You may be wondering how long the implantation window lasts—and your concern is valid. The implantation window is a brief, critical period when your uterus is most receptive to an embryo. Missing this window can significantly lower your chances of pregnancy, even with healthy embryos and advanced fertility treatments. Studies show that even a 12-hour deviation from this optimal timeframe can nearly double the risk of pregnancy loss and cut pregnancy rates in half.
Research confirms that the implantation window typically lasts less than 48 hours, usually occurring about 7 to 10 days after ovulation. This period is tightly regulated by your hormones, especially estrogen and progesterone, and can vary from person to person. Understanding and accurately identifying your unique window can make a real difference in your fertility journey, offering hope and practical steps for improving your chances of success.
- What exactly is the implantation window, and how long does it stay open?
- When does the window fall if my cycle isn’t textbook 28 days?
- Why is the window so brief, and which hormones run the show?
- How can I spot my personal implantation window without invasive tests?
- Which daily habits keep your uterine lining receptive?
- Implantation advice online: what’s solid science and what’s folklore?
- Does timing change in IVF, ICSI, and frozen embryo transfer?
- What if implantation keeps failing—when should you call a specialist?
- Your top questions, answered
- Final Thoughts
- References
What exactly is the implantation window, and how long does it stay open?
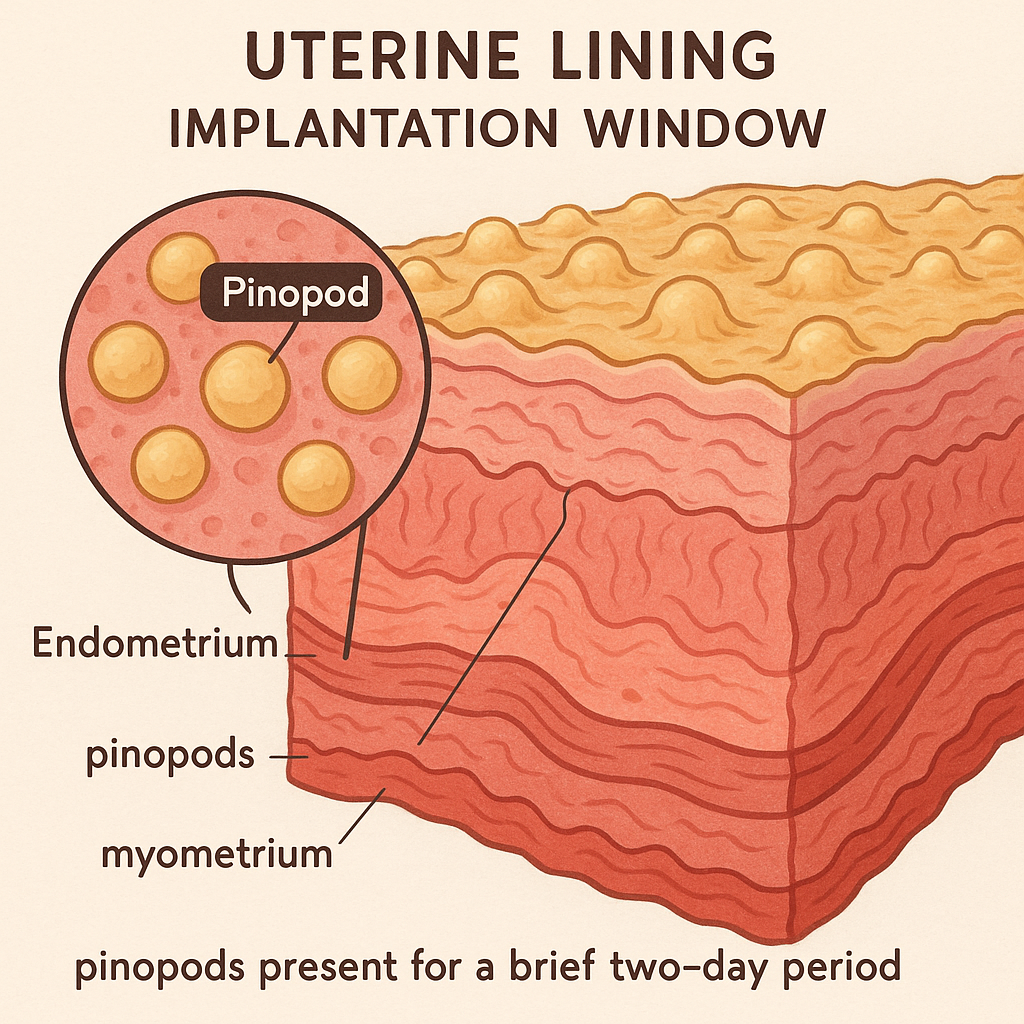
The implantation window is a short, precisely timed period during your menstrual cycle when your uterus is most receptive to an embryo. This window opens after ovulation, when the lining of your uterus (the endometrium) undergoes specific changes in response to hormones like estrogen and progesterone, making it ready for the embryo to attach and begin pregnancy. During this time, the endometrium expresses unique molecules and develops structures such as pinopodes, which help the embryo adhere and implant successfully.
In most people, the implantation window typically occurs about 7 to 10 days after ovulation and lasts less than 48 hours. The exact timing can vary from person to person and even from cycle to cycle, influenced by your individual hormonal patterns and other factors. If embryo transfer or natural conception does not align with this narrow window, the chances of successful implantation and ongoing pregnancy drop significantly—even a deviation of 12 hours can have a major impact. Understanding and, when possible, precisely identifying your implantation window can improve your chances of conception, especially if you are undergoing fertility treatments.
When does the window fall if my cycle isn’t textbook 28 days?
If your menstrual cycle is not the standard 28 days, the timing of your implantation window will shift accordingly. The implantation window generally opens about 6 to 10 days after ovulation, which itself usually occurs about 14 days before your next period, regardless of total cycle length. For example, if your cycle is 32 days, ovulation likely happens around day 18, and your implantation window would fall between days 24 and 28. If your cycle is shorter, say 25 days, ovulation may occur around day 11, with the implantation window between days 17 and 21.
Research shows that the first signs of implantation (detected by sensitive hCG tests) typically occur about 4 days before your expected period, no matter your cycle length. The window itself remains brief—usually less than 48 hours—so accurately tracking ovulation is key to identifying your personal window. Tools like ovulation predictor kits, basal body temperature charting, or hormone monitoring can help you pinpoint ovulation and better estimate when your uterus is most receptive. Understanding your unique cycle pattern empowers you to time conception efforts more effectively and increases your chances of success.
Because ovulation moves in longer or shorter cycles, the implantation window moves with it. Use the table below to see how timing shifts:
| Cycle Length | Probable Ovulation | Window Opens | Window Closes |
|---|---|---|---|
| 26 days | Day 12 | Day 18 | Day 22 |
| 28 days | Day 14 | Day 20 | Day 24 |
| 30 days | Day 16 | Day 22 | Day 26 |
| 32 days | Day 18 | Day 24 | Day 28 |
A consistently short luteal phase (<11 days) can push the window too close to your period. If that sounds familiar, see Short Luteal Phase: Causes and Fixes for targeted solutions.
Why is the window so brief, and which hormones run the show?
The implantation window is brief because your uterus must be in a highly specialized, receptive state for successful embryo attachment, and this state is tightly controlled by hormones—primarily estrogen and progesterone.
Progesterone prepares your endometrial lining for implantation, while estrogen determines both when the window opens and how long it stays open. Research shows that only a narrow range of estrogen levels will keep the uterus receptive: low estrogen can extend the window, but high estrogen causes it to close quickly, making the uterus unreceptive and even altering the expression of key implantation-related genes. This precise hormonal balance ensures that the endometrium is only receptive for about 24 to 48 hours, reducing the risk of abnormal implantation and supporting healthy pregnancy development.
Other molecules, such as cytokines, integrins, and growth factors, also play supporting roles in fine-tuning receptivity and signaling between the embryo and uterus. However, the main “conductors” of this process are estrogen and progesterone, which synchronize the timing of endometrial changes with embryo development. Once the window closes, the endometrium becomes refractory, actively resisting implantation until the next cycle. This tight regulation is essential for maximizing your chances of a healthy pregnancy and explains why even small hormonal imbalances can impact fertility outcomes.
Dive deeper into the hormone dance in Key Hormones: Estrogen, Progesterone, Testosterone.
How can I spot my personal implantation window without invasive tests?
You can estimate your personal implantation window using several non-invasive methods, though none are perfect yet.
- Track ovulation at home using ovulation predictor kits, basal body temperature, or cervical mucus monitoring to estimate when your implantation window is likely to occur.
- Analyze extracellular vesicles (EVs) or exosomes from uterine flushings or a cervical brush, which can reflect endometrial receptivity through specific molecular markers—this is a promising, less-invasive research method but not yet widely available for home use.
- Use advanced ultrasound imaging (radiomics) combined with machine learning to assess endometrial receptivity non-invasively; this approach is under investigation and may help identify the optimal window in the future.
- Monitor hormone levels (such as progesterone and estrogen) through blood or saliva tests to help estimate the timing of ovulation and the likely window, though this is an indirect method.
- Future non-invasive, mechanism-based molecular tests are being developed to directly assess endometrial readiness using single-cell or fluid-based sampling, aiming for more accurate and accessible detection of the implantation window.
Which daily habits keep your uterine lining receptive?
Daily habits that help keep your uterine lining receptive focus on supporting overall reproductive health, hormone balance, and reducing inflammation.
- Maintain a healthy weight, as obesity can disrupt endometrial gene expression and reduce uterine receptivity.
- Eat a balanced diet rich in antioxidants, vitamins (especially vitamin D and E), and healthy fats to support endometrial health; vitamin D supplementation has been shown to improve receptivity by enhancing key molecular pathways.
- Engage in regular moderate exercise to help regulate hormones and reduce inflammation, but avoid excessive or intense workouts that may negatively affect reproductive hormones.
- Avoid smoking and limit alcohol consumption, as both can impair hormone function and endometrial receptivity.
- Manage stress through relaxation techniques, mindfulness, or counseling, since chronic stress can disrupt hormonal balance and uterine health.
- Ensure adequate sleep and address chronic health conditions (like diabetes or thyroid disorders) to support overall reproductive health.
- Gentle pelvic tilts, deep squats, and five minutes of belly breathing can enhance pelvic perfusion. For a bigger boost, try the stretches in Boost Uterine Blood Flow: Easy Moves and Tips.
- Consider complementary practices such as acupuncture, which may improve blood flow to the uterus and support receptivity.
- Nutritional supplements like carnitines, melatonin, and vitamin E may offer additional benefits for endometrial receptivity, but consult a healthcare provider before starting new supplements.
For lining thickness benchmarks and ultrasound tips, visit Healthy Uterine Lining: Why Thickness Matters.
Implantation advice online: what’s solid science and what’s folklore?
When seeking implantation advice online, it’s important to distinguish evidence-based guidance from common myths. Here’s what current science supports—and what’s folklore:
Solid Science:
- Track ovulation using ovulation predictor kits, basal body temperature, or cervical mucus to time intercourse or embryo transfer. This aligns with American College of Obstetricians and Gynecologists (ACOG) and National Institutes of Health (NIH) guidance.
- Maintain a healthy weight, balanced diet, and regular moderate exercise. These habits support hormone balance and endometrial health.
- Avoid smoking and limit alcohol, as both can reduce fertility and impair uterine receptivity.
- Manage stress and get adequate sleep; chronic stress can disrupt reproductive hormones.
- Vitamin D supplementation may improve endometrial receptivity, according to recent peer-reviewed studies.
“There is no evidence that lying flat after intercourse or embryo transfer increases implantation rates,” says Dr. Eve Feinberg, MD, Associate Professor of Obstetrics and Gynecology, Northwestern University.
Folklore/Myths:
- Eating pineapple core, drinking pomegranate juice, or using fertility crystals has no proven effect on implantation.
- Special sexual positions or keeping your legs elevated after intercourse do not increase your chances.
- Over-the-counter “implantation boosters” are not supported by clinical research.
About 85% of healthy couples conceive within one year of regular, unprotected intercourse (CDC). If you have concerns, consult a reproductive endocrinologist for personalized, evidence-based care.
For myths about cramps and uterine movement see Uterine Contractions: Good vs. Bad Cramps Explained.
Does timing change in IVF, ICSI, and frozen embryo transfer?
The timing of embryo implantation in in vitro fertilization (IVF), intracytoplasmic sperm injection (ICSI), and frozen embryo transfer (FET) is carefully managed to maximize success. In fresh IVF and ICSI cycles, embryos are usually transferred a few days after egg retrieval, aiming to match the embryo’s stage with the endometrium’s natural window of receptivity. In FET cycles, embryos are thawed and transferred in a later cycle, allowing more flexibility and precise synchronization with the endometrium. Recent meta-analyses show that immediate FET (in the cycle right after egg retrieval) is at least as effective as postponing FET for one or more cycles, with a slightly higher live birth rate and clinical pregnancy rate for immediate FET (adjusted odds ratio for live birth rate: 1.20, 95% CI 1.01–1.44).
The choice between fresh and frozen transfer does not significantly affect overall cumulative live birth rates, but FET can reduce the risk of ovarian hyperstimulation syndrome (OHSS), especially in high responders. The timing of FET is guided by endometrial preparation, embryo stage (cleavage or blastocyst), and sometimes personalized endometrial receptivity testing to ensure optimal conditions for implantation. For most patients, the cumulative live birth rate is similar whether using a fresh or freeze-all strategy, but time to pregnancy may be shorter with fresh transfer since FET involves a delay. In summary, while the timing of implantation is carefully managed in all approaches, FET offers more control and can be timed immediately or after a delay, with similar or slightly improved outcomes compared to fresh transfers.
As Dr. S. Bergenheim, MD, PhD, notes: “The standard clinical practice of postponing FET for at least one menstrual cycle following a failed fresh transfer or a freeze-all cycle may not be best clinical practice”.
Embryo quality still matters, so explore Strong Egg Mitochondria: Simple Ways to Boost Cell Power alongside timing tweaks.
What if implantation keeps failing—when should you call a specialist?
If implantation keeps failing, you should consider calling a fertility specialist when you have experienced at least three failed embryo transfers with good-quality embryos, especially if you are under age 40. This is often referred to as recurrent implantation failure (RIF). Some guidelines recommend seeking further evaluation after failing to achieve pregnancy following the transfer of embryos with a cumulative predicted chance of implantation greater than 60%. True RIF is rare, affecting less than 5% of couples undergoing assisted reproductive technology (ART).
You should also seek help sooner if you have risk factors such as advanced maternal age, known uterine abnormalities, repeated miscarriages, or if you have concerns about your or your partner’s health. A specialist will investigate possible causes, including uterine or anatomical issues, embryo quality, male factors, immune or hormonal imbalances, and lifestyle factors like smoking or high body mass index.
Dr. N. Macklon, MD, Professor of Obstetrics and Gynaecology, states: “When a couple have not had a successful implantation by a certain number of embryo transfers and the cumulative predicted chance of implantation is greater than 60%, then they should be counselled on further investigation and/or treatment options”.
About 10% of women seeking IVF experience RIF, and most can become pregnant after targeted clinical intervention. If you are unsure, it is always appropriate to reach out to a reproductive endocrinologist for personalized guidance and support.
Expect tests for progesterone levels, thyroid function, semen quality, uterine anatomy, and, if needed, immune factors Immunity and Fertility: Can Your Body Reject Pregnancy?.
Your top questions, answered
How soon after implantation will a pregnancy test turn positive?
You can usually get a positive result on a home urine pregnancy test about 10–14 days after ovulation, which is roughly 1–2 days after implantation. Blood tests can detect pregnancy slightly earlier, often within 7–10 days after ovulation.
Can stress shift my implantation window?
Yes, high stress can disrupt the hormonal and cellular environment of your uterus, potentially shifting or narrowing your window of implantation. Research shows that stress responses in the endometrium can lead to changes in cell function and may increase the risk of implantation failure or miscarriage.
Does caffeine hurt implantation?
Caffeine may negatively affect implantation. Animal studies and epidemiological data suggest that caffeine can impair embryo transport, development, and uterine receptivity, leading to abnormal implantation and increased risk of pregnancy loss. Sensitivity to caffeine varies, but it’s safest to limit intake during early pregnancy. The Centers for Disease Control and Prevention (CDC) recommends keeping caffeine below 200 mg per day.
Is the window later in long cycles?
Yes, if your menstrual cycles are longer than average, your window of implantation (the days when your uterus is most receptive) will likely occur later. The window typically opens about 6–10 days after ovulation, so a later ovulation means a later window. Precise timing is crucial: transfers outside this window can cut pregnancy rates in half and double the risk of pregnancy loss.
Final Thoughts
The implantation window—the brief period when your uterus is receptive to an embryo—typically lasts about 24 to 48 hours in a natural cycle, usually occurring 6 to 10 days after ovulation. This window is tightly regulated by hormones, especially estrogen and progesterone, and can shift slightly based on your individual cycle or fertility treatments. Research shows that even a deviation of more than 12 hours from this optimal window can cut pregnancy rates in half and double the risk of pregnancy loss. In assisted reproductive technology (ART), such as frozen embryo transfer, the window can be personalized and may extend up to several days with careful hormonal preparation, but precision remains crucial.
Markers like pinopodes and specific gene expression patterns help specialists pinpoint your unique window. As Dr. Maria Enciso, PhD, explains: “Precise determination of the window of implantation and personalized embryo transfer can significantly improve clinical outcomes”. If you’re struggling with implantation, ask your provider about tests to identify your optimal window. Remember, timing is everything—successful implantation depends on matching embryo development with your endometrium’s readiness.
References
-
The precise determination of the window of implantation significantly improves ART outcomes. Scientific Reports, 11. https://doi.org/10.1038/s41598-021-92955-w
-
Non-invasive prediction of implantation window in controlled hyperstimulation cycles: Can the time from the menstrual day at embryo transfer to expected menstrual cycle give a clue?. Turkish Journal of Obstetrics and Gynecology, 13, 116 - 122. https://doi.org/10.4274/tjod.34651
-
Non-Invasive and Mechanism-Based Molecular Assessment of Endometrial Receptivity During the Window of Implantation: Current Concepts and Future Prospective Testing Directions. Frontiers in Reproductive Health, 4. https://doi.org/10.3389/frph.2022.863173
-
Optimizing evaluation of endometrial receptivity in recurrent pregnancy loss: a preliminary investigation integrating radiomics from multimodal ultrasound via machine learning. Frontiers in Endocrinology, 15. https://doi.org/10.3389/fendo.2024.1380829
-
The Molecular Link between Obesity and the Endometrial Environment: A Starting Point for Female Infertility. International Journal of Molecular Sciences, 25. https://doi.org/10.3390/ijms25136855
-
Immediate versus postponed frozen embryo transfer after IVF/ICSI: a systematic review and meta-analysis… Human reproduction update. https://doi.org/10.1093/humupd/dmab002
-
The role of timing in frozen embryo transfer… Fertility and sterility. https://doi.org/10.1016/j.fertnstert.2022.08.009
-
Recurrent implantation failure. Human Reproduction. https://doi.org/10.1093/humrep/dead093.119
-
RECURRENT IMPLANTATION FAILURE (RIF): REALITY OR A STATISTICAL MIRAGE? Consensus statement from the July 1, 2022 Lugano Workshop on repeated implantation failures (RIF)… Fertility and sterility. https://doi.org/10.1016/j.fertnstert.2023.02.014