Did you know your dominant follicle can swell from 6 mm to 22 mm in just 10 days—doubling your odds of conception?
Many people navigating fertility journeys want clear, reliable information about how follicles develop and what to expect. Follicle growth is a dynamic, carefully regulated process that underpins your reproductive health and chances of conception. Understanding this process can help you make informed decisions and feel more in control.
Follicles grow in distinct stages, with rapid changes occurring over just a few weeks. Research shows that early follicle development involves key milestones, such as cell proliferation and the formation of the antrum, typically unfolding over a two- to three-week period in mammals. The most significant growth often happens in the second and third weeks, when follicles expand quickly and prepare for ovulation, though the exact timing can vary from person to person. Knowing these patterns can empower you to interpret your follicle growth charts and advocate for your needs during fertility care.
You deserve compassionate, evidence-based guidance as you navigate this process. By understanding the week-by-week changes in follicle growth, you can better communicate with your healthcare team and take proactive steps toward your fertility goals.
- What exactly is an ovarian follicle and why does its size matter for fertility success?
- How do follicles grow week by week in a natural 28-day menstrual cycle?
- How does a stimulated IVF cycle change the day-by-day follicle chart?
- Which factors can speed up—or stall—follicle growth?
- How can you read your follicular ultrasound like a pro?
- What if your follicles grow too slowly, too quickly, or unevenly?
- Your top questions, answered
- How does follicle growth sync with the rest of your fertility puzzle?
- Final Thoughts
- References
What exactly is an ovarian follicle and why does its size matter for fertility success?
An ovarian follicle is a small, fluid-filled sac in your ovary that contains an immature egg (oocyte). Each month, several follicles begin to grow, but usually only one becomes dominant and reaches full maturity, releasing its egg during ovulation. The size of your follicles is a key indicator of their readiness: follicles typically need to reach about 15–18 mm in diameter before the egg inside is mature and most likely to fertilize successfully 167. Follicles smaller than this are less likely to yield mature eggs, while those much larger may not improve outcomes and could even be associated with lower quality eggs or embryos.
Monitoring follicle size helps:
- Follicle size is a strong predictor of whether the egg inside is mature and ready for fertilization; follicles typically need to reach at least 15–16 mm for optimal oocyte maturity and fertilization rates.
- Larger follicles (15–18 mm) are more likely to yield mature eggs, good-quality embryos, and higher pregnancy and live birth rates, while smaller follicles are less likely to produce mature, fertilizable eggs.
- Triggering ovulation or egg retrieval when follicles are too small can result in immature eggs and lower pregnancy rates; conversely, waiting too long can lead to post-mature or degenerated eggs.
- The proportion of follicles within the optimal size range (13–18 mm) on trigger day is directly linked to better outcomes, including more mature eggs and higher live birth rates.
- For individuals with diminished ovarian reserve, mature and competent eggs can still be obtained from slightly smaller follicles (as small as 13 mm), supporting more flexible treatment timing.
- Follicle size helps your care team personalize the timing of interventions, maximizing your chances of conception and successful pregnancy.
For a refresher on the hormones orchestrating this growth, visit Key Hormones: Estrogen, Progesterone, Testosterone.
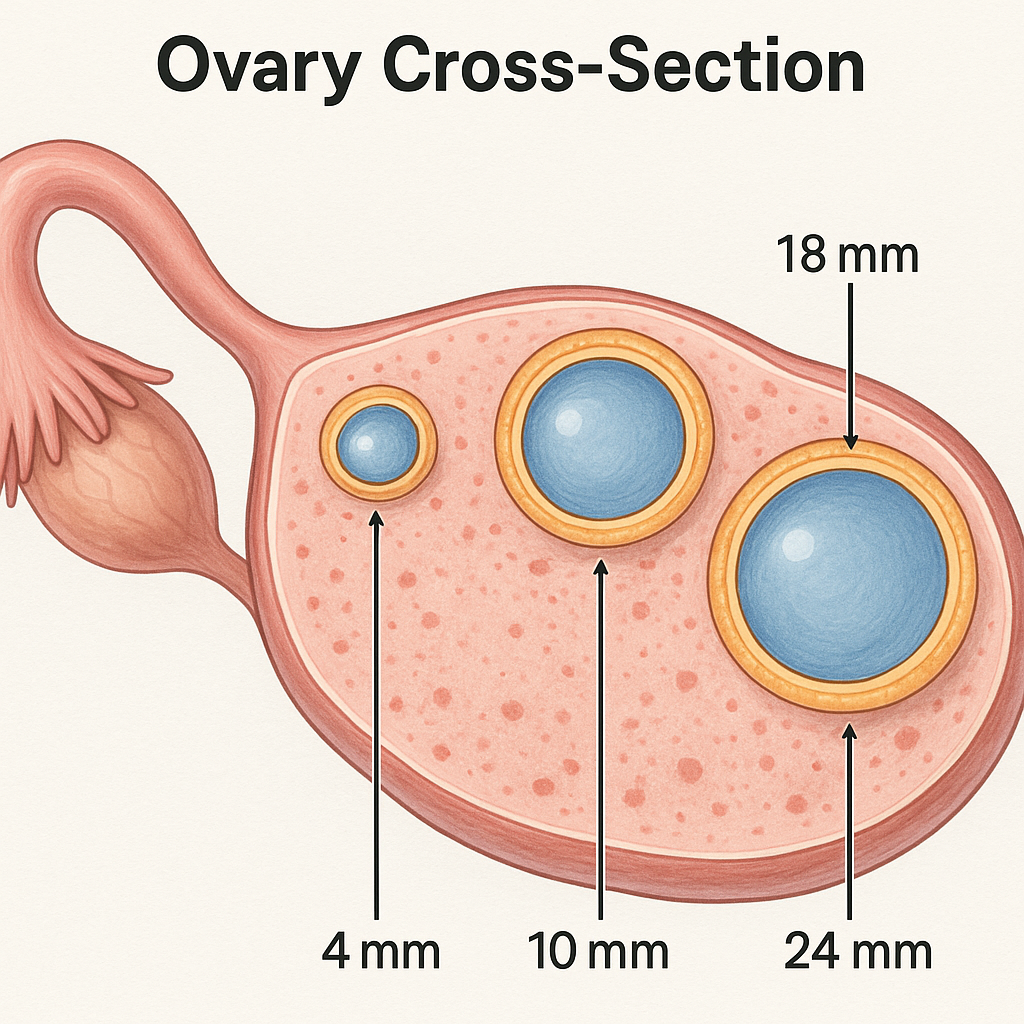
How do follicles grow week by week in a natural 28-day menstrual cycle?
During a natural 28-day menstrual cycle, follicle growth follows a predictable week-by-week pattern.
Week 1 (Days 1–7): Your period starts. Several small follicles (2–5 millimeters) begin to grow in your ovaries, stimulated by follicle-stimulating hormone (FSH). By the end of this week, one follicle becomes dominant, reaching about 9–12 millimeters. The others stop growing. This process sets the stage for ovulation.
Week 2 (Days 8–14): The dominant follicle grows quickly, about 1–2 millimeters per day. By ovulation (around day 14), it usually measures 18–20 millimeters. A surge in luteinizing hormone (LH) triggers the release of the mature egg. Estrogen peaks, thickening your uterine lining for possible pregnancy.
Week 3 (Days 15–21): After ovulation, the follicle transforms into the corpus luteum. This structure produces progesterone, which supports the uterine lining and early pregnancy if fertilization occurs. The corpus luteum reaches its peak size and hormone output about 6–7 days after ovulation.
Week 4 (Days 22–28): If you do not become pregnant, the corpus luteum shrinks. Progesterone and estrogen levels fall. The uterine lining breaks down, leading to your next period and a new cycle.
According to a 2017 study in the Chinese Journal of Laboratory Medicine, the average pre-ovulatory follicle measures about 19.3 millimeters, and both FSH and LH peak just before ovulation. “Understanding your follicle growth can help you and your care team time interventions for the best chance of pregnancy.” — Dr. Meizhi Liu, MD, PhD, reproductive endocrinologist.
Check how your lining keeps pace in Healthy Uterine Lining: Why Thickness Matters.
How does a stimulated IVF cycle change the day-by-day follicle chart?
In a stimulated in vitro fertilization (IVF) cycle, your follicle growth chart changes significantly compared to a natural cycle. Instead of one dominant follicle, you develop multiple follicles at the same time. This is achieved by daily injections of follicle-stimulating hormone (FSH), often starting on day 2 or 3 of your period. By day 5 of stimulation, many follicles may reach 8–12 millimeters. Over the next 5–7 days, follicles grow rapidly—often 1–2 millimeters per day—until several reach the mature size of 17–20 millimeters. Your care team monitors growth with frequent ultrasounds and blood tests. When enough follicles are mature, you receive a trigger shot to induce final egg maturation, and egg retrieval is scheduled about 36 hours later. Individualized FSH dosing can reduce uneven follicle growth and improve the number of mature eggs collected.
According to a 2019 study in Frontiers in Endocrinology, starting with the right FSH dose from day one leads to more synchronized follicle growth and a higher number of mature eggs at retrieval. Early and sufficient FSH dosing is key to recruiting more follicles and maximizing your chances of success.
| IVF Stimulation Day | Typical Follicle Size |
|---|---|
| 1–3 | < 9 mm |
| 4 | 7–11 mm |
| 5 | 9–13 mm |
| 6 | 11–15 mm |
| 7 | 13–17 mm |
| 8 | 15–19 mm |
| 9 | 17–21 mm |
| 10 | 19–23 mm |
| 11 | 21–25 mm |
When two or more follicles hit 18–22 mm, clinics give an hCG “trigger,” and retrieval follows about 36 hours later. Ten or more mature-sized follicles signal a robust response, but counts above 12 plus soaring estradiol raise ovarian-hyperstimulation risk.
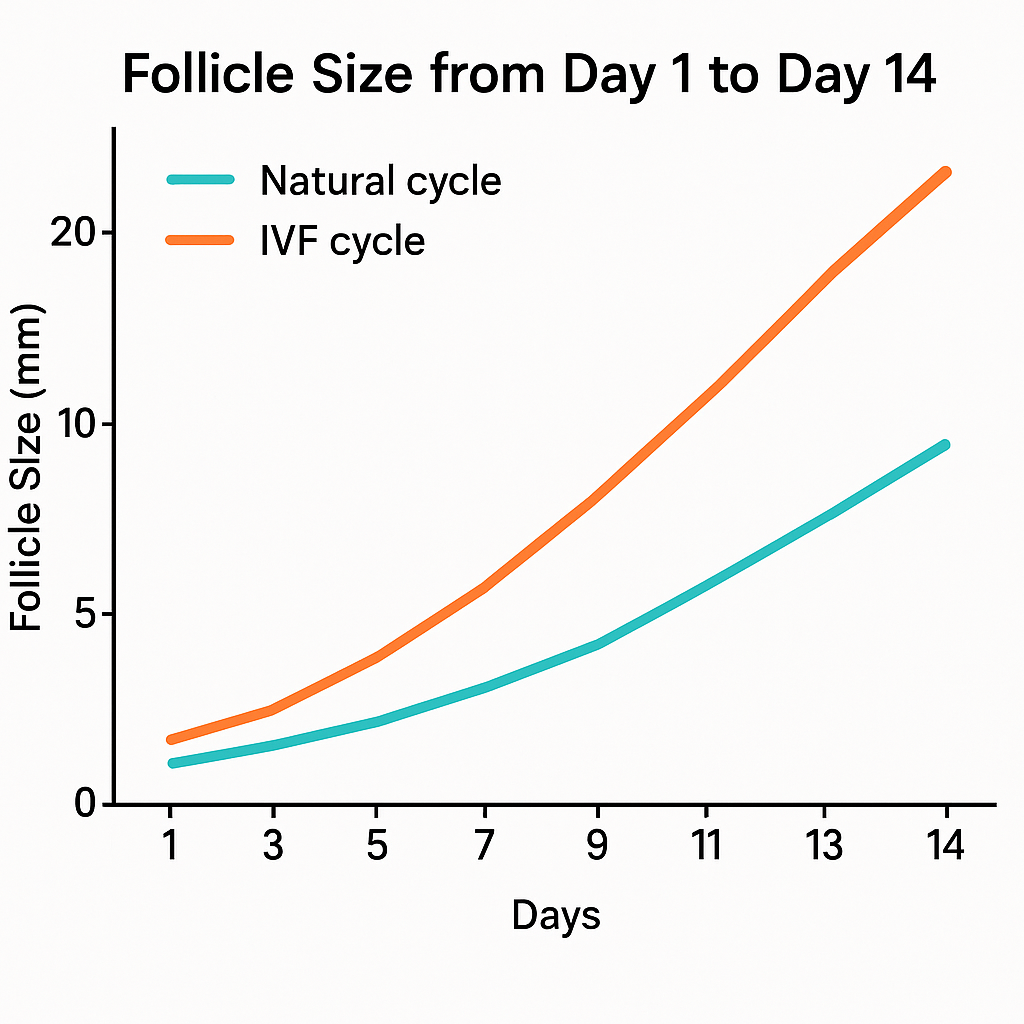
Which factors can speed up—or stall—follicle growth?
Several factors can speed up or stall your follicle growth during a menstrual or fertility treatment cycle. Understanding these can help you optimize your fertility journey:
Factors that can speed up follicle growth:
- Higher levels of follicle-stimulating hormone (FSH): FSH directly stimulates follicle growth.
- Androgens (like testosterone): In moderate amounts, androgens can enhance FSH action and promote early follicle development.
- Insulin-like growth factors (IGFs): These work with FSH to support follicle growth and maturation.
- Good nutrition: Adequate calories, protein, and healthy fats support hormone production and follicle development.
- Optimal ovarian blood flow: Good circulation delivers hormones and nutrients to growing follicles.
Factors that can stall or slow follicle growth:
- Hormonal imbalances: Low FSH, excess androgens (as in polycystic ovary syndrome), or thyroid disorders can disrupt growth.
- Poor nutrition or low body weight: These can reduce hormone levels and ovarian function.
- Chronic stress: High stress can alter hormone production and slow follicle development.
- Age: Ovarian reserve and follicle responsiveness naturally decline with age.
- Disrupted intraovarian signaling: Problems with local growth factors or signaling pathways (like the Hippo pathway) can impair follicle activation and growth.
A 2015 review in Endocrine Reviews highlights: “Both systemic hormones and local ovarian factors must work together for healthy follicle growth. Disruption in either can lead to stalled development or infertility.” — Aaron J. W. Hsueh, PhD, Professor of Obstetrics and Gynecology, Stanford University.
For more on optimizing your fertility, see guidance from the American College of Obstetricians and Gynecologists (ACOG) and the National Institutes of Health (NIH).
How can you read your follicular ultrasound like a pro?
To read your follicular ultrasound like a pro, focus on these key elements:
- Follicle Size: Mature follicles typically measure 17–20 millimeters before ovulation or egg retrieval. Multiple follicles in this range suggest a strong response, especially in in vitro fertilization (IVF) cycles.
- Follicle Count: The number of visible follicles helps estimate your ovarian reserve and potential egg yield.
- Blood Flow (Color Doppler): Healthy follicles show strong blood flow around them. The most important measurement is the peak systolic velocity (PSV). A PSV of 10 centimeters per second (cm/s) or higher means a 70–75% chance of retrieving a high-quality egg and embryo. If PSV is below 10 cm/s, the chance drops to 14–24%.
- Endometrial Lining: A thick, triple-line pattern is ideal for implantation.
How to interpret your report:
- Look for the number and size of follicles in each ovary.
- Ask your provider about the blood flow to your leading follicles.
- Check the endometrial thickness and pattern.
Recent research highlights several advances in interpreting follicular ultrasound results for fertility care. Automated and three-dimensional (3D) ultrasound technologies now allow for more accurate and objective measurement of follicle count and size, reducing operator variability and improving reliability. A 2021 study validated a novel software that automatically assesses follicle count and diameter from two-dimensional (2D) ultrasound images, showing strong agreement with manual assessments and suggesting potential time savings and greater consistency. Additionally, 3D ultrasound with automated volume calculation (sono AVC) offers detailed analysis and may further optimize timing for ovulation trigger and egg retrieval in in vitro fertilization (IVF) cycles. Consensus guidelines recommend using high-frequency transvaginal probes (≥7 MHz) and standardized protocols for antral follicle count (AFC), emphasizing that both 2D and 3D methods are effective, with the choice depending on resources and operator skill 2.
For clinical interpretation, focus on the number of antral follicles, their size (mature follicles are typically 17–20 mm), and blood flow patterns. Strong blood flow (peak systolic velocity ≥10 cm/s) is associated with a 70–75% chance of retrieving a high-quality egg and embryo. As summarized by Dr. Wellington P. Martins, MD, PhD, “Standardized ultrasound protocols and new automated tools are making follicle assessment more accurate and accessible for patients and providers”. For best results, ask your provider about the technology used and how your results compare to these benchmarks. See the American College of Obstetricians and Gynecologists (ACOG) and National Institutes of Health (NIH) for further guidance.
Tip: Bring your questions to your provider. Ask them to explain your follicle sizes, blood flow, and lining in plain language. This empowers you to make informed decisions about your fertility care.
For more, see guidance from the American College of Obstetricians and Gynecologists (ACOG) and the National Institutes of Health (NIH).
Painful twinges after scanning? Differentiate them from harmless stretching in Uterine Contractions: Good vs. Bad Cramps Explained.
What if your follicles grow too slowly, too quickly, or unevenly?
If your follicles grow too slowly, too quickly, or unevenly, it can impact ovulation and fertility outcomes.
Slow follicle growth may be caused by hormonal imbalances, such as insufficient follicle-stimulating hormone (FSH) or luteinizing hormone (LH), or by primary granulosa cell defects, which can also lead to luteinized unruptured follicle syndrome—where the follicle matures but fails to release an egg.
Rapid follicle growth is less common but can occur with excessive gonadotropin stimulation or heightened sensitivity to FSH, sometimes resulting in premature ovulation or poor egg quality.
Uneven follicle growth—where some follicles mature faster than others—often results from variations in FSH sensitivity among follicles, local ovarian factors, or disrupted intra-ovarian signaling, and can lead to a lower number of mature eggs available for retrieval or ovulation.
Metabolic and nutritional factors, such as insulin, growth hormone, and IGF-1, also influence the speed and uniformity of follicle development. Age, stress, and underlying ovarian conditions (like polycystic ovary syndrome) can further disrupt normal growth patterns. In summary, optimal follicle growth depends on a delicate balance of systemic hormones, local ovarian signals, and overall health; disruptions in any of these can cause follicles to grow too slowly, too quickly, or unevenly, affecting fertility potential.
PCOS note: Many small follicles don’t guarantee multiple eggs; letrozole protocols often coax a single healthy ovulation. Cervical structure questions? Visit Cervical Length Check: Why It Counts.
Your top questions, answered
What size follicle is ideal for conception?
The most recent and robust studies show that follicles measuring 13–18 mm on the day of ovulation trigger are most likely to yield mature eggs and lead to higher live birth rates, especially when the majority of follicles fall within this range. For natural cycles, follicles sized 18–22 mm are also associated with higher live birth rates. Follicles larger than 18 mm may be linked to premature progesterone elevation, which can negatively affect outcomes in fresh embryo transfers.
How fast do follicles grow each day?
Follicles typically grow about 1 mm per day during the late follicular phase, with some studies reporting an average daily growth rate of 1.04 mm. Estradiol levels and endometrial thickness also increase steadily alongside follicle growth.
Does having six follicles mean six eggs?
Not necessarily. While each visible follicle has the potential to contain an egg, not all follicles will yield a mature, retrievable oocyte. The proportion of mature eggs depends on follicle size and other factors; for example, follicles in the 13–18 mm range are most likely to yield mature eggs, while smaller or larger follicles are less likely to do so.
Can I increase follicle size in two days?
Follicles generally grow about 1 mm per day, so a 2 mm increase over two days is typical, but significant increases beyond this are unlikely. The growth rate is influenced by hormonal stimulation, individual ovarian response, and baseline ovarian reserve.
How many mature follicles are “good” for IVF success?
Having at least three lead follicles ≥17 mm on trigger day is associated with improved mature oocyte yield, but maximizing the proportion of follicles in the 13–18 mm range can improve mature oocyte yield by up to 42% and increase live birth rates. For women under 35, three or more mature follicles is considered favorable, while older women may benefit from a wider range of follicle sizes.
How does follicle growth sync with the rest of your fertility puzzle?
Follicle growth is a central part of the fertility puzzle, tightly coordinated with hormonal, structural, and cellular changes in the ovary to ensure the development of a healthy, fertilizable egg. As follicles grow, they undergo complex interactions with the ovarian environment, including changes in the extracellular matrix and the formation of new blood vessels, which provide nutrients and hormonal signals essential for oocyte maturation and ovulation.
The dialogue between the oocyte and surrounding somatic cells is crucial for follicle survival, growth, and the acquisition of developmental competence, with disruptions in these processes linked to infertility conditions like polycystic ovary syndrome (PCOS), endometriosis, and premature ovarian insufficiency. Follicular fluid, rich in hormones and nutrients, further supports oocyte quality and early embryo development, highlighting the importance of a healthy follicular environment for conception. The activation and growth of primordial follicles from the ovarian reserve are also tightly regulated, as premature or excessive activation can lead to early depletion and infertility.
Strong sperm matter too—see Sperm Morphology Basics: What Healthy Swimmers Look Like. After fertilization, timing slides into the Implantation Window: How Long Does It Last?, and supportive cervical mucus earns its keep—read Cervical Mucus & Sperm: How the Fluid Helps.
In summary, synchronized follicle growth is not an isolated event but is integrated with hormonal cycles, ovarian structure, and cellular communication, all of which must work in harmony for optimal fertility.
Final Thoughts
Final thoughts on ovarian follicle size emphasize its important—but not exclusive—role in predicting oocyte maturity and developmental potential in fertility treatments. Recent large-scale meta-analyses and cohort studies consistently show that follicles measuring at least 15–16 mm are most likely to yield mature oocytes, successful fertilization, and good-quality embryos, with benefits plateauing beyond this size.
While larger follicles are associated with higher rates of oocyte maturity and blastocyst formation, the chance of producing a chromosomally normal (euploid) embryo does not appear to depend on follicle size. Follicles smaller than 12–13 mm rarely yield mature oocytes or good-quality embryos, suggesting a practical lower threshold for oocyte retrieval. However, even among follicles of similar size, growth rate and underlying ovarian health can influence which follicles ultimately ovulate or produce viable eggs.
For patients with low ovarian reserve or poor response, aspirating smaller follicles may still be worthwhile, as some can yield mature oocytes, though the likelihood of developmental competence is lower. In summary, optimal follicle size is a key marker for timing interventions and maximizing IVF success, but it should be considered alongside other factors such as follicle growth dynamics, patient age, and overall ovarian reserve for the best fertility outcomes.
References
-
Clinical monitoring of serum sex hormones during normal menstrual follicle growth cycle. Chinese Journal of Laboratory Medicine, 40, 169-173. https://doi.org/10.3760/CMA.J.ISSN.1009-9158.2017.03.007
-
Intraovarian control of early folliculogenesis… Endocrine reviews, 36 1, 1-24. https://doi.org/10.1210/er.2014-1020
-
From a circle to a sphere: the ultrasound imaging of ovarian follicle with 2D and 3D technology. Gynecological Endocrinology, 35, 184 - 189. https://doi.org/10.1080/09513590.2018.1522297
-
Automated Follicular Assessment Using a Novel Two-dimensional Ultrasound-based Solution. Journal of Medical Ultrasound, 29, 264 - 269. https://doi.org/10.4103/JMU.JMU_149_20
-
Counting ovarian antral follicles by ultrasound: a practical guide. Ultrasound in Obstetrics & Gynecology, 51. https://doi.org/10.1002/uog.18945
-
FSH Requirements for Follicle Growth During Controlled Ovarian Stimulation. Frontiers in Endocrinology, 10. https://doi.org/10.3389/fendo.2019.00579
-
Individualized dosing of rec-FSH for ovarian stimulation in women with PCOS reduces asynchronous follicle growth… Archives of gynecology and obstetrics. https://doi.org/10.1007/s00404-024-07890-8