You may feel anxious about your first transvaginal ultrasound. This is completely normal. Many people share concerns about what to expect, privacy, and comfort. Transvaginal ultrasound is a common and safe procedure used to assess fertility, early pregnancy, and gynecological health. Each year, thousands undergo this scan to gain vital information about their reproductive system and to guide important decisions about care.
Transvaginal ultrasound offers clear, detailed images of your uterus and ovaries. It is the preferred method for early pregnancy evaluation, helping to confirm pregnancy location, detect complications, and assess fetal health. The procedure is quick, usually lasting less than 30 minutes, and is performed by trained professionals who prioritize your dignity and comfort throughout the process.
Understanding what will happen during your scan can ease your mind. You have the right to ask questions and express your needs at any time. Your comfort and well-being are central to the care you receive.
- Why is a transvaginal ultrasound the top starting test in fertility care?
- How should you prepare the night before and the morning of the scan?
- What happens step-by-step from check-in to probe removal?
- What exactly is the clinician looking for and how does it boost conception odds?
- Does a transvaginal ultrasound hurt, and how can you maximize comfort?
- What happens right after the scan, and when will you get results?
- How does this scan integrate with other fertility tests on your roadmap?
- What if the ultrasound reveals something abnormal?
- Where can you find emotional
- Your Top Questions, Answered
- Final Thoughts
- References
Why is a transvaginal ultrasound the top starting test in fertility care?
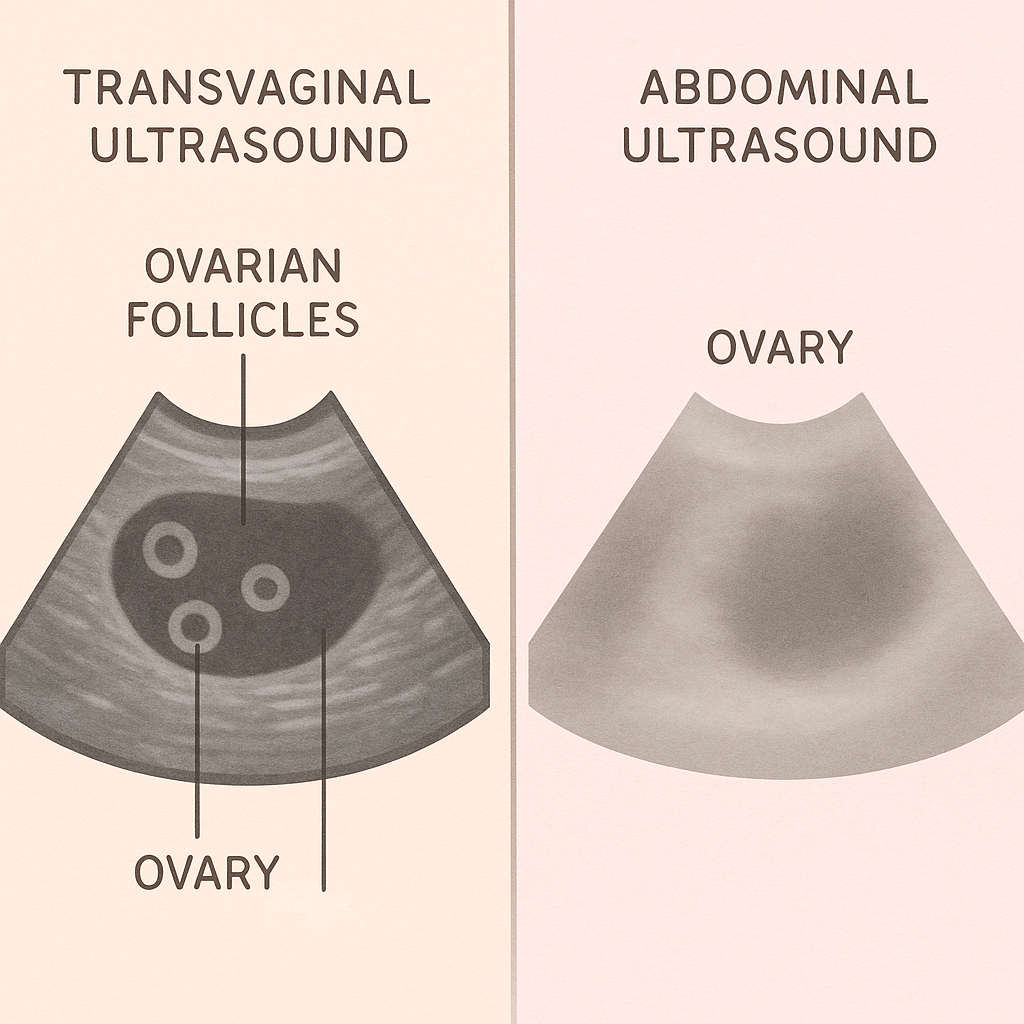
A transvaginal ultrasound is often the first test in fertility care because it provides a clear, detailed view of your reproductive organs. This imaging allows your provider to assess your uterus, ovaries, and endometrial lining with high accuracy. It can quickly identify common causes of infertility, such as polycystic ovary syndrome, fibroids, endometriosis, or structural abnormalities, without the need for invasive procedures. According to the American College of Obstetricians and Gynecologists (ACOG), transvaginal ultrasound is a safe, cost-effective, and rapid diagnostic tool that helps guide your next steps in fertility care 10.
Key reasons for its use include:
- High sensitivity for detecting uterine and ovarian conditions that may affect fertility.
- Ability to monitor your ovarian reserve and follicle development, which is crucial for planning treatments like in vitro fertilization (IVF).
- Non-invasive nature, making it more comfortable and accessible than surgical alternatives.
A recent peer-reviewed study in F1000Research (2023) found that transvaginal ultrasound can reduce the need for more invasive tests, streamlining your fertility evaluation and care. As Dr. Nirja Thaker, MD, reproductive medicine specialist, notes: “Transvaginal ultrasound is the cornerstone of infertility diagnosis, offering rapid, reliable insights that shape effective treatment plans.”
How should you prepare the night before and the morning of the scan?
To prepare thoroughly for your transvaginal ultrasound, follow these detailed steps to ensure comfort and accuracy:
The night before:
- Eat and drink as you normally would; no fasting is required.
- Take your regular medications unless your provider gives different instructions.
- If you are being evaluated for deep endometriosis, your provider may recommend a mild bowel preparation, such as a gentle laxative or enema, to improve image clarity. This is not needed for most routine fertility scans.
The morning of your scan:
- Shower or bathe as usual.
- Wear comfortable, easily removable clothing.
- Empty your bladder just before the procedure, unless told otherwise. A full bladder is not necessary for transvaginal ultrasound.
- Bring a list of your current medications and any questions you want to discuss.
- If you are menstruating, you can still have the scan; this does not affect the results or your provider’s ability to perform the test.
Dr. S. Guerriero, MD, a leading expert in gynecologic imaging, states, “Routine bowel preparation is not necessary for standard transvaginal ultrasound, but it can significantly improve detection of rectosigmoid endometriosis when specifically indicated”.
A 2024 meta-analysis found no significant difference in diagnostic accuracy between bowel preparation with or without water contrast, so most people do not need special preparation unless your provider suspects deep endometriosis. Following these steps will help you feel prepared and confident for your scan.
What happens step-by-step from check-in to probe removal?
When you arrive for your transvaginal ultrasound, you will check in at the front desk and confirm your identity and appointment details. You may be asked to complete or review paperwork about your medical history and current symptoms. A staff member will then guide you to a private exam room, where you will be given privacy to undress from the waist down and cover yourself with a drape or sheet.
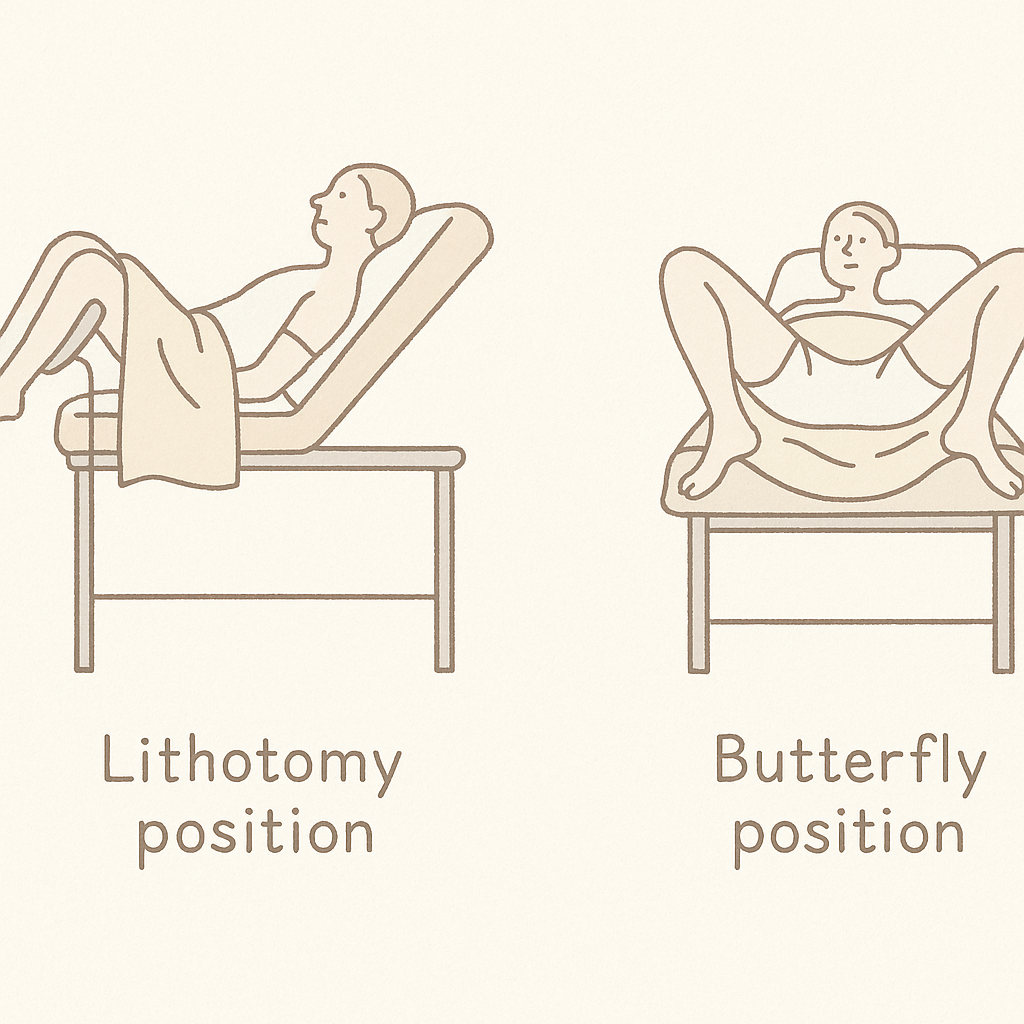
Once you are ready, a trained sonographer or healthcare provider will enter and explain the procedure, answering any questions you have. You will lie on an exam table, usually with your knees bent and feet placed together or in stirrups. The provider will put a sterile, single-use cover (often a condom or specialized sheath) over the ultrasound probe and apply a small amount of sterile gel to ensure clear imaging and comfort.
The provider will gently insert the thin, lubricated probe a few inches into your vagina. You may feel some pressure, but it should not be painful. The probe is moved slightly to capture images of your uterus, ovaries, and surrounding structures. The provider may ask you to adjust your position or perform gentle movements to improve the view. The scan typically takes 10–20 minutes 7.
After the imaging is complete, the provider will carefully remove the probe and leave the room so you can dress. The probe is then cleaned and disinfected according to strict infection control guidelines to prevent any risk of infection. You will have a chance to discuss initial findings or next steps before leaving. This process is designed to protect your privacy, dignity, and comfort at every stage.
What exactly is the clinician looking for and how does it boost conception odds?
During a transvaginal ultrasound, your clinician is looking closely at your uterus, ovaries, fallopian tubes, and surrounding pelvic structures. The main goals are to identify any abnormalities that could affect your ability to conceive, such as polycystic ovary syndrome (PCOS), fibroids, endometriosis, ovarian cysts, or structural issues like uterine septum or adhesions. The scan also assesses the thickness and quality of your endometrial lining, which is crucial for embryo implantation. By detecting these issues early, your care team can tailor treatments to address specific barriers to conception, improving your chances of success.
Transvaginal ultrasound also plays a key role in monitoring your response to fertility medications and tracking follicle development during ovulation induction or in vitro fertilization (IVF). For those undergoing IVF, ultrasound guidance during embryo transfer has been shown to significantly increase pregnancy and implantation rates—one study found rates nearly doubled compared to transfers done without ultrasound guidance (28.9% vs. 13.1% pregnancy rate). This precision helps ensure embryos are placed in the optimal location within the uterus, further boosting your odds of conception.
As reproductive medicine specialist, explains: “Transvaginal ultrasound is an accurate, cost-effective, and rapid method in diagnosing the causes of infertility, which can reduce the need for invasive procedures like hysteroscopy”. This approach not only clarifies your fertility picture but also helps you and your provider make informed, effective decisions to maximize your chances of building a family.
Does a transvaginal ultrasound hurt, and how can you maximize comfort?
A transvaginal ultrasound is generally not painful for most people, but you may feel mild pressure or brief discomfort during probe insertion. Studies show that the majority of patients report the procedure as comfortable or only mildly uncomfortable, with 45.5% agreeing they felt comfortable and most rating pain as low on standard scales 3. However, those with a history of pelvic pain or endometriosis may experience more discomfort. Anxiety, embarrassment, and lack of information can increase perceived pain.
To maximize your comfort:
- Ask your provider to explain each step before and during the scan.
- Request a warm, private environment and use of warm lubricant.
- Practice slow, deep breathing to relax your pelvic muscles.
- Let your provider know if you feel pain—they can adjust their technique.
- Bring a support person if it helps you feel at ease.
As Dr. J.J. Lee, MBBS, MRCOG, notes: “Adequate information and a supportive environment are key to a positive experience during transvaginal ultrasound”. If you have concerns about pain, discuss them with your clinician beforehand so they can tailor the approach to your needs.
What happens right after the scan, and when will you get results?
Immediately after your transvaginal ultrasound, the clinician will gently remove the probe and provide you with tissues or wipes to clean off any remaining gel. You will be given privacy to get dressed. There is typically no special aftercare required, and you can resume normal activities right away, as the procedure is minimally invasive and rarely causes side effects. The clinician may briefly discuss what was seen during the scan, but a detailed interpretation often requires review by a radiologist or your primary provider.
The images and findings are usually analyzed soon after the scan. In many clinics, preliminary results may be shared with you before you leave, especially if the scan was performed by your fertility specialist or gynecologist. However, in some cases, you may need to wait a few days for the official report, which will be sent to your referring doctor or discussed at your next appointment. If a biopsy or additional testing was performed during the scan, those results may take longer, as tissue samples require laboratory analysis. If any urgent findings are detected, your provider will contact you promptly to discuss next steps. Overall, the process is designed to be efficient and to minimize waiting time for results, allowing you to move forward with your fertility or gynecologic care as soon as possible.
- Normal scan → continue cycle monitoring or move to Day-21 progesterone testing via Day-21 Progesterone: Why It Matters.
- Abnormal scan → schedule targeted tests, surgery, or medication changes.
Ask for printouts or patient-portal access; keeping your own image file streamlines second opinions.
How does this scan integrate with other fertility tests on your roadmap?
Transvaginal ultrasound is a foundational step in the fertility evaluation roadmap, working alongside other tests to provide a comprehensive picture of reproductive health. It is often the first-line imaging tool, used to assess the uterus, ovaries, and endometrial lining for structural abnormalities, ovarian reserve (via antral follicle count), and ovulatory status. This scan complements blood tests such as anti-Müllerian hormone (AMH) and follicle-stimulating hormone (FSH), which measure ovarian reserve from a hormonal perspective, while ultrasound provides a direct count of developing follicles—often considered more accurate for predicting ovarian response to stimulation in IVF.
Transvaginal ultrasound also guides the timing and monitoring of ovulation, tracks follicle growth during fertility treatments, and helps plan procedures like egg retrieval or embryo transfer, where real-time imaging can improve success rates. When combined with other diagnostic tools such as hysterosalpingography (to check fallopian tube patency), hysteroscopy (for direct uterine visualization), and semen analysis—it enables clinicians to pinpoint causes of infertility and tailor treatment plans. While ultrasound excels at detecting structural and some functional issues, it is most effective when integrated with hormonal, genetic, and lifestyle assessments for a holistic approach to fertility care. This integration streamlines diagnosis, reduces the need for invasive procedures, and helps optimize the chances of conception.
What if the ultrasound reveals something abnormal?
If a transvaginal ultrasound reveals something abnormal, the next steps depend on the specific findings and your symptoms. Common abnormalities include uterine fibroids, polyps, ovarian cysts, endometrial thickening, or signs of malignancy. For example, if fibroids or polyps are detected, your clinician may recommend further evaluation with additional imaging, a biopsy, or procedures like hysteroscopy to confirm the diagnosis and guide treatment. If the scan shows endometrial thickening or suspicious masses, especially in postmenopausal women, a biopsy may be performed to rule out cancer.
In cases of acute symptoms, such as severe pain or bleeding, findings like adnexal torsion or vascular abnormalities may require urgent intervention or surgery. Sometimes, the ultrasound may also detect non-gynecological issues, such as urinary tract or bowel abnormalities, which would prompt referral to the appropriate specialist. Your provider will discuss the results with you, explain what they mean, and outline a personalized plan for follow-up, which may include monitoring, medication, or surgical options depending on the diagnosis and your fertility goals. The integration of ultrasound findings with your overall clinical picture ensures that any abnormality is addressed promptly and appropriately to optimize your health and fertility outcomes.
Where can you find emotional
Finding emotional support, inclusive care, and cost clarity during fertility treatment can be challenging, but several resources and approaches can help. Many patients report that emotional support from clinics is often lacking, with less than half perceiving a supportive culture and many desiring more accessible support services within their clinics. Peer support groups, both online and in-person, can provide valuable emotional connection and shared experiences, especially when clinic-based support falls short. Inclusive care means clinics should recognize and respect diverse backgrounds, relationship types, and cultural needs, as patient-centered frameworks emphasize the importance of individualized, respectful care that considers emotional, physical, and financial burdens.
For emotional well-being, psychological counseling offered in person or increasingly via telemedicine, can help manage anxiety, depression, and the unique stresses of fertility treatment. Clinics that provide clear, upfront information about treatment costs, insurance coverage, and financial assistance options help patients make informed decisions and reduce financial stress. Decision support tools and transparent communication about risks, timelines, and costs are key to patient-centered, inclusive care. Ultimately, seeking clinics that prioritize open communication, offer or refer to mental health professionals, and provide clear cost breakdowns can significantly improve the fertility treatment experience.
Your Top Questions, Answered
Can I have the scan while on my period?
Yes, you can have a transvaginal ultrasound during your period. Bleeding does not interfere with the ability to assess ovarian reserve or antral follicle count, and the scan can be performed on any day of the menstrual cycle for fertility evaluation .
How many ultrasounds will I need in an IVF cycle?
You will typically need several ultrasounds, usually between 3 and 6—during an IVF cycle. These scans monitor follicle development, endometrial thickness, and help time egg retrieval for the best results.
Is any radiation involved?
No, there is no radiation involved in transvaginal or abdominal ultrasound. These imaging techniques use sound waves, making them safe for reproductive organs and early pregnancy.
Can I refuse the internal scan and choose an abdominal one?
You can refuse a transvaginal (internal) scan and request an abdominal ultrasound, but abdominal scans are generally less detailed for visualizing ovaries and early follicles. This may limit the information available for fertility assessment. Virtual, self-administered transvaginal ultrasounds are also emerging as an alternative, offering similar accuracy and greater patient satisfaction.
Will the ultrasound affect my egg reserve?
A standard transvaginal ultrasound does not affect your egg reserve or harm your ovaries. It is a noninvasive imaging technique that observes the follicles and ovarian structure without causing damage or loss of eggs.
Final Thoughts
Transvaginal ultrasound is a highly valuable tool in gynecology and fertility care, offering detailed images of pelvic organs and enabling early, accurate diagnosis of conditions like ectopic pregnancy, cervical changes, and pelvic masses. Its benefits include higher diagnostic accuracy compared to abdominal ultrasound, minimal invasiveness, and the ability to guide procedures such as embryo transfer and biopsies, which can improve IVF outcomes and reduce the need for more invasive surgeries. However, it is an intimate and sometimes uncomfortable procedure, and universal use may not always improve outcomes or be necessary for every patient, especially if risk factors are absent.
Risks are generally low but include the potential for minor discomfort, rare infection transmission (which can be minimized with proper probe cleaning and single-use covers), and, in rare cases, complications during procedures like selective embryo reduction. Careful patient selection, informed consent, and adherence to infection control protocols are essential to maximize safety and comfort. Overall, when used appropriately, transvaginal ultrasound is a safe, effective, and patient-friendly method that plays a central role in modern reproductive medicine.
When you’re ready to pair these images with your hormone story, explore Fertility Blood Tests: What Each Number Means. Every clear snapshot and data point puts you one step closer to the family you’re dreaming of.
References
-
The role of transvaginal sonography in diagnosis of female infertility: a study protocol. F1000Research. https://doi.org/10.12688/f1000research.140962.1
-
SMFM Patient Safety Guideline: Reducing the risk of transmitting infection by transvaginal ultrasound examination… American journal of obstetrics and gynecology. https://doi.org/10.1016/j.ajog.2020.05.043
-
Role of transvaginal ultrasound-guided biopsy in gynecology. International Journal of Gynecological Cancer, 30, 128 - 132. https://doi.org/10.1136/ijgc-2019-000734
-
Use of Trans-Vaginal Ultrasound to Diagnose and Treat Infertility and Its Performance. Open Journal of Radiology. https://doi.org/10.4236/ojrad.2023.133018
-
Transvaginal ultrasound with bowel preparation versus transvaginal ultrasound with bowel preparation and water contrast for diagnosing Recto-Sigmoid endometriosis. A systematic review and Meta-Analysis… European journal of obstetrics, gynecology, and reproductive biology, 297, 233-240. https://doi.org/10.1016/j.ejogrb.2024.04.015
-
Transvaginal ultrasound-guided embryo transfer in IVF… Journal of gynecology obstetrics and human reproduction, 46 5, 411-416. https://doi.org/10.1016/j.jogoh.2017.02.015
-
Relationship Between Ultrasound Diagnosis, Symptoms and Pain Scale Score on Examination in Patients with Uterosacral Ligament Endometriosis. Journal of Clinical Medicine, 13. https://doi.org/10.3390/jcm13226901
-
Patient perceptions of transvaginal ultrasound in the diagnosis and management of infertility: a cross-sectional study. International Journal Of Community Medicine And Public Health. https://doi.org/10.18203/2394-6040.ijcmph20244032