You may feel anxious or uncertain about having your cervical length checked. This concern is valid. Cervical length measurement is a key part of monitoring pregnancy health, especially when it comes to preventing preterm birth—a leading cause of complications for newborns in the United States. Knowing your cervical length helps your care team identify if you are at higher risk, so they can offer timely support and interventions tailored to your needs.
A cervical length check is a simple, safe procedure, usually done with a transvaginal ultrasound. It gives clear, reliable information about your risk for early labor, whether you have symptoms or not. If your cervix is shorter than expected, your provider can discuss options like closer monitoring, medication, or other preventive steps to help protect your pregnancy. Taking this step empowers you and your care team to make informed decisions for your health and your baby’s well-being.
- What exactly is cervical length, and why should future parents care?
- How and when is cervical length measured for best accuracy?
- What cervical length numbers are considered normal, short, or critical?
- How solid is the evidence that a short cervix leads to preterm birth?
- Who benefits most from serial cervical length checks?
- Which proven interventions protect pregnancies with a short cervix?
- Can everyday choices help keep your cervix strong?
- What fears or myths still surround cervical length scans?
- Where does cervical length monitoring fit in your bigger fertility plan?
- Your top questions, answered
- Final thoughts: Measuring millimeters today can mean months of safety tomorrow
- References
What exactly is cervical length, and why should future parents care?
Cervical length is the measurement of the lower part of your uterus, known as the cervix, typically assessed by a painless transvaginal ultrasound during pregnancy. This measurement matters because a shorter cervix increases the risk of preterm birth, which can lead to serious health challenges for newborns. For future parents, knowing your cervical length helps your healthcare team identify if you or your partner are at higher risk, allowing for early interventions that can improve pregnancy outcomes and reduce complications.
A short cervical length; often defined as 25-30 mm or less, depending on your specific situation signals a higher chance of delivering early, even if you have no symptoms. This information is especially important for those with a history of preterm birth, multiple pregnancies, or certain pregnancy complications. By monitoring cervical length, you and your provider can make informed decisions about preventive treatments, such as progesterone therapy or closer monitoring, to help protect your pregnancy and your baby’s health.
If you’ve ever wondered how cervical mucus steers sperm, Cervical Mucus & Sperm is of importance to you.
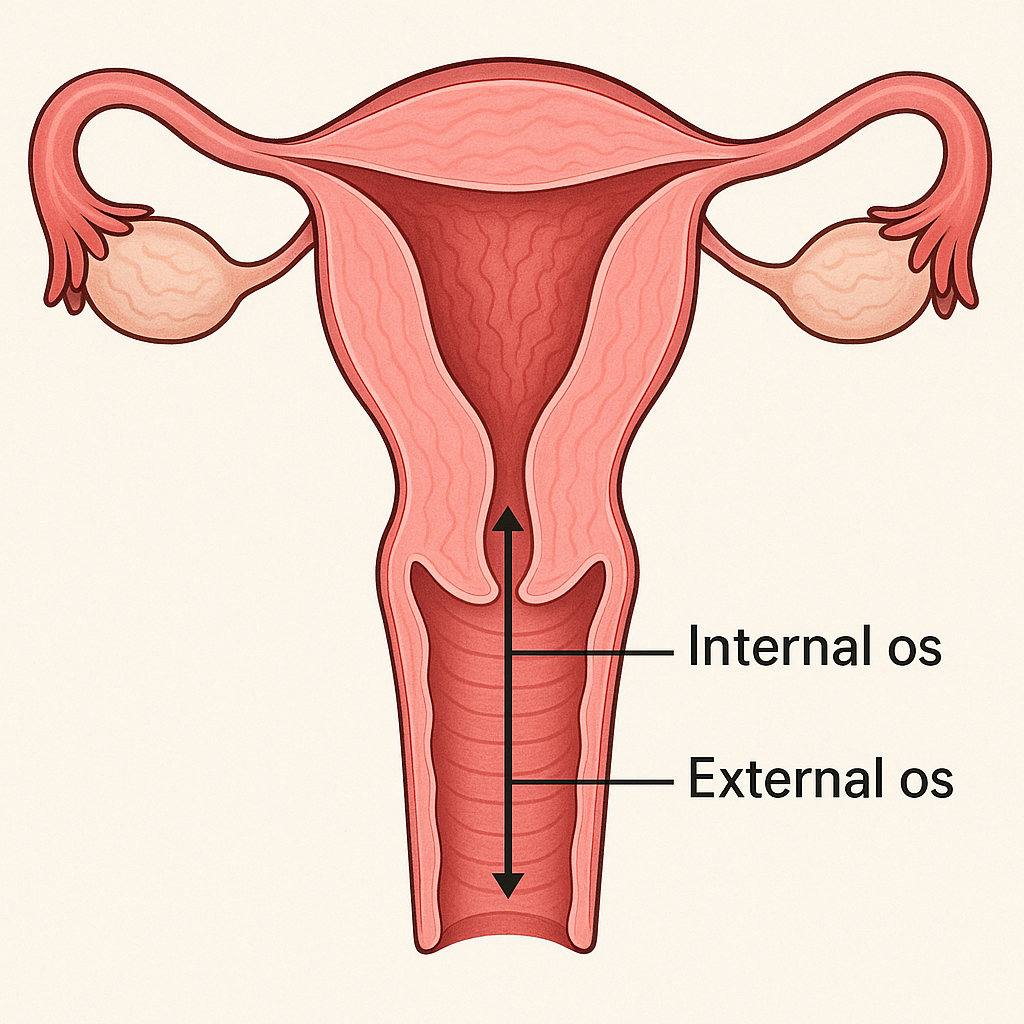
How and when is cervical length measured for best accuracy?
Cervical length is most accurately measured using transvaginal ultrasound, which provides a clear and reliable view of the cervix and minimizes variability between different examiners. This method is significantly more precise than digital (manual) examination, which tends to underestimate cervical length and is less consistent. For best accuracy, the measurement should be performed between 18 and 24 weeks of pregnancy, as this window offers the strongest ability to predict the risk of preterm birth in both single and twin pregnancies. A single measurement during this period is generally more predictive than tracking changes in cervical length over time.
The procedure is quick, safe, and does not harm you or your baby. Consistency in technique and timing is important, and both straight-line and two-line measurement methods show excellent reliability across all trimesters. Automated, deep learning-based tools are emerging and may further improve accuracy and reduce differences between providers, but expert-performed transvaginal ultrasound remains the gold standard for now.
What cervical length numbers are considered normal, short, or critical?
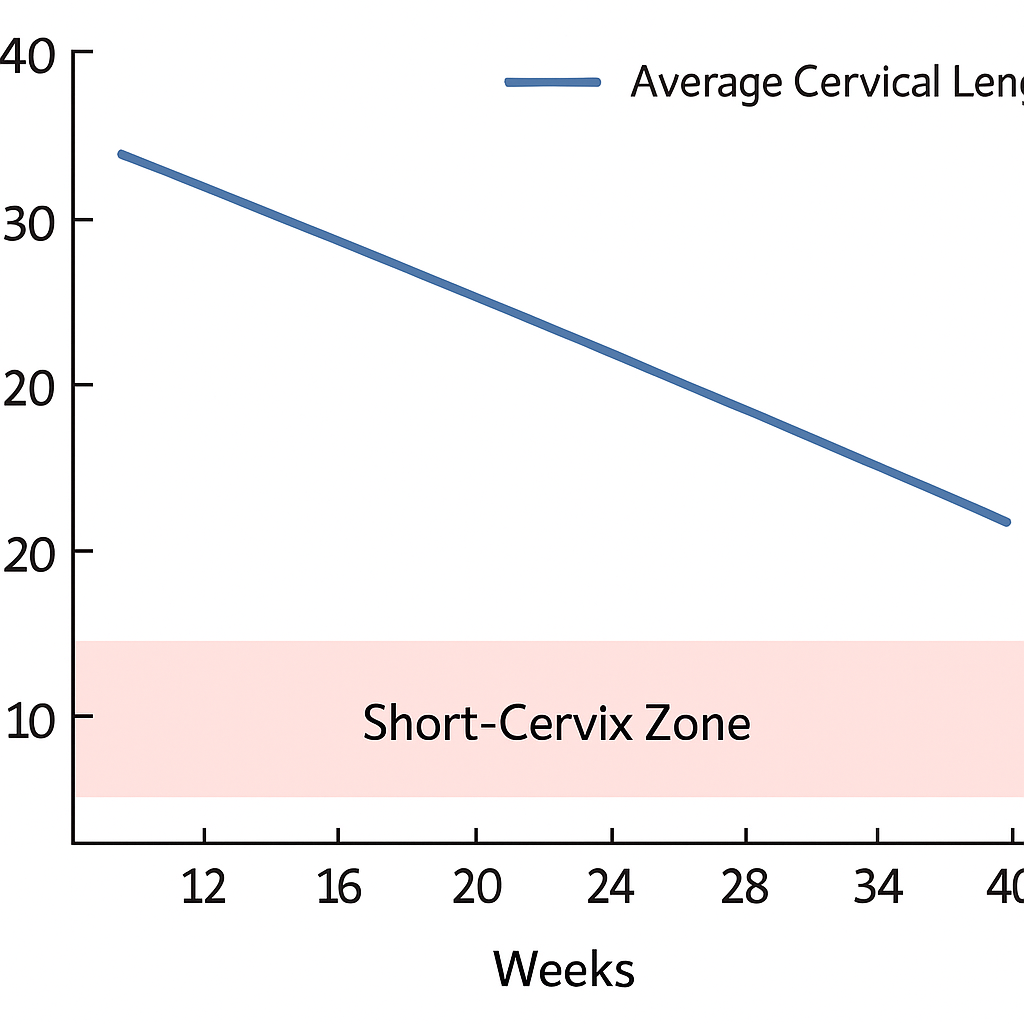
A normal cervical length during mid-pregnancy (around 16–24 weeks) is typically between 35 and 40 mm (3.5–4.0 cm), with average values reported near 36–38 mm.
A cervical length of 30 mm (3.0 cm) or more is generally considered reassuring and low risk for preterm birth.
When the cervical length measures between 25 and 30 mm, it is often viewed as borderline or “shortening,” and may warrant closer monitoring, especially if you have other risk factors.
A cervical length of 25 mm (2.5 cm) or less is widely recognized as “short” and signals a higher risk for preterm birth, prompting consideration of preventive treatments or more frequent checks.
Measurements of 15 mm (1.5 cm) or less are considered “critically short” and are associated with the highest risk for early delivery and related complications.
These cutoffs may vary slightly depending on your individual health, pregnancy history, and population background, so your provider will interpret your results in context.
Special note for IVF conceptions: a cutoff of ≤30 mm already signals elevated risk.
How solid is the evidence that a short cervix leads to preterm birth?
Extensive, high-quality research confirms that a short cervix usually defined as 25 mm or less on mid-trimester ultrasound is a strong, independent predictor of spontaneous preterm birth. Large cohort studies and meta-analyses show that as cervical length decreases, the risk of delivering early rises sharply, with the highest risk seen in those with a cervix of 10 mm or less. This association holds true even in people without symptoms or a prior history of preterm birth, and across different populations. For example, one major study found that women with a cervical length ≤10 mm at 23–28 weeks had the shortest time to delivery and the highest rates of preterm birth before 32 and 34 weeks.
The predictive value of a short cervix is so robust that it is now considered the gold standard for identifying those at risk for preterm birth. Interventions based on this measurement, such as vaginal progesterone, have been shown in multiple randomized controlled trials and meta-analyses to significantly reduce the risk of preterm birth and improve newborn outcomes, including lowering rates of respiratory distress syndrome, NICU admission, and neonatal death.
Universal cervical length screening and targeted treatment are cost-effective and could prevent tens of thousands of preterm births and serious complications each year in the United States 2. While the risk is highest with the shortest cervical lengths, even moderate shortening (16–25 mm) increases risk, and personalized assessment can further refine predictions. In summary, the link between a short cervix and preterm birth is supported by strong, consistent evidence, making cervical length a critical factor in pregnancy care and prevention strategies.
Who benefits most from serial cervical length checks?
Serial cervical length checks are most beneficial for people at higher risk of preterm birth, including those with multiple pregnancies (twins or triplets), a history of preterm birth, prior cervical surgery (like conization), or borderline cervical length measurements in mid-pregnancy.
In women with twin or triplet pregnancies, serial measurements significantly improve the ability to detect those at risk for early delivery compared to a single check, as cervical shortening can develop later in pregnancy and may be missed otherwise.
For low-risk women with singleton pregnancies and a borderline cervical length (26–29 mm), follow-up scans can identify the 15% who will go on to develop a short cervix (≤25 mm), who then face a much higher risk of preterm birth.
Women with a history of preterm birth or cervical surgery also benefit, as serial scans can catch late cervical shortening and allow for timely interventions like progesterone or cerclage. In high-risk clinics, serial checks combined with preventive treatments have been shown to reduce preterm birth rates and improve outcomes.
However, for women with consistently normal cervical length and no risk factors, the added value of repeated scans is limited and may not justify the extra cost or effort.
Overall, serial cervical length monitoring is most valuable for those with known risk factors or early signs of cervical shortening, helping guide targeted prevention strategies and improve pregnancy outcomes.
Which proven interventions protect pregnancies with a short cervix?
For pregnancies with a short cervix (≤25 mm), several interventions have proven effective in reducing the risk of preterm birth and improving neonatal outcomes.
The most robust evidence supports the use of vaginal progesterone. It significantly lowers the risk of preterm birth, respiratory distress syndrome, neonatal intensive care admission, and neonatal death in women with singleton pregnancies, regardless of prior preterm birth history.
Cervical cerclage, a surgical stitch placed around the cervix. It is also effective especially for women with a history of preterm birth or those whose cervix continues to shorten despite progesterone therapy. It can further reduce preterm birth rates and improve outcomes when the cervix is extremely short (<10 mm).
Cervical pessaries, which are silicone devices placed around the cervix, have shown similar effectiveness to progesterone and cerclage in some studies, though their benefit is less consistently supported and may depend on individual risk factors.
Recent large randomized trials indicate that all three interventions; vaginal progesterone, cerclage, and pessary are similarly effective for women with a short cervix. It thus, allows clinicians to tailor treatment based on patient preference, side effect profiles, and specific clinical scenarios.
Universal cervical length screening combined with targeted use of these interventions is cost-effective and could prevent thousands of preterm births annually. In summary, vaginal progesterone, cervical cerclage, and pessary are all proven options for protecting pregnancies with a short cervix, with the choice guided by individual risk factors and clinical judgment.
Gentle moves that boost pelvic blood flow can help overall pregnancy health—see Boost Uterine Blood Flow.
Can everyday choices help keep your cervix strong?
Everyday choices can play a role in supporting cervical health during pregnancy, though their impact is more indirect compared to medical interventions.
Avoiding alcohol is important, as alcohol consumption during pregnancy has been linked to a higher risk of HPV infection, which can compromise cervical health.
Smoking is another key risk factor; it increases the risk of cervical problems, including cervical ectopic pregnancy, especially in women with a history of multiple pregnancies or miscarriages.
Maintaining a healthy weight, engaging in regular physical activity, and managing stress may also help. Animal studies suggest that a stimulating, low-stress environment can reduce inflammation and prevent premature cervical changes that lead to preterm birth.
Additionally, staying up to date with cervical cancer screening and following preconception care guidelines such as taking recommended supplements and seeking medical advice before pregnancy can further support reproductive and cervical health.
While these lifestyle choices cannot guarantee a strong cervix, they contribute to overall pregnancy health and may help reduce risks associated with cervical weakness or infection.
What fears or myths still surround cervical length scans?
Despite strong evidence supporting cervical length scans, several fears and myths persist. Some people worry that transvaginal ultrasound is painful, invasive, or could harm the pregnancy, though research shows it is safe and well-tolerated when performed by trained professionals.
There is also a misconception that cervical length scans are unnecessary unless symptoms are present, but studies confirm their value in predicting and preventing preterm birth even in asymptomatic women.
Cultural beliefs, mistrust of medical interventions, and lack of understanding about the purpose of the scan can lead some groups such as younger women, African Americans, smokers, and those with higher body weight to decline screening, even though these groups may be at higher risk for preterm birth.
Another myth is that a normal cervical length guarantees a full-term pregnancy, when in reality, it only reduces and not eliminates the risk.
Some also fear that a short cervix diagnosis will automatically lead to unnecessary interventions, but evidence-based guidelines recommend treatment only for those at significant risk.
Overall, education and clear communication from healthcare providers are key to dispelling these myths and encouraging acceptance of cervical length screening as a safe, effective tool for protecting pregnancy health.
Where does cervical length monitoring fit in your bigger fertility plan?
Cervical length monitoring plays a crucial role in a comprehensive fertility and pregnancy plan, especially for those aiming to optimize outcomes and reduce risks. While it is not a tool for tracking ovulation or timing conception unlike fertility awareness methods that focus on cycle length, basal body temperature, and cervical fluid; cervical length assessment becomes highly relevant once pregnancy is established.
Measuring cervical length by transvaginal ultrasound during mid-pregnancy helps identify individuals at increased risk for preterm birth, allowing for early intervention with proven therapies such as progesterone or cerclage. This is particularly important for women with a history of preterm birth, cervical surgery, or other risk factors, as well as those with multiple pregnancies.
Personalized cervical length assessment, which takes into account maternal characteristics and gestational age, can further refine risk prediction and guide tailored care. Routine cervical length screening is recommended for high-risk pregnancies, and universal screening may be considered in some settings to maximize prevention of preterm birth.
Additionally, cervical length measurement can help anticipate both early and prolonged pregnancies, informing decisions and reducing anxiety about timing of delivery.
In summary, while cervical length monitoring is not part of preconception fertility tracking, it is a vital component of prenatal care that fits into a larger fertility plan by safeguarding pregnancy health and supporting the goal of a healthy, full-term birth.
Your top questions, answered
Does a long cervix make it harder to conceive?
No, having a long cervix does not make it harder to conceive. Cervical length is not linked to fertility or the ability to get pregnant; instead, it becomes important during pregnancy as a predictor of preterm birth risk. Fertility is more influenced by factors like ovulation, egg and sperm health, and reproductive anatomy, not cervical length.
Can my cervix grow longer again during pregnancy?
Once the cervix shortens during pregnancy, it typically does not lengthen again. Cervical shortening is usually a gradual, one-way process as the body prepares for birth, and while treatments like progesterone can slow or stabilize further shortening, they do not restore lost length.
Is universal screening worth it if I have no risk factors?
Universal cervical length screening in mid-pregnancy can be valuable even for those without risk factors, as most preterm births occur in people with no prior history. Relying only on risk factors misses many at-risk pregnancies, and universal screening helps identify those who could benefit from preventive treatment, making it a more effective strategy overall.
What’s the fastest help if my cervix measures under 15 mm?
If your cervix measures under 15 mm before 24 weeks and you have no symptoms, the fastest and most effective intervention is starting vaginal progesterone, which reduces the risk of preterm birth. If you have a history of preterm birth or additional risk factors, your doctor may also discuss a cervical cerclage (a stitch to reinforce the cervix). Immediate hospitalization or emergency interventions are usually not needed unless you have symptoms like contractions or bleeding, but close monitoring and prompt treatment are essential.
Final thoughts: Measuring millimeters today can mean months of safety tomorrow
Measuring cervical length during pregnancy is a small step that can have a big impact on the safety and health of both mother and baby. Cervical length monitoring, especially by transvaginal ultrasound, is a proven way to identify women at increased risk for preterm birth. This is even before symptoms appear; allowing for timely preventive interventions that can add weeks or even months to a pregnancy. The approach is particularly valuable for women with a history of preterm birth. However, universal screening can also catch unexpected cases in low-risk pregnancies, since most preterm births occur in women without known risk factors. Serial measurements, especially in high-risk groups like twin pregnancies, further improve the ability to predict and prevent early delivery. This gives families more time to prepare and babies more time to develop.
Cervical length assessment is safe, noninvasive, and, when combined with other maternal factors, offers a powerful tool for personalized pregnancy care. By acting on these millimeter-level changes today, healthcare providers can help ensure more pregnancies reach full term, reducing the risk of complications and long-term health issues for newborns. In short, a simple measurement now can mean months of safety and peace of mind tomorrow.
References
-
Vaginal progesterone to prevent preterm birth in pregnant women with a sonographic short cervix: clinical and public health implications… American journal of obstetrics and gynecology, 214 2, 235-242 . https://doi.org/10.1016/j.ajog.2015.09.102.
-
Personalized assessment of cervical length improves prediction of spontaneous preterm birth: a standard and a percentile calculator… American journal of obstetrics and gynecology. https://doi.org/10.1016/j.ajog.2020.09.002.
-
The risk of spontaneous preterm birth in asymptomatic women with a short cervix (≤25 mm) at 23-28 weeks’ gestation… American journal of obstetrics & gynecology MFM, 2 2, 100059 . https://doi.org/10.1016/j.ajogmf.2019.100059.
-
Serial Cervical Length Screening to Prevent Preterm Birth Among U.S. Women with a Singleton Gestation and a History of Preterm Birth: A Decision Analysis. SSRN Electronic Journal. https://doi.org/10.2139/ssrn.4525630.
-
Utility of Follow up Cervical Length Screening in Low Risk Women with Cervical Length 26-29mm… American journal of obstetrics and gynecology. https://doi.org/10.1016/j.ajog.2021.02.027.
-
Comparing cervical cerclage, pessary and vaginal progesterone for prevention of preterm birth in women with a short cervix (SuPPoRT): A multicentre randomised controlled trial. PLOS Medicine, 21. https://doi.org/10.1371/journal.pmed.1004427.
-
The enrichment of maternal environment prevents pre-term birth in a mice model… Reproduction. https://doi.org/10.1530/REP-19-0572.