If you’re looking at an AMH levels chart and feeling anxious or uncertain about what it means for your fertility, you’re not alone. Only 14 % of women under 35 have “low” AMH—are you in the other 86 %? Many people worry that a single number might define their chances of having a child, or feel overwhelmed by the idea that their “ovarian reserve” is being measured and compared. It’s completely valid to have questions or even fears about what your AMH level says about your body and your future. The truth is, AMH is a helpful tool for understanding the number of eggs you might have, but it doesn’t tell the whole story about your fertility, your health, or your worth as a parent.
It’s also important to know that AMH levels can fluctuate for reasons that have nothing to do with your actual fertility. Things like hormonal birth control, body size, or even the specific test used can all affect your results. Seeing a “low” or “high” number on a chart can feel discouraging or confusing, but your AMH level is just one piece of a much bigger picture. Your age, overall health, and personal goals matter just as much, if not more. If you’re feeling lost or worried, it’s okay to ask questions and seek support. You deserve clear, compassionate answers and care that respects your unique journey.
- What exactly is AMH, and why does it reveal your egg count?
- How do I read the AMH levels chart for my age?
- What do low, normal, and high AMH levels mean for fertility planning?
- How should your AMH guide next steps like natural conception, egg freezing, or IVF?
- Which factors can skew an AMH test—and when should you retest?
- Your top AMH questions, answered
- Final thoughts: turn your AMH number into confident action
- References
What exactly is AMH, and why does it reveal your egg count?
Anti-Müllerian hormone (AMH) is a protein your ovaries make, mostly from the small follicles that hold immature eggs. When you check your AMH level, you’re getting a snapshot of your “ovarian reserve” , the number of eggs you have left. Higher AMH usually means you have more of these small follicles, while lower AMH suggests your egg supply is naturally declining, which happens as you get older. AMH doesn’t measure the quality of your eggs, but it does help your healthcare provider understand your current egg quantity and how your ovaries might respond to fertility treatments like in vitro fertilization (IVF).
Here’s why AMH reveal your egg count:
- Unlike other hormones, AMH stays fairly stable throughout your menstrual cycle, so you can test it any time.
- It’s a better predictor of how many eggs you might produce during fertility treatments than other hormones or tests.
- It can help guide decisions about fertility preservation, especially if you’re considering egg freezing or have a medical condition that could affect your ovaries.
- AMH is made by the same follicles that contain your eggs, so the more follicles you have, the higher your AMH.
- AMH levels naturally drop as you age, reflecting the gradual loss of eggs over time.
Dr. Richard J. Paulson, MD, past president of the American Society for Reproductive Medicine, explains: “AMH is the best available marker for ovarian reserve, but it’s important to remember that it’s just one piece of the puzzle. Your age and overall health matter, too.” (ACOG, 2023)
Fertility Blood Tests: What Each Number Means gives you more insights.
Fun fact: AMH peaks around age 25 after puberty when the follicles ready to grow is at its lifetime high.
How do I read the AMH levels chart for my age?
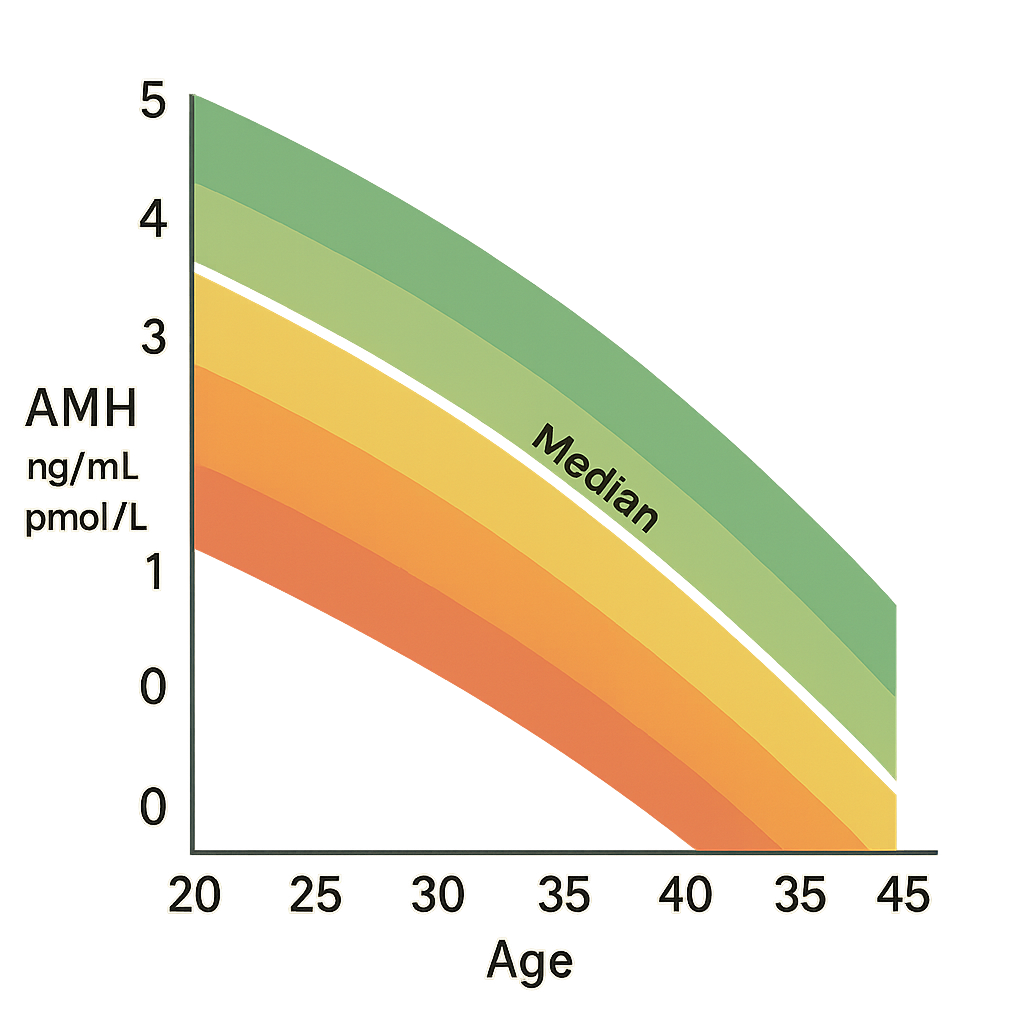
Reading an Anti-Müllerian hormone (AMH) levels chart by age can feel overwhelming, but it’s really about understanding how your ovarian reserve changes over time. AMH naturally declines as you get older, and what’s “normal” depends on your age group.
Here’s a simple table to help you visualize typical Anti-Müllerian hormone (AMH) levels by age group. These numbers are based on large studies of non-infertile women in the USA and can help you see how AMH usually changes as you get older. Remember, “median” means the middle value, and the “IQR” (interquartile range) shows the typical spread for most people in that group1.
| Age(years) | Median AMH (ng/mL) | Typical Range (IQR, ng/mL) | Zone Color | What It Means |
|---|---|---|---|---|
| <30 | 2.91 | 1.79 – 4.82 | 🟩 Green | Above average/average reserve for age |
| 30–34 | 2.42 | 1.38 – 4.22 | 🟩 Green | Above average/average reserve for age |
| 35–37 | 2.03 | 1.14 – 3.54 | 🟨 Yellow | Normal, but reserve is starting to decline |
| 38–40 | 1.50 | 0.77 – 2.69 | 🟨 Yellow | Lower reserve, expected for this age |
| 41–42 | 0.92 | 0.32 – 2.19 | 🟧 Orange | Low reserve, common as menopause approaches |
| >42 | 0.59 | 0.25 – 1.20 | 🟥 Red | Significantly reduced reserve, typical >42 |
How to use this table:
Find your age group.
Compare your AMH to the median and range.
Green: Ovarian reserve is above average or average for your age.
Yellow: Reserve is declining, but still within expected range.
Orange: Reserve is low for age, but not unusual as you approach menopause.
Red: Reserve is very low, which is typical after age 42.
Dr. B. Maslow, MD, says, “Accurate representation of physiologic AMH ranges in non-infertile women is a critical element of counseling women regarding their reproductive goals”.
What do low, normal, and high AMH levels mean for fertility planning?
Low, normal, and high Anti-Müllerian hormone (AMH) levels each play a different role in fertility planning, but it’s important to know that AMH is just one piece of your overall fertility picture. Here’s what your AMH level can mean for your fertility planning:
Low AMH: This usually means your ovarian reserve (egg supply) is lower than average for your age. It can suggest a shorter window for getting pregnant, but it does not mean pregnancy is impossible. Many people with low AMH still conceive naturally or with help. For fertility treatments like in vitro fertilization (IVF), low AMH may mean fewer eggs retrieved, but it doesn’t always predict pregnancy success.
Normal AMH: This suggests your ovarian reserve is typical for your age. It can help your provider estimate how you might respond to fertility treatments and guide decisions about medication dosing. However, AMH does not measure egg quality or guarantee pregnancy.
High AMH: Higher levels can mean a larger egg supply. If your AMH is very high and you have irregular periods, it could be a sign of polycystic ovary syndrome (PCOS). People with PCOS may have more eggs retrieved during IVF, but sometimes face lower fertilization or pregnancy rates and a higher risk of ovarian hyperstimulation.
Recent research shows that while AMH is a reliable marker for ovarian reserve, it should not be used alone to predict your chances of pregnancy. For example, one study found that even women with low AMH can have good outcomes with fertility treatments, highlighting the need for a personalized approach that considers other factors like age and overall health.
How should your AMH guide next steps like natural conception, egg freezing, or IVF?
Your Anti-Müllerian hormone (AMH) level can help guide your fertility decisions, but it’s not the only factor to consider. A large prospective study of nearly 900 women found that higher AMH levels were strongly linked to better outcomes with in vitro fertilization (IVF): live birth rates increased from about 11% for those with low AMH to over 30% for those with higher AMH, even after accounting for age and number of eggs retrieved. This means that if your AMH is higher, you may have a better chance of success with IVF, and your provider can use this information to tailor your treatment plan. However, even with low AMH, pregnancy is still possible, and AMH does not guarantee or rule out success.
Here’s how AMH might guide your options:
- Natural conception: AMH does not predict your ability to get pregnant naturally. Even with low AMH, many people conceive without treatment. Age and overall health are more important for natural fertility, so don’t let a low AMH level discourage you .
- Egg freezing: If you’re thinking about freezing your eggs, AMH can help estimate how many eggs you might retrieve in one cycle. Lower AMH may mean fewer eggs per cycle, so you might need to start sooner or plan for more than one cycle. Higher AMH usually means more eggs can be retrieved, making the process more efficient.
- In vitro fertilization (IVF): AMH is useful for planning IVF. Higher AMH often means a better response to stimulation and more eggs retrieved, but it doesn’t guarantee pregnancy. If you have polycystic ovary syndrome (PCOS) and very high AMH, you may have more eggs but sometimes lower pregnancy rates and a higher risk of ovarian hyperstimulation. If your AMH is low, you may still have a chance at pregnancy with IVF, but you might need higher medication doses or more cycles.
Dr. Marcelle Cedars, MD, reproductive endocrinologist and past president of the American Society for Reproductive Medicine, says, “AMH is a good marker of how your ovaries might respond to treatment, but it doesn’t tell us about egg quality or your actual chances of getting pregnant”.
Your provider can help you interpret your AMH in context and create a plan that fits your needs like Egg Freezing 101: Preserve Fertility for Later and Follicle Scans 101: How Doctors Track Egg Growth.
Which factors can skew an AMH test—and when should you retest?
Several factors can skew your Anti-Müllerian hormone (AMH) test results, so it’s important to know what might affect your numbers.
Here are the main factors:
- Age: AMH naturally declines as you get older, especially after age 3.
- Body mass index (BMI): Higher BMI is linked to lower AMH, even if your ovarian reserve is normal.
- Smoking: Current smokers can have AMH levels up to 44% lower than non-smokers.
- Hormonal birth control: Using oral contraceptives can lower AMH by 17–31%, so wait at least 2–3 months after stopping before testing.
- Physical activity: Intense exercise may reduce AMH, especially in people with polycystic ovary syndrome (PCOS).
- Stress and nutrition: High stress and poor nutrition can also impact AMH levels.
- Medical treatments: Chemotherapy, certain surgeries, and some medications can lower AMH.
- Technical/lab factors: How your blood sample is stored and processed, or which lab runs the test, can affect results. For example, improper storage or hemolysis (breakdown of red blood cells) can skew numbers.
When should you retest?
- If you were on hormonal birth control or recently stopped, wait 2–3 months before retesting.
- If you’ve made big lifestyle changes (like quitting smoking or major weight loss).
- If your result doesn’t match your overall fertility picture or other test results.
Dr. Lotte Werner, MD, lead author of a 2024 review, says: “Lifestyle factors are associated with differences in AMH levels and thus should be taken into account when interpreting individual AMH measurements.”
Your top AMH questions, answered
What is a “good” AMH at 35?
At age 35, an AMH level between about 1.0 and 3.0 ng/mL is generally considered within the normal range for ovarian reserve, but there is no strict cutoff. AMH reflects egg quantity, not quality, and levels naturally decline with age. Importantly, even women with lower AMH can sometimes respond well to fertility treatment.
Can I boost my AMH naturally?
There is no proven way to significantly increase AMH levels through lifestyle or supplements. While maintaining a healthy weight and avoiding smoking may help preserve ovarian reserve, these changes do not meaningfully raise AMH once it has declined.
Does AMH predict menopause?
AMH declines years before menopause and can help estimate the timing, but individual predictions are imprecise. AMH is best used as a general indicator of reproductive aging rather than a precise menopause predictor.
How low is too low for IVF?
An AMH below 1.0 ng/mL is often considered “low” and may indicate a reduced response to ovarian stimulation, but it does not mean IVF is impossible or should be withheld. Many women with low AMH still achieve pregnancy with IVF, so AMH should guide expectations, not exclude treatment.
Can AMH predict natural fertility?
While AMH is a good indicator of ovarian reserve, it is less reliable for predicting natural conception or ongoing pregnancy, as many other factors are involved in fertility.
Final thoughts: turn your AMH number into confident action
Turning your AMH number into confident action starts with understanding what it truly means: AMH is a reliable marker of ovarian reserve, helping estimate how many eggs you have, but it does not predict your egg quality or guarantee your chances of pregnancy. Use your AMH result as a tool to guide conversations with your healthcare provider about your reproductive timeline, fertility preservation options, or the best approach to fertility treatments like IVF.
Remember, age remains the strongest factor in fertility outcomes, so your AMH should be interpreted alongside your age and overall health. If your AMH is lower than expected, don’t panic; many women with low AMH still conceive, especially with individualized treatment plans. Avoid making major decisions based on AMH alone; instead, consider a comprehensive fertility assessment that includes other hormones and ultrasound findings. If you’re not ready for pregnancy now, your AMH can help you plan ahead, but it shouldn’t be the sole reason to rush or delay your choices. Finally, discuss any concerns or questions with a fertility specialist, who can help you turn your AMH result into a clear, personalized action plan for your goals.
More from thebabyprotocol: Clomid vs. Letrozole: How They Trigger Ovulation.
References
-
A systematic review of the association between modifiable lifestyle factors and circulating anti-Müllerian hormone… Human reproduction update. 2024 https://doi.org/10.1093/humupd/dmae004
-
Antimüllerian hormone levels are strongly associated with live-birth rates after assisted reproduction… The Journal of clinical endocrinology and metabolism. 2013; 98 3. https://doi.org/10.1210/jc.2012-3676.
-
AMH and Ovarian Reserve Testing… The Journal of clinical endocrinology and metabolism. 2022 https://doi.org/10.1210/clinem/dgac039.
-
Anti-Müllerian Hormone Concentrations in Women of Different Reproductive Age and the Chances of IVF Outcome: A Paradigm Shift is needed… Aging and disease. 2025 https://doi.org/10.14336/AD.2024.1615
-
Age-Based Interpretation of Anti-Mullerian Hormone (AMH) Levels in Non-infertile Women [37J]. Obstetrics & Gynecology. 2019 https://doi.org/10.1097/01.AOG.0000558853.91697.B0
-
Distribution and Related Influencing Factors of AMH Level in Family-Planning Women of Childbearing Age: A Cross-Sectional Study from Beijing, China. International Journal of Women’s Health. 2025; 17. https://doi.org/10.2147/IJWH.S499220