If you are concerned about sperm health, you are not alone. Sperm morphology; how sperm look under a microscope, has long been considered an important part of fertility assessments. In the United States, about 9% of men of reproductive age experience fertility challenges, and sperm quality is a key factor for many couples trying to conceive. Understanding what healthy sperm look like can help you make informed decisions and feel more in control of your fertility journey.
Healthy sperm typically have an oval head, an intact midpiece, and a straight tail, all of which are important for swimming efficiently and reaching the egg. However, only a small percentage of sperm in a typical sample, often less than 10%, meet these strict criteria for “normal” morphology, even in fertile men. While abnormal shapes are common, research shows that having some normal-shaped sperm is usually enough for natural conception, and the exact percentage needed is still debated.
It’s important to remember that sperm morphology is just one piece of the fertility puzzle. Many people with low percentages of “normal” sperm still achieve pregnancy, and other factors like sperm count, movement, and overall health matter just as much. If you have concerns about your fertility, seeking guidance and support is a positive first step.
- What is sperm morphology, and how do labs judge those shapes?
- Why do only 4 % “perfect” sperm still get the job done?
- What does a healthy swimmer look like under the microscope?
- What sparks abnormal sperm shapes in the first place?
- How can targeted lifestyle shifts reshape sperm within one 72-day cycle?
- Which supplements truly improve sperm shape—and which are hype?
- When should you pivot from lifestyle tweaks to medical help?
- How do I read my semen analysis report without freaking out?
- Can we still conceive naturally with low morphology?
- What does a 90-day “Sperm Shape Upgrade” plan look like?
- Your top sperm-morphology questions, answered
- Final thoughts
- References
What is sperm morphology, and how do labs judge those shapes?
Sperm morphology refers to the size and shape of sperm cells, which are evaluated as part of a standard semen analysis to help assess male fertility. Laboratories judge sperm morphology by examining stained semen samples under a microscope and classifying each sperm as “normal” or “abnormal” based on strict criteria. These criteria, often called “Kruger strict criteria,” require a sperm to have an oval head, an intact midpiece, and a straight, uncoiled tail to be considered normal. Even small irregularities, such as a tapered head or bent tail, can cause a sperm to be labeled abnormal under these standards.
The percentage of normal-shaped sperm is then reported, with most fertile men having less than 10% normal forms by strict criteria. Labs may use either strict or more liberal criteria, but strict criteria are more predictive of fertilization success, especially in IVF settings. However, there can be variability between technicians and labs, so consistent training and quality control are important to ensure reliable results. While sperm morphology is just one factor in fertility, its careful assessment provides valuable information for your reproductive planning.
Remember, morphology is only one piece of the semen-analysis puzzle that also measures count, motility, and hormone balance—see how hormones fit in Key Hormones.
Why do only 4 % “perfect” sperm still get the job done?
Even if only about 4% of your sperm are considered “perfect” by strict laboratory standards, you can still achieve pregnancy. This is because the criteria for “normal” sperm morphology are extremely rigorous; most men, even those who are fertile, have a low percentage of sperm that meet these standards. Research shows that having at least 4% normal-shaped sperm is associated with reasonable fertilization and pregnancy rates, especially when other factors like sperm count and motility are within normal ranges.
The reason a small percentage is enough is that only one sperm needs to successfully reach and fertilize the egg. Even when the majority of sperm are misshapen, the few that are normal can still do the job, and the body naturally selects for the healthiest swimmers during the journey to the egg. Studies confirm that men with 4% or slightly less normal forms can still father children, and pregnancy rates do not drop to zero below this threshold, there is just a gradual decrease in success, not an absolute barrier.
So, while a higher percentage of normal sperm may improve your chances, having only 4% “perfect” sperm is often enough for conception, especially if other semen parameters are healthy.
Count and motility often compensate, and supportive cervical mucus further helps healthy-shaped sperm navigate the reproductive tract—read how that works in Cervical Mucus & Sperm.
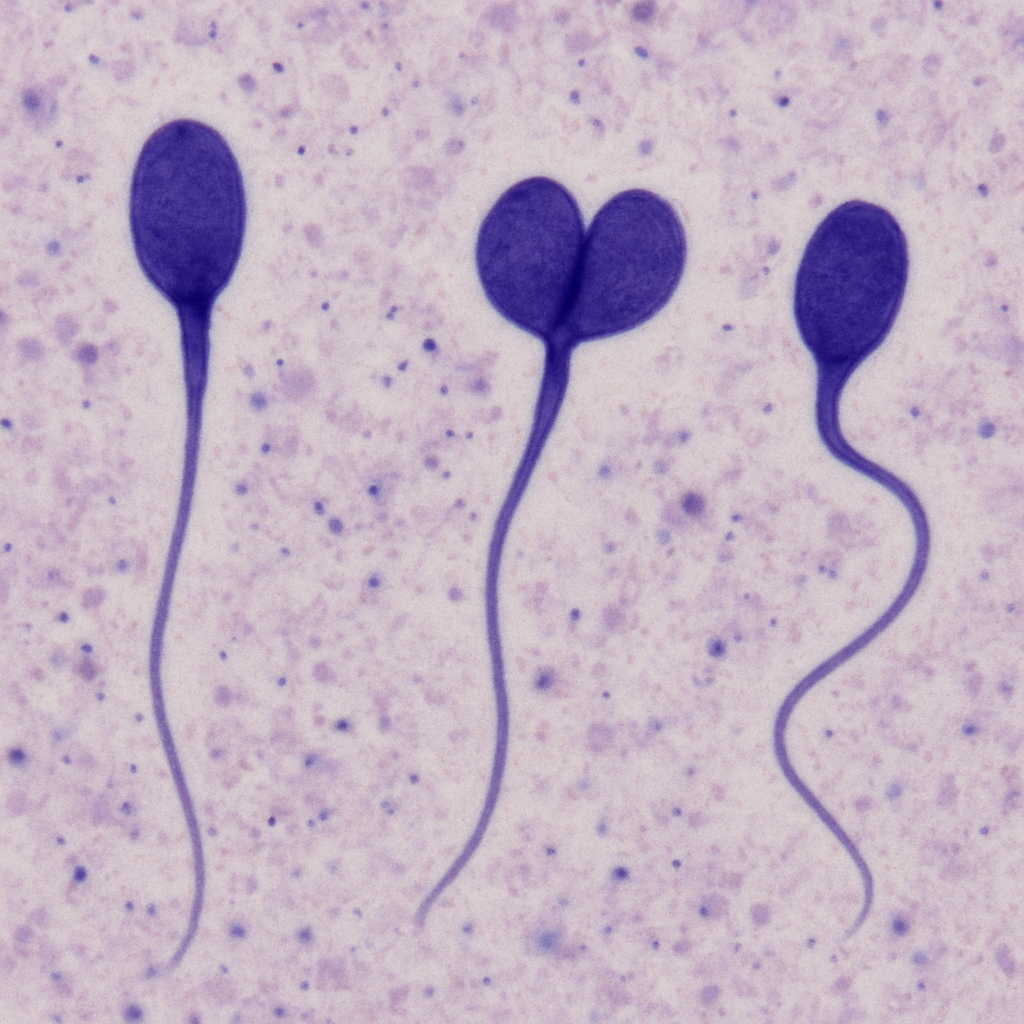
What does a healthy swimmer look like under the microscope?
A healthy sperm, often called a “swimmer,” has a very specific appearance under the microscope. It features an oval-shaped head with a smooth contour, which houses tightly packed genetic material. The midpiece, just behind the head, should be straight and uniform, containing mitochondria that power the sperm’s movement. The tail is long, thin, and uncoiled, allowing the sperm to swim efficiently toward the egg. High-magnification and digital imaging techniques reveal that healthy sperm lack large vacuoles (bubble-like spaces) in the head, which are linked to poor chromatin quality and may affect embryo development.
Recent advances, such as digital holographic microscopy, allow for detailed three-dimensional assessments of sperm shape and structure. They confirm that fertile individuals tend to have sperm with consistent head, midpiece, and tail dimensions, and minimal structural irregularities. Selecting sperm without vacuoles and with ideal morphology is considered favorable for embryo development and may improve fertility outcomes.
What sparks abnormal sperm shapes in the first place?
Abnormal sperm shapes, known as teratozoospermia, can arise from a mix of genetic, environmental, and lifestyle factors. Understanding these causes can help you take practical steps to support your fertility.
Common causes include:
- Genetic mutations: Over 90 genes have been linked to abnormal sperm head or tail shapes. For example, mutations in genes like SUN5, DPY19L2, and DNAH1 can disrupt sperm structure and function. The Centers for Disease Control and Prevention (CDC) notes that genetic factors play a significant role in many cases of male infertility.
- Oxidative stress: High levels of reactive oxygen species (ROS) can damage sperm DNA and membranes, leading to misshapen sperm. This stress often results from inflammation, infection, or exposure to toxins.
- Nutritional deficiencies: Lack of key nutrients, such as zinc, can increase abnormal sperm and oxidative stress. A recent study found that zinc-deficient diets in mice led to more sperm with abnormal shapes, but these changes improved with proper nutrition.
- Environmental exposures: Heat (from fevers or hot tubs), smoking, pollution, and certain chemicals can harm sperm development and shape.
- Medical conditions: Varicoceles (enlarged veins in the scrotum), infections, and hormonal imbalances can also contribute to abnormal morphology.
Dr. Manvi Arora, PhD, reproductive genetics specialist, explains: “Mutations in more than 90 genes have now been identified as direct causes of sperm head and tail defects, highlighting the complex genetic basis of teratozoospermia”.
If you are concerned about sperm shape, know that many causes are manageable. Addressing lifestyle factors, treating medical conditions, and seeking expert guidance can improve your chances of healthy sperm.
Immune misfires can also hinder sperm; learn more in Immunity and Fertility.
How can targeted lifestyle shifts reshape sperm within one 72-day cycle?
You can make meaningful changes to your sperm health within one full spermatogenesis cycle—about 72 days—by targeting key lifestyle factors. Sperm develop continuously, so your choices today can influence the quality of sperm released in just a few months. Here’s how you can help reshape your sperm:
- Improve your diet: A balanced diet rich in antioxidants, vitamins, and minerals supports sperm development and reduces oxidative stress, which can damage sperm structure.
- Maintain a healthy weight: Obesity disrupts hormone levels and impairs sperm production. Weight loss through diet and exercise can improve sperm quality and function.
- Quit smoking and limit alcohol: Both smoking and excessive alcohol use are linked to lower sperm count and abnormal shapes. Stopping these habits can boost sperm health.
- Manage stress: Chronic stress raises cortisol, which can interfere with hormones needed for sperm production. Mindfulness, therapy, or regular exercise can help.
- Prioritize sleep: Poor sleep quality and short duration are associated with lower sperm motility and concentration. Aim for 7–8 hours of restful sleep each night.
By making these targeted shifts, you give your body the best chance to produce healthier sperm in as little as 72 days. Lifestyle interventions like nutritional, physical, and psychological can help couples achieve better health and improve their fertility prospects within a single spermatogenic cycle.
Healthy sperm partners well with a receptive uterus—pair these habits with tips in Boost Uterine Blood Flow for a conception two-fer.
Which supplements truly improve sperm shape—and which are hype?
Some supplements have credible evidence for improving sperm shape (morphology), while others are more hype than help. The most promising supplements, based on recent peer-reviewed studies and meta-analyses, include:
- Carnitine and Coenzyme Q10 (CoQ10): Both have shown significant improvements in sperm morphology, with carnitine increasing normal forms by up to 4.9% and CoQ10 by about 1% in randomized controlled trials. These supplements also boost motility and overall sperm quality.
- Vitamin D: Supplementation can modestly improve sperm morphology and motility, especially in men with low vitamin D levels. A 2023 meta-analysis found a small but significant benefit for sperm shape.
- Vitamin A: Recent research links vitamin A to better acrosome integrity and overall sperm health.
- Lycopene: A 12-week trial in healthy men found that lycopene supplementation significantly improved the proportion of sperm with normal morphology.
- N-acetyl-cysteine (NAC): This antioxidant reduced abnormal sperm forms and DNA damage in men with infertility after three months of use.
- Selenium and omega-3 fatty acids: Both have shown modest improvements in sperm morphology in meta-analyses.
Supplements with less convincing evidence:
- Folic acid and zinc (alone or together): Recent meta-analyses show little to no effect on sperm morphology, though folic acid may help motility.
- Vitamin C: While some analyses suggest a trend toward improved morphology, the effect is not statistically significant.
In summary, carnitine, CoQ10, vitamin D, lycopene, and NAC have the strongest evidence for improving sperm shape, while folic acid, zinc, and vitamin C are less reliable for this specific outcome. Always consult your healthcare provider before starting supplements, as individual needs and underlying causes of abnormal morphology vary.
When should you pivot from lifestyle tweaks to medical help?
You should consider seeking medical help for fertility if you and your partner have been trying to conceive for 12 months or more without success, or after 6 months if you are over age 35. If you have known risk factors such as a history of undescended testicles, testicular cancer, prior chemotherapy/radiation, significant genital trauma, or symptoms like erectile dysfunction, low libido, or pain/swelling in the testicles; seek help sooner.
Medical evaluation typically includes a detailed history, physical exam, and semen analysis. If abnormalities are found, further tests may be needed to identify treatable causes. Pivot to medical care if:
- You have persistently abnormal semen analyses after lifestyle changes.
- You or your partner have known reproductive health issues.
- You experience symptoms suggesting hormonal or anatomical problems.
- You have a history of sexually transmitted infections or chronic illnesses.
The American Urological Association and American Society for Reproductive Medicine recommend early evaluation to identify reversible causes and prevent unnecessary delays. “Male infertility is recognized as a disease with effects on quality of life for both members of the infertile couple,” notes Dr. Michael L. Eisenberg, MD, reproductive urologist. Timely medical help can improve your chances of conception and address underlying health concerns.
Egg quality matters too—see Strong Egg Mitochondria for a balanced approach.
How do I read my semen analysis report without freaking out?
Reading your semen analysis report can feel overwhelming, but understanding the basics helps you focus on what matters and avoid unnecessary worry. Here’s how to approach your results:
- Know the key parameters: Most reports include sperm concentration (how many sperm per milliliter), motility (how well sperm move), and morphology (shape and structure). The World Health Organization (WHO) provides reference ranges, but these are guidelines, not strict pass/fail cutoffs.
- Expect some variation: Sperm counts and quality can fluctuate naturally from sample to sample and even between labs. A single “abnormal” result does not mean you are infertile.
- Look at the big picture: No single number predicts your fertility. Many people with results outside the “normal” range still conceive naturally. Your doctor will interpret your results in the context of your overall health and fertility history.
- Ask about lab quality: Results are more reliable from accredited labs that follow strict protocols. If you have questions, ask your provider about the lab’s standards.
- Don’t panic over small deviations: Slightly low or high values are common and often not cause for alarm. Focus on trends and your doctor’s advice, not isolated numbers.
Remember, “an individual’s sperm production itself may vary widely over a number of months,” says Dr. J. Kirkman-Brown, reproductive scientist. If you’re unsure, bring your report to a fertility specialist—they can explain what your results mean for you and your family-building goals.
Can we still conceive naturally with low morphology?
Yes, you can still conceive naturally with low sperm morphology. Research shows that even men with 0% normal sperm shapes (strict morphology) have achieved natural pregnancies—about 29% did so without assisted reproductive technology, compared to 56% of men with higher morphology scores. Sperm morphology alone is a weak predictor of fertility; many couples conceive naturally despite low percentages of normal forms.
Other factors, such as total sperm count and motility, play a bigger role in your chances of conception. If your sperm count and movement are within normal ranges, low morphology is less likely to prevent pregnancy. The World Health Organization and leading fertility experts now agree that abnormal morphology by itself should not exclude you from trying to conceive naturally.
If you have been trying for a year (or six months if your partner is over 35) without success, or if you have other risk factors, consult a fertility specialist for a full evaluation. As Dr. Jason Kovac, MD, PhD, reproductive urologist, notes: “Strict morphology should not be used to predict fertilization, pregnancy, or live birth potential. In men with 0% normal forms, alternative modalities should be considered before immediate IVF”.
Stay encouraged—many people with low morphology go on to have healthy pregnancies naturally.
Morphology does not raise birth-defect risk; it only affects the sperm’s journey. Synchronizing intercourse with the Implantation Window further tips odds in your favor.
What does a 90-day “Sperm Shape Upgrade” plan look like?
A 90-day “Sperm Shape Upgrade” plan focuses on daily habits and targeted supplements shown to improve sperm morphology within one full spermatogenesis cycle. Start with a balanced diet rich in antioxidants, healthy fats (especially omega-3s from fish, walnuts, or hemp oil), and plenty of fruits and vegetables, as these nutrients support sperm membrane health and reduce oxidative stress.
Consider adding a high-quality omega-3 supplement, since studies in animals and humans link increased omega-3 intake to better sperm shape and motility. Vitamin E supplementation (400–800 IU daily) has also been shown to significantly improve sperm morphology in men with infertility, sometimes outperforming herbal alternatives like carob.
If you’re exposed to environmental stressors (like mobile phone radiation), adding antioxidant-rich foods or supplements such as pomegranate juice may help reverse negative effects on sperm shape. Maintain a healthy weight, exercise regularly, avoid smoking and excess alcohol, and manage stress, as these lifestyle factors all influence sperm quality.
Track your progress by repeating a semen analysis after 90 days to assess improvements. While advanced lab techniques for sperm morphology assessment are evolving, focus on consistent, evidence-based changes for the best results. Always consult a healthcare provider before starting new supplements or making major lifestyle changes.
Partners can sync by checking Healthy Uterine Lining for optimal implantation.
Your top sperm-morphology questions, answered
How fast can morphology improve?
Sperm morphology can begin to improve within one full spermatogenesis cycle, which is about 70–90 days. Lifestyle changes, antioxidant use, and addressing oxidative stress may help, but improvements are gradual and depend on the underlying cause. Seasonal and environmental factors can also influence sperm shape, so consistency in healthy habits is key.
Does abnormal shape raise birth-defect risk?
Current research shows that having a low percentage of normal-shaped sperm does not increase the risk of birth defects or adverse neonatal outcomes. Studies of both IVF and intrauterine insemination (IUI) cycles found no significant difference in birth defect rates between men with low (<4%) and normal sperm morphology. The main impact of poor morphology is a higher chance of fertilization failure, not increased risk to the baby.
Is clear semen a concern?
Semen color varies and clear semen is usually not a cause for concern, especially if the sample is small or if ejaculation is frequent. Semen may appear clearer with lower sperm concentration, but this does not always indicate a problem. If you notice persistent changes in color, volume, or consistency, especially if accompanied by pain or other symptoms, consult a healthcare provider.
Should I abstain or ejaculate often?
Frequent ejaculation (every 2–3 days) is generally recommended for optimal sperm quality, including morphology. Prolonged abstinence does not improve sperm shape and may actually increase the proportion of abnormal forms. Regular ejaculation helps maintain healthy sperm parameters and reduces oxidative stress.
Final thoughts
Sperm morphology—the percentage of sperm with a “normal” shape—has long been included in semen analysis, but its true importance for fertility is now seen as limited. Recent research shows that sperm morphology has low predictive value for natural conception and even for assisted reproductive technologies like IUI and IVF, except in rare cases of severe, specific genetic defects. The thresholds for what counts as “normal” have changed over time, and there is significant variability in how labs assess morphology, making results difficult to interpret and compare.
Most men with low morphology can still conceive naturally, and abnormal shape alone is rarely a reason to move directly to advanced fertility treatments. While morphology can sometimes correlate with other sperm problems, such as DNA fragmentation or oxidative stress, it is not a reliable stand-alone marker of fertility potential. The field is moving toward a more holistic view, considering multiple sperm parameters and the couple’s overall situation, rather than focusing on morphology in isolation.
Future research aims to improve the accuracy and consistency of morphology assessment and to better understand the genetic and environmental factors that influence sperm shape. For now, sperm morphology should be seen as just one piece of the fertility puzzle—not a definitive predictor of success or failure.
Ready to start? Save this plan, share it with your partner, and explore Short Luteal Phase Fixes to support conception from both sides. You’ve got evidence—and hope—on your side.
References
-
Human Sperm Morphology as a Marker of Its Nuclear Quality and Epigenetic Pattern. Cells, 11. https://doi.org/10.3390/cells11111788
-
Human live spermatozoa morphology assessment using digital holographic microscopy. Scientific Reports, 12. https://doi.org/10.1038/s41598-022-08798-6
-
Male infertility. Nature Reviews Disease Primers, 9, 1-22. https://doi.org/10.1038/s41572-023-00459-w
-
Effect of Sperm Morphology on Pregnancy Success via Intrauterine Insemination: A Systematic Review and Meta‐Analysis. The Journal of Urology, 199, 812–821. https://doi.org/10.1016/j.juro.2017.11.045
-
Implications of lifestyle factors on male reproductive health. JBRA Assisted Reproduction, 28, 320 - 330. https://doi.org/10.5935/1518-0557.20240007
-
Influence of Age, Obesity, Smoking, Sleep duration and Sleep Quality on Concentration, Morphology, and Sperm Motility: A Cross-Sectional Study. International Journal of Fertility & Sterility, 18, 240 - 247. https://doi.org/10.22074/IJFS.2023.1983273.1413
-
Impact of Vitamin A and Vitamin D3 in sperm morphology. International Journal of Pharmaceutical Research and Applications. https://doi.org/10.35629/4494-0905840848
-
Effects of folic acid and folic acid plus zinc supplements on the sperm characteristics and pregnancy outcomes of infertile men: A systematic review and meta-analysis. Heliyon, 9. https://doi.org/10.1016/j.heliyon.2023.e18224
-
The Effect of Nutrients and Dietary Supplements on Sperm Quality Parameters: A Systematic Review and Meta-Analysis of Randomized Clinical Trials… Advances in nutrition, 9 6, 833-848. https://doi.org/10.1093/advances/nmy057
-
Diagnostic Semen Analysis. Oxford Textbook of Endocrinology and Diabetes 3e. https://doi.org/10.1093/med/9780198870197.003.0484
-
Vitamin D supplementation for improving sperm parameters in infertile men: A systematic review and meta-analysis of randomized clinical trials. Arab Journal of Urology: An International Journal, 21, 204 - 212. https://doi.org/10.1080/2090598X.2023.2165232
-
Men with a complete absence of normal sperm morphology exhibit high rates of success without assisted reproduction. Asian Journal of Andrology, 19, 39 - 42. https://doi.org/10.4103/1008-682X.189211
-
Intra-Technician Comparison of Sperm Morphology Evaluation. Reproductive BioMedicine Online. https://doi.org/10.1016/j.rbmo.2018.06.012
-
Genetic etiological spectrum of sperm morphological abnormalities… Journal of assisted reproduction and genetics. https://doi.org/10.1007/s10815-024-03274-8
-
Mechanisms of damage to sperm structure in mice on the zinc-deficient diet… Journal of trace elements in medicine and biology : organ of the Society for Minerals and Trace Elements, 79, 127251. https://doi.org/10.1016/j.jtemb.2023.127251