Fertility challenges can feel overwhelming and isolating. You may worry about your body’s ability to support conception and a healthy pregnancy. These concerns are valid and uterine blood flow plays a crucial role in nourishing the uterine lining and supporting embryo implantation.
Uterine blood flow is the movement of blood through the blood vessels that supply your uterus. This blood brings oxygen and nutrients to the uterine lining, creating a healthy environment for a fertilized egg to implant and grow. Good uterine blood flow is essential for supporting the placenta and the developing fetus during pregnancy, as it ensures that both receive the nourishment they need to thrive. If blood flow to the uterus is reduced, it can affect fertility and may lead to complications in pregnancy, such as poor fetal growth or other issues. In simple terms, uterine blood flow is like a delivery system, making sure your uterus gets everything it needs to support conception and a healthy pregnancy.
Many people seeking to grow their families wonder if there are simple, effective ways to improve this vital aspect of reproductive health. You deserve practical, compassionate guidance. While medical treatments are important, small changes in your daily routine can also make a difference. This article will explain why uterine blood flow matters and share easy moves and tips you can use to support your fertility journey.
- Why does uterine blood flow matter for conception success?
- How can you tell if your uterine blood flow needs a boost?
- Which everyday moves instantly wake up pelvic circulation?
- Which yoga poses and pelvic stretches target uterine arteries?
- Can nutrition and hydration really open uterine arteries?
- Do supplements like L-arginine and vitamin E work—and are they safe?
- How do warmth, massage, and acupuncture complement movement?
- When lifestyle fixes aren’t enough, what medical options exist?
- How should you track progress and stay consistent?
- Addressing special cases: PCOS, fibroids, and endometriosis—do the rules change?
- Your top uterine blood flow questions answered
- Final Thoughts
- References
Why does uterine blood flow matter for conception success?
Uterine blood flow is vital for conception because it delivers oxygen and nutrients to your uterine lining, making it receptive for embryo implantation. When blood flow is optimal, your endometrium can better support the early stages of pregnancy. Research published in 2021 highlights that endometrial perfusion, how well blood flows through the uterine lining is directly linked to pregnancy outcomes, both in natural and assisted reproduction settings. Conditions like endometriosis or chronic inflammation can reduce this blood flow and limit your chances of successful implantation.
Key reasons uterine blood flow matters for conception:
- Supports embryo implantation by nourishing the uterine lining
- Helps synchronize the uterus with hormonal changes needed for pregnancy
- Reduces the risk of complications linked to poor endometrial health As Dr. P. Pierzyński, reproductive medicine expert, notes: “Endometrial perfusion was shown to be an independent receptivity parameter, showing a direct association with pregnancy outcomes”. Understanding and supporting your uterine blood flow can help you take positive, evidence-based steps on your fertility journey as in Healthy Uterine Lining.
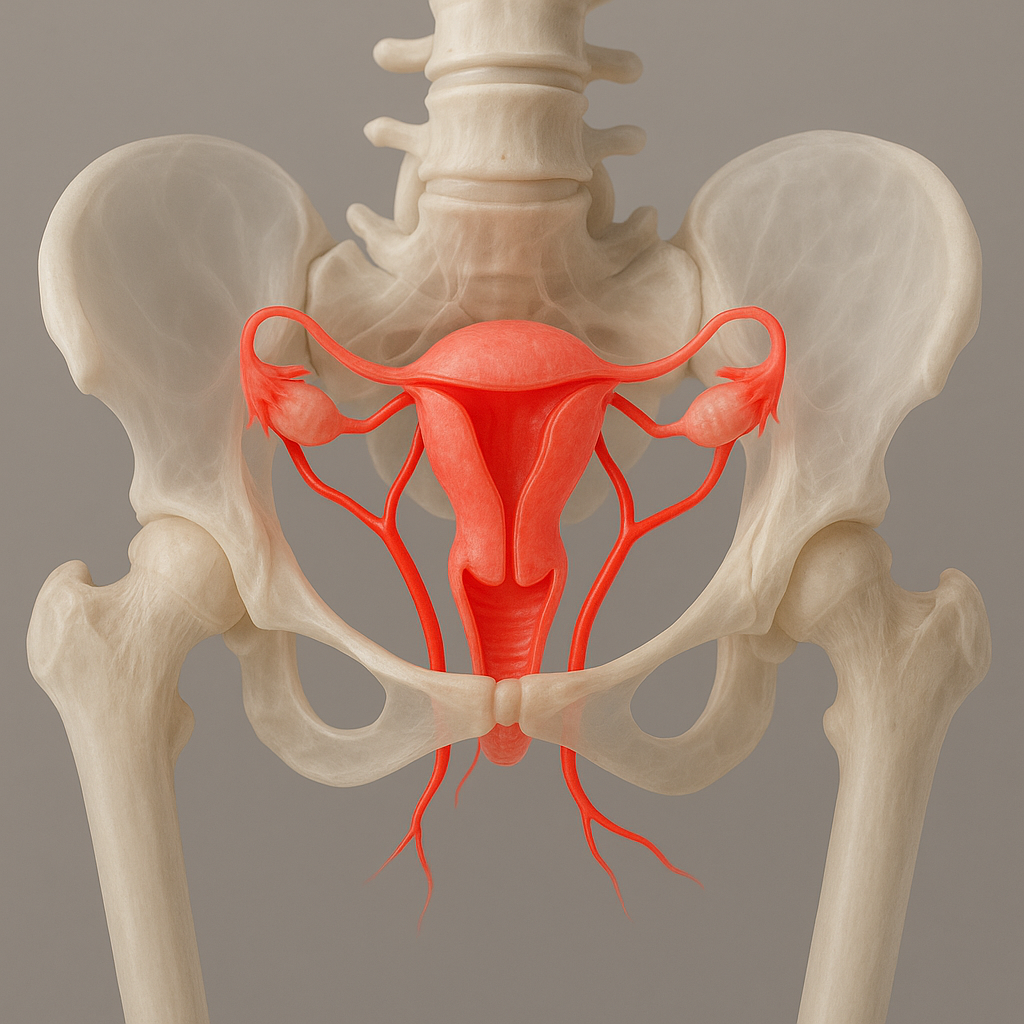
How can you tell if your uterine blood flow needs a boost?
You may not notice obvious symptoms if your uterine blood flow is low, but certain signs and risk factors can suggest you might benefit from a boost. If you have experienced repeated implantation failure, recurrent pregnancy loss, or unexplained infertility, your uterine blood flow could be a factor. Health conditions such as high blood pressure, endometriosis, or a history of preeclampsia may also increase your risk.
To assess your uterine blood flow, your healthcare provider may use a Doppler ultrasound. This non-invasive test measures how well blood moves through your uterine arteries. Abnormal results such as a high pulsatility index or low blood flow volume can indicate reduced perfusion, which is linked to lower pregnancy rates and higher risk of complications.
Key indicators that your uterine blood flow may need a boost:
- History of failed embryo implantation or pregnancy loss
- Diagnosed conditions like hypertension or endometriosis
- Abnormal findings on Doppler ultrasound.
- Heavy or prolonged menstrual bleeding: If your periods last longer than 7 days or you need to change your pad or tampon more frequently than every 2 hours, it could be a sign of excessive blood loss.
- Passing clots the size of a quarter or larger, or passing them frequently, can indicate heavy bleeding and potential blood flow issues.
- Spotting or bleeding between periods. This could suggest a problem with the uterine lining or blood flow. Severe cramping or persistent pelvic pain, especially during your period, can be associated with poor uterine circulation.
- An ultrasound can be used to assess the thickness of your uterine lining. A thin lining (less than 8mm) can indicate poor blood flow.
As Dr. Basky Thilaganathan, Professor of Fetal Medicine, explains: “Maternal uterine artery blood flow is critical to maintaining the intrauterine environment, permitting normal placental function, and supporting fetal growth”. If you have concerns, talk with your provider about testing and ways to support your uterine health. Key Hormones provides useful insights.
Which everyday moves instantly wake up pelvic circulation?
You can instantly boost your pelvic circulation with simple, everyday moves. Research shows that squatting exercises like wall squats, sumo squats, and deep squats significantly improve blood flow to your pelvic area and uterus. These moves also help reduce pelvic congestion and menstrual discomfort when practiced regularly. Pelvic floor muscle training, such as Kegel exercises, also increases blood flow to vulvovaginal tissues and improves muscle strength and relaxation.
Try these moves to wake up your pelvic circulation:
- Bodyweight or sumo squats: Deep or sumo squats are especially effective for boosting pelvic blood flow and reducing congestion.
- Wall squats: Lean against a wall and slide down into a squat position to activate your pelvic muscles.
- Pelvic floor contractions (Kegels): Squeeze and release your pelvic floor muscles to improve circulation and muscle tone 2.
- Bridge pose: Lie on your back, bend your knees, and lift your hips to engage your pelvic and gluteal muscles.
- Gentle yoga stretches: Poses like child’s pose or happy baby can help relax and stimulate pelvic circulation 1.
- Modified lumbo-pelvic exercises: Incorporate dance or abdominal drawing-in maneuvers for added benefit.
- Hypopressive breathing exercises: These postural and breathing techniques activate deep pelvic and abdominal muscles.
As Dr. Marwa Abd El-Rahman Mohamed, physical therapy researcher, explains: “Adding squatting exercises to yoga is more effective than yoga alone in reducing menstrual pain and distress, because of decreased pelvic congestion”. Even a few minutes of these movements each day can support your pelvic health and fertility. If you have health concerns, consult your provider before starting new exercises. Uterine Contractions: Good vs. Bad will help you walk through this journey.

Which yoga poses and pelvic stretches target uterine arteries?
Certain yoga poses and pelvic stretches can help target the uterine arteries by improving blood flow to your pelvic region and supporting uterine health. Research highlights that yoga practices focusing on the pelvic area such as bound angle pose (Baddha Konasana), bridge pose (Setu Bandhasana), child’s pose (Balasana), and deep squats (Malasana) are effective for increasing circulation and reducing pelvic congestion. These poses gently stretch and activate your pelvic floor, hips, and lower abdomen, which can help enhance blood flow to the uterus and its arteries.
Several yoga poses and pelvic stretches can help target your uterine arteries by increasing blood flow to your pelvic region and supporting uterine health. Here’s how to do some of the most effective moves:
- Bound Angle Pose (Baddha Konasana): Sit with your back straight. Bring the soles of your feet together and let your knees fall outward. Hold your feet and gently press your knees toward the floor. This pose opens your hips and stimulates pelvic circulation.
- Bridge Pose (Setu Bandhasana): Lie on your back with knees bent and feet flat on the floor, hip-width apart. Press your feet into the floor and lift your hips toward the ceiling. Hold for a few breaths, then lower down. This pose activates your pelvic and lower abdominal muscles.
- Child’s Pose (Balasana): Kneel on the floor, sit back on your heels, and fold forward, stretching your arms in front of you. Rest your forehead on the mat. This gentle stretch relaxes your lower back and pelvis.
- Deep Squat (Malasana): Stand with feet slightly wider than hip-width. Squat down as low as comfortable, keeping your heels on the floor and your chest lifted. Bring your palms together at your chest and press your elbows into your knees. This pose increases blood flow to your pelvic organs.
- Cat-Cow Stretch (Marjaryasana-Bitilasana): Start on your hands and knees. Inhale, arch your back (cow), and exhale, round your spine (cat). Repeat several times to mobilize your pelvis and lower back.
Practicing these poses for 20–30 minutes, two to three times per week, can support your pelvic and uterine health. As summarized in a 2022 review, “Yoga asanas that activate the pelvic regions have a positive effect on reproductive organ blood flow and can be a valuable adjunct to fertility care”. Always consult your healthcare provider before starting a new exercise routine, especially if you have health concerns.
Can nutrition and hydration really open uterine arteries?
Nutrition plays a key role in supporting healthy uterine arteries and overall reproductive health. A diverse, balanced diet; especially one rich in plant-based foods can lower your risk of abnormal uterine bleeding and support optimal vascular function. In a recent study, each 1-point increase in dietary diversity score was linked to a 22% lower risk of abnormal uterine bleeding. However, severe nutrient restriction in pregnancy did not significantly reduce total uterine artery blood flow in animal studies, but it did result in smaller placentas and lower birth weights, showing that poor nutrition can still compromise reproductive outcomes even if blood flow is preserved. Diets high in fat and processed foods may reduce uterine blood flow and increase inflammation, further impacting uterine health. As Dr. Sha Yu, PhD, Nutrition & Metabolism, states: “Higher dietary diversity and moderate adherence to a ‘low fat plant-based’ dietary pattern may be significant protective factors against abnormal uterine bleeding”.
Hydration is essential for maintaining healthy blood volume and circulation, which indirectly supports uterine artery function. While direct evidence linking hydration to increased uterine artery blood flow is limited, staying well-hydrated helps your cardiovascular system deliver nutrients and oxygen efficiently throughout your body, including your reproductive organs. Dehydration can reduce blood volume and may impair circulation, potentially affecting uterine health. For best results, drink water regularly throughout the day and adjust your intake based on activity level, climate, and individual needs. If you have specific concerns about your hydration or uterine blood flow, consult your healthcare provider for personalized advice.
Strong Egg Mitochondria offer more support.
Do supplements like L-arginine and vitamin E work—and are they safe?
Supplements like L-arginine and vitamin E may help improve uterine blood flow, especially in people with fertility challenges related to thin endometrium or luteal phase defects. In a clinical study, vitamin E (600 mg/day) improved uterine artery blood flow in 72% of participants and endometrial thickness in 52%. L-arginine (6 g/day) showed even greater improvement, with 89% experiencing better blood flow and 67% showing increased endometrial thickness. Both supplements also improved luteal blood flow and hormone levels in people with luteal phase defects. A recent systematic review found that L-arginine supplementation is generally safe in pregnancy and can reduce the risk of preeclampsia, lower blood pressure, and improve fetal growth in certain high-risk groups.
Vitamin E and L-arginine are well-tolerated in most cases, but you should consult your healthcare provider before starting any supplement, especially if you are pregnant or have underlying health conditions. As Dr. D. Menichini, MD, notes: “L-Arginine administration is safe and could be a candidate as an intervention beneficial to maternal and fetal outcomes, at least in moderate clinical disorders”. Always use supplements under medical supervision to ensure safety and effectiveness.
How do warmth, massage, and acupuncture complement movement?
Warmth, massage, and acupuncture can work together with movement to support your fertility and overall well-being. Each therapy offers unique benefits:
- Warmth (such as warm acupuncture) relaxes muscles, increases blood flow, and prepares your body for movement. This can ease discomfort and help tissues recover more quickly.
- Massage boosts circulation, relieves muscle tension, and improves joint mobility. When combined with warmth, massage can make movement more comfortable and effective.
- Acupuncture, especially when paired with heat, has been shown to reduce pain and improve function in people with chronic pelvic pain and joint stiffness. It can also enhance your quality of life and support tissue healing.
When you combine these therapies with regular movement, you may see greater improvements in pain relief, mobility, and daily function. In a recent clinical study, people who received both warm acupuncture and rehabilitation training had better walking ability and balance than those who did rehabilitation alone. As Dr. Miaoran Zhou, PhD, explains: “The immediate thermal effect of warm acupuncture therapy was associated with patient improvement, and its medical thermal effect significantly promoted pain relief and tissue recovery” 3. Always consult your healthcare provider to ensure these therapies are safe and right for you.
Curious about immune factors? Immunity and Fertility got you covered.
When lifestyle fixes aren’t enough, what medical options exist?
When lifestyle changes are not enough, several medical options can help you build your family. For many, the first step is ovarian stimulation with oral medications such as clomiphene citrate or letrozole often combined with intrauterine insemination (IUI). This approach, called ovarian stimulation with IUI (OS-IUI), is typically tried for three or four cycles. If this does not result in pregnancy, in vitro fertilization (IVF) is the next recommended step. IVF may be considered sooner if you are over 38 to 40 years old, have severe male factor infertility, or have blocked fallopian tubes.
Other options include injectable gonadotropins, which can be used alone or with IUI, but these carry a higher risk of multiple pregnancies and ovarian hyperstimulation syndrome. For male infertility, treatments may include hormonal therapies, antioxidant supplements, or assisted reproductive technologies like intracytoplasmic sperm injection (ICSI). According to the American Society for Reproductive Medicine, “the best initial therapy for most couples is a course (typically 3 or 4 cycles) of ovarian stimulation with oral medications and intrauterine insemination (OS-IUI) followed by in vitro fertilization for those unsuccessful with OS-IUI treatments”. Your care team will help you choose the safest and most effective path based on your unique needs.
How should you track progress and stay consistent?
To track your progress and stay consistent during fertility treatment, use a combination of self-monitoring tools and regular feedback. To track your progress and stay consistent during fertility treatment, use these practical steps:
- Monitor your menstrual cycle: Record period dates, ovulation signs (like basal body temperature and cervical mucus), and any symptoms or medications.
- Use a reliable app: Choose one that tracks multiple fertility signs not just calendar dates for more accurate insights.
- Set daily reminders:** Use phone alerts or a calendar to prompt medication, tracking, or appointments.
- Share your records: Bring your tracking data to each healthcare visit to guide decisions and adjust your plan.
- Review your progress: Regularly look for patterns or changes in your data.
- Enlist support: Ask your partner or a trusted friend to help you stay on track.
- Seek feedback: Request regular updates from your care team to stay motivated and make timely adjustments.
- Prioritize self-care: Acknowledge the emotional burden; take breaks and seek support if tracking feels overwhelming.
Consistency is key: set daily reminders and review your data regularly to spot patterns or changes. Share your records with your healthcare team at each visit to guide decisions and adjust your plan as needed.
Staying consistent can feel overwhelming, so consider enlisting your partner or support network to help you stay on track. According to a 2023 randomized controlled trial, using a fertility-tracking app did not significantly increase pregnancy rates overall, but those who used the app consistently saw slightly better outcomes, especially if they had been trying to conceive for several months. Dr. Lauren A. Wise, ScD, Professor of Epidemiology, notes: “Adherence to tracking tools may offer modest benefits for certain groups, but the emotional burden and complexity of self-tracking should not be underestimated”. If you feel stressed or discouraged, talk to your care team. They can help you adjust your approach and provide emotional support.
If your luteal phase runs short, pair tracking with Short Luteal Phase: Causes and Fixes.
Addressing special cases: PCOS, fibroids, and endometriosis—do the rules change?
If you have polycystic ovary syndrome (PCOS), fibroids, or endometriosis, the approach to fertility treatment often changes to address your unique needs. Here’s how the rules adapt:
- PCOS: You may need longer or more intensive ovulation induction, and you might respond differently to medications. PCOS can lower the chance of a quick response to fertility-sparing treatments and increase the risk of recurrence after treatment for related conditions like endometrial hyperplasia or cancer.
- Fibroids: Not all fibroids affect fertility, but those that distort the uterine cavity or are large may need removal (myomectomy). Myomectomy can improve pregnancy rates up to 68% in some studies but carries surgical risks. Uterine artery embolization is not recommended if you wish to conceive, due to higher miscarriage and placental risks.
- Endometriosis: Treatment depends on severity. Mild cases may benefit from intrauterine insemination (IUI), while moderate to severe cases often require in vitro fertilization (IVF). Surgery can help with pain and may improve fertility, but its benefit for pregnancy rates is modest and should be weighed carefully.
- Combined conditions: If you have more than one of these conditions, your chances of pregnancy may be lower, and treatment may be more complex. For example, ongoing pregnancy rates are highest in PCOS alone (38.8%), lower with both PCOS and endometriosis (28%), and lowest with endometriosis alone (16.3%).
Dr. Samra Saleem Azam, MD, notes: “Individualized treatment plans, combining medical, surgical, and lifestyle approaches, are essential to improve fertility outcomes and quality of life for those with PCOS, fibroids, or endometriosis” 1. Always work closely with your care team to tailor your plan to your specific diagnosis and goals.
Keep an eye on cervical integrity too via Cervical Length Check.
Your top uterine blood flow questions answered
Can I keep these moves after embryo transfer?
Yes, gentle movement like walking or light stretching can be continued after embryo transfer. There is no evidence that moderate activity harms implantation or uterine blood flow. However, avoid high-impact exercise or anything that causes discomfort. Always follow your clinic’s specific advice.
Which sign shows improvement fastest?
The fastest sign of improved uterine blood flow is often seen in endometrial perfusion, which can be measured by Doppler ultrasound. Studies show that women with better sub-endometrial blood flow have higher pregnancy and live birth rates, especially in those with thin endometrium. Improved blood flow may be detected within days after interventions or lifestyle changes.
Do men need circulation fixes?
Yes, healthy blood flow is important for sperm quality. Poor circulation can affect sperm morphology (shape), motility, and count. Addressing circulation through exercise, managing blood pressure, and avoiding smoking can support male fertility. See Sperm Morphology Basics.
Is caffeine a hard no?
Moderate caffeine intake (up to 200 mg per day, about one 12-ounce coffee) is generally considered safe during fertility treatment. High caffeine intake may be linked to lower pregnancy rates, but evidence is mixed. Discuss your caffeine habits with your provider to personalize your plan.
How do I know if my blood flow is optimal?
Doppler ultrasound can assess uterine and endometrial blood flow. A pulsatility index (PI) above 2.8 or absent endometrial flow is linked to lower pregnancy rates.
What can I do to improve blood flow?
Stay hydrated, manage stress, avoid smoking, and consider gentle movement. Some medications, like oxytocin antagonists, are being studied for their potential to improve endometrial perfusion.
When should I contact my provider?
If you experience pain, heavy bleeding, or unusual symptoms after transfer, contact your clinic promptly.
Final Thoughts
Optimal uterine blood flow is a crucial factor for successful fertility treatment, especially in procedures like IVF. Studies using Doppler ultrasound show that women with both endometrial and subendometrial blood flow have significantly higher pregnancy and implantation rates compared to those with limited or no detectable flow, indicating that good blood flow reflects a receptive uterine environment. Interventions such as low-dose aspirin, vaginal sildenafil, acupuncture, and certain traditional medicines have been shown to improve uterine artery blood flow, endometrial thickness, and, in some cases, pregnancy rates, though results can vary and more research is needed for some therapies.
Poor uterine perfusion is linked to lower implantation and pregnancy rates, but targeted treatments to enhance blood flow like hormone therapy or vasodilators may help some patients, particularly those with a history of failed IVF cycles. In women with uterine fibroids, altered blood flow patterns can negatively affect implantation, and the choice of fibroid treatment (such as myomectomy or HIFU) can impact both blood flow and fertility outcomes.
Overall, assessing and, when needed, improving uterine blood flow is an important part of maximizing the chances of a successful pregnancy during fertility treatment.
Download the “Pelvic Flow Challenge,” Healthy Uterine Lining, and step into each cycle feeling informed, proactive, and empowered.
References
-
Reproductive Endocrine Disorders: A Comprehensive Guide to the Diagnosis and Management of Infertility, Polycystic Ovary Syndrome, and Endometriosis. Cureus. 2025; 17. https://doi.org/10.7759/cureus.78222.
-
A randomized trial of web-based fertility-tracking software and fecundability… Fertility and sterility. 2023 https://doi.org/10.1016/j.fertnstert.2023.02.005.
-
Evidence-based treatments for couples with unexplained infertility: a guideline… Fertility and sterility. 2020; 113 2. https://doi.org/10.1016/j.fertnstert.2019.10.014.
-
Medical thermal effects and CT radiation image examination in the treatment of sequelae of chronic pelvic inflammatory disease with warm acupuncture therapy: A meta-analysis. Thermal Science and Engineering Progress. 2025 https://doi.org/10.1016/j.tsep.2024.103149.
-
The association between dietary diversity and patterns in Chinese university students with abnormal uterine bleeding: a cross-sectional study. Nutrition & Metabolism. 2024; 21. https://doi.org/10.1186/s12986-024-00873-1.
-
L-Arginine supplementation in pregnancy: a systematic review of maternal and fetal outcomes. The Journal of Maternal-Fetal & Neonatal Medicine. 2023; 36. https://doi.org/10.1080/14767058.2023.2217465.
-
The Effects of Yoga on Pregnancy, Stress, and Anxiety in Infertile Individuals. Holistic Nursing Practice. 2022; 36. https://doi.org/10.1097/HNP.0000000000000543.
-
Effect of different squatting exercises on menstrual aspects, pelvic mechanics and uterine circulation in primary dysmenorrhoea: a randomised controlled trial. Journal of Obstetrics and Gynaecology. 2022; 42. https://doi.org/10.1080/01443615.2022.2153021.
-
Preeclampsia: The Relationship between Uterine Artery Blood Flow and Trophoblast Function. International Journal of Molecular Sciences. 2019; 20. https://doi.org/10.3390/ijms20133263.
-
Uterine Vascular Control Preconception and During Pregnancy… Comprehensive Physiology. 2021; 11 3. https://doi.org/10.1002/cphy.c190015.
-
Importance of blood flow to human implantation. Human Reproduction. 2021 https://doi.org/10.1093/humrep/deab126.030.