Facing fertility challenges can feel overwhelming and isolating. You may wonder if your body is working against you, or worry about the uncertainty of each new treatment. These concerns are valid—infertility is a deeply personal journey, and the choices you make matter.
When it comes to ovulation induction, Clomid (clomiphene citrate) and letrozole are two of the most commonly prescribed medications. Deciding between them can be confusing, especially when you want the best chance of success with the fewest side effects. You deserve clear, compassionate information to help guide your next steps.
This article will explain how Clomid and letrozole work to trigger ovulation, compare their effectiveness, and discuss what the latest research means for your fertility journey. You’ll learn what to expect from each option, so you can make informed decisions with your healthcare team.
- How do Clomid and Letrozole trigger ovulation differently?
- Which medication leads to higher pregnancy and live-birth rates?
- What hidden trade-offs should you consider before picking a pill?
- How are Clomid or Letrozole cycles monitored for success?
- When is it smart to switch, stack, or stop treatment?
- What do cost, insurance, and FDA status mean for you?
- Your top questions, answered
- What’s the bottom line for choosing your ovulation pill?
- References
How do Clomid and Letrozole trigger ovulation differently?
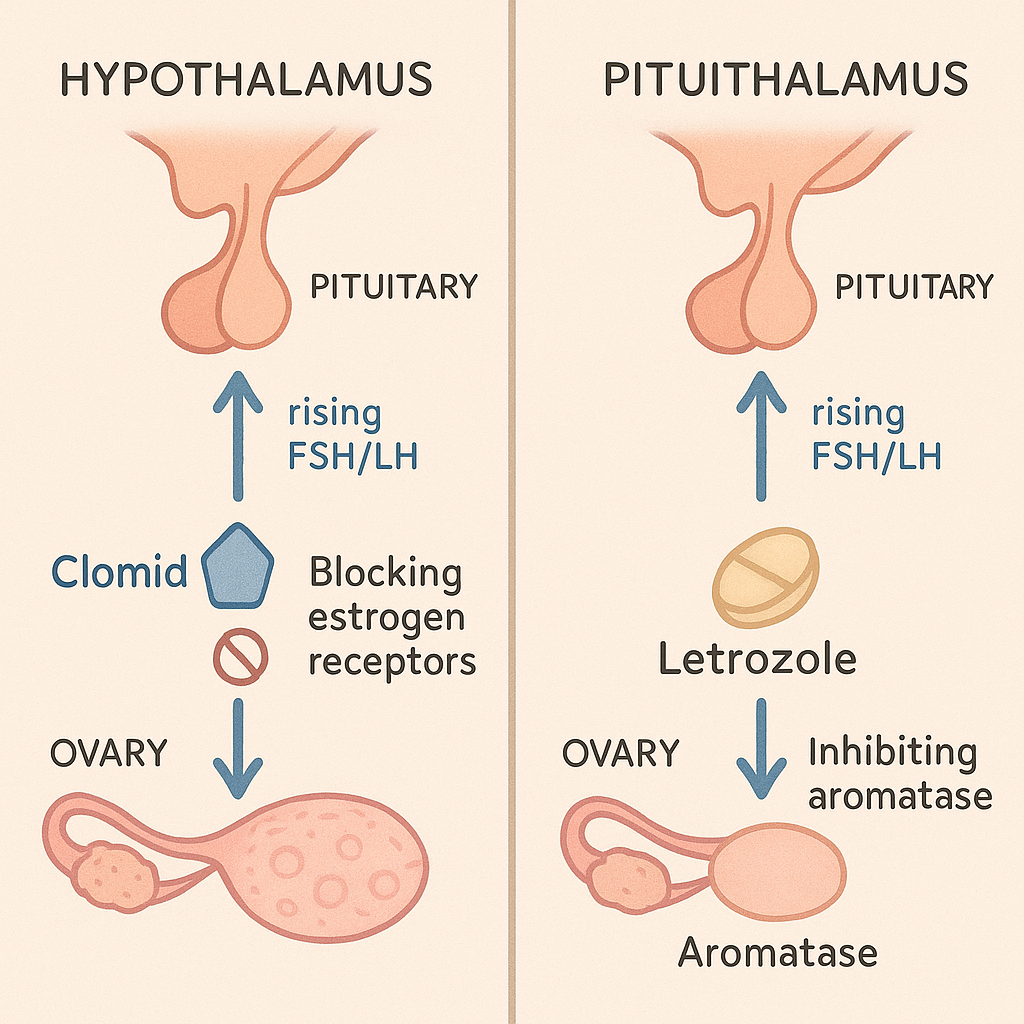
Clomiphene citrate (Clomid) and letrozole both help trigger ovulation, but they work in different ways. Clomiphene citrate is a selective estrogen receptor modulator. It blocks estrogen receptors in your brain, making your body think estrogen levels are low. This prompts your pituitary gland to release more follicle-stimulating hormone (FSH) and luteinizing hormone (LH), which stimulate your ovaries to mature and release eggs. Letrozole, on the other hand, is an aromatase inhibitor. It lowers estrogen production by blocking the enzyme that converts androgens to estrogen. This drop in estrogen also signals your brain to increase FSH and LH, leading to ovulation, but without blocking estrogen’s action in other tissues.
Key differences in how these medications work:
- Clomiphene blocks estrogen receptors in the brain, which can thin the uterine lining and affect cervical mucus.
- Letrozole reduces estrogen production, but allows normal estrogen feedback in the body, often resulting in a thicker uterine lining and better cervical mucus.
According to a 2023 systematic review in Reproductive Sciences, letrozole leads to higher ovulation and pregnancy rates than clomiphene, and is associated with a thicker endometrial lining, which may improve implantation and pregnancy outcomes. Dr. Richard S. Legro, MD, Professor of Obstetrics and Gynecology at Penn State College of Medicine, notes, “Letrozole is now considered a first-line treatment for ovulation induction in women with polycystic ovary syndrome due to its higher live birth rates and favorable side effect profile’’ 1. In summary, while both medications aim to help you ovulate, letrozole’s mechanism may offer advantages in endometrial health and pregnancy success.
Which medication leads to higher pregnancy and live-birth rates?
Letrozole generally leads to higher pregnancy and live-birth rates than clomiphene citrate (Clomid), especially for individuals with polycystic ovary syndrome (PCOS). A 2023 meta-analysis of 29 randomized controlled trials found that letrozole increased the chance of live birth by nearly 50% compared to clomiphene (risk ratio 1.49, 95% CI 1.27–1.74), and also improved ovulation and clinical pregnancy rates. Another large, well-designed trial showed live-birth rates of 27.5% with letrozole versus 19.1% with clomiphene in women with PCOS, with no significant difference in major birth defects. For women with unexplained infertility, both medications result in similar pregnancy and live-birth rates.
In summary:
- For PCOS: Letrozole offers higher pregnancy and live-birth rates than clomiphene.
- For unexplained infertility: Both medications are similarly effective.
- Letrozole may also result in a thicker uterine lining and fewer side effects.
Letrozole is now considered a first-line treatment for ovulation induction in women with polycystic ovary syndrome due to its higher live birth rates and favorable side effect profile. Always discuss your options with your healthcare provider to find the best fit for your needs.
If you’re tracking success, mid-luteal progesterone of ≥10 ng/mL confirms ovulation; Day-21 Progesterone will guide you on how to interpret.
What hidden trade-offs should you consider before picking a pill?
Before choosing between clomiphene citrate (Clomid) and letrozole, you should consider several hidden trade-offs beyond just pregnancy rates. For individuals with polycystic ovary syndrome (PCOS), letrozole offers a higher chance of pregnancy and live birth. Both medications stimulate ovulation, but their effects on your body and potential risks differ.:
- Pregnancy and live birth: Letrozole leads to higher pregnancy and live-birth rates than clomiphene, especially for people with polycystic ovary syndrome (PCOS). In a large U.S. study, the probability of pregnancy was 43% with letrozole versus 37% with clomiphene, and live birth was 32% versus 29%
- Multiple gestation (twins or more): Letrozole increases the risk of twins or more (19% with letrozole vs. 9% with clomiphene in PCOS).
- Preterm birth and NICU admission: Letrozole is linked to higher rates of preterm birth (20% vs. 15%) and neonatal intensive care unit (NICU) admission (22% vs. 16%) compared to clomiphene in PCOS.
- Congenital malformations: The risk of major congenital malformations is higher with letrozole (8%) than with clomiphene (2%) among those who have a live birth, though overall rates remain low.
- Endometrial effects: Letrozole often results in a thicker uterine lining, which may help with implantation, while clomiphene can thin the lining and affect cervical mucus, possibly making conception harder for some.
- Side effects: Clomiphene is more likely to cause hot flashes, while letrozole may cause fatigue and dizziness.
For those with unexplained infertility, both medications have similar pregnancy and neonatal outcomes, so these risks are less of a concern. Letrozole often results in a thicker endometrial lining, which may help with implantation, while clomiphene can thin the uterine lining and affect cervical mucus, possibly making conception harder for some. Side effects also differ: clomiphene is more likely to cause hot flashes, while letrozole may cause fatigue and dizziness.
If implantation timing is a concern, learn how specialists fine-tune it with the Endometrial Receptivity Test.
How are Clomid or Letrozole cycles monitored for success?
Your healthcare team will closely monitor your cycles when you use clomiphene citrate (Clomid) or letrozole to ensure the medication is working and to maximize your chances of pregnancy. Monitoring helps track your body’s response and reduces risks like multiple pregnancies.
Key steps in monitoring include:
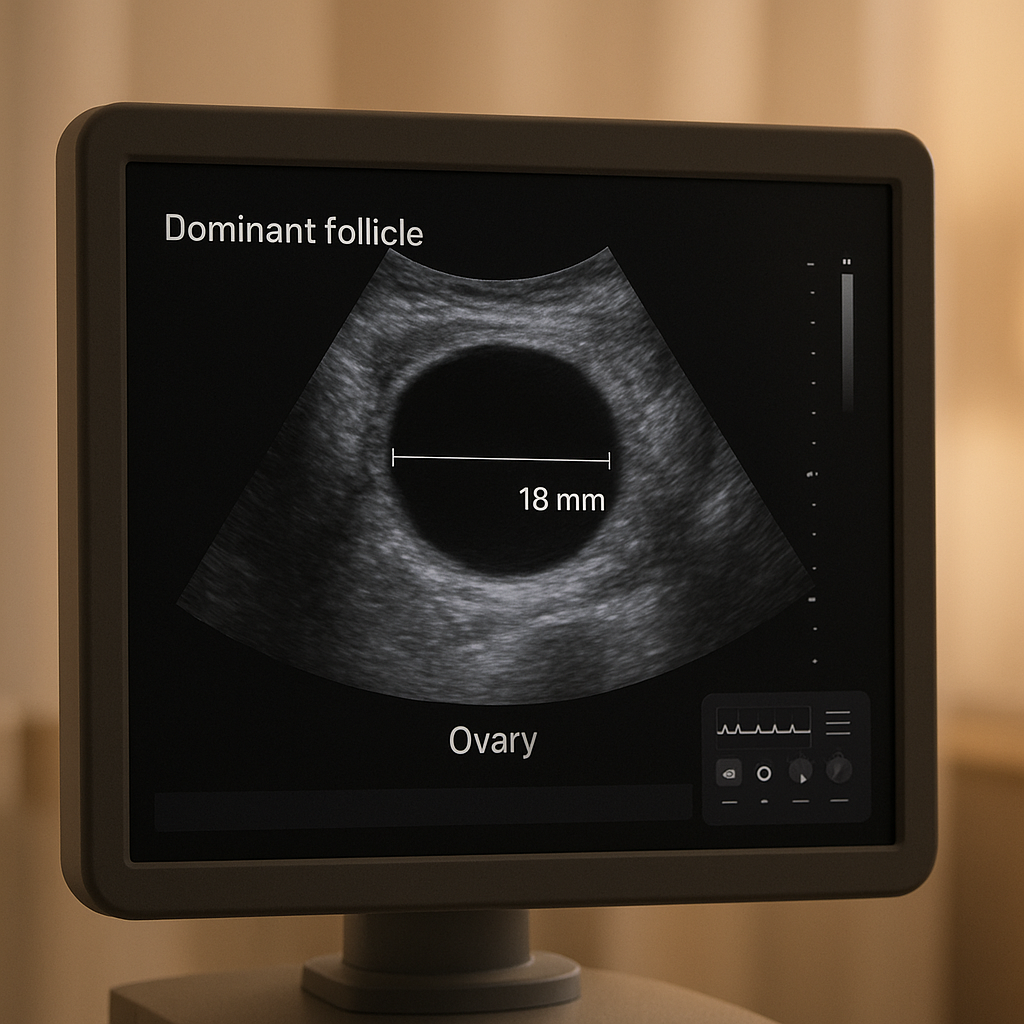
- Ultrasound scans: You will likely have transvaginal ultrasounds starting around day 10 of your cycle. These scans measure the growth of ovarian follicles and check endometrial (uterine lining) thickness. Letrozole often results in a thicker lining than clomiphene, which may help with implantation.
- Blood tests: Your provider may check hormone levels, such as estradiol, luteinizing hormone (LH), and progesterone, to confirm ovulation and assess your response.
- Ovulation prediction: You may use at-home LH surge kits or your provider may give you a “trigger shot” of human chorionic gonadotropin (hCG) to time ovulation and intercourse or intrauterine insemination (IUI).
- Cycle tracking: Your provider will ask about your menstrual cycle, symptoms, and any side effects.
If you do not ovulate or respond to the initial dose, your provider may adjust your medication or try a different protocol. Dr. Saad Amer, MD, Professor of Reproductive Medicine, notes, “Ultrasound follicle tracking and mid-luteal serum progesterone measurement are standard for monitoring ovulation induction cycles and optimizing outcomes”. Careful monitoring helps you and your provider make informed decisions and increases your chances of a healthy pregnancy.
Fertility Blood Tests and Follicle Scans 101 will help you understand more.
When is it smart to switch, stack, or stop treatment?
When using clomiphene citrate (Clomid) or letrozole for ovulation induction, you may need to switch, stack, or stop treatment based on your response and goals. Here’s when each approach is smart:
Switch if:
- Switch to a different medication if you do not ovulate or conceive after 3–6 cycles, or if you experience significant side effects.
- Consider switching from clomiphene to letrozole if you have a thin uterine lining or poor cervical mucus, as letrozole often improves these issues and may increase pregnancy rates, especially in people with polycystic ovary syndrome (PCOS)12.
- For unexplained infertility, switching may not change outcomes, as both medications have similar success rates.
Stack when:
- Stack (combine) medications, such as adding metformin to clomiphene, if you have a partial response or specific metabolic concerns.
- Stacking can improve ovulation and pregnancy rates, particularly in people with PCOS. Research shows clomiphene plus metformin is more effective than clomiphene alone and nearly as effective as letrozole for pregnancy and ovulation.
- Consider stacking if you are not ready to move to more advanced treatments but need a stronger response.
Stop if:
- Stop oral ovulation induction if you have completed 6 cycles without success, develop serious side effects, or achieve pregnancy.
- At this point, your provider may recommend moving to advanced treatments like gonadotropins or in vitro fertilization (IVF).
Stopping is also appropriate if the risks or burdens of continued treatment outweigh the potential benefits. Dr. Richard Legro, MD, Professor of Obstetrics and Gynecology, advises, “If you do not conceive after several cycles, it is reasonable to switch agents or escalate therapy to maximize your chances of success”.
What do cost, insurance, and FDA status mean for you?
Understanding cost, insurance, and U.S. Food and Drug Administration (FDA) status helps you make informed choices about clomiphene citrate (Clomid) and letrozole for fertility treatment:
- Cost: Clomid is usually less expensive than letrozole. Generic clomiphene can cost $10–$50 per cycle, while letrozole may range from $20–$100 per cycle, depending on your pharmacy and location. Prices can vary widely.
- *Insurance: Many insurance plans cover some or all of the cost of these medications, especially if you have a diagnosis of infertility. However, coverage varies by state and plan. Some plans may require prior authorization or limit the number of covered cycles. Always check with your insurer before starting treatment.
- FDA Status: Clomid is FDA-approved for ovulation induction in people with infertility. Letrozole is FDA-approved for breast cancer, but not specifically for infertility. However, letrozole is widely used “off-label” for ovulation induction, and major medical organizations support its use for this purpose, especially in people with polycystic ovary syndrome (PCOS).
- What this means for you: Clomid may be easier to get insurance coverage for, but letrozole is often more effective for PCOS and is considered safe and standard by fertility experts. You may need your provider to submit extra paperwork for letrozole.
According to Dr. Zhuo Liu, MD, PhD, lead author of a 2023 meta-analysis, “Letrozole was associated with improved ovulation, pregnancy, and live-birth rates compared with clomiphene citrate. We recommend letrozole over clomiphene citrate as an ovulation induction drug in women with infertility and PCOS, although the quality of the evidence is mixed”.
Talk with your provider and insurance company to find the best, most affordable option for your needs.
Your top questions, answered
Does either drug increase birth-defect risk?
The overall risk of birth defects is low and similar to natural conception. Clomiphene may be linked to a slightly higher risk of neural tube defects and hypospadias, especially after many cycles, but the absolute risk increase is small (about 1–2%). Letrozole does not appear to increase the risk of birth defects and is considered non-teratogenic.
How many cycles are considered safe?
Most experts recommend up to 6 cycles of clomiphene or letrozole. Using more cycles may slightly increase the risk of certain birth defects with clomiphene, but overall risks remain low. If pregnancy has not occurred after 6 cycles, it is usually time to consider other treatments.
Can supplements like myo-inositol boost my response?
Myo-inositol is sometimes used, especially in people with polycystic ovary syndrome (PCOS), to improve ovulation and insulin sensitivity. Some studies suggest it may enhance the response to ovulation induction, but it is not a guaranteed booster and should be discussed with your provider.
Are these pills ever used for male infertility?
Yes, both clomiphene and letrozole are sometimes prescribed off-label for male infertility, particularly to improve sperm count and hormone balance in men with certain hormonal imbalances. However, evidence is mixed, and these uses are less common than in women.
What are my chances of twins?
Both drugs increase the chance of twins compared to natural conception, but the risk is moderate. With clomiphene, the twin rate is about 7–9%, and with letrozole, it is similar or slightly lower. Higher-order multiples (triplets or more) are rare with either drug, especially compared to injectable fertility medications.
What’s the bottom line for choosing your ovulation pill?
The bottom line for choosing between clomiphene citrate (Clomid) and letrozole depends on your diagnosis and treatment goals. For people with polycystic ovary syndrome (PCOS), letrozole consistently leads to higher ovulation, pregnancy, and live birth rates compared to clomiphene, and is now widely recommended as the first-line option. Letrozole also tends to have fewer side effects and a lower risk of multiple pregnancies, especially higher-order multiples, though the risk of twins is still present. For those with unexplained infertility, both drugs are similarly effective, so either may be a reasonable choice. Safety profiles are comparable, with no significant difference in birth defect risk between the two medications. Ultimately, letrozole is generally preferred for PCOS, while both options are valid for unexplained infertility; your doctor will help tailor the choice based on your specific needs, side effect tolerance, and insurance coverage.
References
-
Treatment strategies for women with WHO group II anovulation: systematic review and network meta-analysis. The BMJ. 2017; 356. https://doi.org/10.1136/bmj.j138.
-
Double-blind randomized controlled trial of letrozole versus clomiphene citrate in subfertile women with polycystic ovarian syndrome. Human Reproduction (Oxford, England). 2017; 32. https://doi.org/10.1093/humrep/dex227.
-
Emulating a target trial of the comparative effectiveness of clomiphene citrate and letrozole for ovulation induction… Human reproduction. 2022 https://doi.org/10.1093/humrep/deac005.
-
Letrozole Compared With Clomiphene Citrate for Polycystic Ovarian Syndrome. Obstetrics & Gynecology. 2023; 141. https://doi.org/10.1097/AOG.0000000000005070.
-
Comparison of Letrozole and Clomiphene Citrate in Pregnancy Outcomes in Patients with Polycystic Ovary Syndrome: A Systematic Review and Meta-analysis… Reproductive sciences. 2023 https://doi.org/10.1007/s43032-023-01404-8.
-
Letrozole versus clomiphene for infertility in the polycystic ovary syndrome… The New England journal of medicine. 2014; 371 2. https://doi.org/10.1056/NEJMoa1313517.