If you’re navigating fertility questions, you may have heard about the “Day-21 progesterone” test. Your concern is valid—this test is a key tool for understanding your reproductive health. Progesterone is a hormone your body produces after ovulation, and its level around day 21 of a typical menstrual cycle can reveal if you’ve ovulated and whether your body is supporting a potential pregnancy.
Knowing your progesterone level at this point helps your care team assess if your cycle is on track for conception. Low levels may signal problems with ovulation or the luteal phase, which can affect your chances of becoming pregnant. Testing on day 21 is especially important if you’re experiencing irregular cycles or have been trying to conceive without success, as it guides next steps and treatment options tailored to your needs. Understanding and addressing your progesterone levels empowers you to make informed decisions on your fertility journey.
- Why does progesterone spike after ovulation, and why do we measure it?
- Is “Day-21” always the right day to test progesterone?
- How do doctors interpret Day-21 progesterone numbers?
- What if your progesterone is low—mistiming or luteal phase defect?
- Which evidence-based strategies can raise mid-luteal progesterone?
- Could a high Day-21 progesterone signal pregnancy or twins?
- Your Top Questions, Answered
- Final Thoughts
- References
Why does progesterone spike after ovulation, and why do we measure it?
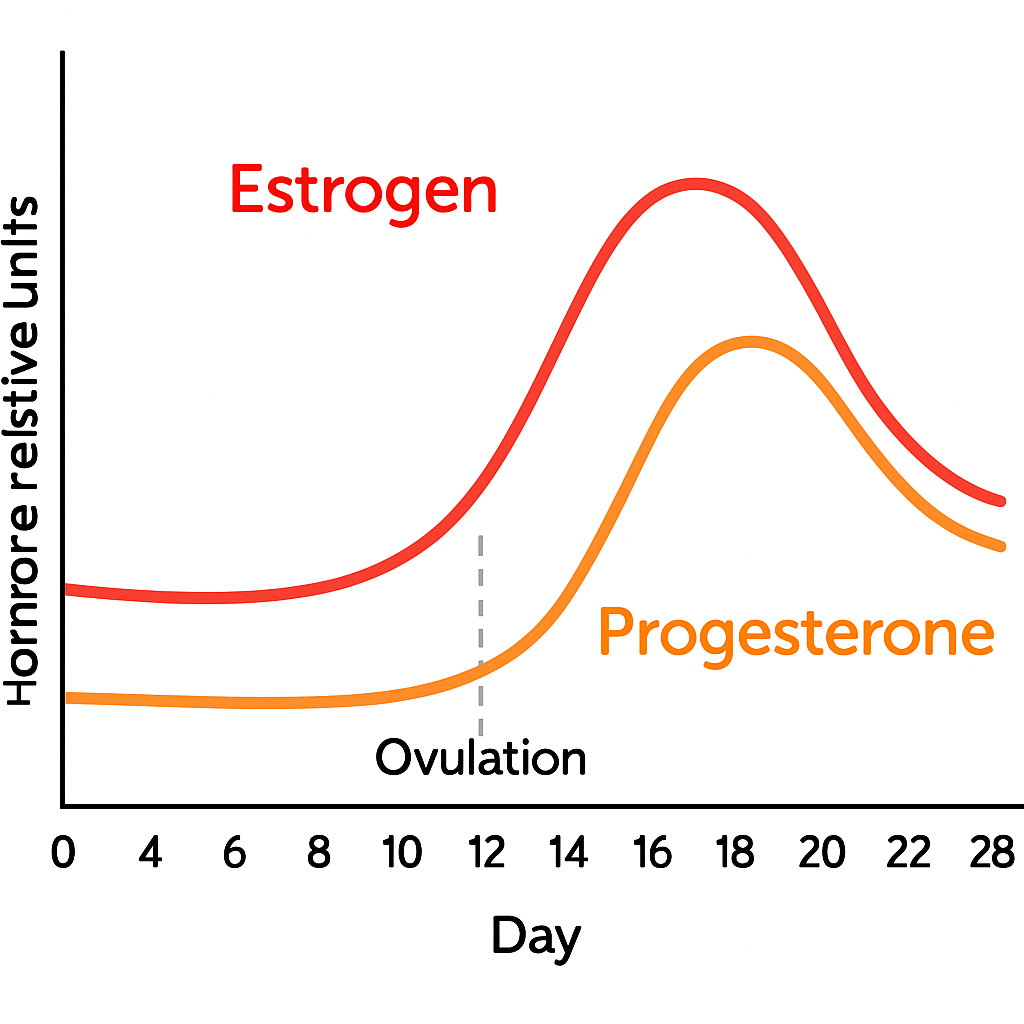
After ovulation, your body produces more progesterone to prepare the uterus for a possible pregnancy. This hormone is released by the corpus luteum, a temporary gland formed from the follicle that released the egg. Progesterone’s main job is to thicken and stabilize the uterine lining, making it ready for an embryo to implant. If you do not become pregnant, progesterone levels drop, leading to your next period.
Measuring progesterone after ovulation is important for several reasons:
- It confirms that ovulation has actually occurred.
- It helps assess whether your body is producing enough progesterone to support a potential pregnancy.
- It can guide your healthcare provider in diagnosing fertility issues and planning treatment.
A single blood test showing a progesterone level of at least 5 nanograms per milliliter (ng/mL) about a week after ovulation is highly specific (98.4%) and sensitive (89.6%) for confirming ovulation. According to the American College of Obstetricians and Gynecologists (ACOG), this measurement is a practical and reliable way to check if your cycle is functioning as it should.
Want the bigger picture? See how this value fits into a full Fertility Blood Panel.
Is “Day-21” always the right day to test progesterone?
“Day-21” is not always the best day to test your progesterone. The ideal timing depends on your unique menstrual cycle. The “Day-21” guideline assumes a 28-day cycle with ovulation on day 14, but many people ovulate earlier or later. If your cycle is longer or shorter, testing on day 21 may miss your true progesterone peak.
For the most accurate results, aim to test about 7 days after you ovulate—this is when progesterone should be at its highest. For example, if you ovulate on day 18, your optimal test day would be around day 25. Research shows that measuring progesterone later in the cycle, such as days 25–26, can improve the accuracy of diagnosing luteal phase issues, especially if your cycles are not exactly 28 days long.
Consider these timing truths:
- Progesterone can fluctuate up to eight-fold in 90 minutes.
- A single mistimed draw is the top reason for “false-low” results.
- Tools like ovulation predictor kits, basal body temperature charts, or Follicle Scans help you nail the exact 7 days-past-ovulation (7 DPO) window.
As Dr. Farahnaz Farzaneh, MD, reproductive endocrinologist, explains: “Elevated serum progesterone levels on the day of oocyte retrieval may predict positive pregnancy outcomes, highlighting the importance of monitoring progesterone to optimize the success rate of assisted reproductive technology”. Always track your ovulation and discuss timing with your healthcare provider to ensure your results truly reflect your body’s cycle.
How do doctors interpret Day-21 progesterone numbers?
Doctors interpret your Day-21 progesterone results by looking for evidence that you have ovulated and that your body is producing enough progesterone to support a possible pregnancy. In a natural cycle, a progesterone level above about 5 nanograms per milliliter (ng/mL) typically confirms ovulation. Higher levels—often above 10 ng/mL—suggest a strong ovulatory response, while lower levels may indicate that ovulation did not occur or that the luteal phase is not robust enough to support implantation.
Here’s how your results are generally viewed:
| Interpretation | ng/mL | nmol/L | What it means |
|---|---|---|---|
| Likely no ovulation | < 3 | < 9.5 | Anovulatory or badly mistimed test |
| Borderline / gray zone | 3 – 5 | 9.5 – 15.9 | Possible ovulation; retest or confirm timing |
| Confirmed ovulation | ≥ 5 – 6 | ≥ 15.9 – 19 | Corpus luteum active |
| Optimal natural cycle | ≥ 10 | ≥ 31.8 | Strong luteal support |
| Medicated cycles (Clomid, Letrozole, IVF) | ≥ 10 – 15 | ≥ 31.8 – 47.7 | Target often set higher |
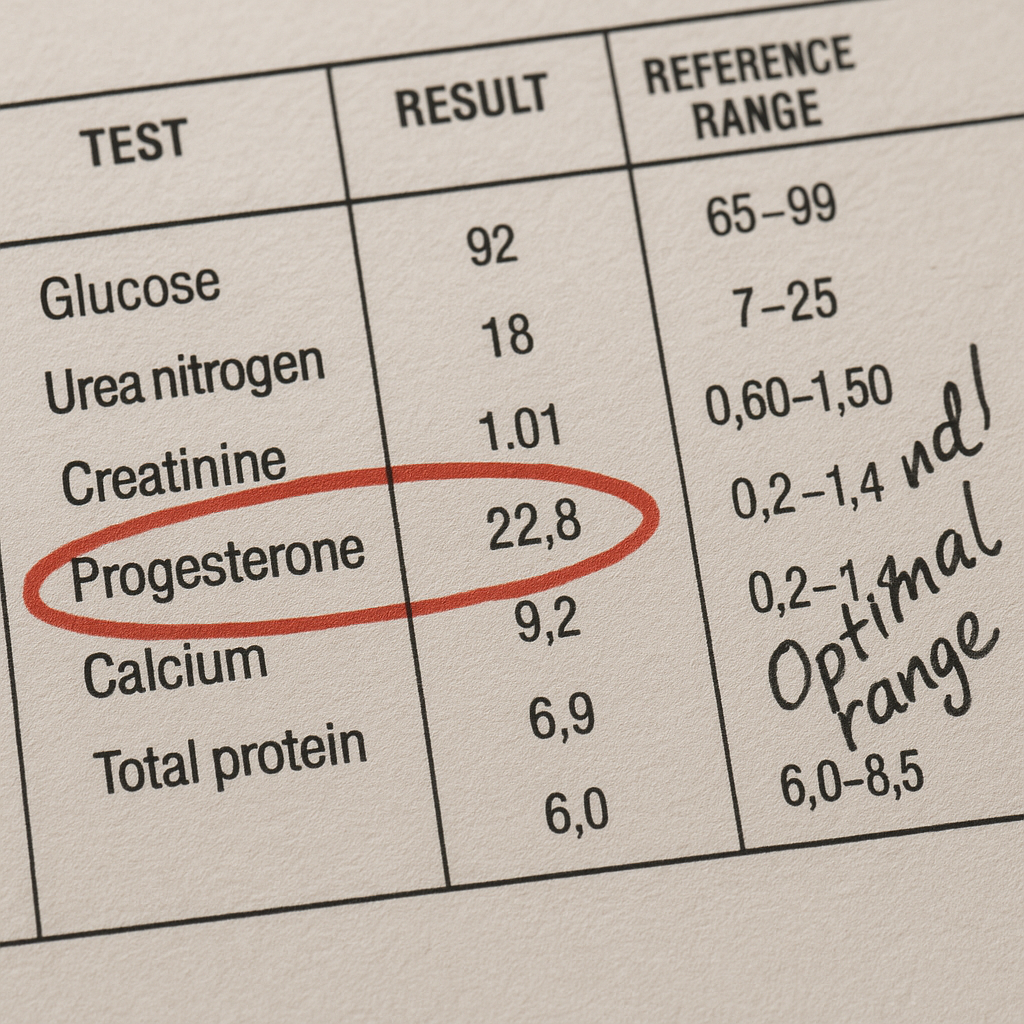
Lab cut-offs vary, so always request the reference interval that prints beside your result.
If you are undergoing fertility treatments, your doctor may look for even higher progesterone levels, especially if you are taking supplements or medications. In assisted reproductive technology cycles, such as in vitro fertilization, doctors may monitor progesterone to optimize timing and support, but the interpretation can differ based on your treatment plan. Always discuss your specific results with your healthcare provider, as individual factors and timing can affect interpretation.
What if your progesterone is low—mistiming or luteal phase defect?
If your progesterone is low, it can be due to either mistiming of the test or a true luteal phase defect. Mistiming is common—if the blood test is not done about 7 days after ovulation, your progesterone may appear falsely low, even if your body is functioning normally. This is why tracking ovulation and timing your test carefully is so important.
A luteal phase defect (LPD) means your body is not producing enough progesterone after ovulation, or your uterine lining is not responding properly to the hormone. LPD can be linked to a luteal phase shorter than 10 days and may contribute to difficulties with implantation or early pregnancy loss, but the exact role of LPD in infertility is still debated. There is no single, validated test for LPD, and low progesterone on one test does not always confirm the diagnosis.
If your progesterone is low, your doctor will consider both timing and your overall cycle history before diagnosing LPD. As experts note, “the current lack of validated diagnostic criteria creates a challenge for its routine incorporation in the workup of infertility” 1. If LPD is suspected, your provider may recommend further evaluation or, in some cases, discuss progesterone supplementation, though evidence for its effectiveness remains mixed.
Quick decision guide:
- Check timing: Was the draw exactly 7 DPO or 7 days before your expected period?
- If mistimed, repeat next cycle with precise tracking.
- If correctly timed and < 5 ng/mL, discuss possible luteal phase defect (LPD).
- Confirm ovulation with ultrasound or a second hormone panel.
- Consider an endometrial lining assessment such as the Endometrial Receptivity Test.
A true LPD often shows a luteal phase shorter than 11 days or persistently low progesterone despite perfect timing.
Which evidence-based strategies can raise mid-luteal progesterone?
Evidence-based strategies to raise mid-luteal progesterone focus on supplementing with progestogens, especially in fertility treatments or when luteal phase deficiency is suspected. The most effective and widely used approach is progesterone supplementation, which can be administered vaginally, orally, intramuscularly, or subcutaneously. Studies show that progesterone support after ovulation induction or intrauterine insemination increases live birth and clinical pregnancy rates compared to no treatment, particularly when gonadotropins are used for stimulation. There is no clear evidence that higher doses or longer duration of progesterone further improve outcomes, so standard dosing is typically recommended.
Adding oral dydrogesterone to vaginal progesterone may further improve live birth rates and reduce miscarriage in frozen embryo transfer cycles. In assisted reproduction, both progesterone and human chorionic gonadotropin (hCG) can be used for luteal phase support, but hCG increases the risk of ovarian hyperstimulation and is less commonly recommended. The route of progesterone administration (vaginal, oral, intramuscular, or subcutaneous) does not significantly affect pregnancy outcomes, so the choice can be tailored to your comfort and preference.
For those trying to conceive naturally, the benefit of progesterone supplementation is less clear, but it may be considered in cases of unexplained infertility or recurrent pregnancy loss. As Dr. G. Casarramona, MD, notes: “Progesterone luteal phase support after ovarian stimulation and intrauterine insemination leads to higher live birth and clinical pregnancy rates than no support, with no increase in miscarriage or multiple pregnancy rates”. Always consult your healthcare provider to determine the best strategy for your individual needs.
Could a high Day-21 progesterone signal pregnancy or twins?
A high Day-21 progesterone level can sometimes suggest early pregnancy, as progesterone rises after ovulation and remains elevated if implantation occurs. However, a single high value is not a definitive sign of pregnancy, since progesterone naturally peaks in the mid-luteal phase even in non-pregnant cycles. In the case of twin pregnancies, progesterone levels may be somewhat higher due to the increased hormonal activity from two developing embryos, but research shows that routine progesterone measurements are not reliable for diagnosing twins or confirming pregnancy. Instead, pregnancy is best confirmed with a positive hCG test, and twins are diagnosed by ultrasound.
While persistently high progesterone after the expected period can support the likelihood of pregnancy, and possibly twins, it should not be used alone for diagnosis. In summary, high Day-21 progesterone may be a reassuring sign that ovulation has occurred and the luteal phase is robust, but it is not a specific marker for pregnancy or multiples.
Your Top Questions, Answered
Can I check progesterone at home?
Currently, there are no widely available, reliable at-home blood tests for mid-luteal progesterone. Most accurate testing requires a blood draw at a clinic or lab, though some companies are developing home collection kits. For now, in-person testing remains the standard for precise results.
Does insurance usually cover the test?
Insurance often covers progesterone testing when ordered for fertility evaluation or related medical reasons, but coverage varies by plan. A quick call or a telehealth consult with billing codes in hand clarifies your cost.
Can low progesterone alone prevent pregnancy?
Low mid-luteal progesterone can make it harder for the uterine lining to support implantation, potentially lowering pregnancy chances, especially in assisted reproduction cycles. However, low progesterone is rarely the sole cause of infertility, and other factors are usually involved.
What number confirms ovulation?
A mid-luteal progesterone level above 5 ng/mL generally confirms ovulation, with levels above 10 ng/mL considered more reassuring for fertility and pregnancy support.
How soon after a low result should I retest?
If your progesterone result is low, retesting in the next cycle—timed about 7 days after ovulation—can help determine if the low value was due to mistiming or a consistent issue. In fertility treatments, doctors may adjust progesterone support immediately if low levels are detected around embryo transfer, as “rescue” dosing can improve outcomes to match those with adequate progesterone. Always consult your provider for personalized timing and follow-up.
Final Thoughts
Day-21 progesterone testing is a valuable tool for assessing whether ovulation has occurred and if the luteal phase is sufficient to support early pregnancy. A level above 5 ng/mL typically confirms ovulation, while higher values are more reassuring for fertility, especially in assisted reproduction settings. However, interpretation must consider timing, as testing too early or late in the cycle can yield misleading results.
In fertility treatments, both oral and intramuscular progesterone can achieve adequate hormone levels, but the route of administration may affect implantation rates. While high Day-21 progesterone can be a positive sign, it is not a definitive marker for pregnancy or multiples, and low values may reflect either mistiming or a true luteal phase issue. Ultimately, Day-21 progesterone is one piece of the fertility puzzle, best interpreted alongside other clinical findings and in consultation with a healthcare provider.
Download our free Mid-Luteal Timing Calculator and explore the full Fertility Workup Guide to keep momentum on your path to parenthood. Remember, the better you understand your hormones, the more empowered you are to welcome the baby you’re dreaming of.
References
-
Random serum progesterone threshold to confirm ovulation. Steroids, 101, 125-129. https://doi.org/10.1016/j.steroids.2015.06.013
-
Serum Progesterone Levels on the Day of Oocyte Retrieval as a Predictor of Pregnancy Outcomes in Fresh Embryo Transfer Cycles. Journal of Reproduction & Infertility, 25, 272 - 280. https://doi.org/10.18502/jri.v25i4.18125
-
Luteal Phase Defects and Progesterone Supplementation. Obstetrical & Gynecological Survey, 79, 122 - 128. https://doi.org/10.1097/OGX.0000000000001242
-
Luteal phase support for assisted reproduction cycles… The Cochrane database of systematic reviews, 7, CD009154. https://doi.org/10.1002/14651858.CD009154.pub3
-
Luteal Phase Support Using Subcutaneous Progesterone: A Systematic Review. Frontiers in Reproductive Health, 3. https://doi.org/10.3389/frph.2021.634813
-
Luteal Phase Support in IVF: Comparison Between Evidence-Based Medicine and Real-Life Practices. Frontiers in Endocrinology, 11. https://doi.org/10.3389/fendo.2020.00500
-
Micronized progesterone plus dydrogesterone versus micronized progesterone alone for luteal phase support in frozen-thawed cycles (MIDRONE): a prospective cohort study… Human reproduction. https://doi.org/10.1093/humrep/deab093
-
Luteal phase support for women trying to conceive by intrauterine insemination or sexual intercourse… The Cochrane database of systematic reviews, 8, CD012396. https://doi.org/10.1002/14651858.CD012396.pub2
-
Progesterone Luteal Support in Natural Cycles for Unexplained Infertility: A Randomised Controlled Trial (The PiNC Trial)… BJOG : an international journal of obstetrics and gynaecology. https://doi.org/10.1111/1471-0528.18171
-
The efficacy and safety of luteal phase support with progesterone following ovarian stimulation and intrauterine insemination: A systematic review and meta-analysis. Frontiers in Endocrinology, 13. https://doi.org/10.3389/fendo.2022.960393