed and degree of improvement vary by individual. In general, a lining of at least 7–10 mm is considered optimal for embryo transfer, with live birth rates plateauing above this range.
Are castor-oil packs effective?
There is currently no high-quality scientific evidence supporting the use of castor-oil packs to improve endometrial thickness or fertility outcomes. Most research and clinical guidelines do not include castor-oil packs as a recommended intervention for preparing the uterus for implantation.
Is bed rest helpful after embryo transfer?
Bed rest after embryo transfer is not supported by evidence and does not improve implantation or pregnancy rates. In fact, studies suggest that immediate resumption of normal activities is safe and may even be preferable, as prolonged bed rest can increase stress and discomfort without any proven benefit.
Does eating pineapple core boost implantation?
The idea that eating pineapple core can boost implantation is a popular myth, but there is no scientific evidence to support this claim. While pineapple contains bromelain, an enzyme thought to have anti-inflammatory properties, no clinical studies have shown that consuming pineapple or its core improves endometrial receptivity or pregnancy rates. For optimal results, focus on evidence-based medical and lifestyle interventions.
Final Thoughts
Building a “baby-ready” uterine environment is about more than just achieving the right thickness of the endometrial lining, it requires a harmonious interplay of tissue remodeling, immune balance, and molecular signaling. Recent research shows that remodeling the uterine extracellular matrix, for example through controlled enzymatic treatments, can release growth factors and improve blood vessel formation, directly enhancing the uterus’s ability to support embryo implantation.
The immune system, particularly regulatory T cells and innate immune cells, must strike a careful balance between inflammation and tolerance to create a welcoming environment for the embryo. Lifestyle factors, such as stress reduction and environmental enrichment, can also promote healthy vascular remodeling and reduce the risk of embryo loss. Advances in imaging and organoid technology are now allowing scientists to visualize and study the three-dimensional structure and function of the endometrium in unprecedented detail, helping to identify subtle abnormalities and test new therapies.
Ultimately, optimizing the uterine environment means orchestrating a complex set of biological processes to create the best possible home for a developing embryo, and ongoing research continues to uncover new strategies for making this “home” as welcoming as possible.
Download our printable checklist inside Fertility 101 and start furnishing your baby’s very first home today—because the journey to parenthood begins from the inside out.
References
-
Enhancing uterine receptivity for embryo implantation through controlled collagenase intervention. Life Science Alliance, 7. https://doi.org/10.1101/2022.01.18.476712
-
Cellular Regulation of the Uterine Microenvironment That Enables Embryo Implantation. Frontiers in Immunology, 6. https://doi.org/10.3389/fimmu.2015.00321
-
The Role of Inflammation for a Successful Implantation. American Journal of Reproductive Immunology, 72, 141 - 147. https://doi.org/10.1111/aji.12266
-
Maternal exposure to an enrichment environment promotes uterine vascular remodeling and prevents embryo loss in mice… Reproduction. https://doi.org/10.1530/REP-21-0297
-
Insights from imaging the implanting embryo and the uterine environment in three dimensions. Development, 143, 4749 - 4754. https://doi.org/10.1242/dev.144386
-
Revolutionizing Implantation Studies: Uterine-Specific Models and Advanced Technologies. Biomolecules, 15. https://doi.org/10.3390/biom15030450
-
A critical appraisal of studies on endometrial thickness and embryo transfer outcome… Reproductive biomedicine online, 47 4, 103259. https://doi.org/10.1016/j.rbmo.2023.103259
-
O-026 RCT of INTRA - Uterine administration of granulocyte colony-stimulating factor (G-CSF) before embryo-transfer in resistant thin endometrium in IVF-ICSI cycles. Human Reproduction. https://doi.org/10.1093/humrep/deac104.026
-
Endometrial pattern, but not endometrial thickness, affects implantation rates in euploid embryo transfers… Fertility and sterility, 104 3, 620-8.e5. https://doi.org/10.1016/j.fertnstert.2015.05.036
-
Optimal endometrial thickness in fresh and frozen-thaw in vitro fertilization cycles: an analysis of live birth rates from 96,000 autologous embryo transfers… Fertility and sterility. https://doi.org/10.1016/j.fertnstert.2021.12.025