One in five babies with chronic ear infections faces measurable language delays, a hidden risk that can worry any parent. But by understanding how a “simple” earache impacts the developing brain, you can take proactive steps to keep your child’s language, learning, and social skills on track.
- Why are ear infections so common in babies and why should brain-conscious parents care?
- How does temporary hearing loss from an ear infection disrupt language circuits in the developing brain?
- Can an ear infection really reach the brain, and what warning signs demand emergency care?
- What are the long-term cognitive and behavioral ripples of recurrent ear infections?
- What proven steps can parents take to prevent ear infections and safeguard brain development?
- When should you push for a hearing test, antibiotics, or specialist referral?
- How do you balance antibiotics, gut health, and resistance worries?
- Rapid-fire answers to parents’ top ear-infection questions
- Final Thoughts: Protecting Tiny Ears, Nurturing Growing Brains
Why are ear infections so common in babies and why should brain-conscious parents care?
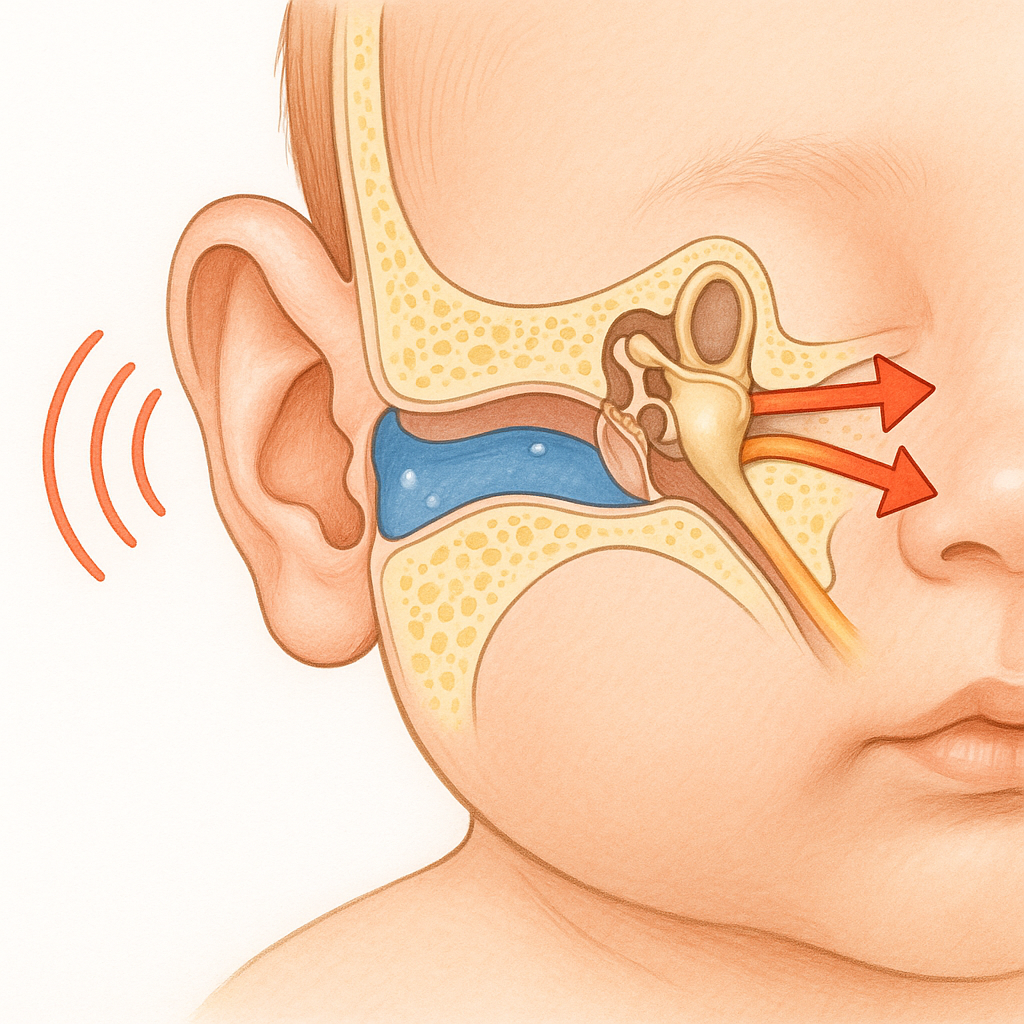
Babies are prone to ear infections, or otitis media, due to their unique anatomy and developing immune systems. Their eustachian tubes—small passages connecting the middle ear to the throat—are short, narrow, and nearly horizontal. This design traps fluid behind the eardrum, creating a perfect environment for bacteria or viruses to thrive, especially after a cold or respiratory infection. An immature immune system struggles to fight off these invaders, making ear infections a frequent challenge. According to the National Institute on Deafness and Other Communication Disorders, five out of six children experience at least one ear infection by age 3, making it one of the most common reasons for pediatric visits.
Beyond the immediate discomfort of pain and fever, the real concern lies in the lingering effects. Fluid buildup, known as otitis media with effusioncan persist for weeks or months, muffling sounds during a critical window when your baby’s brain is wiring its language and auditory circuits. This temporary hearing loss can weaken connections essential for speech, attention, and even social-emotional development. Clear hearing is vital for learning, as explored in Hearing & Vision: Why They’re Key for Baby’s Learning. For brain-conscious parents, understanding this connection is the first step to protecting your child’s cognitive growth.
How does temporary hearing loss from an ear infection disrupt language circuits in the developing brain?
The first three years of life are a whirlwind of brain development. The auditory cortex, responsible for processing sound, is highly plastic, meaning every word, song, or sound you share strengthens neural synapses. When fluid from an ear infection blocks the eardrum—a condition called “glue ear”—sounds are dampened by 20–30 decibels, akin to hearing the world through earmuffs. This muffled input starves the brain of clear auditory signals, disrupting the formation of robust language circuits.
- A 2024 study from the University of Florida found that children with three or more ear infections before age 3 had vocabularies 25% smaller than their peers, with delays persisting into preschool.
- Brain-wave studies, such as auditory brainstem response (ABR) tests, show slower neural processing after just one month of conductive hearing loss as per American Speech-Language-Hearing Association - Effects of Hearing Loss.
- Parents may notice subtle signs: fewer new words, unclear or inconsistent babbling, reduced response to soft sounds, or frustration during story time or conversations.
Once the ear clears, you can help your baby’s brain recover by flooding it with rich, clear sounds. Singing lullabies, reading aloud, naming objects during play, and engaging in activities from 5 Baby Exercises to Boost Brain Development can stimulate auditory pathways and support catch-up growth. For example, repetitive exposure to rhyming books or interactive games like peek-a-boo can reinforce sound recognition and language skills.
Can an ear infection really reach the brain, and what warning signs demand emergency care?
While rare, untreated middle-ear infections can lead to serious complications, with 0.5–4% of cases spreading to the brain or its protective coverings, potentially causing conditions like meningitis or mastoiditis. These risks, though uncommon, are life-threatening, making early recognition critical.
Emergency warning signs include:
- High fever above 102°F (38.9°C) that doesn’t respond to acetaminophen or ibuprofen
- Persistent vomiting or severe, unrelenting headaches
- Neck stiffness, seizures, or a bulging soft spot (fontanelle) in infants
- Pus, blood, or swelling behind the ear, often indicating mastoiditis
If any of these symptoms appear, seek emergency care immediately. Babies born prematurely or with weakened immune systems face higher risks, so extra vigilance is key. Learn more about supporting preterm infants in Premature Baby Brain: Helping Your Preemie Thrive.
What are the long-term cognitive and behavioral ripples of recurrent ear infections?
Recurrent ear infections can create ripples that extend beyond toddlerhood. The temporary hearing loss caused by chronic fluid buildup disrupts the brain’s ability to process auditory cues, which can affect language, learning, and social skills over time. A 2021 study in BMC Pediatrics found that children with frequent ear infections at ages 4–5 were twice as likely to struggle with peer relationships by ages 10–11, likely due to missed social cues during early interactions.
Potential long-term effects include:
- Language challenges: Slower word retrieval, weaker reading fluency, and difficulty following conversations in noisy settings like classrooms.
- Attention difficulties: A shorter attention span, especially in environments with background noise, as the brain struggles to filter auditory input.
- Behavioral issues: Increased frustration or irritability, stemming from communication challenges or missed social signals.
What proven steps can parents take to prevent ear infections and safeguard brain development?
Small, consistent habits can dramatically reduce the risk of ear infections and safeguard your baby’s brain. Here are evidence-based strategies:
- Vaccinate on schedule. The PCV13 (pneumococcal) and annual flu vaccines reduce ear infection risk by up to 35%, as they target bacteria and viruses commonly linked to otitis media as per CDC - Childhood Immunization Schedule.
- Breastfeed exclusively for six months, if possible. Breast milk contains antibodies that protect the middle ear, reducing infection risk by approximately 23%. See Baby Friendly Initiative - Research on Ear Infections.
- Maintain a smoke-free home. Secondhand smoke triples the risk of ear infections by irritating the eustachian tubes as noted in the American Academy of Pediatrics - Secondhand Smoke.
- Feed bottles upright. Avoid “bottle propping” to prevent milk from flowing into the eustachian tubes, which promote bacterial growth.
- Practice good hygiene. Regularly hand-wash and limit exposure to sick children in daycare settings reduce the spread of infections.
For a holistic approach to immune health, explore how gut health supports brain development in Baby Gut Health: How It Supports Brain Development.
When should you push for a hearing test, antibiotics, or specialist referral?
Act promptly to protect hearing and development. Treatment depends on your baby’s age and symptoms:
- Under 6 months: Ear infection signs typically require immediate antibiotics due to higher risks and incomplete vaccinations according to Johns Hopkins Medicine - Ear Infections.
- 6 months to 2 years: For mild cases (pain less than 48 hours, fever below 102°F/38.9°C), pediatricians may recommend watchful waiting for 48–72 hours, as many infections resolve naturally.
- Persistent issues: Fluid lasting more than 3 months, three infections in six months, or signs of speech delays warrant a hearing test (e.g., otoacoustic emissions or ABR screenings) and possible referral to an ear, nose, and throat (ENT) specialist.
Newborns are eligible for painless hearing screenings from birth, which can establish a baseline for monitoring auditory health. If you suspect delays, don’t hesitate to request an evaluation—early intervention is key.
How do you balance antibiotics, gut health, and resistance worries?
Antibiotics are a powerful tool but require careful use. For high-risk infants (e.g., those under 6 months or with severe symptoms), antibiotics are often necessary to prevent complications. For older babies with milder cases, watchful waiting may suffice. When antibiotics are prescribed, completing the full course is critical to prevent antibiotic-resistant bacteria, or “superbugs.”
To mitigate side effects like diarrhea, consider probiotics such as Lactobacillus rhamnosus. A 2023 Cochrane review found that probiotics reduced antibiotic-associated diarrhea by up to 50% in children. Emerging research is also exploring long-acting gel antibiotics that target bacterial biofilms in chronic cases, offering hope for fewer recurrences. Always consult your pediatrician before starting probiotics or altering treatment plans.
Rapid-fire answers to parents’ top ear-infection questions
-
Do ear infections always cause fever?
No. Up to 30% of babies show no fever, with signs like ear tugging, fussiness, or sleep disturbances as the only clues. -
Are breastfed babies really safer?
Yes. Exclusive breastfeeding for six months reduces ear infection risk by about 23%, thanks to protective antibodies in breast milk -
Can fluid without infection still hurt learning?
Absolutely. Chronic effusion can drop hearing by 30 dB, similar to someone whispering from another room, and slow language growth. -
How fast do ear tubes restore hearing?
Often within days. Once tubes drain fluid, parents often notice improved babbling and responsiveness to soft sounds almost immediately. -
Will my child “catch up” after delays?
Usually, with support. Early speech therapy, combined with rich language exposure like reading and singing, helps most children close the gap within 6–12 months
Final Thoughts: Protecting Tiny Ears, Nurturing Growing Brains
Ear infections may be a near-universal part of childhood, but their impact on your baby’s developing brain doesn’t have to be. By staying vigilant for subtle signs, adopting preventive habits, and seeking timely care, you can keep your child’s auditory world clear and vibrant. From singing silly songs to scheduling vaccinations, every step you take supports their language, learning, and laughter—today and for years to come. For more ways to foster your baby’s growth, explore Your Baby’s Brain: A Parent’s Guide to Development.