You want reliable, easy-to-use tools to help track your fertility. Couples who monitor basal body temperature with a connected device conceive up to 2× faster than those who guess their fertile days. Traditional methods, like daily basal body temperature (BBT) checks, can be inconvenient and prone to error, especially with busy schedules or disrupted sleep patterns.
Smart thermometers and wearables offer a practical solution. These devices automatically record your temperature and other physiological signals, syncing data to your phone for simple, real-time tracking. Recent studies show that smart thermometers and wrist or ear wearables can detect ovulation and fertile windows with high accuracy, often outperforming manual methods.
This technology is especially helpful if you want a compassionate, gender-inclusive approach to family planning; giving you more control and confidence in your fertility journey. Below, you’ll find an evidence-based guide to choosing and using the best smart thermometer for your fertility journey.
- Why does basal body temperature matter when you’re trying to get pregnant?
- How are smart thermometers different from regular digital or classic basal models?
- Which smart thermometers rank highest for easy, accurate cycle tracking in 2025?
- Which features should top your checklist before you buy?
- Do wearables outshine stick thermometers for irregular cycles, shift work, or PCOS?
- Are these devices truly evidence-backed and FDA-cleared?
- How much will a smart thermometer set you back—and can FSA or HSA dollars help?
- What’s the simplest daily workflow to boost your conception odds?
- Is your fertility data safe, and will these apps play nicely with your doctor’s software?
- How can overlooked audiences benefit from smart thermometers?
- Your top questions, answered
- How can the right smart thermometer turn data into faster pregnancies?
- References
Why does basal body temperature matter when you’re trying to get pregnant?
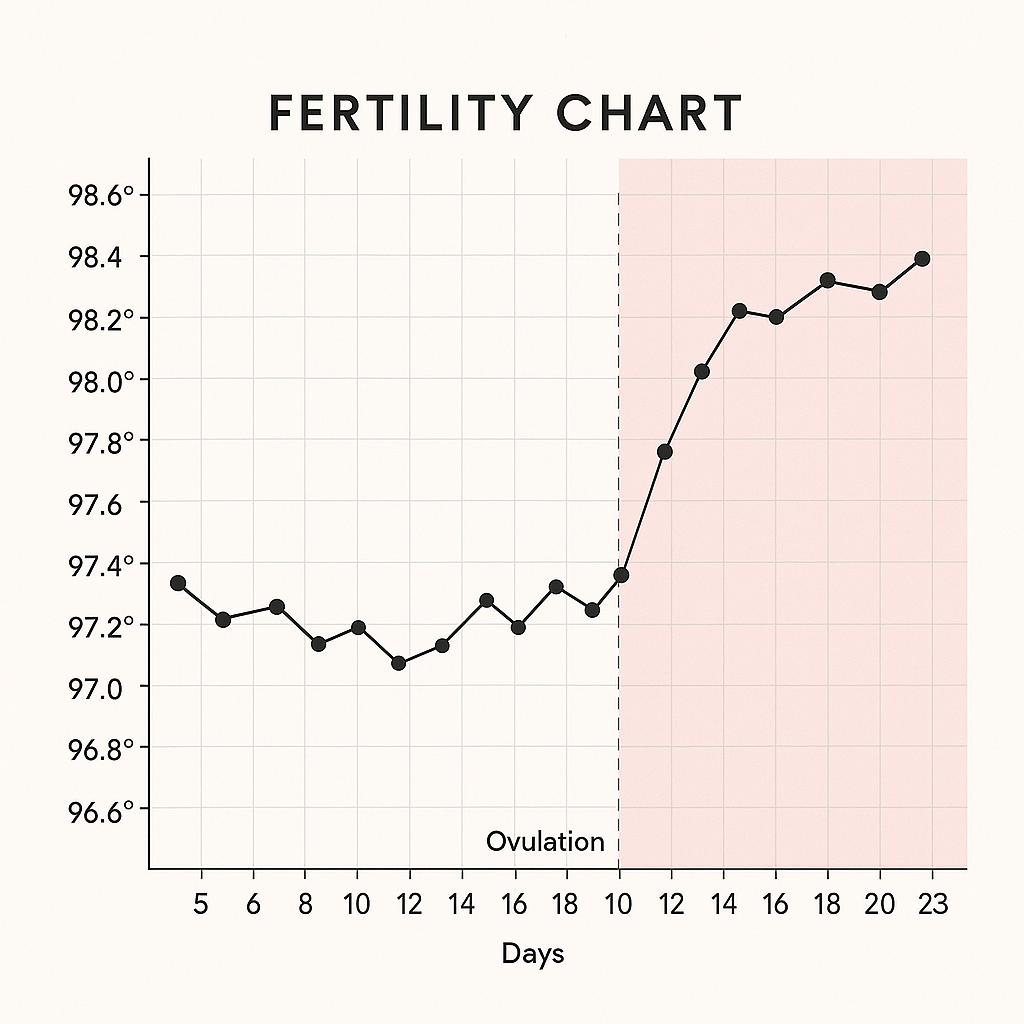
Basal body temperature (BBT) matters when you’re trying to get pregnant because it helps you identify when ovulation occurs. After ovulation, your body releases progesterone, which causes a small but measurable rise in your resting temperature. By tracking your BBT daily, you can spot this temperature shift and pinpoint your fertile window, the days when you’re most likely to conceive. Research shows that conception usually happens within a few days before or just after this temperature rise, making BBT a practical guide for timing intercourse.
That sustained rise, often called the luteal “high,” helps you:
- Verify that ovulation actually happened in a given cycle.
- Time intercourse during the five most fertile days leading up to ovulation.
- Spot early pregnancy when temperatures stay high for 15 + days.
- Flag possible luteal-phase defects if temps drop too soon.
- Build a data set your OB/GYN can review for patterns.
BBT tracking is a long-standing, non-invasive method for understanding your menstrual cycle and confirming that ovulation is happening. While it’s not perfect; about 20% of ovulatory cycles may not show a clear temperature shift, it remains a valuable tool, especially when combined with other fertility signs like cervical mucus. For many, BBT charting offers insight into cycle patterns, helps detect irregularities, and empowers you to make informed decisions on your fertility journey.
Pairing BBT with LH strips or cervical-mucus checks raises cycle-prediction accuracy to roughly 95 %, turning raw numbers into a full fertility map. For more sensor options, explore our deep dive on Fertility Wearables.
How are smart thermometers different from regular digital or classic basal models?
Smart thermometers are a significant upgrade from regular digital or classic basal thermometers, especially for fertility tracking. With classic basal thermometers, you must take your temperature manually every morning before getting out of bed and record the result yourself. This process can be tedious and is often affected by missed readings, user error, or inconsistent routines, making it harder to reliably detect the subtle temperature changes that signal ovulation.
Smart thermometers and wearable devices, on the other hand, automatically measure and record your temperature, often continuously, while you sleep. They sync this data to your smartphone, providing easy-to-read charts and ovulation predictions without manual tracking. Advanced sensors in smart thermometers can capture the biphasic temperature pattern of your cycle more accurately, even if your sleep schedule varies or you forget a reading. This automation reduces stress, increases accuracy, and makes fertility tracking more convenient and accessible for busy lifestyles. As technology advances, smart thermometers are becoming the preferred choice for many seeking reliable, user-friendly fertility monitoring.
Need an app primer? Check the comparison in Top Fertility Apps 2025.
Which smart thermometers rank highest for easy, accurate cycle tracking in 2025?
For easy and accurate cycle tracking in 2025, smart thermometers with Bluetooth connectivity and advanced sensor technology are leading the way. Recent developments highlight Bluetooth-enabled thermometers that use improved low-power resistive transducer circuits, achieving temperature measurement errors of less than 0.1 °C—well within clinical standards and ideal for fertility tracking. These devices automatically sync data to your smartphone, reducing manual errors and making daily tracking effortless.
Smart thermometers designed with enhanced calibration and nonlinear curvature correction further improve accuracy, with some models reaching ±0.15 °C across a wide temperature range. This level of precision is crucial for detecting the subtle temperature shifts that signal ovulation. Additionally, new digital thermometers based on microcontroller technology offer real-time, automatic readings with similar high accuracy and user-friendly displays. When choosing a smart thermometer, look for models that emphasize low error rates, seamless app integration, and reliable data storage—features now standard in the best devices for cycle tracking.
Below is a snapshot of devices tested by parents, clinicians, and peer-review sites.
| Device | Best For | Accuracy | Key Perks | Price |
|---|---|---|---|---|
| Easy@Home Smart Basal | All-around starter | ±0.09°F | 60-reading memory, Premom app, FSA-eligible | $39 |
| Tempdrop 2.0 (wearable) | Irregular sleep/shift work | Algorithm-smoothed | Overnight armband, FDA-cleared, 6-month battery | $149–$215 |
| Mira Starter Kit | PCOS & long cycles | 99 % lab-grade (LH, E3G, PdG) | Combines hormones + BBT, real-time fertile score | $249 + strips |
| Femometer Vinca 2.0 | Tight budgets | ±0.09°F | Backlit, app reminders, fast < 30 s read | $25 |
| Oura Ring Gen 3 | Data enthusiasts | 83 % ovulation detection | Sleep, HRV, skin temp sync to Natural Cycles | $299 |
Which features should top your checklist before you buy?
When choosing a smart thermometer for cycle tracking, prioritize features that ensure both accuracy and ease of use. Look for clinical-grade accuracy, ideally with a measurement error of less than ±0.1 °C, as this level of precision is crucial for detecting the subtle temperature shifts associated with ovulation. Fast response times and high resolution (such as 0.01 °C) are also important for reliable daily readings. Bluetooth connectivity or app integration allows for automatic data syncing, reducing manual errors and making it easier to visualize trends over time.
Low power consumption and long battery life are practical for daily use, while features like single-point calibration and advanced error correction (such as neural network calibration) further enhance measurement reliability. A clear, user-friendly display and simple operation add to convenience, and robust data privacy protections are essential when syncing personal health data to apps. Finally, consider devices that are comfortable to use and fit seamlessly into your morning routine, as consistency is key for effective cycle tracking.
Do wearables outshine stick thermometers for irregular cycles, shift work, or PCOS?
Irregular Cycles: Wearable thermometers generally outperform stick thermometers for tracking ovulation in people with irregular cycles. Wearables continuously monitor skin or core temperature throughout the night, capturing subtle, real-time temperature fluctuations that may be missed by a single morning reading with a stick thermometer. This continuous data allows for more accurate modeling of menstrual rhythms, even when cycles are unpredictable, and can help identify ovulatory patterns that classic methods might overlook. Advanced algorithms in wearables can analyze these complex patterns, providing clearer insights for those whose cycles do not follow a regular schedule.
Shift Work: For shift workers, wearables offer a clear advantage because they automatically record temperature regardless of when you sleep or wake. Stick thermometers require a consistent wake-up time and immediate measurement, which is often impractical for people with variable schedules. Wearables remove this barrier by tracking temperature passively and syncing data to an app, making them much more reliable for those whose routines change frequently.
PCOS: In people with polycystic ovary syndrome (PCOS), cycles are often long, irregular, or anovulatory, making ovulation detection with stick thermometers challenging. Wearables, by collecting continuous temperature data and applying sophisticated analysis, can better detect subtle or atypical ovulatory signals that might be missed with single-point measurements. This makes wearables a promising tool for those with PCOS who want to monitor their cycles more accurately and non-invasively, although further research is needed to optimize these technologies specifically for PCOS populations.
For the machine-learning magic behind these algorithms, see our feature on AI in IVF.
Are these devices truly evidence-backed and FDA-cleared?
Some smart thermometers are indeed evidence-backed and have received FDA clearance, meaning they meet regulatory standards for safety and accuracy as medical devices. For example, Kinsa’s smart thermometers are FDA-cleared and have been shown in studies to provide temperature data that closely correlates with regional public health surveillance, supporting their reliability for health monitoring. However, not all devices marketed as “smart” or “AI-enabled” are necessarily FDA-cleared for their advanced features; some discrepancies exist between marketing claims and actual FDA approval, especially for devices with artificial intelligence or machine learning components.
While FDA clearance is a strong indicator of device quality, it is important to verify that a specific model’s features, especially those related to cycle tracking or health analytics, are included in its regulatory approval. Overall, while there is growing evidence supporting the clinical value of some smart thermometers, users should look for FDA clearance and published validation studies to ensure they are choosing a device that is both safe and effective.
How much will a smart thermometer set you back—and can FSA or HSA dollars help?
A smart thermometer typically costs between $20 and $100, depending on features like Bluetooth connectivity, app integration, and continuous monitoring capabilities. Basic models are on the lower end, while advanced wearables or those with fertility tracking algorithms are at the higher end of the range.
Many smart thermometers are eligible for purchase with Flexible Spending Account (FSA) or Health Savings Account (HSA) dollars, as they are considered medical devices when used for health monitoring or fertility tracking. However, eligibility can vary by brand and retailer, so it’s important to check that the specific model is FSA/HSA-approved before purchasing. Using FSA or HSA funds can make these devices more affordable by allowing you to use pre-tax dollars. For the most up-to-date information, consult your FSA/HSA provider or the retailer’s product listing to confirm eligibility. This approach helps ensure you get both the health benefits and the financial savings available for smart thermometer purchases.
What’s the simplest daily workflow to boost your conception odds?
The simplest daily workflow to boost your conception odds centers on accurately identifying your fertile window and timing intercourse accordingly. Start each morning by taking your basal body temperature (BBT) before getting out of bed, as this helps pinpoint ovulation when tracked over time. Combine BBT charting with monitoring cervical mucus changes, which become clearer and more slippery around ovulation, further refining your fertile days. For even greater accuracy, consider using home ovulation predictor kits or digital fertility monitors that detect urinary luteinizing hormone surges, providing instant feedback on your fertility status.
Aim to have intercourse during the 5–6 days leading up to and including ovulation, as this is when conception is most likely. Keep daily records of your temperature, cervical mucus, and test results in a dedicated app or chart to spot patterns and optimize timing. Maintain a healthy lifestyle; get enough sleep, manage stress, and avoid smoking or excessive alcohol, to support reproductive health. If you experience early pregnancy loss, know that your odds of conceiving in the next cycle may actually increase. This straightforward, evidence-based routine maximizes your chances of conception by aligning your efforts with your body’s natural fertility signals.
If pregnancy hasn’t happened after 6–12 well-tracked cycles, consider bringing your charts to a specialist and exploring Predictive Analytics for next-level guidance.
Is your fertility data safe, and will these apps play nicely with your doctor’s software?
Fertility apps collect highly sensitive personal data, including menstrual cycles, sexual activity, and health conditions, raising significant privacy concerns. Studies show that many popular fertility apps have unclear or misleading privacy policies, often sharing or selling user data to third parties for advertising or research without adequate user consent or proper de-identification.
Users frequently lack meaningful control over how their data is used, and data may be retained long after app use ends, increasing the risk of breaches. While regulations like the GDPR aim to protect such intimate data, enforcement and transparency remain inconsistent, and many apps do not fully comply with best privacy practices. Users consistently express a desire for greater transparency and control, such as clear data-sharing options and the ability to manage or delete their information.
Regarding compatibility with doctors’ software, most fertility apps are not directly integrated with electronic health record (EHR) systems, making seamless data sharing with healthcare providers challenging. Instead, users often have to manually export or share reports, which may not be in a format compatible with medical software. In summary, while fertility apps offer convenience, users should be cautious about data privacy and should not assume automatic compatibility with their doctor’s systems.
How can overlooked audiences benefit from smart thermometers?
Overlooked audiences, including children, older adults, people in multi-generational households, and those in community settings, can benefit significantly from smart thermometers.
For families, especially those with children, smart thermometers help track fevers and potential illness transmission within the household, providing early warnings and supporting timely care decisions. Older adults, who may be less likely to self-report symptoms, can benefit from passive, easy-to-use monitoring that reduces the burden of manual tracking and helps caregivers or family members stay informed.
In large communities or institutions, such as schools or campuses, smart thermometers enable non-contact, automated temperature checks, reducing the need for direct staff involvement and minimizing infection risk during outbreaks like COVID-19. These devices also support real-time, population-level disease surveillance, offering valuable insights for public health officials to identify and respond to outbreaks more quickly and efficiently.
Additionally, smart thermometers with companion apps can engage users in participatory health reporting, empowering individuals who might otherwise be excluded from traditional surveillance systems to contribute to and benefit from collective health data. Overall, smart thermometers offer tailored advantages for groups that may face barriers to regular health monitoring or timely healthcare access.
For an immersive anatomy refresher, explore our 3D Uterus Models experience.
Your top questions, answered
How long before I see reliable patterns?
Most people need to track at least one to three full menstrual cycles to see reliable basal body temperature (BBT) patterns and accurately identify ovulation, as the biphasic temperature shift becomes clearer with consistent data. Wearable devices that measure temperature during sleep can make this process easier and more consistent, often matching the accuracy of traditional BBT methods.
Do I still need LH sticks if I track BBT?
BBT tracking can confirm ovulation after it happens, but LH sticks (ovulation predictor kits) detect the hormonal surge that precedes ovulation, allowing you to time intercourse more precisely. Using both methods together provides the most accurate picture of your fertile window, as BBT alone may not predict ovulation in advance.
Can a fever ruin my chart?
Yes, a fever or illness can temporarily raise your body temperature and disrupt your BBT chart, making it harder to interpret ovulation patterns for that cycle. It’s best to note any illness or unusual events in your chart for accurate interpretation.
Which thermometer reads the fastest?
Non-contact infrared thermometers and temporal artery thermometers are among the fastest, often providing readings in just a few seconds, but their accuracy can vary by age group and fever threshold. For fertility tracking, however, a digital oral or wearable thermometer that records temperature over several minutes or during sleep is recommended for accuracy.
Is Natural Cycles accurate when paired with Oura Ring?
Pairing Natural Cycles with the Oura Ring can provide accurate tracking of temperature changes across the menstrual cycle, as the Oura Ring reliably detects the biphasic temperature pattern associated with ovulation. This combination offers a convenient and evidence-backed way to monitor fertility, though individual results may vary and consistent use is key.
How can the right smart thermometer turn data into faster pregnancies?
The right smart thermometer, especially when integrated into wearable devices or smart health systems, can transform temperature data into actionable insights that may help couples achieve pregnancy faster. Continuous temperature monitoring allows for precise detection of ovulation and fertile windows, enabling better timing of conception efforts.
Advanced smart thermometers and wearables use artificial intelligence and data analytics to identify subtle physiological changes, such as shifts in skin temperature, that signal hormonal changes and impending ovulation or labor. These systems can provide daily predictions and personalized recommendations, reducing guesswork and increasing the likelihood of conception by ensuring intercourse is timed optimally. In addition, smart thermometers can alert users and healthcare providers to potential health issues, supporting early intervention and safer pregnancies.
The convenience of at-home, non-invasive monitoring also reduces the burden of frequent clinic visits, making fertility tracking more accessible and less stressful. Overall, by turning continuous temperature data into clear, timely guidance, smart thermometers can help streamline the path to pregnancy for many users.
References
-
Tracking of menstrual cycles and prediction of the fertile window via measurements of basal body temperature and heart rate as well as machine-learning algorithms. Reproductive Biology and Endocrinology : RB&E, 20. https://doi.org/10.1186/s12958-022-00993-4
-
Digital contraceptives based on basal body temperature measurements. Biomed. Signal Process. Control., 52, 141-151. https://doi.org/10.1016/J.BSPC.2019.04.019
-
The use of wearable devices for predicting biphasic basal body temperature to estimate the date of ovulation in women… Journal of thermal biology, 108, 103290. https://doi.org/10.1016/j.jtherbio.2022.103290
-
Assessing the utility of a smart thermometer and mobile application as a surveillance tool for influenza and influenza-like illness. Health Informatics Journal, 26, 2148 - 2158. https://doi.org/10.1177/1460458219897152
-
Marketing and US Food and Drug Administration Clearance of Artificial Intelligence and Machine Learning Enabled Software in and as Medical Devices. JAMA Network Open, 6. https://doi.org/10.1001/jamanetworkopen.2023.21792
-
The state of artificial intelligence-based FDA-approved medical devices and algorithms: an online database. NPJ Digital Medicine, 3. https://doi.org/10.1038/s41746-020-00324-0
-
Your Body, Our Data: Unfair and Unsafe Privacy Practices of Popular Fertility Apps. SSRN Electronic Journal. https://doi.org/10.2139/ssrn.4396029
-
Intimate Data Sharing: Enhancing Transparency and Control in Fertility Tracking. Proceedings of the 2025 CHI Conference on Human Factors in Computing Systems. https://doi.org/10.1145/3706598.3714089
-
Enhanced Accuracy of CMOS Smart Temperature Sensors by Nonlinear Curvature Correction. Sensors (Basel, Switzerland), 18. https://doi.org/10.3390/s18124087
-
Development of a Smart Clinical Bluetooth Thermometer Based on an Improved Low-Power Resistive Transducer Circuit. Sensors (Basel, Switzerland), 22. https://doi.org/10.3390/s22030874
-
A CMOS Temperature Sensor with a Smart Calibrated Inaccuracy of ±0.11 (3σ). Sensors (Basel, Switzerland), 23. https://doi.org/10.3390/s23115132
-
Using Wearable Skin Temperature Data to Advance Tracking and Characterization of the Menstrual Cycle in a Real-World Setting. Journal of Biological Rhythms, 39, 331 - 350. https://doi.org/10.1177/07487304241247893
-
Wearable Sensors Reveal Menses-Driven Changes in Physiology and Enable Prediction of the Fertile Window: Observational Study. Journal of Medical Internet Research, 21. https://doi.org/10.2196/13404