If you are considering intrauterine insemination (IUI), you are not alone. IUI is a common fertility treatment in the United States, often recommended as a first step for individuals and couples facing challenges with conception. Each year, thousands turn to IUI for its relative simplicity, lower cost compared to IVF, and its potential to help a wide range of people—including those with unexplained infertility, mild male factor infertility, or ovulation issues.
Your concerns about the IUI process are valid. Success rates for IUI can vary, with clinical pregnancy rates typically ranging from 7% to 19% per cycle, depending on factors like age, underlying fertility issues, and the specific protocols used. Advances in timing ovulation and sperm preparation have improved outcomes, but no single approach guarantees success for everyone. Understanding each step—from preparation to the pregnancy test can empower you to make informed decisions and advocate for your needs throughout the journey.
- What pre-IUI tests, habits, and timelines set the groundwork for success?
- Which fertility tests give you (and your doctor) the full picture?
- How does AMH influence medication choice and cycle planning?
- Which lifestyle tweaks move the needle?
- How do stimulation meds, follicle scans, and the trigger shot align the perfect IUI window?
- Clomid or Letrozole—what’s best for your ovaries?
- How do doctors know when follicles are ready?
- Why is the trigger shot the countdown clock?
- Do natural cycles work?
- What happens on IUI day, and how can you close overlooked gaps in care?
- What’s the minute-by-minute clinic flow?
- Does it hurt?
- Where does emotional support fit?
- How is care adapted for single parents and LGBTQ+ families?
- Can I skip leg elevation and day-long bedrest?
- What do’s, don’ts, and coping tools guide the infamous two-week wait (TWW)?
- Which physical guidelines actually matter?
- How do you decode every twinge?
- What keeps anxiety from taking over?
- When should you take a pregnancy test after IUI, and how do you read the results accurately?
- Why is day 14 the golden rule?
- How do you avoid false readings from the trigger shot?
- What if you see a faint line or no line at all?
- How do age, diagnosis, and cycle count alter your roadmap—and when should you pivot to IVF?
- What do the numbers say about age?
- How does your diagnosis steer expectations?
- How many tries make sense?
- Which lingering questions do readers ask most—and what are the concise, evidence-based answers?
- Final Thoughts
- References
What pre-IUI tests, habits, and timelines set the groundwork for success?
Which fertility tests give you (and your doctor) the full picture?
To prepare for IUI, you and your doctor should review several key fertility tests. For you, ovarian reserve tests like FSH and AMH, as well as assessments of endometrial thickness and tubal patency, are essential. For your partner, a thorough semen analysis including sperm count, motility, and morphology, is critical. Sperm DNA fragmentation testing (DFI) can further clarify the likelihood of IUI success, as lower DFI (<30%) is strongly linked to higher pregnancy rates. These tests help tailor your treatment and set realistic expectations. Review how each value fits into the puzzle in Fertility Blood Tests: What Each Number Means.
How does AMH influence medication choice and cycle planning?
AMH (anti-Müllerian hormone) reflects your ovarian reserve and helps guide medication choices for ovarian stimulation. Higher AMH levels suggest a greater number of eggs and may allow for lower medication doses, while lower AMH may prompt your doctor to adjust protocols to maximize your response. This individualized approach aims to optimize the number of mature follicles and improve your chances of success. Compare your number to the visuals in the AMH Levels Chart.
Which lifestyle tweaks move the needle?
- Eat a Mediterranean-style diet: colorful produce, lean protein, olive oil.
- Cap caffeine at 200 mg/day and skip alcohol or tobacco—smoking alone drops IUI success by about 3 %.
- Sleep 7–8 hours nightly and aim for 150 minutes of moderate exercise each week.
- For partners providing sperm: abstain 2–3 days, keep laptops off laps, and add antioxidants (vitamin C, CoQ10).
How do stimulation meds, follicle scans, and the trigger shot align the perfect IUI window?
Stimulation medications, follicle scans, and the trigger shot work together to time IUI for your best chance at pregnancy.
Clomid or Letrozole—what’s best for your ovaries?
Clomid and Letrozole are both effective, safe, and affordable first-line medications for ovarian stimulation in IUI cycles. Letrozole may offer slightly higher live birth rates and fewer side effects for some, but both are widely used and recommended. Your doctor will help choose based on your medical history, ovarian reserve, and how your body responds to stimulation. Dive deeper in Clomid vs. Letrozole.
How do doctors know when follicles are ready?
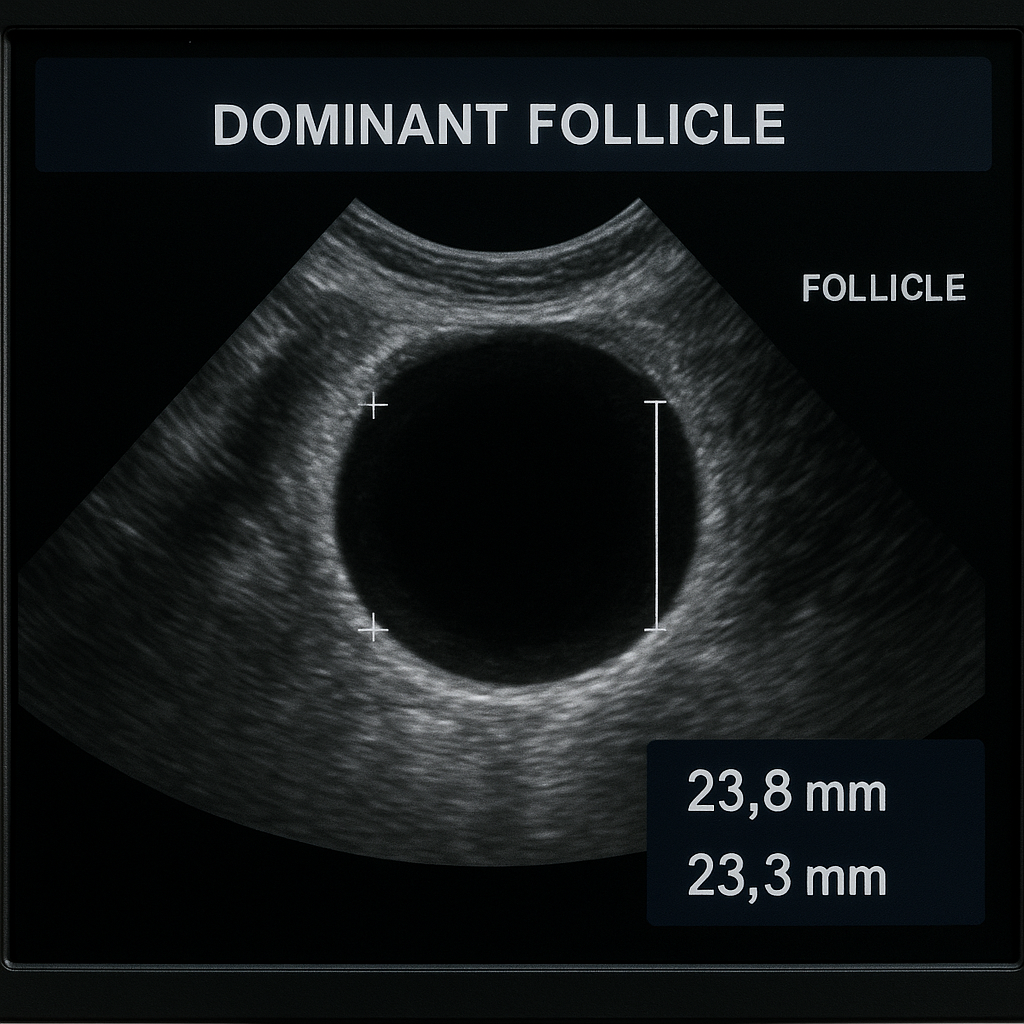
Doctors use ultrasound scans to monitor follicle growth during your cycle. When a leading follicle reaches about 18 mm in diameter, it is considered mature and ready for ovulation. The timing of the trigger shot and IUI is based on this measurement, ensuring insemination happens at the optimal moment. See step-by-step images in Follicle Scans 101.
Why is the trigger shot the countdown clock?
The trigger shot, usually hCG, induces ovulation about 36 hours after administration. This precise timing allows your doctor to schedule IUI so sperm and egg meet at the best possible time, maximizing your chance of conception.
Do natural cycles work?
What happens on IUI day, and how can you close overlooked gaps in care?
What’s the minute-by-minute clinic flow?
On IUI day, you’ll check in and confirm your details. Your partner or donor provides a semen sample, which the lab processes to concentrate healthy sperm; a step that takes about 1–2 hours. When ready, you’ll be called to a private room. The clinician inserts a thin catheter through your cervix to place the sperm directly into your uterus, a process lasting just a few minutes. You may rest briefly afterward, but extended bedrest is not required. The entire visit usually takes 1.5–2.5 hours.
Does it hurt?
Most people experience only mild discomfort, similar to a Pap smear. Some report brief cramping or pressure during the procedure. Techniques like therapeutic touch or virtual reality can reduce pain and anxiety, and many find the experience tolerable and quick.
Where does emotional support fit?
Emotional support is vital. Anxiety is common on IUI day, but interventions such as therapeutic touch, calming environments, and supportive staff can lower stress and improve satisfaction. Clinics should offer compassionate care, clear communication, and access to counseling or support groups to help you feel seen and supported. If in-person visits feel overwhelming, check our Telehealth Tips for remote support options.
How is care adapted for single parents and LGBTQ+ families?
Inclusive clinics recognize diverse family structures. They offer tailored counseling, use gender-inclusive language, and respect your choices regarding donor sperm or eggs. Staff are trained to support single parents and LGBTQ+ families, ensuring you feel welcome and your needs are met throughout the process.
Can I skip leg elevation and day-long bedrest?
Yes, you can. Research shows that neither leg elevation nor prolonged bedrest after IUI improves pregnancy rates. Most clinics recommend resting for just a few minutes before resuming normal activities, so you can return to your day with confidence.
What do’s, don’ts, and coping tools guide the infamous two-week wait (TWW)?
Which physical guidelines actually matter?
During the two-week wait (TWW) after IUI, the most important physical guidelines are to continue any medications prescribed by your doctor, such as progesterone, and to maintain your usual daily activities unless you experience pain or bleeding. There is no evidence that strict bedrest, leg elevation, or major activity restrictions improve your chances of pregnancy—normal movement and gentle exercise are safe for most people. Some research suggests that medications like piroxicam, when prescribed by your doctor, may improve IUI success rates, but always consult your provider before starting anything new. Continue gentle movement such as yoga, walking, swimming. Avoid hot tubs or saunas above 101 °F / 38 °C. Take prenatal vitamins and stay hydrated.
How do you decode every twinge?
It’s completely normal to notice every cramp, twinge, or symptom during the TWW, but these sensations are rarely reliable indicators of pregnancy. Hormonal changes from fertility medications and the stress of waiting can cause bloating, breast tenderness, or mild cramping, which are also common premenstrual symptoms. Try not to over-interpret these signs, as they usually do not provide clear answers before your scheduled pregnancy test. Many people in this situation turn to online forums for reassurance and to share experiences, which can help normalize these feelings and reduce anxiety.
What keeps anxiety from taking over?
Coping with TWW anxiety is challenging, but support and distraction are key. Many people find comfort in online forums or support groups, where sharing experiences with others in the same situation can reduce feelings of isolation and stress. Mindfulness, gentle exercise, hobbies, and limiting internet symptom searches can also help. If anxiety feels overwhelming, consider reaching out to a counselor or therapist familiar with fertility journeys; emotional support is just as important as physical care during this time.
Find more community resources in Fertility Workup 101.

When should you take a pregnancy test after IUI, and how do you read the results accurately?
Why is day 14 the golden rule?
A pregnancy test is typically recommended 14 days after IUI because this timing allows for the most accurate detection of the pregnancy hormone (hCG) in urine or blood. Testing too early can lead to false negatives, as the embryo may not have implanted or started producing enough hCG to be detected. The “day 14” rule is based on the average time it takes for implantation and early hormone production after insemination, aligning with the natural menstrual cycle’s luteal phase. Some studies use a slightly later window, such as day 18, to confirm pregnancy and reduce the risk of ambiguous results, but day 14 remains the standard for most clinics. To read results accurately, follow the test instructions carefully and use first-morning urine for the highest hormone concentration. If the test is negative but your period does not start, repeat the test a few days later or consult your doctor for a blood test, which is more sensitive. This approach helps avoid the confusion and disappointment of testing too soon and ensures reliable results.
| Test type | Detectable hCG (mIU/mL) | Earliest accuracy |
|---|---|---|
| Urine strip | 20–25 | 14 days post-IUI |
| Clinic blood draw | 5 | 12–14 days post-IUI |
How do you avoid false readings from the trigger shot?
To avoid false readings from the trigger shot (hCG injection), it’s crucial to understand that the synthetic hCG used to trigger ovulation can remain in your system for up to 10–14 days after administration. If you take a pregnancy test too soon—before this medication has cleared—you may get a false positive, as the test cannot distinguish between hCG from the shot and hCG from an early pregnancy. That’s why most clinics recommend waiting at least 14 days after IUI before testing, as this allows time for the trigger shot to leave your body and for any pregnancy-related hCG to rise to detectable levels
What if you see a faint line or no line at all?
If you see a faint line on your pregnancy test, it could mean a low but rising level of hCG, which may indicate early pregnancy, or it could be residual hCG from the trigger shot if you tested too early. The only way to know for sure is to repeat the test after 48 hours: if the line gets darker, it suggests rising hCG from a pregnancy; if it fades or disappears, it was likely from the trigger shot. If there’s no line at all, the test is negative, but if your period hasn’t started, repeat the test in a few days to confirm. For the most reliable results, always use first-morning urine, follow the test instructions carefully, and consider a blood test at your clinic for a definitive answer, as blood tests can measure the exact hCG level and help distinguish between medication and pregnancy. Low or falling hCG points to chemical pregnancy, while stable progesterone (see Day-21 Progesterone) helps confirm an early but viable pregnancy.
How do age, diagnosis, and cycle count alter your roadmap—and when should you pivot to IVF?
What do the numbers say about age?
Per-cycle success averages:
• Under 35: 15–20 %
• 35–40: ~10 %
• Over 40: 2–5 %
Age is the most important predictor of IUI success. Women under 30 have the highest live birth rates per cycle (around 12%), but rates begin to decline after age 28 and drop further after 35, with women over 40 experiencing very low success; often less than 2% per cycle, and virtually negligible after age 43, regardless of stimulation or sperm source. For example, one study found a live birth rate of 7.2% per cycle with a mean age of 35, but almost no live births in women over 40.
How does your diagnosis steer expectations?
Diagnosis significantly affects IUI outcomes. IUI is most effective for anovulation (such as PCOS), unexplained infertility, and mild male factor infertility, with the highest success seen in anovulatory patients, where live birth and clinical pregnancy rates are notably higher than in other groups. For unexplained infertility and mild male factor, success rates are moderate, while women with diminished ovarian reserve or severe male factor infertility have much lower chances of success.
How many tries make sense?
Most pregnancies from IUI occur within the first three to four cycles, and cumulative success rates plateau after this point, suggesting limited benefit in continuing beyond four attempts. For women over 38, especially those over 40, or those with poor ovarian reserve, moving to IVF after one or two failed IUIs is generally recommended due to rapidly declining chances with further IUI. In summary, younger women with favorable diagnoses may try up to four IUIs, but older women or those with less favorable diagnoses should consider earlier transition to IVF for the best chance of success. If you’re still waiting after cycle 4, discuss IVF (see IVF Made Easy) or fertility preservation options like Egg Freezing 101.
Which lingering questions do readers ask most—and what are the concise, evidence-based answers?
Can acupuncture boost IUI success?
While most research focuses on acupuncture with IVF, some evidence suggests acupuncture may improve pregnancy rates, especially when performed during ovarian stimulation or around embryo transfer, and may also reduce anxiety. However, robust data specifically for IUI are limited, and benefits for IUI remain unproven; more research is needed to confirm any effect.
Is sex after IUI helpful or harmful?
Sex after IUI is generally considered safe and may even be beneficial. Some studies suggest that intercourse after IUI could improve pregnancy rates by stimulating uterine contractions that help sperm reach the egg, but there is no evidence of harm unless your doctor advises otherwise due to specific medical concerns.
What if my period is late but tests stay negative?
If your period is late and pregnancy tests remain negative, it could be due to delayed ovulation, stress, or hormonal fluctuations rather than pregnancy. If your period does not start within a week, repeat the test and consult your doctor to rule out other causes or to check for a very early pregnancy that may not yet be detectable.
How many IUIs before considering donor eggs or sperm?
Most pregnancies from IUI occur within the first three to four cycles. If you have not conceived after three to four IUIs; especially if you are over 35, have diminished ovarian reserve, or severe male factor infertility, it may be time to discuss moving to IVF or considering donor eggs or sperm, depending on your diagnosis and age. Donor sperm is often used after several unsuccessful IUIs with partner sperm or in cases of severe male infertility, while donor eggs are considered when ovarian reserve is very low or after repeated failed cycles.
Final Thoughts
In summary, the IUI roadmap is shaped by balancing effectiveness, safety, and cost. IUI is less invasive and more affordable than IVF, and is often recommended as a first-line treatment for certain infertility diagnoses, especially in younger women and those with unexplained infertility or mild male factor issues. Success rates per cycle are modest; typically around 7–12% and most pregnancies occur within the first three to four cycles. Ovarian stimulation can slightly improve outcomes but also increases the risk of multiple pregnancies, so protocols with mild stimulation and strict cancellation criteria are preferred to minimize complications.
While IUI is safer and more cost-effective than IVF, its effectiveness is limited, especially for older women or those with poor prognoses, who may benefit from earlier transition to IVF. Evidence-based guidelines recommend individualized treatment plans, careful monitoring, and timely reassessment to optimize results and minimize risks. Ultimately, IUI offers a reasonable, lower-risk starting point for many, but ongoing evaluation is essential to determine when to pivot to more advanced options like IVF. For deeper dives into related tests, explore the HSG Test: Can It Boost Pregnancy Odds? and Endometrial Receptivity Test: Timing Implantation Right. You’ve got the roadmap—now take each step with confidence and hope.
References
-
A new accurate model to assess intrauterine insemination success based on clinical parameters: Optimizing fertility treatment… International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics. https://doi.org/10.1002/ijgo.70104
-
The Timing and Dose Effect of Acupuncture on Pregnancy Outcomes for Infertile Women Undergoing In Vitro Fertilization and Embryo Transfer: A Systematic Review and Meta-Analysis… Journal of integrative and complementary medicine. https://doi.org/10.1089/jicm.2023.0478
-
How to dose follitropin delta for the first insemination cycle according to the ESHRE and ASRM guidelines; a retrospective cohort study. Journal of Ovarian Research, 16. https://doi.org/10.1186/s13048-022-01079-w
-
A proof-of-concept study evaluating the effect of personalized dosages of follitropin delta in intra-uterine insemination (IUI): Personalized IUI Treatment Study (PITS). Human Reproduction. https://doi.org/10.1093/humrep/deac107.725
-
The effect of virtual reality (VR) glasses and therapeutic touch (TT) on pain, anxiety, and patient satisfaction during intrauterine insemination (IUI) compared to standard care: a single-blind, randomized controlled trial. BMC Pregnancy and Childbirth, 25. https://doi.org/10.1186/s12884-025-07435-0
-
Outcome of single and double intrauterine insemination techniques in infertility cases. Journal of Marine Medical Society, 25, 193 - 197. https://doi.org/10.4103/jmms.jmms_50_23
-
Unlocking fertility success: A comprehensive exploration of age and intrauterine insemination outcomes. Medical Science. https://doi.org/10.54905/disssi.v28i146.e26ms3315
-
An evaluation of couples undergoing intrauterine insemination at the BioART Fertility Centre, Johannesburg. Global Reproductive Health, 9. https://doi.org/10.1097/GRH.0000000000000096